Back
Weech Formula for Weight and Height: Pediatrics High-Yield Guide for NEET PG and USMLE (2026)
Master the Weech formula for pediatric weight, height, and head circumference calculations. Essential guide for NEET PG and USMLE with mnemonics, practice questions, and clinical applications.

Weech Formula for Weight and Height: Pediatrics High-Yield Guide for NEET PG and USMLE (2026)
You are probably staring at a pediatrics question about expected weight for a 3-year-old and thinking: "Is there actually a formula for this, or am I supposed to memorize every single growth chart?" Here is the truth — the Weech formula is your secret weapon for pediatric growth calculations in NEET PG and USMLE Step 1.
The Weech formula gives you expected weight, height, and head circumference for any age between 1-12 years. No guesswork. No fumbling through percentile charts during your exam. Just clean, mathematical precision that works every single time.
NEET PG loves testing growth parameters. Out of 200 questions, you will see 3-4 pediatrics growth scenarios. The difference between knowing these formulas and not knowing them? 12-16 marks. That is the difference between your rank and someone else's admission.
What is the Weech Formula?
The Weech formula is a set of mathematical equations used to calculate expected anthropometric measurements for children aged 1-12 years. Named after Dr. A.A. Weech, these formulas provide quick, reliable estimates for:
Expected weight for age
Expected height for age
Expected head circumference for age
These formulas are particularly valuable in clinical practice for assessing growth patterns, identifying malnutrition, and screening for growth disorders. For exam purposes, they are essential for solving pediatric growth-related MCQs without needing to reference complex growth charts.
The beauty of the Weech formula lies in its simplicity. Instead of memorizing dozens of percentile values, you memorize 3 core formulas and can calculate any growth parameter for any age.
Core Weech Formulas: The Essential Trio
1. Expected Weight Formula
For children 1-12 years:
```
Expected Weight (kg) = Age (years) × 2 + 8
```
Examples:
2-year-old: (2 × 2) + 8 = 12 kg
5-year-old: (5 × 2) + 8 = 18 kg
10-year-old: (10 × 2) + 8 = 28 kg
2. Expected Height Formula
For children 1-12 years:
```
Expected Height (cm) = Age (years) × 6 + 77
```
Examples:
3-year-old: (3 × 6) + 77 = 95 cm
6-year-old: (6 × 6) + 77 = 113 cm
8-year-old: (8 × 6) + 77 = 125 cm
3. Expected Head Circumference Formula
For children 1-5 years:
```
Expected Head Circumference (cm) = Age (years) × 1 + 46
```
Examples:
1-year-old: (1 × 1) + 46 = 47 cm
3-year-old: (3 × 1) + 46 = 49 cm
5-year-old: (5 × 1) + 46 = 51 cm
Important: Head circumference formula is only valid up to 5 years, as head growth plateaus significantly after this age.
Memory Tricks That Actually Work
The "2-8 Weight Rule"
Remember: "Two times age plus eight"
The number 2 appears twice (multiply by 2, add 8)
Think: "2 + 8 = 10" (easy to remember)
Mental anchor: A 1-year-old should weigh 10 kg (2×1+8=10)
The "6-77 Height Rule"
Remember: "Six times age plus seventy-seven"
77 looks like two lucky sevens
Think: 77 cm is roughly 2.5 feet (newborn length)
Mental anchor: A 2-year-old should be 89 cm tall (6×2+77=89)
The "1-46 Head Rule"
Remember: "One times age plus forty-six"
Simplest formula (just add age to 46)
46 is close to 50 (easy round number)
Mental anchor: Head grows 1 cm per year after first birthday
Clinical Applications in Pediatric Assessment
Malnutrition Screening
The Weech formula is crucial for identifying malnutrition patterns:
Grade I Malnutrition (Mild):
Weight 75-80% of expected weight for age
Example: 4-year-old weighing 12 kg (expected: 16 kg = 75%)
Grade II Malnutrition (Moderate):
Weight 60-74% of expected weight for age
Example: 6-year-old weighing 14 kg (expected: 20 kg = 70%)
Grade III Malnutrition (Severe):
Weight <60% of expected weight for age
Example: 8-year-old weighing 14 kg (expected: 24 kg = 58%)
Growth Velocity Assessment
Normal Growth Patterns:
Weight gain: 2 kg per year (derived from formula)
Height gain: 6 cm per year (derived from formula)
Head circumference gain: 1 cm per year (up to 5 years)
Red Flags:
Weight <70% of expected (consider malnutrition)
Height <90% of expected (consider growth hormone deficiency)
Head circumference >2 SD below expected (consider microcephaly)
Failure to Thrive Evaluation
Use Weech formulas as first-line screening:
1. Calculate expected weight for age
2. Compare actual weight to expected
3. If <80% of expected → investigate further
4. Combine with height assessment for comprehensive evaluation
High-Yield NEET PG Question Patterns
Pattern 1: Direct Calculation Questions
Question Type: "What is the expected weight of a 7-year-old child?" Approach:
Apply formula: (7 × 2) + 8 = 22 kg
Look for closest option
Common distractors: 20 kg, 24 kg, 26 kg
Pattern 2: Malnutrition Grading Questions
Question Type: "A 5-year-old child weighs 12 kg. What grade of malnutrition is this?" Approach:
Expected weight: (5 × 2) + 8 = 18 kg
Actual percentage: (12/18) × 100 = 67%
Grade II malnutrition (60-74% range)
Pattern 3: Growth Comparison Questions
Question Type: "Which child has the most significant growth delay?"
Option A: 3-year-old, height 85 cm
Option B: 4-year-old, height 95 cm
Option C: 6-year-old, height 105 cm
Approach:
Calculate expected heights: 95 cm, 101 cm, 113 cm
Find percentage of expected: 89%, 94%, 93%
Option A has lowest percentage
Pattern 4: Combined Parameter Questions
Question Type: Multiple measurements given, identify the abnormal one Strategy:
Calculate expected values for all parameters
Compare percentages systematically
Flag values <80% of expected as abnormal
Comparison with Other Growth Standards
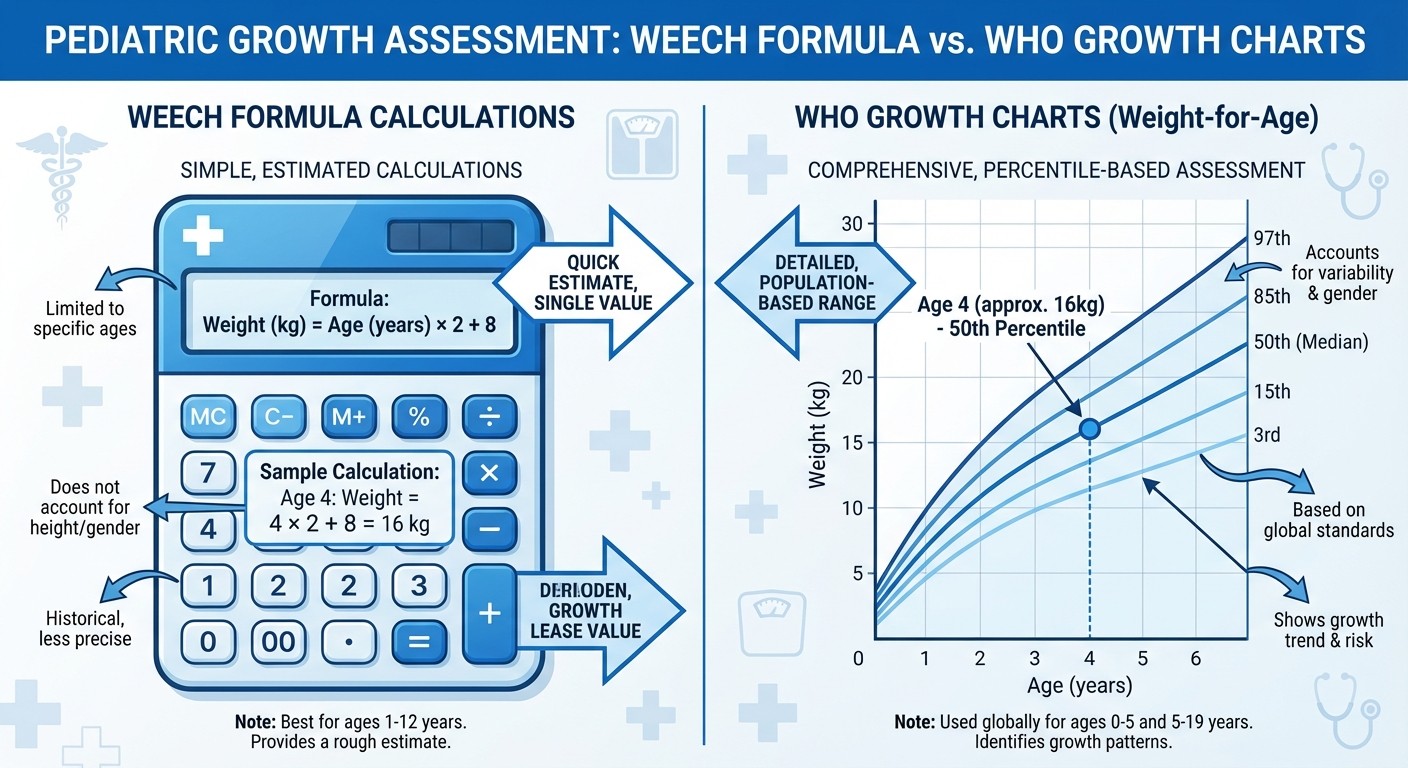
WHO Growth Standards vs Weech Formula
Aspect | WHO Standards | Weech Formula |
|---|---|---|
Age Range | 0-19 years | 1-12 years |
Method | Percentile charts | Mathematical formulas |
Accuracy | Population-specific | Quick estimates |
Exam Utility | Time-consuming | Rapid calculation |
Clinical Use | Gold standard | Screening tool |
IAP Growth Charts vs Weech Formula
Indian Academy of Pediatrics (IAP) Charts:
Based on Indian population data
More accurate for Indian children
Requires chart reference during calculation
Weech Formula:
Universal application
No charts needed
Slightly less population-specific accuracy
Perfect for exam conditions
When to Use Each Method
Use Weech Formula for:
NEET PG and USMLE questions
Quick screening in OPD
Emergency situations without charts
Mental calculations during rounds
Use WHO/IAP Charts for:
Detailed growth monitoring
Research purposes
Plotting growth trajectories
Identifying specific percentiles
Advanced Applications and Modifications
Modified Formulas for Special Populations
Premature Infants:
Use corrected age for calculations
Corrected age = Chronological age - (40 weeks - gestational age at birth)
Apply Weech formula to corrected age
Chronic Disease Conditions:
Expected values may need 10-15% downward adjustment
Consider disease-specific growth charts when available
Use Weech formula as baseline reference
Nutritional Status Classification
Gomez Classification (Weight-for-Age):
Normal: >90% of expected weight
Grade I: 76-90% of expected weight
Grade II: 61-75% of expected weight
Grade III: ≤60% of expected weight
Waterlow Classification (Height and Weight):
Acute malnutrition (wasting): Weight-for-height <80%
Chronic malnutrition (stunting): Height-for-age <95%
Combined: Both parameters affected
Practice Questions with Detailed Solutions
Question 1
A 6-year-old child weighs 14 kg and has a height of 105 cm. What is the most appropriate assessment?
A) Normal growth parameters
B) Grade I malnutrition with normal height
C) Grade II malnutrition with stunting
D) Grade III malnutrition with normal height
Solution:
Expected weight: (6 × 2) + 8 = 20 kg
Actual weight percentage: (14/20) × 100 = 70%
Expected height: (6 × 6) + 77 = 113 cm
Actual height percentage: (105/113) × 100 = 93%
Weight 70% = Grade II malnutrition
Height 93% = Normal range
Answer: B
Question 2
The head circumference of a 3-year-old child measures 47 cm. This indicates:
A) Microcephaly
B) Normal head circumference
C) Macrocephaly
D) Craniosynostosis
Solution:
Expected head circumference: (3 × 1) + 46 = 49 cm
Actual measurement: 47 cm
Percentage: (47/49) × 100 = 96%
96% falls within normal range (>95%)
Answer: B
How Oncourse AI Enhances Pediatric Learning
Oncourse transforms pediatric growth assessment from memorization nightmare into systematic mastery. Our adaptive learning system identifies exactly where you struggle with growth formulas and provides targeted practice.
Key Features for Pediatric Growth Topics:
Smart MCQ Selection: Our AI identifies your weak areas in growth assessment and serves relevant questions
Formula Integration: Every growth-related question includes formula reminders and step-by-step calculations
Pattern Recognition: Practice questions organized by NEET PG question patterns (direct calculation, malnutrition grading, etc.)
Real-time Explanations: Instant AI feedback on why you got growth calculations wrong
Spaced Repetition: Pediatric growth flashcards ensure formula retention
Our question bank includes 1,200+ pediatric growth questions across all difficulty levels. Each question comes with detailed explanations showing formula application and clinical reasoning.
Advanced Learning Tools:
Practice with comprehensive pediatric growth lessons covering normal parameters, disorders, and assessment methods
Test yourself with targeted MCQs on malnutrition and growth disorders
Master nutritional assessment methods for both NEET PG and USMLE preparation
Common Mistakes and How to Avoid Them
Calculation Errors
Mistake 1: Using wrong age unit
Wrong: 18 months → (18 × 2) + 8 = 44 kg
Correct: 18 months = 1.5 years → (1.5 × 2) + 8 = 11 kg
Mistake 2: Applying head circumference formula beyond 5 years
Wrong: 8-year-old head circumference = (8 × 1) + 46 = 54 cm
Correct: Head circumference formula only valid up to 5 years
Mistake 3: Forgetting formula constants
Wrong: Weight = Age × 2 = 10 kg for 5-year-old
Correct: Weight = (Age × 2) + 8 = 18 kg for 5-year-old
Interpretation Errors
Mistake 4: Confusing malnutrition grades
Grade II is 60-75%, not 60-70%
Grade III is <60%, not <65%
Mistake 5: Using single parameter for assessment
Always assess weight AND height together
Consider age-appropriate head circumference when relevant
Beyond the Formulas: Clinical Context
Real-World Application Scenarios
Scenario 1: OPD Screening
A mother brings her 4-year-old for routine checkup. Quick Weech calculation shows expected weight 16 kg, actual weight 12 kg (75%). This triggers detailed nutritional assessment without waiting for chart consultation.
Scenario 2: Emergency Department
A 7-year-old arrives unconscious. Quick height estimation using Weech formula (119 cm expected) helps determine appropriate medication dosing while obtaining accurate measurements.
Scenario 3: School Health Screening
Mass screening of 100 children becomes feasible with mental Weech calculations, identifying 12 children needing detailed growth assessment.
Integration with Modern Pediatric Practice
Digital Health Records:
Weech values serve as automatic red flags in EMR systems
Trigger alerts when actual measurements deviate significantly
Provide baseline expectations for growth trajectory planning
Telemedicine Applications:
Parents can use Weech formulas for home monitoring
Virtual consultations benefit from quick growth assessments
Remote screening becomes more systematic and standardized
Frequently Asked Questions
Can the Weech formula be used for children above 12 years?
No, the Weech formula accuracy decreases significantly after 12 years due to pubertal growth spurts and individual variations. For adolescents, use WHO growth charts or population-specific references that account for pubertal timing.
How accurate is the Weech formula compared to WHO standards?
The Weech formula provides estimates within 5-10% of WHO standards for most children. While not as precise as detailed growth charts, it offers excellent screening accuracy for clinical and exam purposes.
Should I adjust Weech formula calculations for Indian children?
For NEET PG purposes, use the standard Weech formula without modifications. Indian children may have slightly lower average weights, but exam questions are designed around standard formula calculations.
What if a child's measurements dont match any formula?
Always consider the clinical context. Formulas provide expected values for healthy children. Chronic diseases, genetic conditions, or nutritional factors can cause significant deviations from expected values.
Can I use Weech formula for height prediction?
The Weech height formula gives current expected height, not future height prediction. For height prediction, you need bone age assessment, parental height data, and specific prediction formulas.
How do I handle fractional ages in Weech calculations?
Convert months to decimal years (e.g., 30 months = 2.5 years) and apply the formula normally. For exam questions, this level of precision is rarely required, but its good practice for clinical use.
Master pediatric growth assessment systematically with Oncourse's comprehensive pediatric lessons. Our adaptive MCQ system and spaced repetition flashcards ensure you never forget these critical formulas.
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for NEET PG and USMLE. Download free on Android and iOS.