Postpartum Care

On this page
🏥 The Fourth Trimester Command Center: Mastering Postpartum Care Excellence
The postpartum period transforms a woman's body through one of medicine's most dramatic physiological cascades, yet it remains one of the most vulnerable windows for maternal morbidity and mortality. You'll master the systematic assessment of involution, lochia patterns, and hemodynamic changes while building the pattern recognition skills to detect hemorrhage, infection, and hypertensive emergencies before they become critical. This lesson equips you with evidence-based protocols and clinical decision frameworks that integrate physical recovery, lactation support, and psychological screening into cohesive care that protects mothers during their most transformative-and medically complex-weeks.

📌 Remember: PUERPERAL - Physical recovery, Uterine involution, Emotional support, Rest and nutrition, Pain management, Education, Risk assessment, Activity guidance, Lactation support
Understanding postpartum care transforms routine follow-up into systematic prevention, where recognizing early warning signs prevents life-threatening complications and optimizes maternal-infant bonding outcomes.
🏥 The Fourth Trimester Command Center: Mastering Postpartum Care Excellence
🔄 Physiological Reset: The Body's Remarkable Recovery Architecture
| System | Peak Change | Recovery Timeline | Key Markers | Monitoring Frequency |
|---|---|---|---|---|
| Cardiovascular | 40% ↑ blood volume | 2-3 weeks | BP normalization | Daily first week |
| Renal | 50% ↑ GFR | 4-6 weeks | Creatinine <1.0mg/dL | Weekly |
| Respiratory | 20% ↑ tidal volume | 1-2 weeks | Normal spirometry | As needed |
| Endocrine | 10x ↑ estrogen | 6-8 weeks | Menstrual return | Monthly |
| Musculoskeletal | 2-3cm diastasis recti | 12-16 weeks | Functional strength | 6-week check |
-
Cardiovascular Recovery Cascade
- Blood volume decreases 15-20% within 48 hours through diuresis
- Cardiac output normalizes by 2 weeks in 90% of patients
- Stroke volume returns to baseline: 70mL (from 85mL)
- Heart rate stabilizes: 70-80 bpm (from 90-100 bpm)
- Peripheral resistance increases 25% as progesterone withdrawal occurs
-
Hormonal Rebalancing Architecture
- Estrogen drops 90% within 72 hours, triggering mood vulnerability
- Prolactin surges 10-20x baseline (200-400 ng/mL) if breastfeeding
- Non-breastfeeding: Returns to <25 ng/mL by 3 weeks
- Breastfeeding: Maintains 100-300 ng/mL throughout lactation
💡 Master This: Every 1°C temperature elevation above 38°C after 24 hours postpartum indicates infection until proven otherwise, requiring immediate blood cultures and broad-spectrum antibiotics within 1 hour.
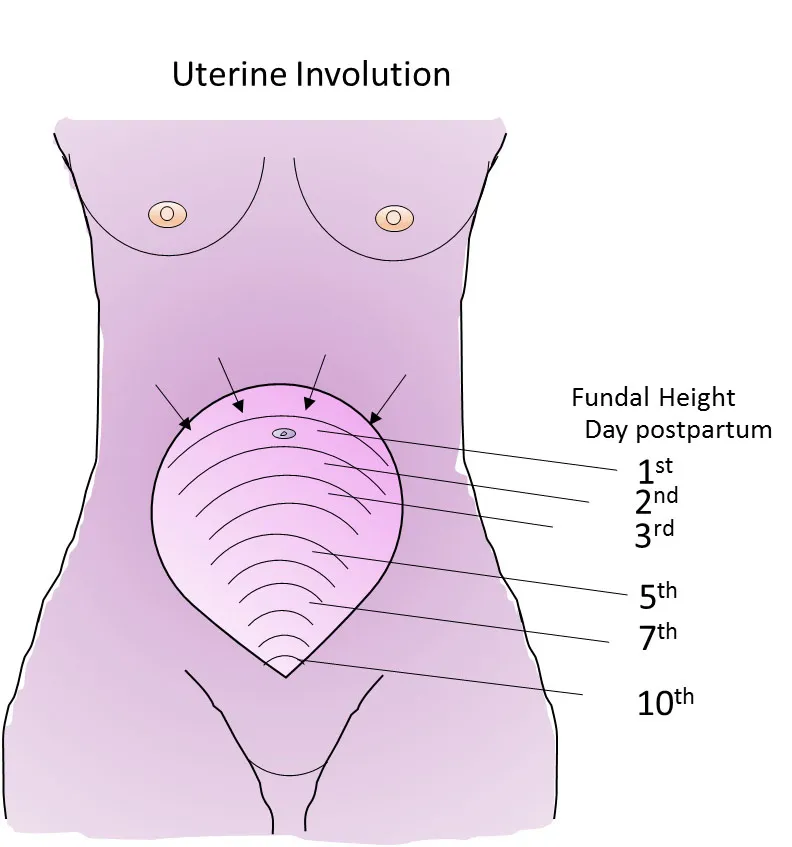
📌 Remember: LOCHIA progression - Lochia rubra (days 1-3), Orange-pink transition, Color lightening, Healthy serosa (days 4-10), Increasing alba, Alba completion (days 11-21)
Connect physiological recovery patterns through systematic assessment frameworks to identify complications requiring immediate intervention versus normal adaptation processes.
🔄 Physiological Reset: The Body's Remarkable Recovery Architecture
🎯 Clinical Assessment Matrix: Pattern Recognition for Optimal Outcomes
-
Primary Assessment Hierarchy
- Vital Signs Stability: Temperature <38°C, BP <140/90, HR 60-100 bpm
- Hypertension persists in 15% beyond 48 hours, requiring antihypertensive therapy
- Tachycardia >100 bpm suggests hemorrhage, infection, or pulmonary embolism
- Uterine Evaluation: Fundal firmness, position, tenderness assessment
- Boggy uterus indicates 90% probability of retained products or infection
- Lateral deviation suggests bladder distention or pelvic hematoma
- Vital Signs Stability: Temperature <38°C, BP <140/90, HR 60-100 bpm
-
Secondary Assessment Framework
- Lochia Characteristics: Volume <80mL/day by day 7, odor assessment
- Foul-smelling lochia has 85% sensitivity for endometritis
- Sudden increase after day 10 suggests secondary hemorrhage (2-3% incidence)
- Breast Examination: Engorgement, nipple integrity, mastitis signs
- Unilateral erythema with fever indicates mastitis in 95% of cases
- Bilateral engorgement peaks day 3-5, resolving with proper management
- Lochia Characteristics: Volume <80mL/day by day 7, odor assessment
| Assessment Domain | Normal Findings | Warning Signs | Action Threshold | Intervention Timeline |
|---|---|---|---|---|
| Uterine Involution | Firm, midline, decreasing | Boggy, enlarged, tender | Fundus >2cm above expected | <2 hours |
| Lochia Pattern | Decreasing, odorless | Increasing, malodorous | >80mL/day after day 7 | <4 hours |
| Vital Signs | Stable, afebrile | Fever, hypotension | Temp >38°C, SBP <90 | <1 hour |
| Breast Health | Soft or bilateral firm | Unilateral red, hot | Localized inflammation | <6 hours |
| Emotional State | Mood lability | Persistent depression | EPDS >12 | <24 hours |
💡 Master This: BUBBLE-HE assessment (Breasts, Uterus, Bladder, Bowel, Lochia, Episiotomy, Homan's sign, Emotional state) completed in <5 minutes identifies 95% of postpartum complications requiring intervention.
📌 Remember: DANGER signs - Dyspnea, Abdominal pain, Nausea/vomiting, Gush of blood, Elevated temperature, Red streaks on legs (thrombophlebitis indicators)
Pattern recognition mastery through structured assessment protocols enables early intervention, transforming potential complications into manageable conditions with optimal maternal outcomes.
🎯 Clinical Assessment Matrix: Pattern Recognition for Optimal Outcomes
🔬 Complication Recognition: The Early Warning System Architecture
- Hemorrhage Recognition Cascade
- Primary PPH: >500mL vaginal delivery, >1000mL cesarean within 24 hours
- Vital sign changes lag behind blood loss by 15-30 minutes
- Tachycardia >100 bpm indicates >15% blood volume loss (750-1000mL)
- Hypotension appears only after >30% loss (>1500mL)
- Secondary PPH: >500mL bleeding 24 hours to 6 weeks postpartum
- Incidence: 1-2% of deliveries, mortality 10x higher than primary
- 75% caused by retained placental fragments or endometritis
- Primary PPH: >500mL vaginal delivery, >1000mL cesarean within 24 hours
- Infection Spectrum Analysis
- Endometritis: 2-5% vaginal deliveries, 15-20% cesarean deliveries
- Classic triad: Fever >38.5°C, uterine tenderness, purulent lochia
- Polymicrobial in 80%: E.coli, Enterococcus, Bacteroides species
- Responds to ampicillin + gentamicin in 95% within 48 hours
- Wound Infections: 3-5% cesarean incisions, 1-2% episiotomies
- Risk factors: Obesity (BMI >30), diabetes, prolonged rupture >18 hours
- Cellulitis vs. abscess distinction crucial for management approach
- Endometritis: 2-5% vaginal deliveries, 15-20% cesarean deliveries
| Complication | Incidence | Peak Onset | Key Symptoms | Diagnostic Threshold |
|---|---|---|---|---|
| Endometritis | 2-20% | Days 2-5 | Fever, uterine pain | Temp >38.5°C + tenderness |
| Mastitis | 10-15% | Weeks 2-6 | Breast pain, erythema | Unilateral symptoms + fever |
| DVT/PE | 0.5-2% | Days 3-14 | Leg swelling, dyspnea | Wells score >2 |
| Depression | 10-20% | Weeks 2-8 | Mood changes, anxiety | EPDS >12 |
| Thyroiditis | 5-10% | Months 2-6 | Fatigue, palpitations | TSH abnormal |
💡 Master This: Temperature trajectory predicts infection severity - persistent fever >48 hours despite antibiotics indicates resistant organisms or abscess formation, requiring CT imaging and infectious disease consultation.
📌 Remember: SEPSIS criteria - Systemic inflammatory response, Elevated lactate >2, Persistent hypotension, Source identification, Immediate antibiotics, Supportive care
Connect early warning recognition through systematic monitoring protocols to prevent progression from minor complications to life-threatening emergencies requiring intensive interventions.
🔬 Complication Recognition: The Early Warning System Architecture
⚖️ Evidence-Based Management: Treatment Algorithms for Optimal Recovery
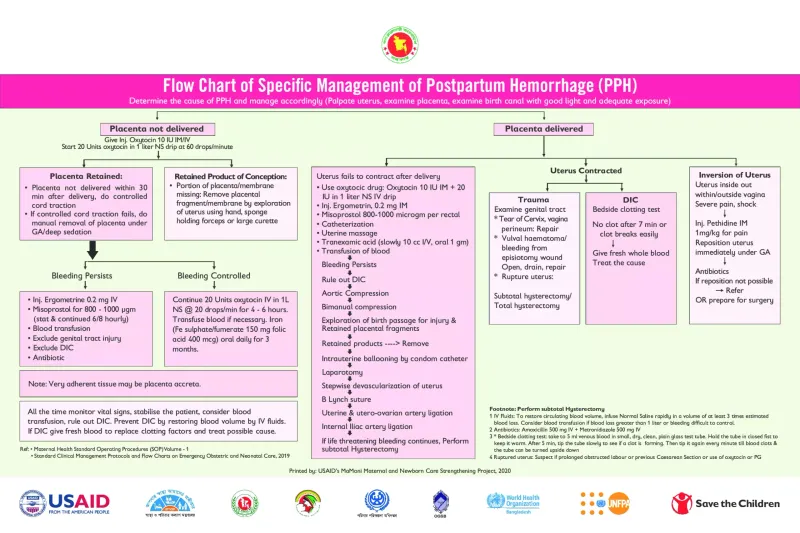
- Hemorrhage Management Protocol
- First-Line Interventions (implement within 5 minutes)
- Uterine massage + IV access (2 large-bore 16-18G)
- Oxytocin 10-40 units in 500mL NS at 125-200mL/hour
- Methylergonovine 0.2mg IM (contraindicated if HTN >140/90)
- Second-Line Therapies (if bleeding continues >15 minutes)
- Misoprostol 800-1000mcg rectally (effective in 85% of cases)
- Tranexamic acid 1g IV over 10 minutes (reduces mortality 19%)
- Balloon tamponade or compression sutures if medical therapy fails
- First-Line Interventions (implement within 5 minutes)
- Infection Treatment Frameworks
- Endometritis Standard Protocol
- Clindamycin 900mg IV q8h + Gentamicin 5mg/kg IV q24h
- Alternative: Ampicillin 2g IV q6h + Gentamicin 5mg/kg q24h
- Add Ampicillin 2g IV q6h if no improvement in 48 hours (enterococcal coverage)
- Duration: Continue 24-48 hours after fever resolution (>95% cure rate)
- Endometritis Standard Protocol
| Condition | First-Line Treatment | Success Rate | Alternative Options | Monitoring Parameters |
|---|---|---|---|---|
| PPH | Oxytocin 10-40U | 90% | Methylergonovine, Misoprostol | Vital signs q15min |
| Endometritis | Clindamycin + Gentamicin | 95% | Ampicillin-based regimen | Temperature q6h |
| Mastitis | Dicloxacillin 500mg q6h | 85% | Cephalexin, Clindamycin | Symptom resolution 48h |
| Depression | Sertraline 50mg daily | 70% | CBT, Support groups | PHQ-9 monthly |
| Thyroiditis | Propranolol 40mg BID | 80% | Methimazole if severe | TSH q6-8 weeks |
- Pain Management Optimization
- Multimodal Approach reduces opioid requirements by 50%
- Ibuprofen 600mg q6h (anti-inflammatory + analgesic)
- Acetaminophen 1000mg q6h (synergistic with NSAIDs)
- Topical anesthetics for perineal pain (lidocaine 5% gel)
- Opioid Prescribing Guidelines
- Limit to 3-7 days supply (<30 tablets total)
- Oxycodone 5-10mg q4-6h PRN for severe pain
- Educate about addiction risk (8-12% develop dependence)
- Multimodal Approach reduces opioid requirements by 50%
💡 Master This: Enhanced Recovery After Surgery (ERAS) protocols for cesarean delivery reduce length of stay by 1.5 days and complications by 30% through standardized perioperative care pathways.
📌 Remember: TREATMENT priorities - Time-sensitive interventions, Resuscitation if needed, Evidence-based protocols, Antibiotic stewardship, Thromboprophylaxis, Monitoring response, Education, Next steps planning, Team communication
Evidence-based treatment algorithms through systematic protocol implementation ensure optimal outcomes while minimizing complications and healthcare resource utilization across diverse patient populations.
⚖️ Evidence-Based Management: Treatment Algorithms for Optimal Recovery
🔗 Comprehensive Care Integration: The Multisystem Coordination Matrix
- Integrated Care Delivery Model
- Medical Optimization: Systematic organ system recovery monitoring
- Cardiovascular: BP control in 15% with persistent hypertension
- Metabolic: Diabetes screening in 50% with GDM history (A1C <7% target)
- Hematologic: Iron supplementation if Hgb <10g/dL (affects 25-30%)
- Lactation Support Integration: Evidence-based breastfeeding promotion
- 80% initiation rate achievable with proper support systems
- Exclusive breastfeeding >6 months reduces infant infections by 40%
- Maternal benefits: 50% reduction in breast cancer risk, faster weight loss
- Medical Optimization: Systematic organ system recovery monitoring
- Psychosocial Support Architecture
- Mental Health Screening: Universal depression screening protocols
- Edinburgh Postnatal Depression Scale (EPDS) at 2, 6, 12 weeks
- 10-20% develop postpartum depression requiring intervention
- 0.1-0.2% develop postpartum psychosis (psychiatric emergency)
- Social Support Assessment: Family dynamics and resource evaluation
- Partner support quality predicts 60% of maternal adjustment variance
- Socioeconomic factors influence 40% of health outcomes
- Cultural competency improves adherence by 30%
- Mental Health Screening: Universal depression screening protocols
| Integration Domain | Key Metrics | Target Outcomes | Intervention Strategies | Success Indicators |
|---|---|---|---|---|
| Physical Recovery | Weight loss 1-2 lbs/week | Pre-pregnancy weight 6 months | Nutrition counseling, Exercise | 80% achieve target |
| Mental Health | EPDS score <10 | No depression symptoms | Screening, Therapy, Medication | 90% screen negative |
| Lactation | Exclusive BF 6 months | 50% continuation rate | Support groups, Education | 60% meet goals |
| Family Planning | IPI >18 months | Planned pregnancies | Contraception counseling | 85% use effective method |
| Preventive Care | Annual screening compliance | >90% participation | Reminder systems, Access | 95% completion rate |
- Technology-Enhanced Care Delivery
- Remote Monitoring Systems: Wearable devices tracking vital signs
- Blood pressure monitoring reduces preeclampsia complications by 40%
- Activity trackers encourage gradual exercise progression
- Sleep pattern analysis identifies postpartum fatigue issues
- Mobile Health Applications: Educational content and symptom tracking
- 75% of mothers use smartphone apps for health information
- Medication reminders improve adherence by 30%
- Peer support networks reduce isolation and improve outcomes
- Remote Monitoring Systems: Wearable devices tracking vital signs
💡 Master This: Care transitions from hospital to home represent the highest risk period. Structured discharge planning with 48-72 hour follow-up contact reduces emergency department visits by 20%.
📌 Remember: INTEGRATION components - Individualized care plans, Needs assessment, Team coordination, Evidence-based protocols, Goal setting, Resource allocation, Accessibility, Technology utilization, Improvement monitoring, Outcome evaluation, Next level planning
Comprehensive care integration through systematic coordination ensures seamless transitions, optimal outcomes, and sustainable health improvements extending beyond the immediate postpartum period into long-term maternal wellness.
🔗 Comprehensive Care Integration: The Multisystem Coordination Matrix
🎯 Clinical Mastery Arsenal: Your Postpartum Care Command Center
- Essential Clinical Thresholds
- Vital Sign Red Flags: Temperature >38.4°C, SBP <90 or >160, HR >120
- Bleeding Parameters: >80mL/hour for >2 hours = immediate intervention
- Pain Scores: >7/10 despite multimodal therapy requires reassessment
- Laboratory Triggers: Hgb <7g/dL, WBC >15,000 with left shift, Platelets <100,000
📌 Remember: RAPID assessment - Respiratory rate >24, Altered mental status, Persistent hypotension, Increasing pain, Decreasing urine output (<30mL/hour)
| Clinical Scenario | Immediate Action | Time Frame | Success Metric | Escalation Trigger |
|---|---|---|---|---|
| Fever >38.5°C | Blood cultures + antibiotics | <1 hour | Defervescence 48h | Persistent fever >72h |
| Heavy bleeding | IV access + oxytocin | <5 minutes | Bleeding control | >500mL in 30 minutes |
| Severe pain | Multimodal analgesia | <15 minutes | Pain <4/10 | No improvement 2 hours |
| Mood changes | EPDS screening | <24 hours | Score <10 | Suicidal ideation |
| Breast problems | Lactation consultation | <4 hours | Symptom resolution | Abscess formation |
- Rapid Decision Framework
- ABC Priority Assessment: Airway, Breathing, Circulation stability
- Respiratory distress suggests pulmonary embolism (0.5-2% incidence)
- Hypotension indicates hemorrhage or sepsis requiring immediate resuscitation
- Altered consciousness demands glucose check and neurologic evaluation
- System-Based Evaluation: Structured approach preventing missed diagnoses
- HEENT: Visual changes (preeclampsia), neck stiffness (meningitis)
- Cardiovascular: Murmurs (peripartum cardiomyopathy), peripheral edema
- Pulmonary: Dyspnea (PE, pneumonia), chest pain (PE, pneumothorax)
- Abdominal: Uterine tenderness, surgical site evaluation
- Extremities: Calf tenderness (DVT), joint swelling (arthritis)
- ABC Priority Assessment: Airway, Breathing, Circulation stability
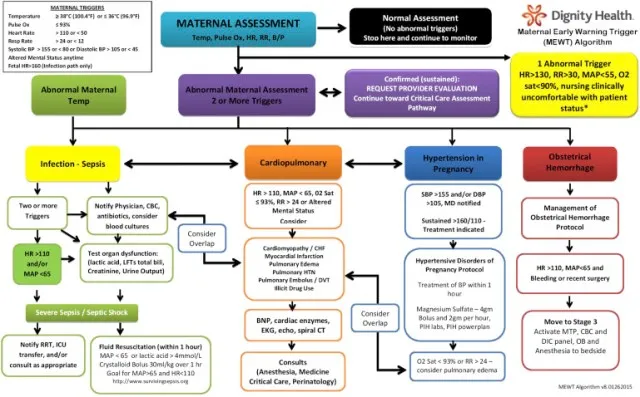
💡 Master This: Pattern Recognition Mastery - 90% of postpartum complications present with predictable symptom clusters. Master these patterns, and you achieve <2-minute diagnosis-to-treatment times.
- Clinical Excellence Commandments
- Never assume normal - 15% of complications present atypically
- Trust maternal instinct - 85% accuracy when mothers report "something's wrong"
- Document everything - Legal protection and continuity of care
- Communicate clearly - 50% of errors result from communication failures
- Follow up systematically - 30% of complications emerge after discharge
📌 Remember: EXCELLENCE principles - Evidence-based decisions, Xcellent communication, Comprehensive assessment, Early intervention, Lifelong learning, Legal documentation, Empathy and support, Never stop improving, Continuous monitoring, Emergency preparedness
Master these rapid-reference tools and systematic approaches to transform postpartum encounters into opportunities for optimal maternal health outcomes and professional excellence in women's healthcare delivery.
🎯 Clinical Mastery Arsenal: Your Postpartum Care Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















