Antibiotics — MCQs

On this page
A 63-year-old man with non-Hodgkin lymphoma is brought to the emergency department because of fever and confusion that have progressively worsened over the past 3 days. He also has a 3-day history of loose stools. He returned from France 2 weeks ago where he stayed in the countryside and ate typical French cuisine, including frog, snail, and various homemade cheeses. His last chemotherapy cycle was 3 weeks ago. He is oriented to person but not to place or time. His temperature is 39.5°C (103.1°F), pulse is 110/min, and blood pressure is 100/60 mm Hg. Examination shows cervical and axillary lymphadenopathy. The lungs are clear to auscultation. There is involuntary flexion of the bilateral hips and knees with passive flexion of the neck. Neurologic examination shows no focal findings. Laboratory studies show: Hemoglobin 9.3 g/dL Leukocyte count 3600/mm3 Platelet count 151,000/mm3 Serum Na+ 134 mEq/L Cl- 103 mEq/L K+ 3.7 mEq/L Glucose 102 mg/dL Creatinine 1.3 mg/dL A lumbar puncture is performed. Cerebrospinal fluid analysis shows a leukocyte count of 1200/mm3 (76% segmented neutrophils, 24% lymphocytes), a protein concentration of 113 mg/dL, and a glucose concentration of 21 mg/dL. The results of blood cultures are pending. Which of the following is the most appropriate initial pharmacotherapy?
A 60-year-old woman presents to the physician with a 2-day history of fever and painful swelling of the left knee. She was diagnosed with rheumatoid arthritis about 15 years ago and has a 7-year history of diabetes mellitus. Over the past year, she has been admitted to the hospital twice for acute, painful swelling of the knees and hands. She is on insulin therapy and takes methotrexate, metformin, aspirin, and prednisolone 5 mg/day. Her temperature is 38.5°C (101.3°F), pulse is 86/min, respirations are 14/min, and blood pressure is 125/70 mm Hg. A finger-stick glucose test shows 230 mg/dL. Her left knee is diffusely swollen, warm, and painful on both active and passive motion. There is evidence of deformity in several small joints of the hands and feet without any acute swelling or pain. Physical examination of the lungs, abdomen, and perineum shows no abnormalities. The synovial fluid analysis shows the following: Color turbid, purulent, gray Viscosity reduced WBC 25,000/µL–250,000/µL Neutrophils > 90% Crystals may be present (presence indicates coexistence, but does not rule out infection) Which of the following is the most appropriate initial pharmacotherapy in this patient?
A 28-year-old man presents to the Emergency Department after a window he was installing fell on him. The patient complains of left ocular pain, blurred vision, and obscured lower portion of the left visual field. The patient’s vital signs are as follows: blood pressure 140/80 mm Hg, heart rate 88/min, respiratory rate 14/min, and temperature 36.9℃ (98.4℉). On physical examination, he has multiple superficial lacerations on his face, arms, and legs. Examination of his right eye shows a superficial upper eyelid laceration. Examination of the left eye shows conjunctival hyperemia, peaked pupil, iridial asymmetry, hyphema, and vitreous hemorrhage. The fundus is hard to visualize due to the vitreous hemorrhage. The visual acuity is 20/25 in the right eye and difficult to evaluate in the left. Which of the following is a proper step to undertake in the diagnosis and management of this patient?
An 18-year old college freshman presents to his university clinic because he has not been feeling well for the past two weeks. He has had a persistent headache, occasional cough, and chills without rigors. The patient’s vital signs are normal and physical exam is unremarkable. His radiograph shows patchy interstitial lung infiltrates and he is diagnosed with atypical pneumonia. The patient is prescribed azithromycin and takes his medication as instructed. Despite adherence to his drug regimen, he returns to the clinic one week later because his symptoms have not improved. The organism responsible for this infection is likely resistant to azithromycin through which mechanism?
A 17-year-old girl comes to the physician because of a 2-day history of pain in her right knee. Last week she had right wrist pain. She has no history of recent trauma. She returned from summer camp in Connecticut 2 weeks ago. She is sexually active with one male partner and uses an oral contraceptive. Her temperature is 38°C (100.4°F). Examination shows several painless vesiculopustular lesions on the back and one lesion on the right sole of the foot. There is swelling of the right knee with tenderness to palpation. Passive extension of the right wrist and fingers elicits pain. Which of the following is the most likely diagnosis?
A 22-year-old female is brought to the emergency department by her roommate with a one day history of fever and malaise. She did not feel well after class the previous night and has been in her room since then. She has not been eating or drinking due to severe nausea. Her roommate checked on her one hour ago and was alarmed to find a fever of 102°F (38.9°C). On physical exam temperature is 103°F (40°C), blood pressure is 110/66 mmHg, pulse is 110/min, respirations are 23/min, and pulse oximetry is 98% on room air. She refuses to move her neck and has a rash on her trunk. You perform a lumbar puncture and the CSF analysis is shown below. Appearance: Cloudy Opening pressure: 180 mm H2O WBC count: 150 cells/µL (93% PMN) Glucose level: < 40 mg/dL Protein level: 50 mg/dL Gram stain: gram-negative diplococci Based on this patient's clinical presentation, which of the following should most likely be administered?
A 12-year-old girl is brought to the physician by her mother because of high fever and left ankle and knee joint swelling. She had a sore throat 3 weeks ago. There is no family history of serious illness. Her immunizations are up-to-date. She had an episode of breathlessness and generalized rash when she received dicloxacillin for a skin infection 2 years ago. She appears ill. Her temperature is 38.8°C (102.3°F), pulse is 87/min, and blood pressure is 98/62 mm Hg. Examination shows left ankle and knee joint swelling and tenderness; range of motion is limited. Breath sounds over both lungs are normal. A grade 3/6 holosytolic murmur is heard best at the apex. Abdominal examination is normal. Which of the following is the most appropriate pharmacotherapy?
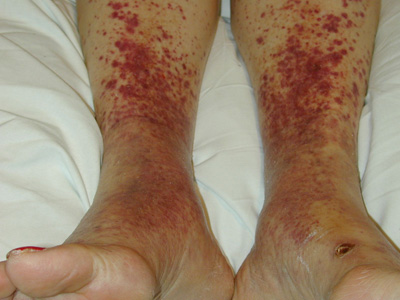
A 26-year-old male with no significant past medical history goes camping with several friends in Virginia. Several days after returning, he begins to experience fevers, headaches, myalgias, and malaise. He also notices a rash on his wrists and ankles (Figure A). Which of following should be initiated for treatment of his condition?
A 60-year-old diabetic male presents to your clinic for right ear pain. The patient reports noting worsening right ear pain for three weeks, purulent otorrhea initially which has resolved, and facial asymmetry for the past several days. He reports being poorly compliant with his diabetes medication regimen. His temperature is 100.4 deg F (38 deg C), blood pressure is 140/90 mmHg, pulse is 90/min, and respirations are 18/min. On physical exam, the patient’s right external auditory canal is noted to have granulation tissue at the bony cartilaginous junction. He is also noted to have right facial droop. Which of the following is the best next step in treatment?
Ten days after being discharged from the hospital, a 42-year-old man comes to the emergency department because of reduced urine output for 3 days. Physical examination is normal. Serum creatinine concentration is 2.9 mg/dL. Urinalysis shows brownish granular casts and 2+ proteinuria. Renal biopsy shows patchy necrosis of the proximal convoluted tubule with sloughing of tubular cells into the lumen and preservation of tubular basement membranes. Administration of which of the following drugs during this patient's hospitalization is most likely the cause of the observed decrease in renal function?
Practice by Chapter
Penicillins and beta-lactamase inhibitors
Practice Questions
Cephalosporins
Practice Questions
Carbapenems and monobactams
Practice Questions
Fluoroquinolones
Practice Questions
Aminoglycosides
Practice Questions
Macrolides, ketolides, and lincosamides
Practice Questions
Tetracyclines and glycylcyclines
Practice Questions
Sulfonamides and trimethoprim
Practice Questions
Vancomycin and other glycopeptides
Practice Questions
Oxazolidinones and streptogramins
Practice Questions
Daptomycin and lipopeptides
Practice Questions
Polymyxins
Practice Questions
Antibiotic resistance mechanisms
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
