Back
CVS Pharmacology Mnemonics Glossary: High-Yield Cardiovascular Drugs for NEET PG, INI-CET & USMLE 2026
Master cardiovascular pharmacology with proven mnemonics and memory techniques. Complete guide to high-yield CVS drugs for NEET PG, INI-CET & USMLE 2026 with classification, mechanisms, and exam tips.

CVS Pharmacology Mnemonics Glossary: High-Yield Cardiovascular Drugs for NEET PG, INI-CET & USMLE 2026
Cardiovascular pharmacology represents one of the highest-yield topics in medical entrance examinations, consistently appearing in 15-20% of pharmacology questions in NEET PG, INI-CET, and USMLE. With over 200 cardiovascular drugs to master, memory techniques and mnemonics become essential tools for medical students aiming to excel in these competitive exams in 2026.
This comprehensive glossary provides proven mnemonics and memory techniques for cardiovascular drugs, organized by therapeutic classes to maximize retention and recall during high-pressure exam situations. Whether you're preparing for NEET PG, INI-CET, or USMLE, these time-tested memory aids will help you master CVS pharmacology efficiently.
Why CVS Pharmacology Mnemonics Are Essential in 2026
Medical entrance examinations have become increasingly competitive, with NEET PG receiving over 200,000 applications annually. The cardiovascular system's complexity, combined with the vast array of drugs affecting heart function, blood pressure, and circulation, makes systematic memorization crucial.
Key Statistics for CVS Pharmacology in Medical Exams:
NEET PG: 8-12 questions per exam (15-20% of pharmacology)
INI-CET: 6-10 questions per exam (12-18% of pharmacology)
USMLE Step 1: 10-15 questions per exam (10-15% of pharmacology)
The challenge lies not just in memorizing drug names, but understanding their mechanisms, side effects, contraindications, and clinical applications. Effective mnemonics bridge this gap by creating memorable connections between complex pharmacological concepts.
Essential CVS Drug Classification Overview
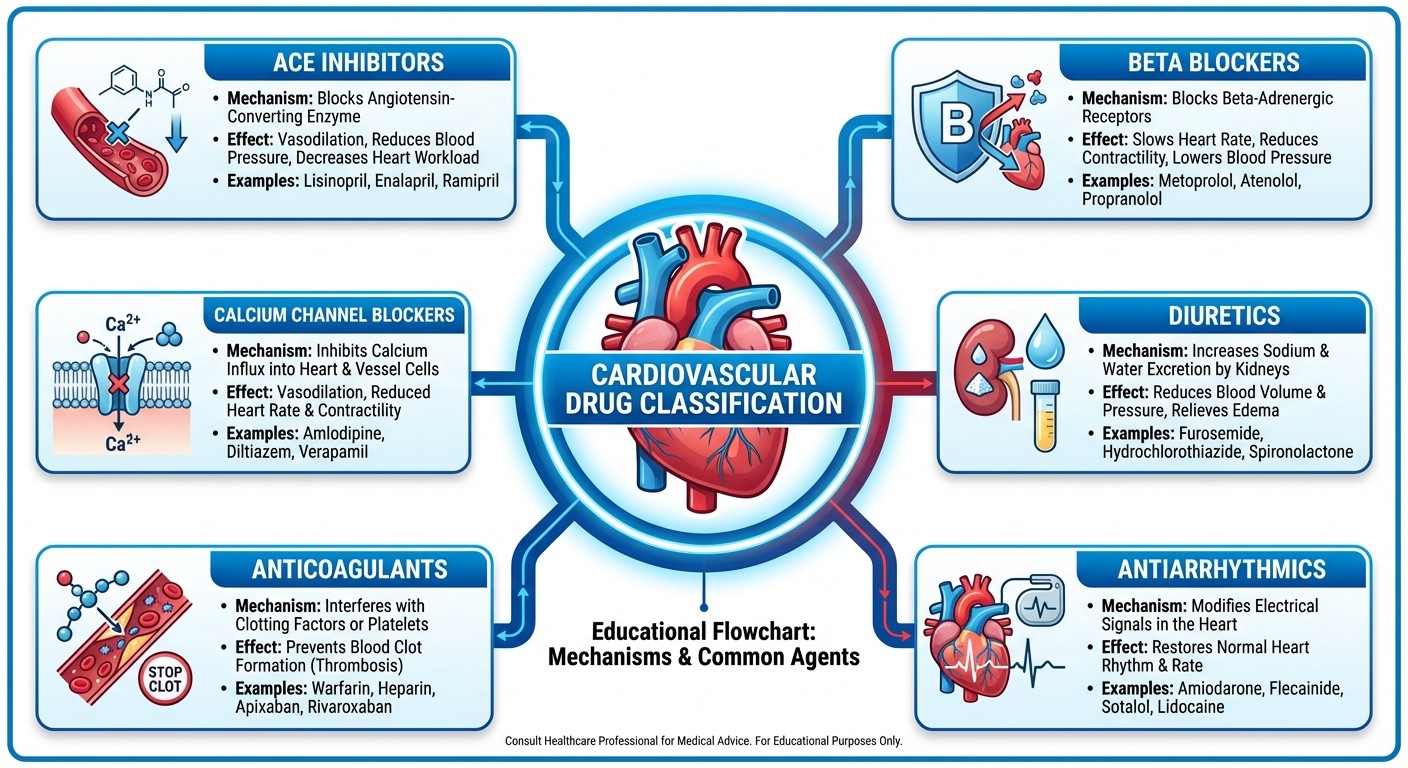
Before diving into specific mnemonics, understanding the broad classification of cardiovascular drugs provides a framework for organized learning:
Drug Class | Primary Mechanism | Common Exams Focus |
|---|---|---|
ACE Inhibitors | Block angiotensin conversion | Mechanism, side effects |
Beta Blockers | Block β-adrenergic receptors | Classification, selectivity |
Calcium Channel Blockers | Block calcium channels | Types, cardiac vs vascular |
Diuretics | Modify electrolyte balance | Sites of action, side effects |
Anticoagulants | Prevent clot formation | Monitoring, reversal agents |
Antiarrhythmics | Modify cardiac conduction | Vaughan Williams classification |
ACE Inhibitors and ARBs: The "CAPTOPRIL" System
ACE Inhibitors Mnemonic: "CAPTAINS LOVE PEACE"
Captopril
Alalapril (Alacepril)
Perindopril
Trandolapril
Alalapril
Imipril (Imidapril)
Nisinopril (Lisinopril)
Silazapril
Mechanism Memory Aid: "ACE Cuts Angel to Devil"
ACE enzyme converts Angiotensin I to Angiotensin II
ACE inhibitors block this conversion
Remember: Less "devil" (Angiotensin II) = Less vasoconstriction
ARBs Mnemonic: "LOSERS Can't TELL VALS"
LOSartan
Eprosartan
Rrosartan (Irbesartan)
Sartans end with "-sartan"
Candesartan
Telmisartan
Eposartan (Eprosartan)
Losartan (repeated for emphasis)
Losartan
VALsartan
Sartans
Side Effects Memory: "ACE gives you HACK"
Hyperkalemia
Angioedema
Cough (dry, persistent)
Kidney dysfunction
For comprehensive understanding of ACE inhibitors and their clinical applications, explore our cardiovascular drugs lessons and practice with cardiovascular pharmacology questions.
Beta Blockers: The "SMART BETA" Classification
Non-Selective Beta Blockers: "PINT"
Propranolol
Ioprenaline (blocks)
Nadolol
Timolol
Beta-1 Selective (Cardioselective): "BEAM"
Betaxolol
Esmolol
Atenolol
Metoprolol
Alpha + Beta Blockers: "CARL"
Carvedilol
Alpha and beta action
Recognize dual action
Labetalol
Beta Blocker Side Effects: "BACHELOR"
Bradycardia
Asthma exacerbation
CHF precipitation
Hypoglycemia masking
Erectile dysfunction
Lipid profile changes
Orthostatic hypotension
Raynaud's phenomenon
Clinical Uses Memory: "MATCH"
Myocardial infarction
Angina
Tachycardia
CHF (specific agents)
Hypertension
Practice beta blocker concepts with our specialized cardiovascular pharmacology flashcards for optimal retention.
Calcium Channel Blockers: The "DHP vs Non-DHP" System
Dihydropyridines (DHP): "NICE FAMILY"
Nifedipine
Isrpradipine (Isradipine)
Clevidipine
Emlodipine (Amlodipine)
Felodipine
Amlodipine
Manidipine
Ilodipine (Cilnidipine)
Lacidipine
Yelopidine (Nicardipine)
DHP Characteristics: "VESSEL"
Vascular selectivity
Edema (ankle)
Selective for vessels
Short-acting (some)
Effective in HTN
Less cardiac effects
Non-Dihydropyridines: "VD"
Verapamil
Diltiazem
Non-DHP Memory: "HEART DRUGS"
Heart rate reduction
Effective in arrhythmias
AV node depression
Reduced contractility
Timing important (avoid with beta blockers)
Contraindication Alert: "VD + BB = BAD"
Verapamil/Diltiazem + Beta Blockers = Severe bradycardia/heart block
Diuretics: The "TALC" Classification System
Thiazide and Thiazide-like: "HIT"
Hydrochlorothiazide (HCTZ)
Indapamide
Torisamide (Torasemide - thiazide-like)
Loop Diuretics: "FABLE"
Furosemide
Anidemide (Bumetanide starts with B, but think 'A' for 'Another strong one')
Bumetanide
Lasix (brand name for furosemide)
Ethacrynic acid
Potassium-Sparing: "AMTS"
Amiloride
Milrinone (not typically classified here, but remember spironolactone)
Triamterene
Spironolactone
Diuretic Sites: "Please Take Loop Carefully Daily"
Proximal tubule - Carbonic anhydrase inhibitors
Thick ascending limb - Loop diuretics
Late distal tubule - Thiazides
Collecting duct - K-sparing
Distal effects vary
Side Effects by Class: Thiazides: "DISH"
Diabetes (hyperglycemia)
Improved calcium retention
Sodium loss
Hyperuricemia
Loop Diuretics: "HONDA"
Hypokalemia
Ototoxicity
Nephrotoxicity
Dehydration
Alkalosis
Study diuretic mechanisms in detail with our antihypertensive agents lessons.
Anticoagulants and Antiplatelet Agents: The "CLOT BUSTERS"
Anticoagulants Classification: "HALO"
Heparin (unfractionated)
Argatroban (direct thrombin inhibitor)
LMWH (low molecular weight heparins)
Oral anticoagulants (warfarin, DOACs)
Direct Oral Anticoagulants (DOACs): "BRAD"
Bivalirudin (parenteral, but remember the 'B' sound)
Rivaroxaban (Factor Xa inhibitor)
Apixaban (Factor Xa inhibitor)
Dabigatran (Direct thrombin inhibitor)
Antiplatelet Agents: "ASPIC"
Aspirin
Sulfinpyrazone
Prasugrel
Iclinopidine (Ticlopidine)
Clopidogrel
Anticoagulant Monitoring: "WAR PT"
WARfarin monitored by PT/INR
Time is critical for adjustments
Reversal Agents Memory: "FRESH VITAMIN"
Fresh frozen plasma (warfarin)
Reversal agents exist
Etoxaban (vitamin K)
Specific reversal agents (idarucizumab for dabigatran)
Heparin (protamine sulfate)
VITAMIN K (warfarin antidote)
For detailed anticoagulation protocols, refer to our anticoagulants and antiplatelet drugs lessons.
Antiarrhythmic Drugs: Vaughan Williams Classification
Class I (Sodium Channel Blockers): "DIPPED"
Class Ia: "DIPPED"
Disopyramide
Isopamidine (Procainamide)
Procainamide
Procaine
Encainide (no longer used)
Different kinetics
Class Ib: "LIMP"
Lidocaine
Impidine (Mexiletine)
Mexiteline
Phenytoin
Class Ic: "PERFECT"
Propafenone
Ethmosin (Moricizine, technically class I)
Right ventricular effects
Flecainide
Encainide (discontinued)
Cardiac effects potent
Toxicity concerns
Class II (Beta Blockers): "BEAM" (as mentioned earlier)
Class III (Potassium Channel Blockers): "SODA"
Sotalol
Other drugs in this class
Dofetilide
Amiodarone
Class IV (Calcium Channel Blockers): "VD" (Verapamil, Diltiazem)
Vaughan Williams Memory Master: "Some Drugs Can Kill"
Sodium channel blockers (Class I)
Dynamic beta blockers (Class II)
Channel potassium blockers (Class III)
Kalcium channel blockers (Class IV)
Study comprehensive antiarrhythmic protocols with our antiarrhythmic drugs lessons.
Heart Failure Medications: The "DAVID" Protocol
Primary Heart Failure Drugs: "DAVID"
Digoxin
ACE inhibitors/ARBs
Vasodilators
Inotropes
Diuretics
Positive Inotropes: "DODGE"
Digoxin
Outabain
Dobutamine
Gglucagon
Epinephrine
Digoxin Toxicity: "NAVY"
Nausea/vomiting
Arrhythmias
Vision changes (yellow halos)
Younger patients more susceptible
Heart Failure Stages Memory: "ABCD"
A - At risk
B - Structural changes, no symptoms
C - Symptomatic heart failure
D - Advanced/refractory heart failure
Access comprehensive heart failure management strategies through our drugs for heart failure lessons.
Antianginal Agents: The "NoBBS" Approach
Antianginal Drug Classes: "NoBBS"
Noitrates
Beta blockers
Beta blockers (emphasis on importance)
Statins (for underlying CAD)
Nitrates Classification: "SING"
Short-acting: Sublingual nitroglycerin
Intermediate: Isosorbide dinitrate
Nitroglycerin (various forms)
Glong-acting: Isosorbide mononitrate
Nitrate Side Effects: "HEAD"
Headache
Edema (uncommon)
Acute hypotension
Dizziness
Contraindications: "VIPS"
VViagra (PDE-5 inhibitors)
Isevere aortic stenosis
Pericardial tamponade
Severe hypotension
Learn detailed antianginal therapy protocols in our antianginal agents lessons.
Lipid-Lowering Drugs: The "STATIN FAMILY"
HMG-CoA Reductase Inhibitors (Statins): "RALPH'S FAMILY"
Rosuvastatin
Atorvastatin
Lovastatin
Pravastatin
High potency group
Simvastatin
Fluvastatin
All end in "-statin"
Memory aid complete
Important for exams
Lipid reduction
Yearly monitoring needed
Other Lipid Drugs: "FENCE"
Fibrates (gemfibrozil, fenofibrate)
Ezetimibe
Niacin
Colesevelam (bile acid sequestrant)
Everything else (PCSK9 inhibitors)
Statin Side Effects: "HARM"
Hepatotoxicity
Ache (muscle pain)
Rhabdomyolysis (rare)
Myopathy
Drug Interactions: "CYP-STOP"
CYP3A4 inhibitors increase statin levels
Strong interactions with certain statins
Toxicity risk increases
Optimize by choosing right statin
Particularly important with simvastatin/lovastatin
Explore comprehensive lipid management strategies in our lipid-lowering drugs lessons.
Advanced Cardiovascular Drugs: Specialized Agents
Pulmonary Hypertension Drugs: "BEST"
Bosentan (endothelin receptor antagonist)
Epoprostenol (prostacyclin analogue)
Sildenafil (PDE-5 inhibitor)
Treprostinil (prostacyclin analogue)
Vasodilators: "MINI HELP"
Minoxidil
Isopressin (not typically a vasodilator, but remember hydralazine)
Nitroprusside
Ihydralazine
Vasodilator Toxicity:
Minoxidil: Hirsutism, fluid retention
Hydralazine: Lupus-like syndrome
Nitroprusside: Cyanide toxicity
High-Yield Exam Tips and Memory Strategies
Most Frequently Asked CVS Pharmacology Topics:
1. Mechanism of action questions (40%)
- Focus on unique mechanisms
- Understand receptor specificity
- Know cellular pathways
2. Side effects and contraindications (35%)
- Learn pattern recognition
- Understand pathophysiology of side effects
- Know absolute vs relative contraindications
3. Drug interactions (15%)
- Focus on clinically significant interactions
- Understand CYP450 involvement
- Know additive effects
4. Clinical applications (10%)
- Match drugs to specific conditions
- Understand first-line vs second-line therapy
- Know evidence-based guidelines
Effective Study Strategies for CVS Pharmacology:
The HEART Method:
Highlight key mechanisms
Examine side effects systematically
Associate drugs with clinical scenarios
Review contraindications regularly
Test recall with practice questions
Spaced Repetition Schedule:
Day 1: Learn new mnemonics
Day 3: Review and test recall
Day 7: Comprehensive review
Day 14: Mixed topic practice
Day 30: Pre-exam consolidation
For optimal retention, combine these mnemonics with active practice using our comprehensive cardiovascular pharmacology flashcards, which feature spaced repetition algorithms designed for medical students.
Integration with Other Pharmacology Topics
Connecting CVS Drugs to Other Systems:
Autonomic Nervous System Links:
Beta blockers → ANS pharmacology
Alpha blockers → Hypertension management
Sympathomimetics → Emergency medicine
Study these connections in our autonomic nervous system drugs lessons. Endocrine System Connections:
Diabetes medications + CVS drugs
Thyroid drugs + cardiac effects
Adrenal medications + cardiovascular impact
Renal Pharmacology Integration:
Diuretics mechanism overlap
Nephrotoxic drug interactions
Electrolyte management
Practice Questions and Self-Assessment
High-Yield Question Types:
1. Mechanism-based questions:
"Which drug blocks the conversion of angiotensin I to angiotensin II?"
2. Side effect recognition:
"A patient on ACE inhibitors develops a dry cough. What is the mechanism?"
3. Drug interaction scenarios:
"What happens when verapamil is given with a beta blocker?"
4. Clinical application:
"What is the first-line treatment for heart failure with reduced ejection fraction?"
Self-Assessment Checklist:
[ ] Can recall all major drug classes without notes
[ ] Know primary mechanisms for each class
[ ] Understand contraindications and side effects
[ ] Can solve clinical scenarios quickly
[ ] Familiar with high-yield drug interactions
Test your knowledge comprehensively with our cardiovascular pharmacology practice questions, designed specifically for NEET PG, INI-CET, and USMLE preparation.
Conclusion
Mastering cardiovascular pharmacology through effective mnemonics provides a solid foundation for success in medical entrance examinations. The systematic approach outlined in this glossary, combined with regular practice and spaced repetition, will help you achieve mastery over this high-yield topic.
Remember that while mnemonics provide excellent memory aids, understanding the underlying pathophysiology and clinical applications remains crucial for long-term retention and clinical practice. Use these memory techniques as stepping stones to deeper understanding rather than substitutes for comprehensive study.
For a complete learning experience, explore our comprehensive pharmacology study materials and practice extensively with our question banks designed specifically for competitive medical examinations.
Ready to master cardiovascular pharmacology? Start with our free trial and access thousands of high-yield questions, comprehensive lessons, and scientifically-designed flashcards to accelerate your exam preparation in 2026.