Bones & Joints (Leg & Foot) - Foundation Feats
- Leg Bones:
- Tibia: Medial, primary weight-bearer; medial malleolus.
- Fibula: Lateral, for muscle attachment & ankle stability; lateral malleolus.
- Foot Bones (26 total):
- Tarsals (7): 📌 Tall Californian Navy Medical Interns Lay Cuties (Talus, Calcaneus, Navicular, Medial, Intermediate, Lateral Cuneiforms, Cuboid).
- Talus: Keystone of ankle; articulates tibia/fibula.
- Calcaneus: Heel bone; largest tarsal.
- Metatarsals (5): I-V (medial to lateral).
- Phalanges (14): Proximal, Middle, Distal (Hallux: P, D only).
- Tarsals (7): 📌 Tall Californian Navy Medical Interns Lay Cuties (Talus, Calcaneus, Navicular, Medial, Intermediate, Lateral Cuneiforms, Cuboid).
- Key Joints:
- Ankle (Talocrural): Tibia + Fibula + Talus. Hinge: Dorsiflexion/Plantarflexion.
- Subtalar (Talocalcaneal): Talus + Calcaneus. Inversion/Eversion.
- Midtarsal (Chopart's): Talonavicular & Calcaneocuboid.
- Tarsometatarsal (Lisfranc's).
⭐ Talus has no direct muscular or tendinous attachments. anatomical view for NEET PG medical students showing labels
Leg Compartments - Muscle Mania
-
Anterior Compartment
- Muscles: Tibialis anterior, EHL, EDL, Peroneus tertius.
- Nerve: Deep Peroneal N.
- Action: Dorsiflexion, Toe extension, Inversion (Tib. Ant).
- 📌 Mnemonic: "Teachers Hate Extra Dirty Plays, Never!" (TA,EHL,EDL,PT,Deep Peroneal N.)
-
Lateral Compartment
- Muscles: Peroneus longus & brevis.
- Nerve: Superficial Peroneal N.
- Action: Eversion, Weak plantarflexion.
-
Posterior Compartment (Superficial)
- Muscles: Gastrocnemius, Soleus, Plantaris.
- Nerve: Tibial N.
- Action: Plantarflexion; Knee flexion (Gastrocnemius).
- 📌 Mnemonic: "Go Slow Please" (Gastrocnemius,Soleus,Plantaris).
-
Posterior Compartment (Deep)
- Muscles: Tibialis posterior, FDL, FHL, Popliteus.
- Nerve: Tibial N.
- Action: Plantarflexion, Toe flexion, Inversion (Tib. Post), Unlocks knee (Popliteus).
- 📌 Mnemonic: "Tiny Dogs Hate People" (TP,FDL,FHL,Popliteus).
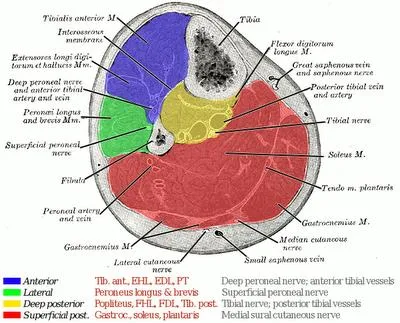
⭐ Anterior compartment is most prone to compartment syndrome.
Foot Anatomy (Muscles & Arches) - Arch & Action
- Arches of the Foot: Provide shock absorption, weight distribution, propulsion.
- Medial Longitudinal Arch (MLA): Higher & more dynamic.
- Bones: Calcaneus, talus, navicular, 3 cuneiforms, medial 3 metatarsals.
- Keystone: Head of Talus.
- Dynamic Support: Tibialis posterior (main), FHL, FDL, Tibialis anterior.
- Static Support: Plantar aponeurosis, spring ligament (plantar calcaneonavicular).
- Lateral Longitudinal Arch (LLA): Flatter & more rigid.
- Bones: Calcaneus, cuboid, lateral 2 metatarsals.
- Keystone: Cuboid.
- Dynamic Support: Peroneus longus & brevis, Peroneus tertius.
- Static Support: Long & short plantar ligaments.
- Transverse Arch: Formed by cuneiforms, cuboid, & metatarsal bases.
- Keystone: Intermediate cuneiform.
- Dynamic Support: Peroneus longus, Tibialis posterior, Adductor hallucis (transverse head).

- Medial Longitudinal Arch (MLA): Higher & more dynamic.
⭐ The tendon of Tibialis Posterior is the primary dynamic support for the medial longitudinal arch of the foot, crucial for maintaining its integrity during weight-bearing activities like walking and running.
Leg & Foot Neurovascular + Clinicals - Nerve Nets & Nasty Knocks
- Arteries: Popliteal → Ant. Tibial (→ Dorsalis Pedis) & Post. Tibial (→ Medial/Lateral Plantar, Peroneal).
- Nerves:
- Clinicals:
- CPN Injury (Fibular neck): Foot drop (↓DF/EV).
⭐ Injury to the Common Peroneal Nerve results in foot drop (inability to dorsiflex and evert the foot).
- Tibial N. Injury: ↓PF/IV; Tarsal Tunnel Syndrome.
- Compartment Syndrome (Ant. most common): ↑pressure; 5 Ps (Pain, Pallor, Paresthesia, Pulselessness, Paralysis - late).
- Achilles Rupture: (+) Thompson test.

- CPN Injury (Fibular neck): Foot drop (↓DF/EV).
High‑Yield Points - ⚡ Biggest Takeaways
- Common peroneal nerve injury at fibular neck causes foot drop and sensory loss on foot dorsum.
- Tibial nerve supplies posterior leg compartment and plantar muscles; injury impairs plantarflexion.
- Anterior talofibular ligament (ATFL) is most commonly injured in inversion ankle sprains.
- Medial longitudinal arch is critically supported by the tibialis posterior tendon.
- Anterior compartment syndrome is most frequent, with severe pain and paresthesia as early signs.
- Deep peroneal nerve innervates anterior leg muscles, its damage also causing foot drop.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

