Back
How to Study OB-GYN for NEET PG 2026: High-Yield Topics, Clinical Cases & Exam Checklist
Master OB-GYN for NEET PG 2026 with this complete study guide. High-yield obstetrics & gynaecology topics, clinical case patterns, image interpretation skills, and exam-day checklist for maximum marks.

How to Study OB-GYN for NEET PG 2026: High-Yield Topics, Clinical Cases & Exam Checklist
You are sitting with your NEET PG prep and OB-GYN feels overwhelming. 47 questions from Obstetrics and Gynaecology — that's 23% of your entire paper. Every mark counts when the cutoff hovers around 600+.
Here's what most students get wrong: they treat OBG like two separate subjects. Fatal mistake. The exam weaves obstetrics cases with gynaec pathophysiology. A single question can test your knowledge of ovarian hormones, pregnancy complications, AND surgical management.
NEET PG 2026 pattern analysis shows 68% of OBG questions are now clinical vignettes with images. Gone are the days of pure factual recall. You need pattern recognition for CTG traces, ultrasound findings, and operative procedures.
This guide breaks down the highest-yield OBG topics, exactly how clinical cases are structured, and a bulletproof exam checklist. No fluff — just what gets you marks.
Understanding OB-GYN Weight in NEET PG 2026
OB-GYN carries 47 questions out of 200 total — the third highest after Medicine and Surgery. The distribution breaks down as:
Component | Questions | Percentage |
|---|---|---|
Obstetrics | 25-27 | 13% |
Gynaecology | 18-20 | 9% |
Reproductive Medicine | 2-3 | 1% |
The scoring pattern is brutal: 4 marks for correct, -1 for wrong. With this weightage, dropping below 75% accuracy in OBG can derail your entire rank.
Recent years show a clear shift toward image-based questions (CTG interpretation, ultrasound findings, operative images) and multi-step clinical reasoning. Pure memory-based questions now make up less than 32% of OBG paper.
High-Yield Obstetrics Topics for NEET PG 2026
Antenatal Care & Investigations (8-9 questions)
Must-know topics:
Triple test and quad test interpretation
Amniocentesis indications and timing
USG findings in different trimesters
Antenatal steroid administration protocols
Management of Rh incompatibility
Pattern recognition: Questions often present a case with specific gestational age and ask about the most appropriate investigation. Master the timing: NT scan (11-13 weeks), anomaly scan (18-20 weeks), growth scan (28-32 weeks).
The antenatal care lessons cover investigation timelines with clinical correlations — exactly what NEET PG tests.
High-Risk Pregnancy (7-8 questions)
Core conditions:
Gestational diabetes management protocols
Preeclampsia classification and management
Antepartum hemorrhage (placenta previa vs abruption)
IUGR vs SGA differentiation
Multiple pregnancy complications
Clinical case structure: Expect vitals, lab values, and USG findings. Questions test your ability to differentiate between similar conditions and choose immediate vs long-term management.
For gestational diabetes, memorize the diagnostic criteria: fasting ≥92 mg/dL, 1-hour ≥180 mg/dL, 2-hour ≥153 mg/dL (IADPSG criteria). Oncourse's OBG question bank includes clinical vignettes that mirror actual exam patterns, with adaptive routing that focuses extra practice on conditions you find challenging.
Labor & Delivery (6-7 questions)
High-yield areas:
CTG interpretation (normal vs pathological)
Stages of labor and partogram plotting
Operative obstetrics (forceps, vacuum, cesarean indications)
Shoulder dystocia management
Postpartum hemorrhage protocols
Image-based focus: CTG traces appear in 60% of labor questions. Learn the patterns: baseline 110-160, variability 5-25, no decelerations = normal. Variable decelerations = cord compression, late decelerations = placental insufficiency.
Practice labor and delivery MCQs that include actual CTG strips — visual pattern recognition is crucial for exam success.
Medical Disorders in Pregnancy (4-5 questions)
Key topics:
Cardiac disease in pregnancy (rheumatic, congenital)
Diabetes in pregnancy (pre-gestational vs gestational)
Thyroid disorders and pregnancy
Anemia in pregnancy types and management
Infections in pregnancy (TORCH, hepatitis)
Remember: pregnancy physiology changes drug dosing and normal lab values. Example: hemoglobin <11 g/dL in pregnancy = anemia (vs <12 g/dL in non-pregnant women).
High-Yield Gynaecology Topics for NEET PG 2026
Menstrual Disorders (6-7 questions)
Essential conditions:
PCOS diagnosis and management
DUB classification and treatment
Amenorrhea workup (primary vs secondary)
Endometriosis clinical presentation
Fibroids management options
Diagnostic criteria mastery: PCOS needs 2 of 3: oligo-ovulation, clinical/biochemical hyperandrogenism, polycystic ovaries on USG. Rotterdam criteria is the gold standard.
The menstrual disorders section breaks down each condition with flowcharts — perfect for quick revision during exam prep.
Gynecologic Oncology (5-6 questions)
Must-cover cancers:
Cervical cancer staging and screening
Ovarian cancer markers and presentation
Endometrial cancer risk factors
Vulvar and vaginal cancers
Gestational trophoblastic disease
Screening protocols: Pap smear every 3 years (21-65 years), HPV co-testing every 5 years (30-65 years). Know the exceptions and special populations.
Beta-hCG levels in GTD: complete mole >100,000 mIU/mL, partial mole <100,000 mIU/mL. These numbers appear repeatedly in NEET PG questions.
Infertility & Reproductive Medicine (4-5 questions)
Core concepts:
Male vs female factor evaluation
Ovulation induction protocols
IVF indications and success rates
Recurrent pregnancy loss workup
Contraception methods and mechanisms
Investigation sequence: Start with semen analysis, ovulation confirmation, tubal patency testing. Questions often test the logical sequence rather than isolated facts.
Use fertility and infertility flashcards for quick recall of investigation timelines and success rate statistics that appear in MCQs.
Urogynecology & Pelvic Floor (3-4 questions)
Key areas:
Urinary incontinence types and management
Pelvic organ prolapse staging
Fistula repair techniques
Pelvic inflammatory disease
Chronic pelvic pain evaluation
Clinical differentiation: Stress incontinence = urine loss with coughing/sneezing, urge incontinence = strong sudden urge, mixed = combination. Treatment varies significantly.
Clinical Case Question Patterns in OB-GYN
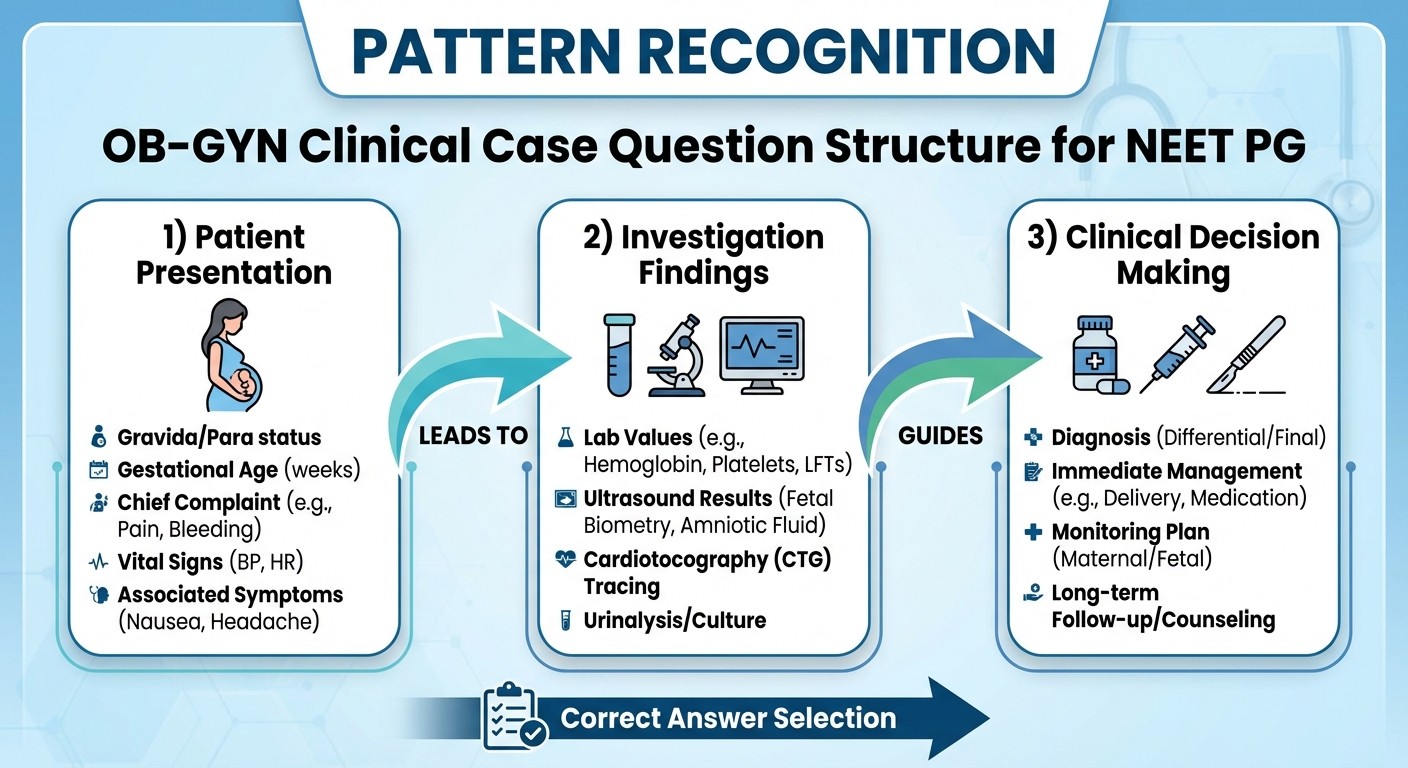
Scenario-Based Questions (65% of OBG paper)
NEET PG 2026 heavily favors clinical vignettes over direct facts. Typical structure:
Case presentation: Age, presenting symptoms, examination findings, investigation results Question stem: "What is the most appropriate next step?" or "What is the most likely diagnosis?"
Example pattern:
"22-year-old female, married for 2 years, presents with amenorrhea for 4 months, weight gain, and hirsutism. On examination: BMI 28, acne on face, male pattern hair growth. USG shows bilateral enlarged ovaries with multiple small cysts. Which investigation confirms the diagnosis?"
Answer approach:
1. Identify the clinical syndrome (PCOS)
2. Recall diagnostic criteria
3. Choose the confirmatory test (hormonal assays)
Oncourse's adaptive question format mimics this exact pattern, building familiarity with multi-step reasoning that NEET PG demands.
Image-Based Questions (35% of OBG paper)
Common image types:
CTG traces (normal vs pathological patterns)
Ultrasound findings (fetal anatomy, placental location)
Histopathology slides (cervical dysplasia, ovarian tumors)
Operative photographs (surgical procedures)
Radiological images (CT/MRI findings)
Success strategy: Practice image interpretation daily. Start with obvious abnormalities, then progress to subtle findings. The performance dashboard helps track accuracy across image-based vs text-based questions, ensuring balanced preparation.
Study Strategy: Building OB-GYN Mastery
Phase 1: Concept Foundation (Weeks 1-4)
Daily schedule:
3 hours theory (textbook + video lectures)
1 hour MCQ practice (30-40 questions)
30 minutes flashcard revision
Topic sequence: Start with normal physiology, then pathology, finally management. Obstetrics and gynecology concepts overlap significantly — studying them together builds stronger connections.
Review basic OBG concepts systematically before jumping into pathological conditions. Foundation gaps show up as wrong answers later.
Phase 2: Clinical Application (Weeks 5-8)
Focus shift: Move from theory to case-based learning. Spend 60% time on MCQs, 40% on concept reinforcement. Pattern recognition training: Practice 50-70 OBG questions daily, focusing on clinical vignettes. The adaptive daily plan automatically adjusts OBG question distribution based on your accuracy — if you drop below 70% in any OBG subtopic, the system increases practice volume for that area. Common mistake: Students memorize individual facts without understanding clinical context. NEET PG tests application, not recall.
Phase 3: Integration & Speed (Weeks 9-12)
Mock test phase: Complete subject-wise OBG tests (47 questions in 60 minutes) twice weekly. Aim for 80%+ accuracy with 1.3 minutes per question. Weakness targeting: Use performance analytics to identify your weakest OBG subsections. Obstetrics accuracy below 75% needs immediate attention — it carries more weightage than gynaecology. Final month: Transition to mixed tests combining OBG with other subjects. Real exam conditions include fatigue and context switching between specialties.
NEET PG OB-GYN Exam Day Checklist
Pre-Exam Preparation
Day before exam:
[ ] Review high-yield formulas (Bishop score, gestational age calculations)
[ ] Practice 20 image-based OBG questions
[ ] Revise emergency protocols (postpartum hemorrhage, eclampsia management)
[ ] Check knowledge gaps using OBG flashcards
Morning of exam:
[ ] Light breakfast (avoid heavy meals that cause drowsiness)
[ ] Review contraindication lists (medications in pregnancy)
[ ] Quick scan of normal values (hemoglobin, blood pressure ranges)
During OB-GYN Questions
Time management:
[ ] Allocate 1.2 minutes per OBG question (56 minutes total for 47 questions)
[ ] Mark image-based questions for review if taking >2 minutes
[ ] Don't spend >3 minutes on any single OBG question
Question approach:
[ ] Read stem completely before looking at options
[ ] Identify key clinical features first
[ ] Eliminate obviously wrong options
[ ] Choose best answer among remaining (avoid overthinking)
Red flags to watch:
[ ] Absolute contraindications vs relative contraindications
[ ] Emergency vs elective management protocols
[ ] Medication dosing in pregnancy vs non-pregnant state
Post-Question Review Strategy
For flagged questions:
[ ] Re-read clinical scenario with fresh perspective
[ ] Focus on missed clinical clues
[ ] Apply exclusion criteria systematically
[ ] Trust your clinical reasoning over memorized facts
Common traps:
[ ] Questions with multiple correct answers (choose MOST appropriate)
[ ] Treatment protocols that differ in pregnancy
[ ] Normal variants vs pathological findings
Memory Techniques for High-Yield OB-GYN Facts
Mnemonics for Critical Information
TORCH infections: Toxoplasma, Other (syphilis, VZV, parvovirus), Rubella, CMV, Herpes HELLP syndrome: Hemolysis, Elevated Liver enzymes, Low Platelets 5 Ts of postpartum hemorrhage: Tone (uterine atony), Trauma, Tissue, Thrombin, Traction Bishop Score components (CEDOW): Cervical position, Effacement, Dilatation, Oscillation (consistency), fetal Station
These mnemonics appear frequently in case-based questions where you need quick recall under time pressure.
Visual Memory for Procedures
Forceps vs vacuum delivery:
Forceps: metal instruments, specific indications, higher skill requirement
Vacuum: suction cup, easier application, lower maternal trauma
USG findings by trimester:
1st trimester: confirm viability, rule out ectopic
2nd trimester: anomaly scan, gender determination
3rd trimester: growth assessment, placental location
Create mental images linking symptoms to conditions. Example: PCOS = "police officer" (male characteristics) with "multiple small arrests" (ovarian cysts).
Advanced Preparation: Image Interpretation Skills
CTG Pattern Recognition
Normal CTG features:
Baseline: 110-160 bpm
Variability: 5-25 bpm
Accelerations: present with fetal movement
Decelerations: absent
Pathological patterns:
Variable decelerations: cord compression (U-shaped)
Late decelerations: placental insufficiency (gradual fall)
Prolonged bradycardia: fetal hypoxia (>3 minutes <100 bpm)
Management decisions: Normal CTG = continue monitoring, pathological = consider intervention (cesarean/instrumental delivery).
Practice CTG interpretation using obstetric emergency questions that include actual monitor traces from clinical scenarios.
Ultrasound Findings Interpretation
Key measurements by gestational age:
CRL (Crown-rump length): 6-14 weeks
BPD (Biparietal diameter): >14 weeks
FL (Femur length): growth assessment
AC (Abdominal circumference): fetal weight estimation
Pathological findings:
Nuchal thickening >3mm: chromosomal abnormalities
Oligohydramnios: AFI <5cm or MVP <2cm
Polyhydramnios: AFI >25cm or MVP >8cm
Clinical correlation: Link USG findings to maternal conditions. Diabetes = polyhydramnios, IUGR = oligohydramnios, neural tube defects = polyhydramnios.
Frequently Asked Questions
How many OB-GYN questions appear in NEET PG 2026?
OB-GYN contributes 47 questions out of 200 total questions in NEET PG 2026. This breaks down to approximately 25-27 questions from Obstetrics and 18-20 questions from Gynaecology, with 2-3 questions from Reproductive Medicine.
What's the best order to study OBG topics for NEET PG?
Start with normal physiology (menstrual cycle, pregnancy physiology), then move to common pathological conditions (PCOS, preeclampsia), followed by emergency management (postpartum hemorrhage, eclampsia), and finish with oncology and advanced reproductive techniques. This sequence builds logical connections between related concepts.
How important are image-based questions in OBG NEET PG?
Image-based questions now constitute 35% of OBG paper in NEET PG 2026. Focus heavily on CTG interpretation, ultrasound findings, and histopathology slides. Practice visual pattern recognition daily using clinical case images.
What's the minimum accuracy needed in OBG to score 600+ in NEET PG?
Target 80%+ accuracy in OBG questions to comfortably cross 600+ overall score. With OBG carrying 47 questions (188 marks), dropping below 75% accuracy can significantly impact your rank. Each wrong answer costs 5 marks (4 positive + 1 negative).
Which OBG textbook is best for NEET PG 2026 preparation?
DC Dutta remains the gold standard for comprehensive coverage. For quick revision, use Sakshi Arora Hans or Novak's Gynecology. However, focus primarily on MCQ practice and clinical cases rather than extensive textbook reading in the final months.
How do I improve CTG interpretation skills for NEET PG?
Practice daily with actual CTG strips, not just theoretical descriptions. Learn the 4 key features: baseline rate, variability, accelerations, and decelerations. Master the management decisions based on CTG patterns — normal vs pathological vs suspicious categories have different protocols.
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for NEET PG. Download free on Android and iOS.