Back
UKMLA Obstetrics and Gynaecology Preparation 2026: High-Yield Topics, Clinical Scenarios and Exam Strategy
Master UKMLA obstetrics gynaecology 2026 with high-yield topics, clinical scenario strategies, and evidence-based revision techniques for AKT success.

UKMLA Obstetrics and Gynaecology Preparation 2026: High-Yield Topics, Clinical Scenarios and Exam Strategy
You are probably wondering which OB/GYN topics will make or break your UKMLA AKT score in 2026. With obstetrics and gynaecology accounting for roughly 12-15% of the Applied Knowledge Test, theres no room for gaps in your preparation. The UKMLA doesnt test textbook recall — it tests whether you can recognise red flags in a 28-week pregnant woman presenting with abdominal pain or choose the right contraceptive for a 35-year-old with migraine.
This isnt about memorising every complication of pre-eclampsia. Its about knowing which complications matter most, how they present clinically, and what the examiners expect you to do next.
UKMLA Obstetrics and Gynaecology: What Gets Tested
The UKMLA AKT tests OB/GYN through single-best-answer clinical scenarios, not isolated facts. You wont see "What hormone causes ovulation?" Instead, expect vignettes like:
"A 32-year-old woman at 36 weeks gestation presents with severe headache, visual disturbances, and epigastric pain. Her BP is 165/105 mmHg. Urinalysis shows 3+ protein. What is the most appropriate immediate management?"
The exam focuses on:
Clinical decision-making: choosing the next best step in management
Red flag recognition: identifying obstetric and gynaecological emergencies
Guidelines application: NICE and RCOG recommendations in practice
Communication scenarios: consent, breaking bad news, safeguarding
Pattern recognition beats pure knowledge. When you see "postmenopausal bleeding," your brain should automatically think malignancy until proven otherwise, not run through every possible cause.
High-Yield Obstetrics Topics for UKMLA 2026
Normal Pregnancy and Antenatal Care
Master the booking visit timeline, screening tests, and monitoring intervals. The exam loves questions about:
Antenatal screening timeline:
Combined screening (10-14 weeks): Down syndrome, Edwards, Patau
Anomaly scan (18-21 weeks): structural abnormalities
Growth scans (28, 32, 36 weeks for high-risk pregnancies)
Red flags in pregnancy get tested repeatedly:
Reduced fetal movements after 28 weeks
Antepartum haemorrhage
Severe headache with visual symptoms
Epigastric pain in third trimester
Oncourse surfaces these antenatal care protocols through spaced repetition flashcards that present NICE guideline facts at optimal revision intervals, preventing last-minute cramming of screening timelines.
Pregnancy Complications
Pre-eclampsia appears in 15-20% of OB/GYN questions. Know the diagnostic criteria:
New-onset hypertension (≥140/90 mmHg) after 20 weeks
Plus proteinuria (≥300mg/24hrs) or maternal organ dysfunction
Management algorithm:
1. BP ≥150/100 mmHg: start antihypertensive (labetalol first-line)
2. Severe features: admit, magnesium sulphate, plan delivery
3. HELLP syndrome: immediate delivery regardless of gestation
Gestational diabetes testing happens at 24-28 weeks (75g OGTT). Treatment starts with dietary modification, then metformin, then insulin. Ectopic pregnancy classic presentation: missed period + abdominal pain + vaginal bleeding. But watch for atypical presentations — shoulder tip pain from peritoneal irritation or just pelvic discomfort.
Labour and Delivery
Focus on partogram interpretation and when to intervene:
Normal cervical dilatation: 0.5cm/hour (nulliparous), 1cm/hour (multiparous)
Prolonged labour: crosses action line on partogram
Fetal heart rate abnormalities: when to expedite delivery
Shoulder dystocia management sequence (HELPERR):
H: Help (call for assistance)
E: Episiotomy
L: Legs (McRoberts position)
P: Pressure (suprapubic)
E: Enter (internal manoeuvres)
R: Remove posterior arm
R: Roll onto all fours
Postnatal Care and Complications
Postnatal depression screening using Edinburgh Postnatal Depression Scale at 6-8 weeks. Score ≥13 indicates possible depression requiring assessment. Mastitis vs breast abscess: mastitis responds to antibiotics within 48 hours; persistent symptoms suggest abscess requiring drainage. Postpartum haemorrhage (>500ml vaginal delivery, >1000ml caesarean):
1. Uterine atony (90% of cases): uterine massage, oxytocin
2. Trauma: examine and repair
3. Tissue retention: manual removal
4. Thrombin disorders: fresh frozen plasma, platelets
Performance analytics help identify which postnatal complications you consistently miss, letting you drill weak areas like postpartum care protocols before exam day.
High-Yield Gynaecology Topics for UKMLA 2026
Menstrual Disorders
Heavy menstrual bleeding first-line treatment:
Mirena IUS (if contraception wanted)
Tranexamic acid (if contraception not wanted)
Combined oral contraceptive pill (if contraception wanted + no contraindications)
Amenorrhoea workup follows a systematic approach:
Primary (no periods by 16): exclude anatomical abnormalities, assess pubertal development
Secondary (periods stop for 6+ months): pregnancy test, then prolactin, FSH, thyroid function
Contraception
The UKMLA tests contraceptive eligibility, not just mechanism. Know the Medical Eligibility Criteria (MEC) categories:
MEC 1: no restriction
MEC 2: advantages generally outweigh risks
MEC 3: risks generally outweigh advantages
MEC 4: unacceptable health risk
COCP contraindications (MEC 3/4):
Migraine with aura
Current or past VTE
Active liver disease
Breast cancer
Smoking + age >35
Emergency contraception timing matters:
Copper IUD: up to 5 days after UPSI (most effective)
Ulipristal acetate: up to 5 days (more effective than levonorgestrel)
Levonorgestrel: up to 3 days
Gynaecological Pathology
Fibroids management depends on symptoms and fertility plans:
Asymptomatic: conservative management
Heavy bleeding: Mirena IUS, tranexamic acid, GnRH analogues
Fertility concerns: myomectomy
Completed family: hysterectomy
Endometriosis gold standard diagnosis remains laparoscopy, though clinical suspicion based on cyclical pain allows empirical treatment. Ovarian cysts management by type:
Simple cysts <5cm: watchful waiting
Complex cysts or >5cm: further imaging (MRI)
Postmenopausal cysts: CA-125 and specialist referral
Cervical screening intervals:
25-49 years: every 3 years
50-64 years: every 5 years
HPV primary screening since 2019
When preparing gynaecological disorders, clinical scenario questions that mirror UKMLA vignettes help you practice applying management algorithms rather than just memorising them.
Menopause
Perimenopause symptoms can start years before periods stop. FSH >30 IU/L suggests menopause in women >45 with typical symptoms. HRT benefits and risks:
Benefits: vasomotor symptoms, bone protection, quality of life
Risks: VTE (oral), breast cancer (combined HRT >5 years), endometrial cancer (unopposed oestrogen)
HRT contraindications: current breast cancer, active liver disease, undiagnosed vaginal bleeding, current VTE.
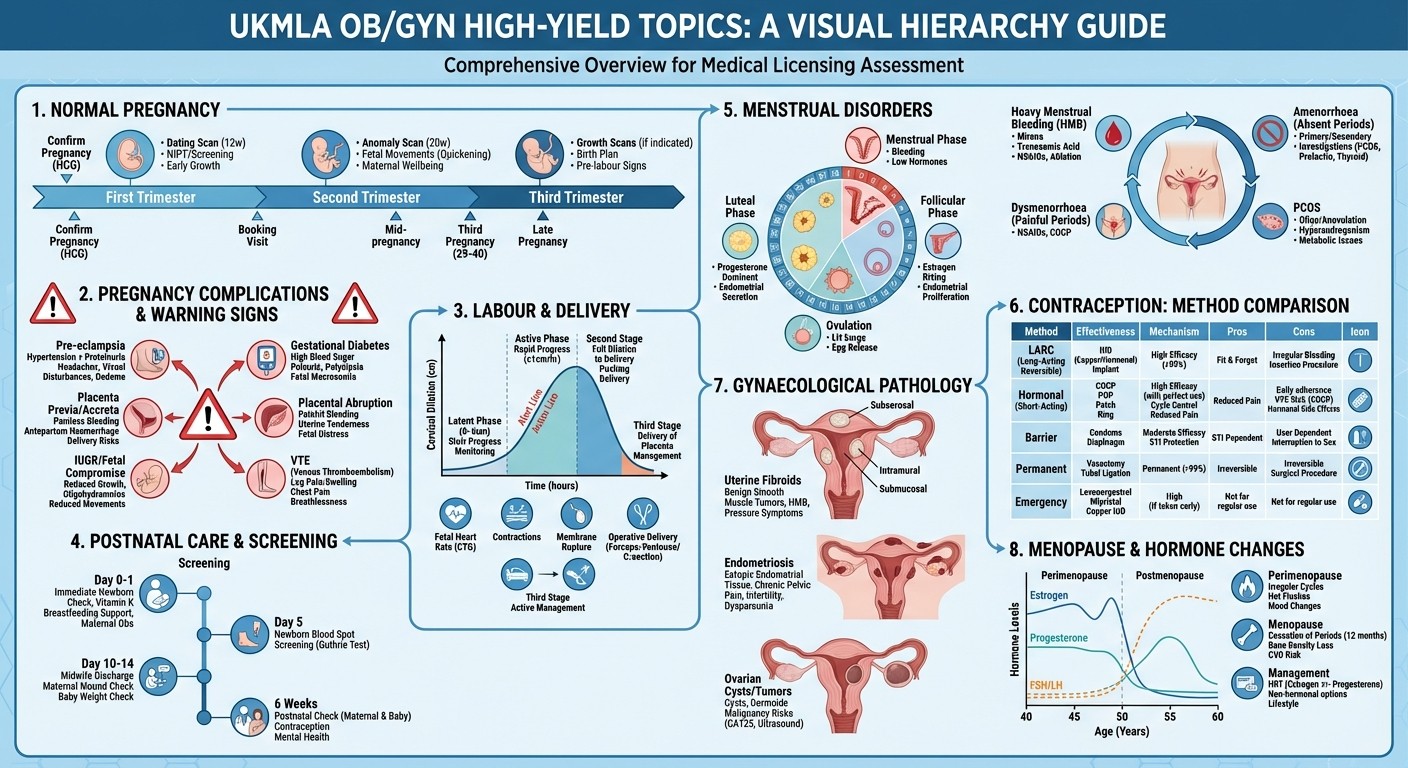
How UKMLA Tests Clinical Scenarios: Pattern Recognition
The UKMLA AKT doesnt ask "What is pre-eclampsia?" It gives you a clinical vignette and tests whether you can recognise the pattern and choose appropriate management.
Common Clinical Scenario Patterns
The "What's the most likely diagnosis?" question:
Presents 3-4 key clinical features
Expects you to synthesise findings into a diagnosis
Wrong answers are often plausible but missing key features
The "What is the most appropriate next step?" question:
Tests clinical decision-making
Often includes multiple reasonable options
Requires knowledge of investigation/treatment sequences
The "What should you tell the patient?" question:
Tests communication skills and consent
Focuses on what patients need to know, not medical details
Wrong answers are often too vague or too technical
Red Flag Recognition
UKMLA questions often hinge on recognising when a scenario represents an emergency. Key red flags include:
Obstetric emergencies:
Reduced fetal movements + abnormal CTG
Antepartum haemorrhage with haemodynamic compromise
Severe pre-eclampsia features (visual symptoms, epigastric pain, hyperreflexia)
Cord prolapse or shoulder dystocia
Gynaecological emergencies:
Ruptured ectopic pregnancy with peritonism
Ovarian torsion (sudden severe pain + vomiting)
Postmenopausal bleeding (malignancy until proven otherwise)
Heavy bleeding requiring transfusion
The key isnt memorising every emergency — its training your pattern recognition so you spot these scenarios quickly during the exam.
UKMLA OB/GYN Revision Strategy
Active Recall vs Passive Reading
Reading through OB/GYN textbooks feels productive but doesnt prepare you for clinical decision-making. Active recall — testing yourself on clinical scenarios — builds the pattern recognition you need.
Instead of reading: "Pre-eclampsia is hypertension plus proteinuria" Practice with scenarios: "32-year-old, 34 weeks pregnant, BP 170/100, 2+ proteinuria, epigastric pain — what's the immediate management?"
This approach trains your brain to jump from clinical presentation to management decision, which is exactly what the UKMLA tests.
Spaced Repetition for Guidelines
OB/GYN is guideline-heavy. You need to know NICE recommendations for antenatal care, RCOG guidelines for operative delivery, contraceptive eligibility criteria, and cervical screening intervals. Pure repetition doesnt work — you forget guidelines within days.
Spaced repetition surfaces these facts when youre about to forget them. Instead of cramming all guidelines in the final week, you encounter them regularly throughout your preparation, building long-term retention.
Case-Based Learning Approach
Week 1-2: Master normal pregnancy, labour, and postnatal care
Focus on timelines and screening schedules
Practice partogram interpretation
Learn postnatal complications recognition
Week 3-4: Pregnancy complications and emergencies
Pre-eclampsia recognition and management
Antepartum and postpartum haemorrhage protocols
Ectopic pregnancy presentations
Week 5-6: Gynaecological conditions
Menstrual disorders and contraception
Benign gynaecological conditions
Cervical screening and HPV management
Week 7-8: Integration and weak areas
Mixed clinical scenarios
Communication and consent questions
Focus on consistently missed topics
Topic-Level Performance Tracking
Rather than studying all OB/GYN equally, identify your weak areas and prioritise accordingly. You might score 85% on normal pregnancy questions but only 60% on gynaecological pathology. Analytics showing topic-level accuracy help you allocate study time where it matters most — drilling ectopic pregnancy management rather than reviewing topics you already know well.
Common UKMLA OB/GYN Exam Traps and How to Avoid Them
Trap 1: Overthinking Simple Scenarios
The trap: Choosing complex investigations or management for straightforward presentations. Example: 25-year-old with 6 weeks amenorrhoea and positive pregnancy test presenting with mild nausea. The answer is routine antenatal care, not urgent scan or beta-hCG levels. How to avoid: Ask yourself "What would I actually do in practice?" rather than "What could I potentially do?"
Trap 2: Missing Timeline Details
The trap: Not noticing gestation age, menstrual cycle timing, or investigation intervals in the question stem. Example: "Cervical screening shows low-grade dyskaryosis" — your management depends entirely on whether this is first abnormal smear or repeat abnormal smear. How to avoid: Circle key dates and timelines in the question before reading the options.
Trap 3: Confusing Similar Presentations
The trap: Mixing up conditions with overlapping symptoms. Example: Ovarian torsion vs appendicitis in pregnant women — both cause right-sided abdominal pain, but torsion is typically sudden onset with vomiting, while appendicitis has more gradual onset with fever. How to avoid: Create comparison tables for similar conditions, focusing on distinguishing features.
Trap 4: Choosing "Textbook" Over "Practical" Management
The trap: Selecting management that sounds comprehensive but isnt the most appropriate next step. Example: Woman with heavy periods — the "textbook" answer might be full hormonal workup, but the "practical" first-line answer is often Mirena IUS or tranexamic acid. How to avoid: Learn NICE and RCOG guidelines rather than general textbook approaches.
Integrating Guidelines into Clinical Practice
NICE Guidelines Priority List
Focus on these NICE guidelines that appear repeatedly in UKMLA questions:
1. Antenatal care for uncomplicated pregnancies (NG201)
2. Hypertension in pregnancy (NG133)
3. Heavy menstrual bleeding (NG88)
4. Contraception (NG142)
5. Menopause (NG23)
RCOG Green Top Guidelines
Key RCOG guidelines for UKMLA preparation:
1. Management of severe pre-eclampsia/eclampsia (GTG10A)
2. Postpartum haemorrhage (GTG52)
3. Shoulder dystocia (GTG42)
4. Management of ectopic pregnancy (GTG21)
Rather than memorising entire guidelines, focus on the decision algorithms and management pathways that translate directly into exam questions.
When you encounter a clinical scenario about heavy menstrual bleeding during practice, you immediately recall the NICE pathway: exclude structural/histological abnormalities, then offer Mirena IUS (if contraception wanted) or tranexamic acid (if contraception not wanted). This guideline-to-practice connection is exactly what separates high scorers from average performers.
Final Month UKMLA OB/GYN Strategy
Week 1: High-Yield Topic Drilling
Focus on the topics that appear most frequently:
Pre-eclampsia recognition and management
Postpartum haemorrhage protocols
Ectopic pregnancy presentations
Contraceptive eligibility
Heavy menstrual bleeding management
Spend 60% of your time on these five areas.
Week 2-3: Weak Area Identification and Improvement
Use your question bank performance data to identify specific subtopics where you consistently score <70%. Common weak areas include:
Shoulder dystocia management sequence
Emergency contraception timing
Cervical screening protocols
Menopause HRT contraindications
Week 4: Integration and Speed
Practice mixed OB/GYN questions under timed conditions. Focus on:
Quick pattern recognition (30 seconds to identify scenario type)
Efficient elimination of wrong answers
Confident decision-making without second-guessing
The goal isnt perfection — its consistent performance across all OB/GYN subtopics.
Frequently Asked Questions
How much time should I spend on OB/GYN for UKMLA preparation?
Allocate about 15% of your study time to OB/GYN, matching its representation in the exam. For a 12-week study plan, this means roughly 10-12 days focused on obstetrics and gynaecology topics.
Which OB/GYN topics are most heavily weighted in UKMLA?
Normal pregnancy and antenatal care, pre-eclampsia, postpartum haemorrhage, contraception, and heavy menstrual bleeding appear most frequently. These five topics account for approximately 60% of OB/GYN questions.
How do I memorise all the NICE and RCOG guidelines?
Dont memorise entire guidelines — focus on the decision algorithms and first-line management recommendations. Use spaced repetition to review key facts like screening intervals and contraceptive eligibility criteria.
Should I study obstetrics and gynaecology together or separately?
Study them together initially to understand the connections, then separate them for focused drilling. Obstetrics focuses more on emergency recognition, while gynaecology emphasises chronic condition management.
What percentage accuracy should I aim for in OB/GYN practice questions?
Target 75-80% accuracy consistently across all subtopics. Scores above 85% suggest youre ready; scores below 70% indicate you need more focused practice on those areas.
How do I improve at clinical scenario recognition?
Practice with vignette-style questions that mirror UKMLA format. Focus on identifying the key clinical features that point toward a specific diagnosis or management approach, rather than memorising isolated facts.
---
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for UKMLA success. Download free on Android and iOS.