Back
How to Study Pathology for USMLE Step 1 2026: High-Yield Topics, Mechanisms and Complete Exam Strategy
Master USMLE Step 1 pathology with mechanism-focused strategies. Complete guide to cell injury, inflammation, neoplasia, and organ-system integration for 2026.

How to Study Pathology for USMLE Step 1 2026: High-Yield Topics, Mechanisms and Complete Exam Strategy
You probably know pathology is the heaviest-weighted subject on USMLE Step 1 — 18-20% of questions. That's roughly 35-40 questions out of 200. But here's what most study guides wont tell you: Step 1 pathology questions dont test memorized disease lists. They test mechanism understanding.
When you see a vignette about a 45-year-old with chest pain, elevated troponins, and ST elevations, the question isnt "what's the diagnosis?" It's "what cellular process caused the myocyte death?" or "which inflammatory mediator triggered the vessel changes?" The exam wants you to think like a pathologist, not recite like a textbook.
This changes everything about how you should study. Instead of cramming disease names, you need to master the fundamental pathways that show up across multiple organ systems. Cell injury mechanisms that cause both myocardial infarction and acute tubular necrosis. Inflammatory cascades that drive both Crohn's disease and rheumatoid arthritis.
Why Pathology Mechanisms Beat Memorization on Step 1
Step 1 pathology questions are built around clinical vignettes that test your ability to connect symptoms to underlying cellular processes. The test writers assume you know that myocardial infarction exists — they want to know if you understand why ischemia leads to membrane damage, or how free radicals trigger cell death.
Here's the pattern: every pathology question starts with a clinical scenario, then asks about the mechanism driving that scenario. The answer choices often contain multiple correct-sounding disease names, but only one mechanistic explanation that fits the vignette.
Example thinking process for a typical question:
Vignette: "55-year-old smoker, chest pain, elevated cardiac enzymes"
Wrong approach: "This is MI, answer must be myocardial infarction"
Right approach: "Ischemia → ATP depletion → Na/K pump failure → cellular swelling → membrane damage. Which answer choice describes this pathway?"
The students who score highest on pathology focus 70% of their time on general pathology mechanisms (cell injury, inflammation, neoplasia) and 30% on organ-specific diseases. This ratio matches how Step 1 actually tests the subject.
The 5 High-Yield Pathology Clusters for Step 1 2026
1. Cell Injury and Death Mechanisms
This is your foundation. Every organ-system pathology question traces back to one of these mechanisms.
Reversible vs Irreversible Injury:
ATP depletion threshold: <5% of normal = irreversible
Membrane integrity: key distinguishing feature
Organelle changes: mitochondrial swelling (reversible) vs rupture (irreversible)
Apoptosis vs Necrosis Pathways:
Apoptosis: intrinsic (mitochondrial) and extrinsic (death receptor) pathways
Caspase cascades: initiator vs effector caspases
Necrosis types: coagulative, liquefactive, caseous, fat, fibrinoid
When each type occurs: ischemia (coagulative), infection (liquefactive), TB (caseous)
Ischemic Cascade (appears in cardiac, renal, neuro pathology):
1. Oxygen deprivation → oxidative phosphorylation stops
2. ATP levels drop → Na/K pumps fail
3. Cellular swelling → organelle damage
4. Reperfusion injury: free radical formation
5. Inflammatory response activation
Master this sequence. It explains everything from stroke pathophysiology to acute kidney injury to myocardial infarction. Oncourse's pathology lessons break down each step with interactive diagrams that connect the molecular level to clinical presentations.
2. Inflammation: Acute, Chronic, and Granulomatous
Acute Inflammation (minutes to days):
Vascular changes: vasodilation, increased permeability
Cellular events: neutrophil recruitment, margination, diapedesis
Mediators: histamine, prostaglandins, complement, cytokines
Clinical signs: rubor, tumor, calor, dolor, functio laesa
Chronic Inflammation (weeks to years):
Cellular infiltrate: lymphocytes, macrophages, plasma cells
Tissue changes: fibrosis, angiogenesis
Examples: atherosclerosis, inflammatory bowel disease, rheumatoid arthritis
Granulomatous Disease (high-yield for Step 1):
Definition: collection of epithelioid cells (activated macrophages)
Caseating: TB, histoplasmosis
Non-caseating: sarcoidosis, Crohn's disease, foreign body
Th1 response: IL-2, IFN-γ driving macrophage activation
The inflammation mechanisms you learn here apply directly to cardiovascular pathology (atherosclerosis), respiratory pathology (asthma, COPD), GI pathology (IBD), and autoimmune conditions. Spaced repetition via Synapses helps cement these cross-system connections through timed flashcard sessions that link inflammation concepts across different organ contexts.
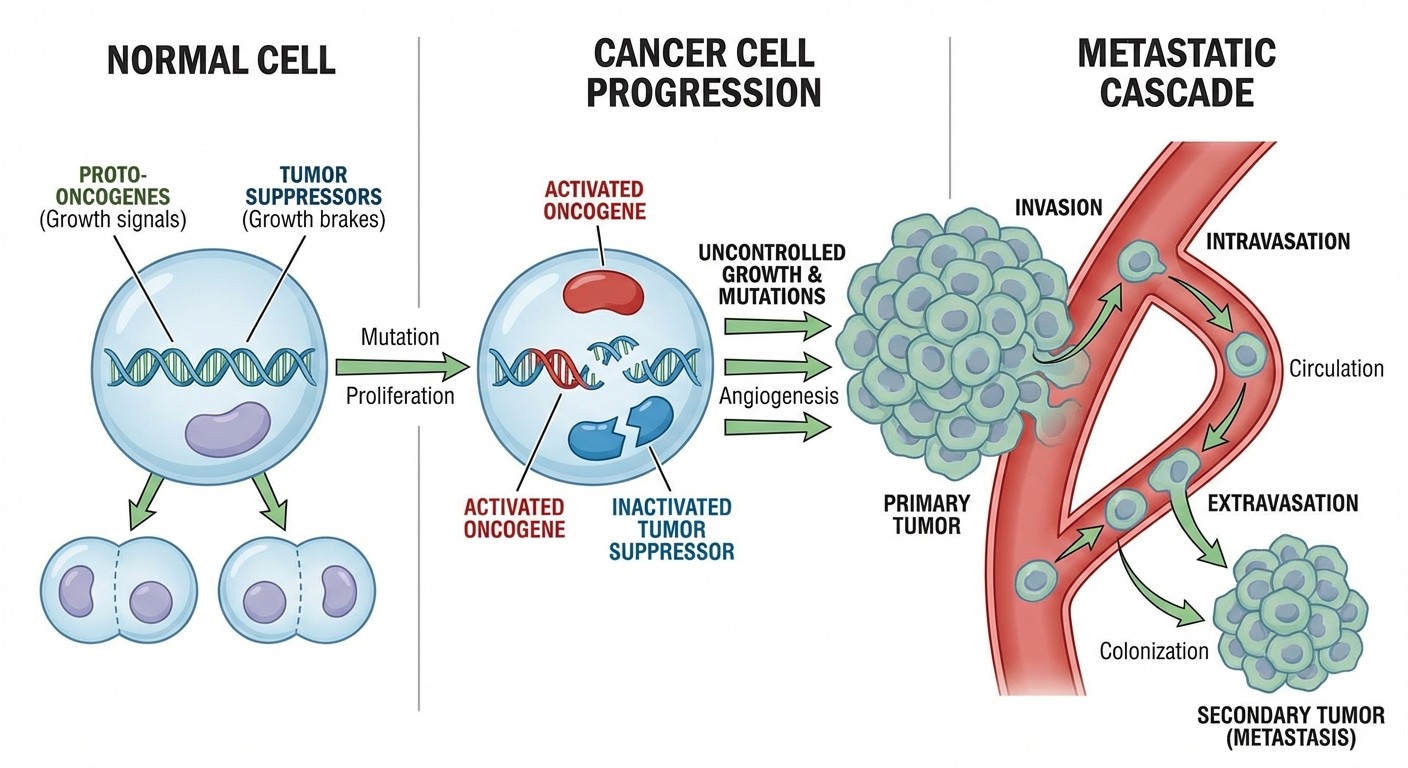
3. Neoplasia: Oncogenes, Tumor Suppressors, and Metastasis
Oncogenes vs Tumor Suppressors:
Oncogenes: gain-of-function mutations (RAS, MYC, HER2)
Tumor suppressors: loss-of-function mutations (p53, RB, APC)
Two-hit hypothesis: both alleles must be lost for tumor suppressors
p53 pathway: DNA damage → cell cycle arrest → apoptosis or repair
Carcinogenesis Steps:
1. Initiation: DNA damage (chemicals, radiation, viruses)
2. Promotion: clonal expansion of initiated cells
3. Progression: additional mutations → malignant transformation
Metastasis Mechanisms:
Local invasion: basement membrane degradation
Vascular/lymphatic spread: intravasation → extravasation
Seed and soil hypothesis: organ-specific metastasis patterns
Common metastasis sites by primary: lung → bone/brain, colon → liver, prostate → bone
These concepts integrate heavily with other subjects. Oncogenes connect to pharmacology (targeted therapies), tumor suppressors link to genetics (hereditary cancer syndromes), and metastasis pathways tie into anatomy (lymphatic drainage patterns).
4. Vascular Pathology: Atherosclerosis and Hypertensive Disease
Atherosclerosis Mechanism (shows up in cardiology, neuro, renal questions):
1. Endothelial injury: oxidized LDL, hypertension, smoking
2. Inflammatory response: macrophage infiltration
3. Foam cell formation: macrophages engulf oxidized lipids
4. Smooth muscle proliferation: growth factors from platelets
5. Plaque formation: lipid core + fibrous cap
6. Complications: rupture, thrombosis, embolism
Hypertensive End-Organ Damage:
Arterial changes: hyaline vs hyperplastic arteriopathy
Target organs: heart (LVH), brain (stroke), kidney (nephrosclerosis), retina
Malignant hypertension: acute arterial necrosis, papilledema
Aneurysm Types:
True vs false aneurysms
Atherosclerotic: abdominal aorta
Syphilitic: ascending aorta
Berry: anterior communicating artery
Dissection: aortic root, Marfan syndrome
5. Organ-System Integration: Where Pathology Meets Physiology
This is where Step 1 gets tricky. Questions that seem like pure pathology often test your ability to connect pathological processes to normal physiology and pharmacology.
Cardiac Pathology Integration:
Ischemic heart disease: relates to coronary anatomy, cardiac output physiology
Heart failure: connects to Frank-Starling mechanism, neurohormonal activation
Cardiomyopathies: ties to sarcomere proteins, calcium handling
Pulmonary Pathology Integration:
Pneumonia: links to ventilation/perfusion matching, gas exchange
COPD: connects to elastic recoil, airway resistance
Pulmonary embolism: relates to Virchow's triad, coagulation cascade
Renal Pathology Integration:
Glomerular disease: connects to filtration physiology, autoimmune mechanisms
Acute kidney injury: links to GFR regulation, electrolyte handling
Nephrotic vs nephritic: distinguishes by proteinuria mechanisms
GI Pathology Integration:
Inflammatory bowel disease: connects to immune system, barrier function
Peptic ulcer disease: links to acid secretion, H. pylori pathogenesis
Hepatitis: relates to liver function tests, metabolic pathways
The key insight: Step 1 pathology questions rarely stay within one subject. They test your ability to think across systems. When studying pathology, always ask "how does this connect to physiology?" and "what drugs would target this pathway?"
Your 4-Week Pathology Study Schedule
Week 1: General Pathology Foundation
Days 1-2: Cell injury and death mechanisms
Days 3-4: Inflammation (acute, chronic, granulomatous)
Days 5-7: Neoplasia (oncogenes, tumor suppressors, metastasis)
Focus on mechanisms, not diseases. Use active recall — explain each pathway out loud without looking at notes. Oncourse's adaptive daily plans automatically sequence these topics based on your current knowledge gaps, so you spend more time on mechanisms you haven't mastered yet.
Week 2: Vascular and Hemodynamic Disorders
Days 8-9: Atherosclerosis and ischemic disease
Days 10-11: Hypertensive pathology and end-organ damage
Days 12-14: Thrombosis, embolism, and bleeding disorders
Connect each vascular pathology to the organ systems it affects. Practice questions that integrate cardiovascular pathology with renal, neurologic, and cardiac physiology.
Week 3: Organ-System Pathology
Days 15-16: Cardiac pathology (ischemic, inflammatory, neoplastic)
Days 17-18: Pulmonary pathology (infectious, obstructive, restrictive)
Days 19-21: Renal pathology (glomerular, tubular, vascular)
This week is about connecting general mechanisms to specific diseases. For each organ system, ask: "which of the Week 1 mechanisms apply here?"
Week 4: Integration and High-Yield Review
Days 22-23: GI pathology and hepatic disease
Days 24-25: Hematologic pathology and immune disorders
Days 26-28: Cross-system integration and question practice
Focus on questions that span multiple organ systems. Practice explaining pathophysiology from cellular mechanism through clinical presentation.
Active Recall Strategies That Actually Work
Mechanism Mapping:
Instead of reading pathology passively, create mechanism maps for each major disease category. Start with the cellular process, then work outward to tissue changes, organ dysfunction, and clinical signs.
For atherosclerosis:
1. Cellular level: endothelial dysfunction, foam cell formation
2. Tissue level: plaque formation, arterial wall changes
3. Organ level: decreased perfusion, ischemia
4. Clinical level: chest pain, MI, stroke
Cross-System Connections:
When you learn a new pathological process, immediately identify where else it appears. Inflammation mechanisms show up in arthritis (joints), atherosclerosis (vessels), asthma (airways), and Crohn's disease (gut). The Synapses game helps reinforce these connections by presenting related concepts in quick succession — you might see inflammatory mediators followed by rheumatoid arthritis, then atherosclerosis, cementing the mechanistic link.
Question Stem Analysis:
For every practice question, identify:
1. What clinical scenario is described?
2. Which pathological mechanism explains this scenario?
3. What other diseases use the same mechanism?
4. How would changing one variable alter the outcome?
This approach transforms each question into multiple learning opportunities. When you miss a question about myocardial infarction, you're not just learning about MI — you're reinforcing ischemic injury mechanisms that apply to stroke, kidney injury, and intestinal ischemia.
Integrating Pathology with Other Step 1 Subjects
Pathology + Pharmacology: Every pathological process has corresponding drug targets. When studying inflammation, simultaneously review NSAIDs, corticosteroids, and immunosuppressants. When learning about neoplasia, study chemotherapy mechanisms and targeted therapies. Our USMLE Step 1 pharmacology guide shows how to link drug mechanisms to pathological processes. Pathology + Microbiology: Infectious disease pathology directly connects to microbiology. Granulomatous inflammation leads to TB, histoplasmosis, and blastomycosis. Acute inflammation connects to bacterial infections and endotoxin response. The microbiology study strategies we've outlined integrate seamlessly with inflammatory pathology concepts. Pathology + Physiology:
Every pathological process disrupts normal physiology. Heart failure pathology connects to cardiac output regulation. Renal pathology ties to GFR and electrolyte balance. Pulmonary pathology relates to ventilation/perfusion matching. Study these connections actively — dont treat them as separate subjects.
High-Yield Pathology Facts for Step 1 2026
Most Tested Cell Death Mechanisms:
Apoptosis: p53 pathway, caspase activation
Necrosis: ischemic injury, free radical damage
Autophagy: cellular stress response, protein aggregation
Inflammation Red Flags:
Granulomatous disease: always consider TB, sarcoid, Crohn's
Acute inflammation: neutrophil recruitment, complement activation
Chronic inflammation: fibrosis, lymphocyte infiltration
Neoplasia High-Yield:
p53: most commonly mutated tumor suppressor
RAS: most commonly mutated oncogene
Metastasis patterns: bone (prostate, breast), liver (GI), lung (everywhere)
Vascular Pathology Must-Know:
Atherosclerosis: oxidized LDL, foam cells, plaque rupture
Hypertension: arteriolar changes, end-organ damage
Thrombosis: Virchow's triad application
Using Technology to Master Pathology Mechanisms
Adaptive Learning for Efficiency:
Traditional study approaches treat all pathology topics equally. But Step 1 doesnt. Some mechanisms show up in 15% of pathology questions, others in 1%. Oncourse's adaptive daily plans track which pathology topics you've mastered and which need reinforcement, automatically adjusting your study load based on Step 1 question frequency and your personal knowledge gaps.
Visual Learning for Histology: 5-10% of Step 1 questions include histological images or gross pathology slides. You cant afford to skip visual pattern recognition. Image Rush delivers timed histology identification practice — you'll see slides of acute inflammation, chronic inflammation, neoplasia, and organ-specific pathology with immediate feedback on identifying features. AI-Powered Explanations for Deep Learning:
When you miss a pathology question, the explanation matters more than the score. Every pathology question in Oncourse includes AI explanations that connect the clinical vignette to the underlying mechanism. Instead of just telling you the right answer, the AI walks through why that mechanism explains the presented symptoms — turning every wrong answer into a learning opportunity.
Spaced Repetition for Long-Term Retention: Pathology involves hundreds of mechanisms, and you need to retain all of them through Step 1 and beyond. The traditional cramming approach leads to rapid forgetting. Spaced repetition through Synapses presents pathology concepts at optimal intervals — you'll review inflammation mediators just as you're about to forget them, cementing long-term retention without wasted effort.
Common Pathology Study Mistakes to Avoid
Mistake 1: Disease List Memorization
Many students try to memorize every disease mentioned in standard Step 1 resources. This approach fails because Step 1 tests mechanisms, not disease names. Instead of memorizing that "sarcoidosis causes granulomatous inflammation," focus on understanding why Th1 responses lead to epithelioid cell formation and how this mechanism distinguishes granulomatous from other inflammatory patterns.
Mistake 2: Ignoring Cross-System Integration
Studying cardiac pathology separately from renal pathology misses the point. Hypertensive heart disease and nephrosclerosis share identical mechanisms. Inflammatory bowel disease and rheumatoid arthritis involve similar autoimmune pathways. Step 1 questions often test your ability to recognize these mechanistic connections across organ systems.
Mistake 3: Passive Reading Over Active Recall
Reading pathology textbooks feels productive but doesnt translate to Step 1 performance. Active recall — explaining mechanisms without looking at notes, drawing pathways from memory, teaching concepts to study partners — creates the neural patterns needed for exam success.
Mistake 4: Skipping Histology Practice
"I'll just focus on clinical vignettes" is a costly mistake. Step 1 includes histological images in pathology questions, and visual pattern recognition requires specific practice. You need to identify acute vs chronic inflammation on slides, recognize neoplastic changes, and distinguish inflammatory from neoplastic processes based on cellular morphology.
Pathology Study Resources and Integration
Core Resource Integration:
Standard Step 1 resources organize pathology into general principles followed by organ-system coverage. This structure works well if you maintain the mechanism focus throughout. When reading about specific diseases, always connect back to the general pathology principles that explain them.
Question Bank Strategy:
Use pathology questions to reinforce mechanisms, not just test knowledge. For each question:
1. Identify the underlying pathological mechanism before looking at answer choices
2. Predict what the answer should explain based on that mechanism
3. After answering, explain why the other choices dont fit the mechanism
4. Identify other diseases that use the same mechanism
Laboratory Integration:
Pathology questions often include laboratory values that reflect underlying mechanisms. Elevated troponins indicate myocyte death. Increased ESR suggests inflammatory processes. Abnormal tumor markers reflect neoplastic activity. Connect laboratory findings to pathological processes, not just diseases.
Frequently Asked Questions
How much time should I spend on pathology vs other Step 1 subjects?
Pathology represents 18-20% of Step 1 questions, so it should get proportional study time — roughly 18-20% of your total preparation. In a typical 12-week Step 1 study period, this translates to 2-2.5 weeks focused primarily on pathology, plus ongoing integration with other subjects.
Should I memorize all the pathology tables in standard resources?
No. Focus on understanding mechanisms rather than memorizing isolated facts. The tables are useful for organizing information, but Step 1 questions test your ability to apply mechanisms to new scenarios, not recall tabulated information.
How do I balance general pathology vs organ-system pathology?
Spend 70% of your pathology study time on general mechanisms (cell injury, inflammation, neoplasia, vascular pathology) and 30% on organ-specific applications. This ratio matches Step 1 question distribution and ensures you understand the fundamental processes that apply across multiple systems.
What's the best way to review pathology in the final weeks before Step 1?
Focus on high-yield mechanisms and cross-system integration. Review cell injury pathways, inflammatory mediators, oncogene/tumor suppressor functions, and atherosclerosis mechanisms. Practice questions that span multiple organ systems and require mechanistic thinking.
How do I connect pathology to clinical scenarios on Step 1?
Always start with the clinical presentation, identify the likely underlying pathological process, then select the answer choice that best explains that mechanism. Dont jump to diagnosis first — focus on the pathophysiology that explains the clinical findings.
Should I study pathology separately from other subjects?
No. Pathology integrates heavily with physiology, pharmacology, and microbiology. Study these connections actively. When learning about inflammatory pathology, simultaneously review anti-inflammatory drugs. When studying neoplasia, connect to cancer pharmacology and genetics.
Pathology forms the foundation for understanding disease mechanisms across all medical specialties. Master these principles now, and you'll have a framework that serves you throughout medical school and beyond. The mechanisms you learn for Step 1 pathology apply directly to clinical reasoning in residency and practice.
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for USMLE Step 1. Download free on Android and iOS.