MRI Principles - Signal Secrets
- Core Sequences & Tissue Signals:
- T1-Weighted (T1W): Anatomy. Fat is bright (hyperintense); water/CSF is dark (hypointense). 📌 T1: 1 thing bright (fat).
- T2-Weighted (T2W): Pathology. Fat and water/CSF are bright. 📌 T2: 2 things bright (fat, water).
- Proton Density (PD): High signal where proton concentration is high (e.g., brain parenchyma).
- Key Specialized Sequences:
- FLAIR (Fluid Attenuated Inversion Recovery): T2-like, but CSF signal is suppressed (dark). Highlights periventricular lesions (e.g., MS plaques).
- DWI (Diffusion-Weighted Imaging): Shows restricted water movement. Crucial for acute stroke detection.
- GRE (Gradient Recalled Echo) / SWI (Susceptibility Weighted Imaging): Detects hemorrhage (dark), calcification.
- Contrast Agents:
- Gadolinium-based: Shortens T1 relaxation time. Brightens inflamed tissues, tumors, vessels. ⚠️ Risk of Nephrogenic Systemic Fibrosis (NSF) in severe renal impairment.
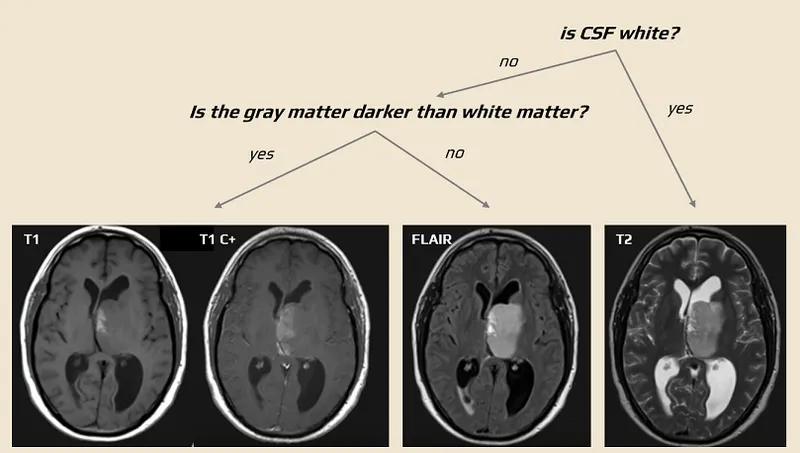
- Signal Characteristics Table:
| Tissue/Pathology | T1W | T2W | FLAIR | DWI |
|---|---|---|---|---|
| CSF | Dark | Bright | Dark | Dark |
| White Matter | Light Grey | Dark Grey | Dark Grey | Grey |
| Grey Matter | Grey | Light Grey | Light Grey | Grey |
| Fat | Bright | Bright | Bright | Dark |
| Acute Hemorrhage | Variable | Dark (oxyHb) / Bright (deoxyHb) | Variable | Variable |
| Chronic Hemorrhage | Bright (metHb) | Dark (hemosiderin) | Dark | Dark |
| Edema (vasogenic) | Dark | Bright | Bright | Dark |
| Acute Ischemic Stroke | Normal/Dark | Bright | Bright | Bright |
| Tumor (enhancing) | Dark (pre), Bright (post-Gd) | Bright | Bright | Variable |
Neuroaxis MRI - Brain & Spine Snapshots
- Brain MRI: Key Structures & Views
- Standard Views (Axial, Sagittal, Coronal): Identify lobes (frontal, parietal, temporal, occipital), ventricles, basal ganglia (caudate, putamen, globus pallidus), thalamus, corpus callosum, brainstem (midbrain, pons, medulla), and cerebellum.
- Dedicated Sequences: For pituitary fossa and Internal Auditory Canals (IACs).
- Spine MRI: Core Assessment
- Vertebral Bodies: Check alignment and height.
- Intervertebral Discs: Evaluate hydration (T2 bright signal) and identify herniation types (bulge, protrusion, extrusion, sequestration).
- Spinal Cord: Assess signal intensity and morphology.
- Neural Elements: Examine nerve roots and facet joints.
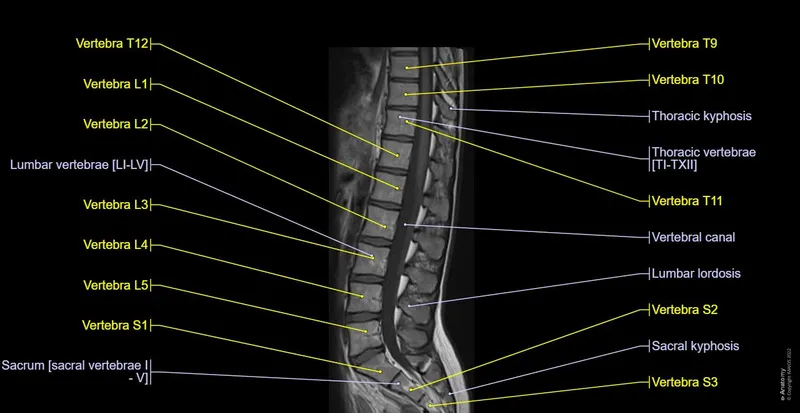
⭐ On T2-weighted images of the spine, normal intervertebral discs appear bright due to high water content; dessicated or degenerated discs lose this hyperintensity.
MSK & Body MRI - Joint & Organ Views
- MSK - Knee:
- Menisci (medial C-shaped, lateral O-shaped): Normal low signal. Tears: ↑ signal reaching articular surface.
- Ligaments: ACL, PCL, MCL, LCL - assess integrity, tears (↑ signal, discontinuity).
- Cartilage: Smooth, intermediate signal. Defects, thinning.
- Bone marrow: Edema (↑ T2 signal), effusions (fluid signal).
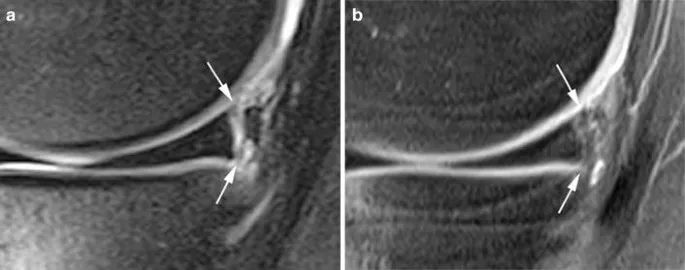
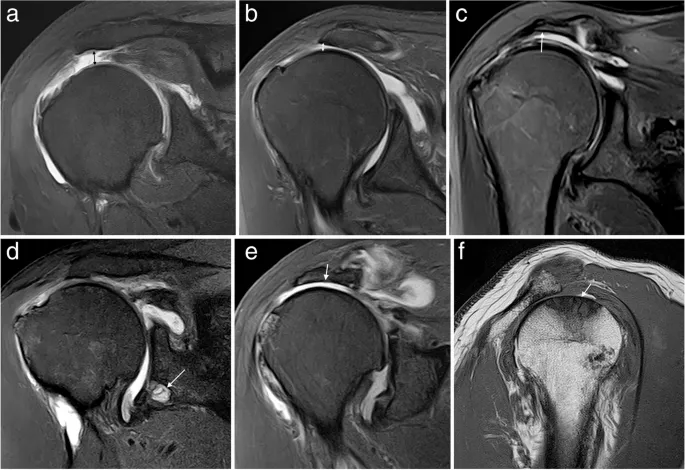
- MSK - Shoulder:
- Rotator Cuff: Supraspinatus, infraspinatus, teres minor, subscapularis. Tears, tendinopathy (↑ signal, thickening).
- Labrum: Glenoid labrum tears.
- Biceps tendon: Tenosynovitis, tears.
- Basic Tissue Appearance (T1, T2, PD):
- Muscle: Intermediate signal.
- Tendon/Ligament: Normally dark (low signal) on all sequences.
- Cartilage: Intermediate signal.
- Body MRI (Basic T1/T2 Appearance & Location):
- Liver, Spleen, Kidneys, Pancreas: Assess signal, morphology.
- Uterus, Bladder: Pelvic anatomy; bladder shows fluid signal.
- Common MRI Artifacts:
- Motion: Blurring, ghosting. Cause: Patient movement.
- Metal Susceptibility (Blooming): Signal loss/distortion near metal. Cause: Metallic implants.
- Chemical Shift: Dark/bright bands at fat-water interfaces. Cause: Different resonant frequencies of fat/water protons.
- Aliasing/Wrap-around: Anatomy outside Field of View (FOV) wraps into image. Cause: FOV too small.
⭐ Fluid-sensitive sequences like T2-weighted with fat suppression (T2 FS) or STIR are crucial in MSK MRI for detecting edema, inflammation, and fluid in ligamentous/meniscal tears.
High‑Yield Points - ⚡ Biggest Takeaways
- T1-Weighted (T1W): Fat is bright, water/CSF dark; excellent for anatomical detail.
- T2-Weighted (T2W): Water/fluid bright, fat also bright; highlights pathology like edema.
- FLAIR: CSF signal suppressed (dark); superior for periventricular lesions (e.g., MS plaques).
- DWI: Detects acute stroke (bright) by showing restricted water diffusion.
- Gadolinium contrast (T1W): Enhances areas of blood-brain barrier disruption (tumors, infections).
- MRI Safety: Paramount due to strong magnetic fields; screen for contraindications (pacemakers).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

