Immunopathology — Flashcards

On this page
LE cell is a phagocytic _____ or _____ that has engulfed the denatured nucleus of an injured cell
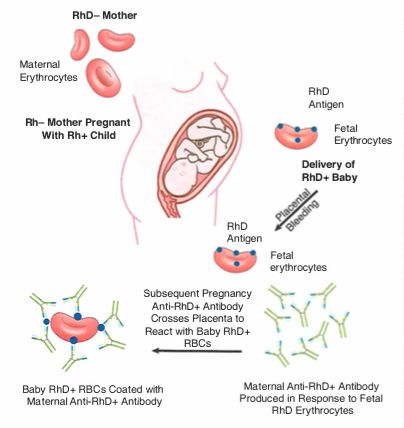
--- Do with heme --- Type II Hypersensitivity Disorders - Cytotoxic: Transfusion Reaction - Antibody against _____ - IgM isohemagglutinins formed naturally in response to bacterial flora cause opsonization and complement activation - Leads to hemolysis **Hemolytic Disease of the Newborn (Erythroblastosis fetalis) Antibody = _____ - Formed in _____ mother carrying _____ child - First pregnancy _____ (doesn't have to be viable pregnancy) - Antibody crosses placenta and injures subsequent fetuses - Prevent with _____ (anti-Rh, binds fetal red cells and prevents mothers immune system from reacting) ABO blood typing and screening for other preformed Abs; always done in case of transplants. Universal donor: type _____ Universal recipient: type _____ (Ex) Type A can donate to _____ and _____. Type A can receive donations from _____ and _____. - Anti-B antibodies prevent donation from type B and type AB. HLA Typing - Microcytotoxicity test Tests for MHC _____ Test hundreds of different haplotypes to find a potential match. Cells recognized by antibody will be attacked by complement and thus become leaky and take up dye. HLA Typing - Mixed lymphocyte reaction Tests for MHC class _____ Take donor cells and irradiate them (prevent proliferation). Irradiated cells are mixed with donor cells to see if proliferation occurs. Higher radioactivity (thymidine) signifies _____ compatibility.
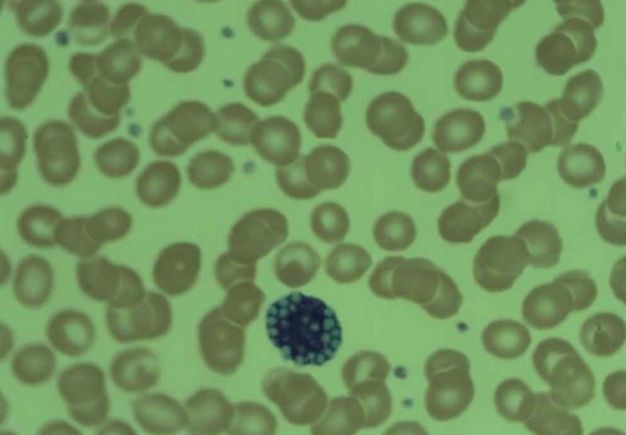
_____ cells are plasma cells characterized by the accumulation of multiple Russell bodies
Type I HSR occurs due to cross-linking of Ig_____ on presensitized mast cells and basophils by antigen
_____ is caused by a defect in the BTK gene
--- Do with heme ---Type II Hypersensitivity Disorders - Cytotoxic:Transfusion Reaction - Antibody against _____ - IgM isohemagglutinins formed naturally in response to bacterial flora cause opsonization and complement activation - Leads to hemolysis**Hemolytic Disease of the Newborn (Erythroblastosis fetalis)Antibody = Anti-RhD+ IgG - Formed in Rh- mother carrying Rh+ child - First pregnancy sensitizes (doesn't have to be viable pregnancy) - Antibody crosses placenta and injures subsequent fetuses - Prevent with RhoGAM (anti-Rh, binds fetal red cells and prevents mothers immune system from reacting) ABO blood typing and screening for other preformed Abs; always done in case of transplants.Universal donor: type OUniversal recipient: type AB (Ex) Type A can donate to type A and type AB. Type A can receive donations from type A and type O. - Anti-B antibodies prevent donation from type B and type AB. HLA Typing - Microcytotoxicity testTests for MHC class I (HLA-A, HLA-B)Test hundreds of different haplotypes to find a potential match. Cells recognized by antibody will be attacked by complement and thus become leaky and take up dye. HLA Typing - Mixed lymphocyte reactionTests for MHC class II (HLA-DR)Take donor cells and irradiate them (prevent proliferation). Irradiated cells are mixed with donor cells to see if proliferation occurs. Higher radioactivity (thymidine) signifies lower compatibility.
What HLA subtypes are associated with type I diabetes mellitus? _____ and DR4
_____ syndrome is most commonly due to mutated CD40L on Th cells
IFN- acts to stimulate an anticancer immune environment in three ways- inhibit the proliferation of _____- activating lymphocytes- enhancing expression of MHCI/II
B-cell activation requires a costimulatory signal from binding between the _____ (B cell) and CD40 ligand (Th2 cell)
Study by Chapter
Cells and Tissues of the Immune System
Flashcards
Innate Immunity
Flashcards
Adaptive Immunity
Flashcards
Hypersensitivity Reactions
Flashcards
Autoimmune Diseases
Flashcards
Immunodeficiency Disorders
Flashcards
Transplantation Immunopathology
Flashcards
Immune Response to Infections
Flashcards
Immunologic Laboratory Techniques
Flashcards
Tumor Immunology
Flashcards
About Immunopathology Flashcards for NEET-PG
These Immunopathology flashcards are designed for NEET-PG Pathology preparation, using active recall to help you retain high-yield concepts, clinical correlations, and commonly tested facts. Each card prompts you to retrieve information from memory rather than passively reviewing notes, which research shows leads to significantly better exam performance.
The 83 cards in this deck cover the most important topics in Immunopathology, including key mechanisms, diagnostic criteria, treatment protocols, and clinical pearls that frequently appear in NEET-PG examinations. Cards are organised by chapter so you can focus on specific areas or work through the entire topic systematically.
For personalised spaced repetition scheduling that adapts to your performance, unlimited flashcards, and detailed progress analytics, download the Oncourse app.
Frequently Asked Questions
Are Immunopathology flashcards free on Oncourse?
How do flashcards help with NEET-PG preparation?
How many Immunopathology flashcards are available?
Can I study Immunopathology flashcards by chapter?
What topics do these Pathology flashcards cover?
Want unlimited flashcards?
Get full access to all flashcards, spaced repetition, and progress tracking.
Start For Free