Cholinergic/Adrenergic drugs — MCQs

On this page
A 55-year-old man comes to the physician with a 3-month history of headache, periodic loss of vision, and easy bruising. Physical examination shows splenomegaly. His hemoglobin concentration is 13.8 g/dL, leukocyte count is 8000/mm3, and platelet count is 995,000/mm3. Bone marrow biopsy shows markedly increased megakaryocytes with hyperlobulated nuclei. Genetic analysis shows upregulation of the JAK-STAT genes. The pathway encoded by these genes is also physiologically responsible for signal transmission of which of the following hormones?
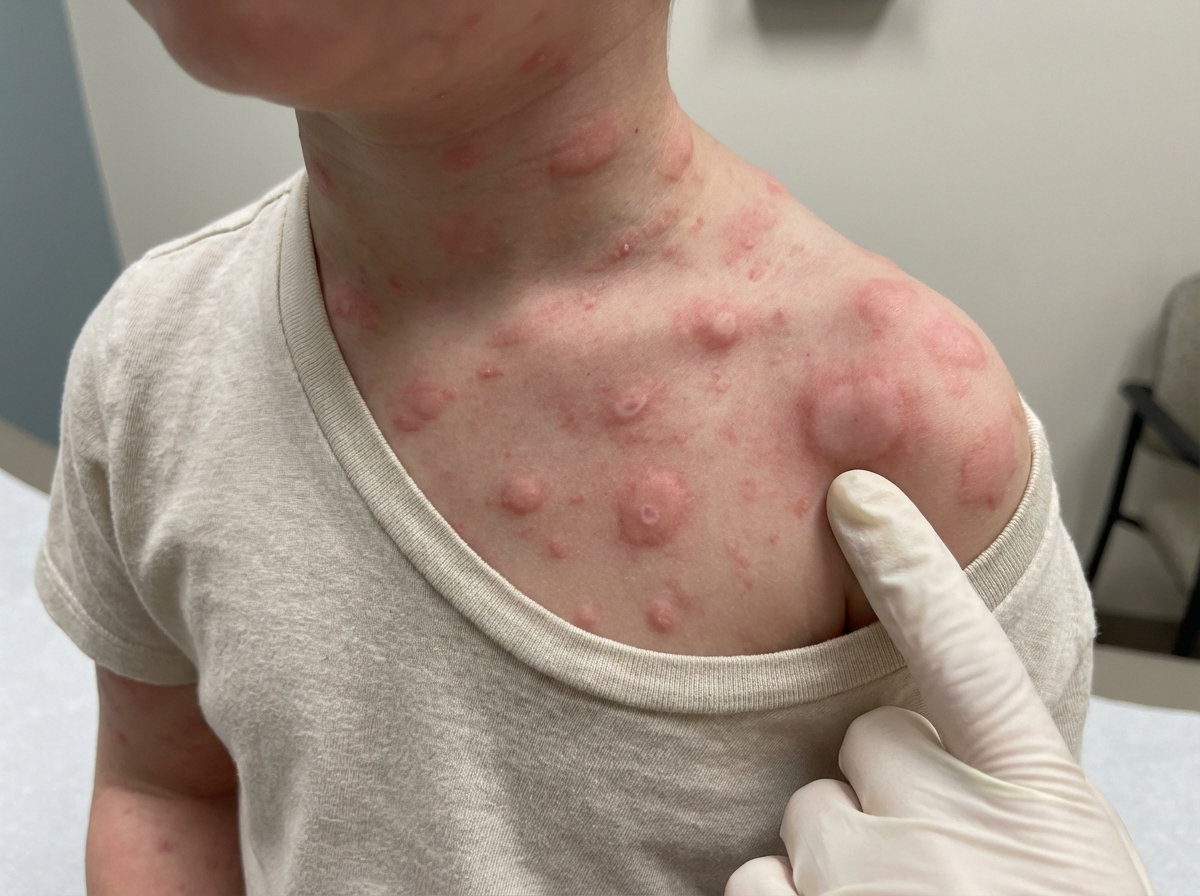
A 4-year-old boy with a rash is brought in by his mother. The patient’s mother says that his symptoms started acutely a few hours ago after they had eaten shellfish at a restaurant which has progressively worsened. She says that the rash started with a few bumps on his neck and chest but quickly spread to involve his arms and upper torso. The patient says the rash makes him uncomfortable and itches badly. He denies any fever, chills, night sweats, dyspnea, or similar symptoms in the past. Past medical history is significant for a history of atopic dermatitis at the age of 9 months which was relieved with some topical medications. The patient is afebrile and his vital signs are within normal limits. On physical examination, the rash consists of multiple areas of erythematous, raised macules that blanch with pressure as shown in the exhibit (see image). There is no evidence of laryngeal swelling and his lungs are clear to auscultation. Which of the following is the best course of treatment for this patient’s most likely condition?
A 42-year-old female complains of feeling anxious and worrying about nearly every aspect of her daily life. She cannot identify a specific cause for these symptoms and admits that this tension is accompanied by tiredness and difficulty falling asleep. To treat this problem, the patient is prescribed sertraline. She endorses a mild improvement with this medication, and over the next several months, her dose is increased to the maximum allowed dose with modest improvement. Her psychiatrist adds an adjunctive treatment, a medication which notably lacks any anticonvulsant or muscle relaxant properties. This drug most likely acts at which of the following receptors?
A 5-year-old girl is brought to the physician for evaluation of a pruritic rash on her face and extremities for the last year that increases with sun exposure. Her parents report that she often seems clumsy and has had several falls in the last two weeks. Physical examination shows an erythematous, scaly rash with hyperpigmentation over the nasal bridge and cheeks as well as on the dorsal forearms and hands. Urinalysis shows high levels of neutral amino acids. The most appropriate treatment for this patient's condition includes administration of an agent that is associated with which of the following adverse effects?
A 25-year-old man is brought to the emergency department by paramedics with a seizure lasting over 30 minutes. The patient's neighbors found him outside his apartment with all four limbs flailing and not responding to his name. No significant past medical history. On physical examination, the patient continues to be unresponsive and slightly cyanotic with irregular breathing. His teeth are clenched tightly. Intravenous glucose and an anticonvulsant medication are administered. Which of the following is the mechanism of action of the drug that was most likely administered to stop this patient’s seizure?
A 23-year-old woman makes an appointment with a dermatologist for treatment of acne. As a result, she feels uncomfortable in public and feels as though everyone is looking at the pimples on her face. She cleans her face several times a day with face wash and avoids using make-up. She has tried many face creams and scar removal creams to help improve the condition of her skin, but nothing has worked. On examination, she has pustular acne on her cheeks and forehead. The physician prescribes an antibiotic along with isotretinoin. Which of the following drugs would you recommend in conjunction with isotretinoin?
A 67-year-old man presents to his primary care physician primarily complaining of a tremor. He said that his symptoms began approximately 1 month ago, when his wife noticed his right hand making "abnormal movements" while watching television. His tremor worsens when he is distracted and improves with purposeful action, such as brushing his teeth or combing his hair. He reports having occasional headaches during times of stress. His wife notices he walks with "poor" posture and he finds himself having trouble staying asleep. He has a past medical history of migraine, generalized anxiety disorder, hypertension, and hyperlipidemia. On physical exam, the patient has a tremor that improves with extension of the arm. On gait testing, the patient has a stooped posture and takes short steps. Which of the following is the most effective treatment for this patient's symptoms?
A 20-year-old college student presents to the emergency room complaining of insomnia for the past 48 hours. He explains that although his body feels tired, he is "full of energy and focus" after taking a certain drug an hour ago. He now wants to sleep because he is having hallucinations. His vital signs are T 100.0 F, HR 110 bpm, and BP of 150/120 mmHg. The patient states that he was recently diagnosed with "inattentiveness." Which of the following is the mechanism of action of the most likely drug causing the intoxication?
A scientist is studying a protein that is present on the plasma membrane of cells. He therefore purifies the protein in a lipid bilayer and subjects it to a number of conditions. His investigations show that the protein has the following properties: 1) It is able to change ion concentrations across the membrane without addition of ATP to the solution. 2) Its activity increases linearly with substrate concentration without any saturation even at mildly supraphysiologic conditions. 3) In some states the protein leads to an ion concentration change; whereas, it has no effect in other states. 4) Changing the electrical charge across the membrane does not affect whether the protein has activity. 5) Adding a small amount of an additional substance to the solution reliably increases the protein's activity. These findings are consistent with a protein with which of the following functions?
A 31-year-old man presents to his primary care physician endorsing three months of decreased sleep. He reports an inability to fall asleep; although once asleep, he generally sleeps through the night and wakes up at a desired time. He has instituted sleep hygiene measures, but this has not helped. He has not felt anxious or depressed and is otherwise healthy. You prescribe him a medication that has the potential side effect of priapism. From which of the following locations is the neurotransmitter affected by this medication released?
Practice by Chapter
Acetylcholine receptors and function
Practice Questions
Cholinergic agonists (direct and indirect)
Practice Questions
Muscarinic antagonists
Practice Questions
Nicotinic antagonists
Practice Questions
Neuromuscular blocking agents
Practice Questions
Adrenergic receptor subtypes
Practice Questions
Alpha-adrenergic agonists
Practice Questions
Beta-adrenergic agonists
Practice Questions
Alpha-adrenergic antagonists
Practice Questions
Beta-adrenergic antagonists
Practice Questions
Sympathomimetics
Practice Questions
Autonomic drug interactions
Practice Questions
Clinical applications in autonomic disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
