Prenatal Care

On this page
🏥 Prenatal Care: The Nine-Month Medical Marathon
Prenatal care transforms nine months of profound physiological change into a systematic surveillance operation where pattern recognition saves lives. You'll master the architecture of routine visits, learn to discriminate normal adaptations from pathologic deviations, and build the clinical judgment to stratify risk and trigger interventions at precisely the right moments. This isn't just scheduling appointments-it's orchestrating a multidisciplinary response system that catches complications before they cascade, turning uncertainty into actionable clinical decisions that protect two patients simultaneously.
🏥 Prenatal Care: The Nine-Month Medical Marathon
🎯 Foundation Blueprint: The Prenatal Care Architecture
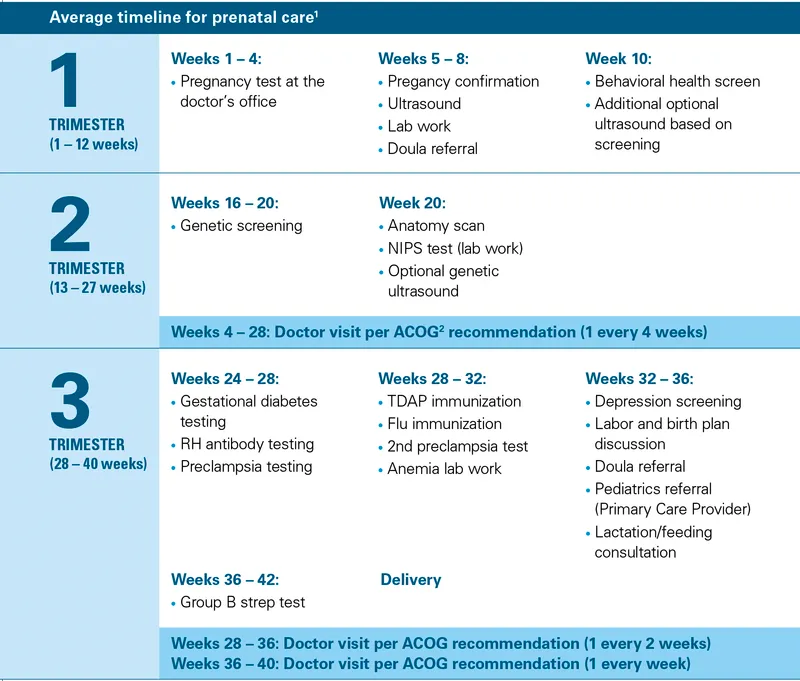
The foundation rests on four core pillars that guide every clinical decision:
-
Risk Stratification Framework
- Initial comprehensive assessment within 10 weeks gestation
- Continuous risk reassessment at every visit
- High-risk identification triggers specialized protocols
- Maternal age >35 years or <18 years
- BMI >30 kg/m² or <18.5 kg/m²
- Previous pregnancy complications with recurrence risk >20%
- Chronic medical conditions affecting >15% of pregnancies
-
Surveillance Schedule Architecture
- Monthly visits until 28 weeks (7 visits)
- Bi-weekly visits from 28-36 weeks (4 visits)
- Weekly visits from 36 weeks to delivery (4+ visits)
- Minimum 15 visits for optimal outcomes
- Each visit includes 8 mandatory assessments
- Laboratory screening at 3 critical timepoints
- Ultrasound evaluation at 4 standardized intervals
📌 Remember: CARE Framework - Continuous monitoring, Assessment protocols, Risk stratification, Evidence-based interventions
⭐ Clinical Pearl: Pregnancies with <4 prenatal visits have 3x higher risk of low birth weight and 2.5x higher risk of preterm delivery compared to adequate care recipients.
| Visit Timing | Gestational Age | Key Assessments | Laboratory Tests | Ultrasound | Risk Factors |
|---|---|---|---|---|---|
| Initial | 6-10 weeks | Complete H&P, baseline vitals | CBC, blood type, STI screen | Dating scan | Medical/surgical history |
| Early | 11-14 weeks | Weight gain, BP monitoring | First trimester screen | NT measurement | Genetic risk assessment |
| Mid | 18-22 weeks | Fundal height, fetal movement | MSAFP, glucose challenge | Anatomy scan | Structural anomalies |
| Late | 32-36 weeks | Cervical assessment, presentation | GBS culture, repeat CBC | Growth assessment | Preterm labor risk |
| Term | 37+ weeks | Cervical ripening, fetal status | Coagulation studies | Biophysical profile | Delivery planning |
- Standard Assessment Protocol (15-minute visits)
- Maternal vital signs with specific thresholds
- Fetal heart rate assessment (110-160 bpm normal range)
- Fundal height measurement (±3 cm from gestational age)
- Symptom review using standardized questionnaires
- Weight gain tracking (25-35 lbs normal BMI)
- Blood pressure monitoring (<140/90 mmHg threshold)
- Proteinuria screening (<300 mg/24h normal)
- Glucose surveillance (<140 mg/dL 1-hour GTT)
💡 Master This: Every prenatal visit follows the SOAP-R format - Subjective complaints, Objective measurements, Assessment of risks, Plan modifications, Return scheduling with specific parameters.
Understanding this architectural framework transforms routine prenatal care into precision medicine, where every measurement connects to evidence-based thresholds and clinical decision points that optimize outcomes for both mother and baby.
🎯 Foundation Blueprint: The Prenatal Care Architecture
🔬 Physiological Surveillance: The Body's Adaptation Monitoring System
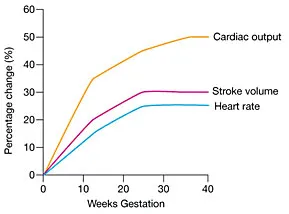
The cardiovascular transformation dominates clinical monitoring priorities:
-
Blood Volume Expansion Architecture
- Plasma volume increases by 45-50% (1,200-1,500 mL)
- Red cell mass increases by 25-30% (300-400 mL)
- Physiological anemia develops when expansion rates differ
- Hemoglobin threshold: 11.0 g/dL first trimester, 10.5 g/dL second trimester
- Hematocrit nadir: 32-34% at 28-32 weeks gestation
- Iron requirements increase to 27 mg daily (vs 18 mg non-pregnant)
-
Cardiac Output Optimization
- Increases by 30-50% above baseline (4-6 L/min to 6-8 L/min)
- Heart rate increases by 15-20 bpm (10-15% above baseline)
- Stroke volume increases by 25-30% until 20 weeks, then plateaus
- Peak cardiac output occurs at 28-32 weeks gestation
- Supine hypotensive syndrome affects 8-10% of pregnancies
- Left lateral positioning improves venous return by 25-30%
📌 Remember: HEART Changes - Heart rate up, Expansion of blood volume, Anemia physiological, Return impaired supine, Thresholds adjusted
Respiratory system adaptations require specific monitoring parameters:
- Ventilatory Changes
- Tidal volume increases by 30-40% (500 mL to 700 mL)
- Minute ventilation increases by 40-50% due to progesterone
- Functional residual capacity decreases by 20% from diaphragm elevation
- Respiratory rate remains unchanged (12-16 breaths/min)
- Oxygen consumption increases by 20-25% above baseline
- Arterial PCO₂ decreases to 27-32 mmHg (respiratory alkalosis)
| System | Parameter | Non-Pregnant | Pregnant | Change | Clinical Significance |
|---|---|---|---|---|---|
| Cardiovascular | Cardiac Output | 4-6 L/min | 6-8 L/min | ↑30-50% | Monitor for heart failure |
| Cardiovascular | Blood Volume | 4-5 L | 5.5-6.5 L | ↑45% | Physiological anemia |
| Respiratory | Tidal Volume | 500 mL | 700 mL | ↑40% | Dyspnea of pregnancy |
| Renal | GFR | 120 mL/min | 150-180 mL/min | ↑50% | Creatinine <0.8 mg/dL |
| Endocrine | Insulin Resistance | Baseline | 2-3x increase | ↑200% | Gestational diabetes risk |
Renal and metabolic surveillance focuses on adaptation thresholds:
- Glomerular Filtration Enhancement
- GFR increases by 40-50% (150-180 mL/min vs 120 mL/min)
- Serum creatinine decreases to 0.4-0.8 mg/dL (vs 0.6-1.2 mg/dL)
- Blood urea nitrogen decreases to 8-12 mg/dL (vs 10-20 mg/dL)
- Creatinine >1.0 mg/dL suggests renal impairment in pregnancy
- Proteinuria >300 mg/24h indicates pathological process
- Glycosuria occurs in 15% of normal pregnancies
💡 Master This: Normal pregnancy creates a hyperdynamic state with increased cardiac output, expanded blood volume, and enhanced renal function - deviations from these patterns signal pathological processes requiring immediate evaluation and intervention.
These physiological adaptations establish the baseline parameters against which all prenatal assessments are measured, transforming routine monitoring into precision surveillance of maternal-fetal wellbeing.
🔬 Physiological Surveillance: The Body's Adaptation Monitoring System
🎯 Clinical Assessment Mastery: The Pattern Recognition Framework
The Primary Assessment Matrix guides every clinical encounter:
-
Vital Sign Pattern Recognition
- Blood Pressure Thresholds: Systolic ≥140 or Diastolic ≥90 mmHg
- Single elevated reading: Repeat in 15 minutes with proper technique
- Persistent elevation: 24-hour monitoring or home BP tracking
- Severe hypertension: ≥160/110 mmHg requires immediate evaluation
- MAP increase >15 mmHg from baseline predicts preeclampsia risk
- Weight Gain Surveillance: Total gain 25-35 lbs for normal BMI
- Excessive gain: >2 lbs/week after 20 weeks gestation
- Inadequate gain: <1 lb/month in second/third trimester
- Sudden gain: >5 lbs/week suggests fluid retention
- Blood Pressure Thresholds: Systolic ≥140 or Diastolic ≥90 mmHg
-
Fetal Assessment Integration
- Fundal Height Correlation: ±3 cm from gestational age in weeks
- Lagging growth: >3 cm below expected suggests IUGR
- Excessive size: >3 cm above suggests macrosomia or polyhydramnios
- Static measurements: No change over 4 weeks requires ultrasound evaluation
- Fetal Heart Rate Patterns: 110-160 bpm normal range
- Bradycardia: <110 bpm may indicate fetal hypoxia or heart block
- Tachycardia: >160 bpm suggests maternal fever, fetal anemia, or arrhythmia
- Absent fetal heart tones: Requires immediate ultrasound confirmation
- Fundal Height Correlation: ±3 cm from gestational age in weeks
📌 Remember: VITAL Assessment - Vitals trending, Interval growth, Timing of changes, Associated symptoms, Laboratory correlation
Symptom-Based Pattern Recognition enables early intervention:
- High-Risk Symptom Clusters
- Preeclampsia Triad: Headache + Visual changes + Epigastric pain
- Severe headache: Unrelieved by acetaminophen, frontal/occipital
- Visual disturbances: Scotomata, photophobia, diplopia
- Right upper quadrant pain: HELLP syndrome consideration
- Hyperreflexia with clonus: CNS irritability marker
- Preterm Labor Indicators: Regular contractions + Cervical change
- Contractions: >6 per hour before 37 weeks
- Pelvic pressure: Constant rather than intermittent
- Low back pain: Rhythmic and increasing intensity
- Vaginal discharge change: Mucus plug loss or fluid leakage
- Preeclampsia Triad: Headache + Visual changes + Epigastric pain
| Symptom Complex | Key Features | Timing | Immediate Action | Follow-up Required |
|---|---|---|---|---|
| Preeclampsia | BP ≥140/90 + Proteinuria | >20 weeks | Lab workup + Monitoring | Weekly visits |
| Preterm Labor | Contractions + Cervical change | 20-37 weeks | Cervical exam + Monitoring | Bed rest + Steroids |
| Placental Abruption | Bleeding + Pain + Rigid uterus | >20 weeks | Immediate delivery | Blood bank + OR |
| PROM | Fluid leak + Positive tests | Any gestation | Sterile exam + Culture | Antibiotic prophylaxis |
| IUGR | Fundal height lag + Decreased movement | >24 weeks | Ultrasound + Doppler | Serial monitoring |
Laboratory Integration Patterns enhance clinical decision-making:
-
Anemia Assessment Framework
- First trimester: Hemoglobin <11.0 g/dL indicates anemia
- Second/third trimester: Hemoglobin <10.5 g/dL requires intervention
- Iron deficiency markers: Ferritin <15 ng/mL, TIBC >450 μg/dL
- Microcytic anemia: MCV <80 fL suggests iron deficiency
- Macrocytic anemia: MCV >100 fL suggests folate/B12 deficiency
- Treatment response: Hemoglobin increase 1-2 g/dL in 4-6 weeks
-
Glucose Screening Interpretation
- 50-gram glucose challenge: ≥140 mg/dL requires 3-hour GTT
- 3-hour GTT thresholds: Fasting ≥95, 1-hr ≥180, 2-hr ≥155, 3-hr ≥140 mg/dL
- Two abnormal values confirm gestational diabetes mellitus
- Risk factors: BMI >30, Previous GDM, Family history diabetes
- Early screening: High-risk patients at first prenatal visit
- Management target: Fasting <95 mg/dL, 2-hour postprandial <120 mg/dL
💡 Master This: Effective prenatal assessment combines quantitative thresholds with pattern recognition - single abnormal values require confirmation and trending, while multiple abnormal parameters demand immediate intervention and specialist consultation.

This systematic approach to clinical assessment transforms routine prenatal visits into precision monitoring encounters where early detection and timely intervention optimize maternal and fetal outcomes through evidence-based care protocols.
🎯 Clinical Assessment Mastery: The Pattern Recognition Framework
🔍 Risk Stratification Excellence: The Precision Discrimination System
The Comprehensive Risk Assessment Framework operates through three distinct phases:
-
Initial Risk Stratification (First Prenatal Visit)
- Maternal Age Analysis: <18 years or >35 years = High Risk
- Teenage pregnancy: 2x risk preterm delivery, 3x risk low birth weight
- Advanced maternal age: 4x risk chromosomal abnormalities, 2x risk pregnancy loss
- Very advanced age (>40 years): 8x risk Down syndrome, 5x risk diabetes
- BMI Risk Categories: <18.5 or >30 kg/m² = Increased Surveillance
- Underweight (BMI <18.5): 2x risk preterm delivery, inadequate fetal growth
- Obese (BMI >30): 3x risk gestational diabetes, 4x risk preeclampsia
- Morbidly obese (BMI >40): 6x risk cesarean delivery, increased anesthesia complications
- Maternal Age Analysis: <18 years or >35 years = High Risk
-
Medical History Risk Quantification
- Chronic Hypertension: 25% risk superimposed preeclampsia, 15% risk placental abruption
- Diabetes Mellitus: 40% risk macrosomia, 20% risk congenital anomalies
- Autoimmune Disorders: 30% risk pregnancy complications, medication teratogenicity concerns
- Systemic lupus: 25% risk pregnancy loss, antiphospholipid syndrome screening
- Thyroid disease: 15% risk preterm delivery, fetal thyroid dysfunction
- Renal disease: 50% risk preeclampsia, creatinine >1.4 mg/dL = high risk
📌 Remember: MOTHER Risk Factors - Medical history, Obstetric history, Teratogen exposure, Hereditary factors, Environmental risks, Reproductive age extremes
Obstetric History Risk Stratification provides predictive accuracy:
- Previous Pregnancy Outcomes
- Recurrent pregnancy loss: ≥2 consecutive losses = 40% recurrence risk
- Previous preterm delivery: <37 weeks = 30% recurrence risk
- Previous preeclampsia: 20% recurrence risk, 40% if severe
- Early-onset preeclampsia (<34 weeks): 65% recurrence risk
- HELLP syndrome history: 25% recurrence risk, increased severity
- Placental abruption: 10% recurrence risk, monitor for bleeding
- Previous gestational diabetes: 50% recurrence risk, early screening indicated
- Previous macrosomia: >4000g = 25% recurrence risk, glucose screening
| Risk Category | Maternal Factors | Recurrence Risk | Monitoring Frequency | Specialist Care |
|---|---|---|---|---|
| Low Risk | Age 18-35, Normal BMI | <5% | Standard schedule | Routine OB |
| Moderate Risk | Age extremes, Obesity | 10-20% | Every 2-3 weeks | OB + Consultation |
| High Risk | Chronic disease, Previous complications | 25-50% | Weekly monitoring | MFM required |
| Very High Risk | Multiple factors, Severe disease | >50% | Twice weekly | Tertiary center |
| Critical Risk | Life-threatening conditions | >75% | Continuous monitoring | ICU-level care |
-
First Trimester Indicators
- Hyperemesis gravidarum: Severe = increased preeclampsia risk
- Bleeding complications: 20% pregnancy loss risk if heavy bleeding
- Multiple gestation: Twin pregnancy = 6x risk preterm delivery
- Monochorionic twins: 15% risk twin-to-twin transfusion syndrome
- Higher-order multiples: 90% risk preterm delivery <37 weeks
- Cervical length <25mm: 50% risk preterm delivery <32 weeks
-
Second/Third Trimester Evolution
- Gestational hypertension: 25% progression to preeclampsia
- Gestational diabetes: 50% risk future Type 2 diabetes
- Oligohydramnios: 30% risk fetal growth restriction
- AFI <5 cm: Increased perinatal morbidity, weekly monitoring
- Polyhydramnios: 20% risk fetal anomalies, diabetes association
- IUGR diagnosis: 10% risk stillbirth, delivery timing critical
⭐ Clinical Pearl: Risk stratification is dynamic - 15-20% of pregnancies change risk categories during gestation, requiring continuous reassessment and care plan modification based on evolving clinical parameters.
Intervention Thresholds guide evidence-based management:
- Low-Risk Management: Standard prenatal care with routine monitoring
- Moderate-Risk Enhancement: Increased visit frequency, additional testing
- High-Risk Protocols: Specialist consultation, intensive monitoring, delivery planning
- Critical-Risk Management: Tertiary care, multidisciplinary teams, early delivery consideration
💡 Master This: Effective risk stratification combines quantitative risk factors with clinical judgment - use evidence-based thresholds for initial categorization, then modify based on clinical evolution and patient-specific factors throughout pregnancy.
This systematic approach to risk stratification transforms prenatal care from one-size-fits-all to precision medicine, where individualized risk assessment drives targeted interventions that optimize maternal and fetal outcomes through evidence-based care escalation.
🔍 Risk Stratification Excellence: The Precision Discrimination System
⚖️ Evidence-Based Intervention Protocols: The Treatment Decision Engine
The Primary Intervention Framework operates through condition-specific protocols:
-
Hypertensive Disorders Management
- Gestational Hypertension Protocol: BP 140-159/90-109 mmHg
- First-line treatment: Methyldopa 250mg TID (safety profile >30 years)
- Alternative agents: Labetalol 100mg BID or Nifedipine XL 30mg daily
- Target BP: 130-150/80-100 mmHg (avoid excessive reduction)
- Monitoring frequency: Twice weekly visits with home BP tracking
- Severe Preeclampsia Management: BP ≥160/110 mmHg + Proteinuria
- Immediate treatment: Labetalol 20mg IV or Hydralazine 5mg IV
- Magnesium sulfate: 6g loading dose, 2g/hr maintenance for seizure prophylaxis
- Delivery timing: <34 weeks = corticosteroids + delivery in 48h
- Laboratory monitoring: CBC, CMP, LFTs every 12-24 hours
- Gestational Hypertension Protocol: BP 140-159/90-109 mmHg
-
Gestational Diabetes Intervention Ladder
- Dietary Management (First-line for 80% of patients)
- Carbohydrate restriction: 40-45% of total calories
- Target glucose levels: Fasting <95 mg/dL, 2-hour postprandial <120 mg/dL
- Weight gain goals: 15-25 lbs for normal BMI, 11-20 lbs for overweight
- Insulin Therapy (Required for 20% of GDM patients)
- Initiation criteria: >2 abnormal glucose values per week
- Starting dose: 0.7-1.0 units/kg current weight
- Monitoring: 4x daily glucose checks, weekly dose adjustments
- Dietary Management (First-line for 80% of patients)
📌 Remember: TREAT Protocol - Target identification, Risk assessment, Evidence review, Action implementation, Tracking outcomes
Preterm Labor Prevention Strategies demonstrate intervention efficacy:
-
Cervical Length Screening Protocol
- Universal screening: Transvaginal ultrasound at 18-24 weeks
- Short cervix definition: <25mm before 24 weeks gestation
- Intervention thresholds: <20mm = high risk, <15mm = very high risk
- Progesterone supplementation: 200mg vaginal daily reduces preterm delivery by 45%
- Cervical cerclage: History-indicated or ultrasound-indicated placement
- Activity modification: Pelvic rest, reduced physical activity
- Serial monitoring: Every 2 weeks until 24 weeks, then weekly
-
Preterm Labor Treatment Protocols
- Tocolytic therapy: 48-hour delay for corticosteroid administration
- Nifedipine: 20mg PO, then 10-20mg q4-6h (first-line)
- Indomethacin: 50-100mg, then 25mg q6h (<32 weeks only)
- Magnesium sulfate: 6g loading, 2-4g/hr maintenance
- Corticosteroid administration: Betamethasone 12mg IM x2 doses 24h apart
- Efficacy window: 24h-7 days after second dose
- Repeat course: Consider if >14 days since initial course
- Neuroprotection: Magnesium sulfate for deliveries <32 weeks
- Tocolytic therapy: 48-hour delay for corticosteroid administration
| Condition | First-Line Treatment | Success Rate | Monitoring Required | Alternative Options |
|---|---|---|---|---|
| Gestational HTN | Methyldopa 250mg TID | 85% BP control | Twice weekly visits | Labetalol, Nifedipine |
| Severe Preeclampsia | Labetalol IV + MgSO4 | 95% seizure prevention | Continuous monitoring | Hydralazine IV |
| Gestational DM | Diet modification | 80% glucose control | Weekly glucose logs | Insulin therapy |
| Preterm Labor | Nifedipine + Steroids | 70% delivery delay | Continuous fetal monitoring | Indomethacin, MgSO4 |
| IUGR | Delivery timing | 90% survival >32 weeks | Twice weekly testing | Expectant management |
Fetal Growth Restriction Management requires precise intervention timing:
-
Surveillance Protocols
- Biophysical profile: Twice weekly starting at diagnosis
- Umbilical artery Doppler: Weekly assessment of resistance indices
- Middle cerebral artery Doppler: Brain-sparing assessment
- Abnormal umbilical Doppler: Absent/reversed end-diastolic flow = delivery indication
- Cerebroplacental ratio: <1.08 indicates fetal compromise
- Ductus venosus Doppler: Abnormal = imminent delivery consideration
-
Delivery Decision Framework
- ≥37 weeks: Delivery recommended regardless of testing results
- 34-36 weeks: Abnormal testing = delivery, normal testing = continue surveillance
- 32-33 weeks: Severe oligohydramnios or abnormal Doppler = delivery
- <32 weeks: Multidisciplinary decision weighing fetal vs neonatal risks
💡 Master This: Evidence-based prenatal interventions require precise timing, appropriate dosing, and systematic monitoring - early intervention prevents progression to severe disease, while delayed intervention may result in irreversible complications affecting both mother and baby.
These intervention protocols transform prenatal care from reactive management to proactive prevention, where evidence-based treatments applied at optimal timing achieve measurable improvements in maternal and fetal outcomes through systematic clinical excellence.
⚖️ Evidence-Based Intervention Protocols: The Treatment Decision Engine
🔗 Multidisciplinary Integration: The Collaborative Care Ecosystem
The Core Integration Framework operates through specialty-specific contributions:
-
Maternal-Fetal Medicine (MFM) Integration
- Consultation triggers: High-risk conditions requiring subspecialty expertise
- Advanced maternal age (>40 years) with multiple risk factors
- Chronic medical conditions: Diabetes, hypertension, autoimmune disorders
- Previous pregnancy complications: Preeclampsia, preterm delivery, stillbirth
- Fetal anomalies: Structural defects, genetic abnormalities, growth restriction
- Shared care protocols: 70% of high-risk patients benefit from collaborative management
- Initial MFM consultation: Risk stratification and management planning
- Ongoing collaboration: Monthly consultations with primary OB provider
- Delivery planning: Timing, mode, and location optimization
- Consultation triggers: High-risk conditions requiring subspecialty expertise
-
Endocrinology Collaboration (15% of pregnancies require glucose management)
- Gestational diabetes management: Dietary counseling + medication optimization
- Pre-gestational diabetes: Insulin adjustment + complication prevention
- Thyroid disorders: Medication titration + fetal monitoring
- Target HbA1c: <6.5% preconception, <6.0% during pregnancy
- Insulin requirements: Increase 2-3x during second/third trimester
- Hypoglycemia prevention: Glucose monitoring 4x daily minimum
📌 Remember: TEAMS Approach - Timing coordination, Expertise sharing, Access facilitation, Monitoring integration, Support optimization
Mental Health Integration addresses psychological wellbeing throughout pregnancy:
-
Screening Protocols (Universal screening at 3 timepoints)
- Initial visit: Edinburgh Postnatal Depression Scale (EPDS)
- 28 weeks gestation: Repeat EPDS + anxiety screening
- Postpartum: 6-week and 3-month follow-up assessments
- EPDS score ≥10: Further evaluation required
- Suicidal ideation: Immediate psychiatric consultation
- Substance use screening: 4P's questionnaire at every visit
-
Treatment Integration
- Mild-moderate depression: Psychotherapy + support groups
- Severe depression: Medication management with reproductive psychiatry
- Anxiety disorders: Cognitive behavioral therapy + medication if needed
- Safe antidepressants: Sertraline, fluoxetine, citalopram
- Avoid medications: Paroxetine (cardiac defects), benzodiazepines (withdrawal)
- Monitoring requirements: Weekly visits during medication initiation
| Specialty | Consultation Triggers | Collaboration Frequency | Key Contributions | Outcome Improvements |
|---|---|---|---|---|
| MFM | High-risk conditions | Monthly visits | Risk assessment, Monitoring protocols | 40% reduction complications |
| Endocrinology | Diabetes, Thyroid disease | Every 2-4 weeks | Medication management | 60% better glucose control |
| Cardiology | Heart disease, Hypertension | As needed | Cardiac monitoring | 50% reduction cardiac events |
| Mental Health | Depression, Anxiety | Weekly-monthly | Psychological support | 70% symptom improvement |
| Nutrition | GDM, Eating disorders | Monthly | Dietary counseling | 30% better weight management |
-
Certified Nurse Midwives (CNMs) provide 40% of low-risk prenatal care
- Scope of practice: Normal pregnancies, routine monitoring, education
- Collaboration protocols: Physician backup for complications
- Patient satisfaction: 95% satisfaction rates with midwifery care
- Longer visit times: 30-45 minutes vs 15-20 minutes physician visits
- Enhanced education: Nutrition, exercise, childbirth preparation
- Continuity of care: Same provider throughout pregnancy and delivery
-
Registered Dietitians (Essential for 25% of pregnancies)
- Gestational diabetes: Medical nutrition therapy reduces insulin needs by 50%
- Eating disorders: Specialized counseling prevents pregnancy complications
- Obesity management: Structured programs limit excessive weight gain
- Individual counseling: 60-90 minute initial assessment
- Follow-up frequency: Every 2-4 weeks based on condition severity
- Group classes: Cost-effective education for multiple patients
⭐ Clinical Pearl: Effective multidisciplinary care requires clear communication protocols - shared electronic records, regular team meetings, and defined roles prevent care fragmentation and improve patient outcomes by ensuring coordinated interventions.
Technology-Enhanced Coordination improves care integration:
- Electronic Health Records (EHR) enable real-time information sharing
- Telemedicine platforms facilitate specialist consultations without travel barriers
- Remote monitoring devices allow continuous data collection between visits
- Patient portals enhance communication and education delivery
💡 Master This: Successful multidisciplinary prenatal care requires proactive coordination, clear communication, and shared accountability - identify team members early, establish consultation thresholds, and maintain regular communication to optimize maternal and fetal outcomes through collaborative expertise.
This integrated approach transforms prenatal care from isolated medical management to comprehensive health optimization, where coordinated expertise addresses all aspects of maternal-fetal wellbeing through evidence-based collaboration and patient-centered care delivery.
🔗 Multidisciplinary Integration: The Collaborative Care Ecosystem
🎯 Clinical Mastery Arsenal: The Rapid Excellence Toolkit
Essential Threshold Arsenal - Memorize These Numbers:
-
Blood Pressure Thresholds
- Normal: <140/90 mmHg throughout pregnancy
- Gestational HTN: ≥140/90 mmHg after 20 weeks without proteinuria
- Severe HTN: ≥160/110 mmHg requires immediate treatment
- Treatment target: 130-150/80-100 mmHg (avoid over-treatment)
-
Laboratory Critical Values
- Hemoglobin: <11.0 g/dL (1st trimester), <10.5 g/dL (2nd/3rd trimester)
- Platelets: <100,000/μL suggests HELLP syndrome or ITP
- Creatinine: >1.0 mg/dL indicates renal impairment in pregnancy
- Glucose: ≥140 mg/dL (1-hour GTT), ≥95 mg/dL (fasting GTT)
📌 Remember: NUMBERS Mastery - Normal ranges, Urgent thresholds, Monitoring intervals, Baseline values, Emergency limits, Reference standards, Screening cutoffs
Rapid Assessment Protocol - The 5-Minute Evaluation:
-
Primary Survey (60 seconds)
- Vital signs: BP, pulse, weight, fundal height
- Fetal assessment: Heart rate, movement, presentation
- Symptom screen: Headache, vision changes, contractions, bleeding
-
Secondary Assessment (4 minutes)
- Interval history: New symptoms, medication compliance, activity level
- Physical examination: Edema, reflexes, cervical assessment (if indicated)
- Risk reassessment: New factors, progression of existing conditions
| Assessment Component | Normal Findings | Abnormal Triggers | Immediate Actions | Follow-up Required |
|---|---|---|---|---|
| Blood Pressure | <140/90 mmHg | ≥140/90 mmHg | Repeat in 15 min | Home monitoring |
| Fundal Height | ±3 cm from GA | >3 cm deviation | Ultrasound evaluation | Serial measurements |
| Fetal Heart Rate | 110-160 bpm | <110 or >160 bpm | Extended monitoring | NST/BPP |
| Weight Gain | 1-2 lbs/month | >5 lbs/week | Evaluate for preeclampsia | Dietary counseling |
| Proteinuria | Trace or negative | 1+ or greater | 24-hour urine | Preeclampsia workup |
Emergency Protocol Arsenal - Immediate Action Plans:
-
Severe Preeclampsia Protocol
- Step 1: IV access + continuous monitoring
- Step 2: Labetalol 20mg IV or Hydralazine 5mg IV
- Step 3: MgSO₄ 6g loading dose over 20 minutes
- Step 4: Laboratory workup (CBC, CMP, LFTs, coagulation)
- Step 5: Delivery planning based on gestational age
-
Preterm Labor Protocol
- Step 1: Cervical examination + fetal monitoring
- Step 2: Tocolysis if <34 weeks and no contraindications
- Step 3: Betamethasone 12mg IM x2 doses 24h apart
- Step 4: GBS prophylaxis if culture unknown
- Step 5: Neuroprotection (MgSO₄) if <32 weeks
Medication Quick Reference - Dosing and Safety:
-
Antihypertensives
- Methyldopa: 250mg TID, maximum 3g/day
- Labetalol: 100mg BID, maximum 2400mg/day
- Nifedipine XL: 30mg daily, maximum 120mg/day
-
Tocolytics
- Nifedipine: 20mg PO, then 10-20mg q4-6h
- Indomethacin: 50-100mg loading, then 25mg q6h (<32 weeks only)
💡 Master This: Clinical excellence in prenatal care requires instant recall of critical thresholds, systematic assessment protocols, and evidence-based interventions - practice rapid decision-making using standardized algorithms until pattern recognition becomes automatic and clinical responses become reflexive.
Quality Metrics Dashboard - Track Your Excellence:
-
Process Measures
- Visit adherence: >90% of scheduled appointments
- Screening completion: 100% of recommended tests
- Documentation quality: Complete assessment at every visit
-
Outcome Measures
- Preterm delivery rate: <10% for low-risk patients
- Cesarean section rate: <25% for nulliparous patients
- Patient satisfaction: >95% satisfaction scores
This Clinical Mastery Arsenal transforms prenatal care delivery from reactive management to proactive excellence, where systematic protocols, evidence-based thresholds, and rapid decision-making optimize maternal and fetal outcomes through clinical precision and professional mastery.
🎯 Clinical Mastery Arsenal: The Rapid Excellence Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















