Cardiac Electrophysiology & Arrhythmia Basics - Shocking Rhythms
- Cardiac Action Potential (AP):
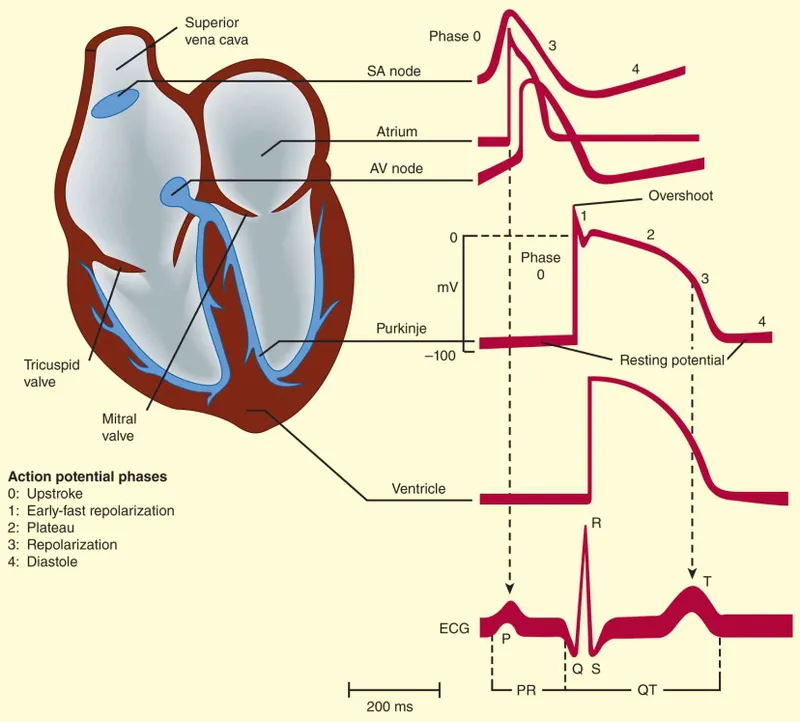
- Phases: 0 (rapid $Na^+$ influx), 1 (early $K^+$ efflux), 2 (plateau: $Ca^{2+}$ influx, $K^+$ efflux), 3 (rapid $K^+$ efflux), 4 (resting potential).
- Key Ions: $Na^+$, $Ca^{2+}$, $K^+$.
- Arrhythmias:
- Types: Tachyarrhythmias (>100 bpm), Bradyarrhythmias (<60 bpm).
- Origin: Supraventricular (atria/AV node), Ventricular.
- Antiarrhythmic Therapy Goals:
- Control rate/rhythm.
- Relieve symptoms, prevent complications (stroke, heart failure).
⭐ Key goals: Restore sinus rhythm or control ventricular rate; improve cardiac output, prevent complications (stroke, heart failure).
Class I Antiarrhythmics ($Na^+$ Blockers) - Salty Channel Tamers
- Vaughan Williams Class I: $Na^+$ channel blockers; state-dependent (act on open/inactivated channels).
| Sub-Class | MOA | Drugs | Uses | Side Effects |
|---|---|---|---|---|
| IA | Moderate block; ↑APD, ↑ERP | Quinidine, Procainamide, Disopyramide | Atrial/Ventricular arr. | Cinchonism (Q); Lupus (P); Anticholinergic (D) |
| IB | Weak block; ↓APD, ↓ERP (or no change) | Lidocaine, Mexiletine, Phenytoin | Ventricular arr. (post-MI) | CNS toxicity, Paresthesias |
| IC | Strong block; No change APD, marked ↑ERP | Flecainide, Propafenone | Refractory SVT/VT | Proarrhythmia, CNS effects |
- Class IA: "Queen Proclaims Diso's pyramid"
- Class IB: "Lidocaine Mexes with Pheny"
- Class IC: "Flecainide Propafenone for life" (but be careful!)
⭐ Class IC antiarrhythmics (e.g., Flecainide) are contraindicated in structural heart disease or post-MI due to ↑mortality (CAST trial).
Class II Antiarrhythmics (β-Blockers) - Beta Beat Controllers
- Vaughan Williams Class II: β-adrenergic blockers.
- Mechanism: ↓cAMP, ↓$Ca^{2+}$ currents; primarily slow SA & AV nodal conduction, ↓slope of phase 4 depolarization.
- Key Drugs: Propranolol, Metoprolol, Esmolol (short-acting).
- Clinical Uses: Rate control in atrial fibrillation/flutter, SVTs, ↓ventricular ectopy, post-MI protection.
- Key Side Effects: Bradycardia, AV block, bronchospasm (non-selective), fatigue.
⭐ Beta-blockers are unique among antiarrhythmics for their proven mortality benefit in post-myocardial infarction patients.
Class III Antiarrhythmics ($K^+$ Blockers) - Potassium's Power Play
- Vaughan Williams Class III: $K^+$ channel blockers.
- Mechanism: Prolong repolarization (Phase 3), ↑Action Potential Duration (APD), ↑Effective Refractory Period (ERP).
- ⚠️ Risk: Torsades de Pointes (TdP).
- Key Drugs:
- Amiodarone: Multi-channel effects; broad spectrum, complex PK.
- Sotalol: Also β-blocker; dose-dependent TdP risk.
- Dofetilide, Ibutilide.
- Amiodarone Side Effects: 📌 P-F-T-L-C-S (Pulmonary fibrosis, Eyes-corneal microdeposits, Thyroid/Testes dysfunction, Liver toxicity, CNS effects, Skin discoloration).
⭐ Amiodarone is notorious for its extensive drug interactions, primarily due to its inhibition of CYP450 enzymes (e.g., CYP3A4, CYP2C9) and P-glycoprotein.
Class IV Antiarrhythmics ($Ca^{2+}$ Blockers) - Calcium's Calming Crew
- Class: Non-DHP $Ca^{2+}$ blockers (L-type).
- Action: ↓SA/AV conduction (↓$phase 0$ nodal).
- Drugs: Verapamil, Diltiazem.
- Uses: AF/AFL rate control, PSVT.
- SEs: Bradycardia, AV block, constipation, edema. ⚠️ HF.
- CIs: WPW + AF, severe LV dysfunction.
⭐ Calcium channel blockers like Verapamil and Diltiazem are contraindicated in patients with Wolff-Parkinson-White (WPW) syndrome and atrial fibrillation as they can paradoxically increase ventricular rate by blocking AV nodal conduction and promoting conduction via the accessory pathway.
Miscellaneous Antiarrhythmics - The Unique Beats
| Drug | MOA | Use | Key SE |
|---|---|---|---|
| Adenosine | A1 agonist, ↑$K^+$ efflux, ↓$Ca^{2+}$ influx | PSVT (6mg→12mg IV) | Flushing, chest pain, asystole |
| Digoxin | Inhibits $Na^+$/$K^+$ ATPase, ↑vagal tone | AF (rate control), HF | Arrhythmias, GI, yellow halos |
| $MgSO_4$ | Affects $Na^+$/$K^+$ ATPase, $Ca^{2+}$ channels | Torsades de Pointes, digoxin toxicity | Hypotension, resp. depression |
📌 Adenosine: 'A-DEN-O-SINE' (Almost Dead, ENd Of SVT, Short-acting, IV, No effect on VT, EKG flatline).
⭐ Adenosine is highly effective for terminating paroxysmal supraventricular tachycardias (PSVTs) involving the AV node, but it is ineffective for atrial fibrillation, atrial flutter, or ventricular tachycardia.
High‑Yield Points - ⚡ Biggest Takeaways
- Vaughan Williams classification (I-IV) is key: Na+, β-blockers, K+, Ca2+ blockers.
- Amiodarone (Class III): broad-spectrum but major toxicities (pulmonary, thyroid, corneal).
- Adenosine: terminates acute SVT; very short half-life, transient asystole.
- Lidocaine (Ib): for ventricular arrhythmias post-MI, especially ischemia-related.
- Class Ic (Flecainide, Propafenone): avoid in structural heart disease (CAST trial risk).
- Beta-blockers (II): crucial for rate control in AFib & post-MI survival.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

