Cholinergic/Adrenergic drugs — MCQs

On this page
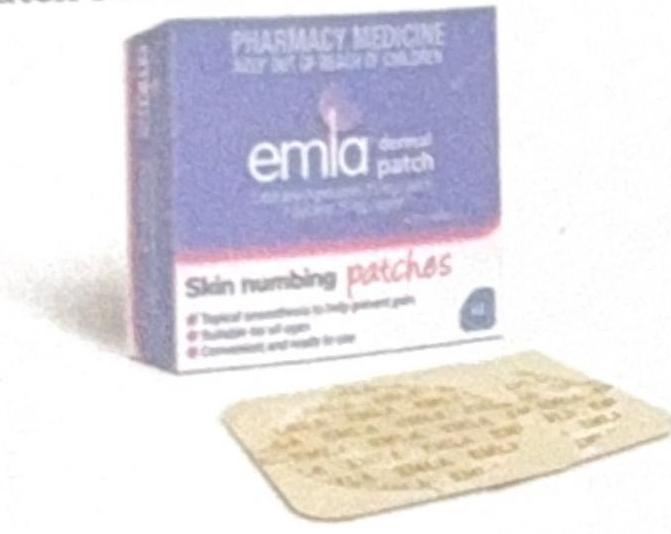
Which of the following is correct about the EMLA patch shown in the image below?
A patient has a history of vomiting and was given an antiemetic. The patient subsequently developed abnormal movements (likely extrapyramidal symptoms or dystonia). What medication should be given to manage these abnormal movements?
A 30-year-old male presents with a history of consuming an unknown substance. On examination, the patient has diaphoresis, headache, and features resembling acute coronary spasm. Which of the following clinical features is least likely to be present in this patient?
A child accidentally ingested a fruit from a tree while playing. After the ingestion, he presented with symptoms of restlessness, painful swallowing, photophobia, dry skin, urinary retention, and elevated body temperature. What is the most likely cause of poisoning, and what is the appropriate antidote for it?
Beta 2 receptors act via which of the following secondary messenger systems
A 68-year-old woman is brought to the emergency department by her son for altered mental status. She recently had a right knee arthroplasty and was discharged 2 days ago. Her medical history is significant for type 2 diabetes mellitus and hypertension, for which she takes metformin and hydrochlorothiazide, respectively. She also had left cataract surgery 1 year ago. Her temperature is 97°F (36.1°C), blood pressure is 99/70 mmHg, pulse is 60/min, respirations are 8/min. Her exam is notable for anisocoria with an irregularly shaped left pupil and a 1 mm in diameter right pupil. She opens her eyes and withdraws all of her limbs to loud voice and painful stimulation. Her fingerstick glucose level is 79. The patient does not have any intravenous access at this time. What is the best next step in management?
A 34-year-old woman presents to the office with weight gain despite her dietary modifications. She also says she has associated constipation and feels she has no energy. She says she often feels the ambient temperature is too cold these days. Her past medical history is insignificant. Her blood pressure is 140/85 mm Hg, the pulse is 60/min, the temperature is 36.7°C (98.0°F), and the respirations are 22/min. On physical examination, deep tendon reflexes are 1+ at the right ankle, which has a delayed relaxation phase. A hormone deficiency disorder is suspected and blood samples are sent to the lab for investigation. The laboratory report confirms the suspicion, and the patient is prescribed a synthetic hormone. How does this hormone most likely act to produce its cellular effects?
A 24-year-old man presents with a history of intermittent fever for the last 2 days. He says his episodes of fever are accompanied by shaking and chills. He mentions that his father has been recently recovered from chloroquine-resistant P. falciparum malaria, which was treated successfully with quinine. On physical examination, his temperature is 38.9°C (102°F), pulse rate is 110/min, blood pressure is 116/80 mm Hg, and respiratory rate is 18/min. Examination of his abdomen reveals splenomegaly. His blood sample is sent for the examination of the peripheral smear, which confirms the diagnosis of Plasmodium falciparum malaria. The patient is placed on treatment with oral quinine. After 5 days, the patient returns with improved symptoms of malaria but with complaints of a headache, tinnitus, nausea, and dizziness. The patient mentions that he has been taking a drug for the last 3 months to control his dyspepsia symptoms. Which of the following drugs is most likely to have caused the above-mentioned symptoms in this patient?
An 81-year-old woman is brought to the physician by her son because of worsening forgetfulness and disorientation over the past 2 years. She has to be reminded of her grandchildren's names and frequently forgets her current address. She lives with her son. She has occasional episodes of urinary incontinence. She appears well nourished. Neurologic examination shows no abnormalities; her gait is normal. Mental status examination shows mild memory impairment. She is oriented to self and place, but not to time. Which of the following is the most appropriate pharmacotherapy?
A 57-year-old woman presents complaining of feeling sleepy all the time. She reports having an uncontrollable urge to take multiple naps during the day and sometimes sees strange shadows in front of her before falling asleep. Although she awakens feeling refreshed and energized, she often finds herself ‘stuck’ and cannot move for a while after waking up. She also mentions she is overweight and has failed to lose weight despite multiple attempts at dieting and using exercise programs. No significant past medical history. No current medications. The patient denies smoking, alcohol consumption, or recreational drug usage. Family history reveals that both her parents were overweight, and her father had hypertension. Her vital signs include: pulse 84/min, respiratory rate 16/min, and blood pressure 128/84 mm Hg. Her body mass index (BMI) is 36 kg/m2. Physical examination is unremarkable. Which of the following medications is the best course of treatment in this patient?
Practice by Chapter
Acetylcholine receptors and function
Practice Questions
Cholinergic agonists (direct and indirect)
Practice Questions
Muscarinic antagonists
Practice Questions
Nicotinic antagonists
Practice Questions
Neuromuscular blocking agents
Practice Questions
Adrenergic receptor subtypes
Practice Questions
Alpha-adrenergic agonists
Practice Questions
Beta-adrenergic agonists
Practice Questions
Alpha-adrenergic antagonists
Practice Questions
Beta-adrenergic antagonists
Practice Questions
Sympathomimetics
Practice Questions
Autonomic drug interactions
Practice Questions
Clinical applications in autonomic disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
