Antibiotics — MCQs

On this page
A 33-year-old man presents to the emergency department complaining of weakness and fatigue. He states that his symptoms have worsened over the past day. He has a past medical history of IV drug abuse and alcoholism and he currently smells of alcohol. His temperature is 102°F (38.9°C), blood pressure is 111/68 mmHg, pulse is 110/min, respirations are 17/min, and oxygen saturation is 98% on room air. Physical exam is notable for focal tenderness over the lumbar spine. Initial lab values and blood cultures are drawn and are notable for leukocytosis and an elevated C-reactive protein (CRP). Which of the following is the best treatment for this patient?
A 39-year-old man presents to his primary care physician with a high fever, cough, and malaise. One week ago, he returned from a vacation to Hawaii where he went waterskiing with his family. Three days before presentation, he started experiencing intermittent abdominal pain, which was followed by flu-like symptoms, itchiness in his eyes, and photosensitivity. On presentation, his temperature is 103°F (39.4°C), blood pressure is 114/72 mmHg, pulse is 105/min, and respirations are 18/min. Physical exam reveals conjunctivitis and mild jaundice. Which of the following treatments could be used to treat this patient's condition?
A 19-year-old woman presents to the family medicine clinic after noticing swelling of her right index finger a few hours ago. She has no past medical history and takes no prescription medications. She takes ibuprofen occasionally, as needed. She says that she has smoked a few cigarettes a day for the last year. On further questioning, the patient says that she has a dog and a cat at home. Her blood pressure is 108/67 mm Hg, heart rate is 94/min, respiratory rate is 12/min, and temperature is 37.8°C (100.1°F). On physical examination, the physician notices 2 clean puncture wounds with localized erythema and induration on the dorsum of the right second digit. Capillary refill is 2 seconds. Sensory and motor function are intact bilaterally. Which of the following is the most appropriate treatment choice for this patient?
Five days after being admitted to the hospital for an open cholecystectomy, a 56-year-old woman develops difficulty breathing. She also has fevers, chills, and malaise. She has a cough productive of minimal amounts of yellowish-white sputum that started two days prior. She has type 2 diabetes mellitus, hypertension, and a history of gallstones. Her current medications include metformin, lisinopril, and atorvastatin. Her temperature is 39.5°C (103.1°F), pulse is 104/minute, blood pressure is 94/68 mm Hg, and respirations are 30/minute. Pulse oximetry on 2 L of oxygen via nasal cannula shows an oxygen saturation of 92%. Examination reveals decreased breath sounds over the right lung base. Abdominal examination shows a well-healing scar without erythema or discharge in the right upper quadrant. The skin is warm and well-perfused. Her hemoglobin concentration is 10.5 g/dL, leukocyte count is 16,000/mm3, platelet count is 345,000/mm3, and creatinine is 1.5 mg/dL. She is admitted to the ICU and started on IV fluids. Blood and urine for cultures are obtained. X-ray of the chest reveals a right sided pleural effusion. Which of the following is the next best step in management?
A 73-year-old man is brought to the emergency department because of fever, headaches, and confusion for the past 24 hours. Three years ago, he underwent heart transplantation because of congestive heart failure. His temperature is 38.1°C (100.5°F). He is oriented only to person. Physical examination shows nuchal rigidity. A cerebrospinal fluid culture on blood agar grows colonies of a gram-positive bacillus surrounded by a narrow transparent rim. Administration of which of the following antibiotics is most likely to be effective in the treatment of this patient's condition?
A 72-year-old man is admitted to the hospital with productive cough and fever. A chest radiograph is obtained and shows lobar consolidation. The patient is diagnosed with pneumonia. He has a history of penicillin allergy. The attending physician orders IV levofloxacin as empiric therapy. On morning rounds the next day, the team discovers that the patient was administered ceftriaxone instead of levofloxacin. The patient has already received a full dose of ceftriaxone and had no signs of allergic reaction, and his pneumonia appears to be improving clinically. What is the most appropriate next step?
Three days after undergoing outpatient percutaneous coronary intervention with stent placement in the right coronary artery, a 60-year-old woman has left-sided painful facial swelling. The pain is worse while chewing. The patient has hypertension and coronary artery disease. Her current medications include enalapril, metoprolol, aspirin, clopidogrel, simvastatin, and a multivitamin. She does not smoke or drink alcohol. Her temperature is 38.1°C (100.5°F), pulse is 72/min, respirations are 16/min, and blood pressure is 128/86 mm Hg. Examination shows swelling and tenderness of the left parotid gland. Intraoral examination shows erythema with scant purulent drainage. Which of the following is the most appropriate next step in management?
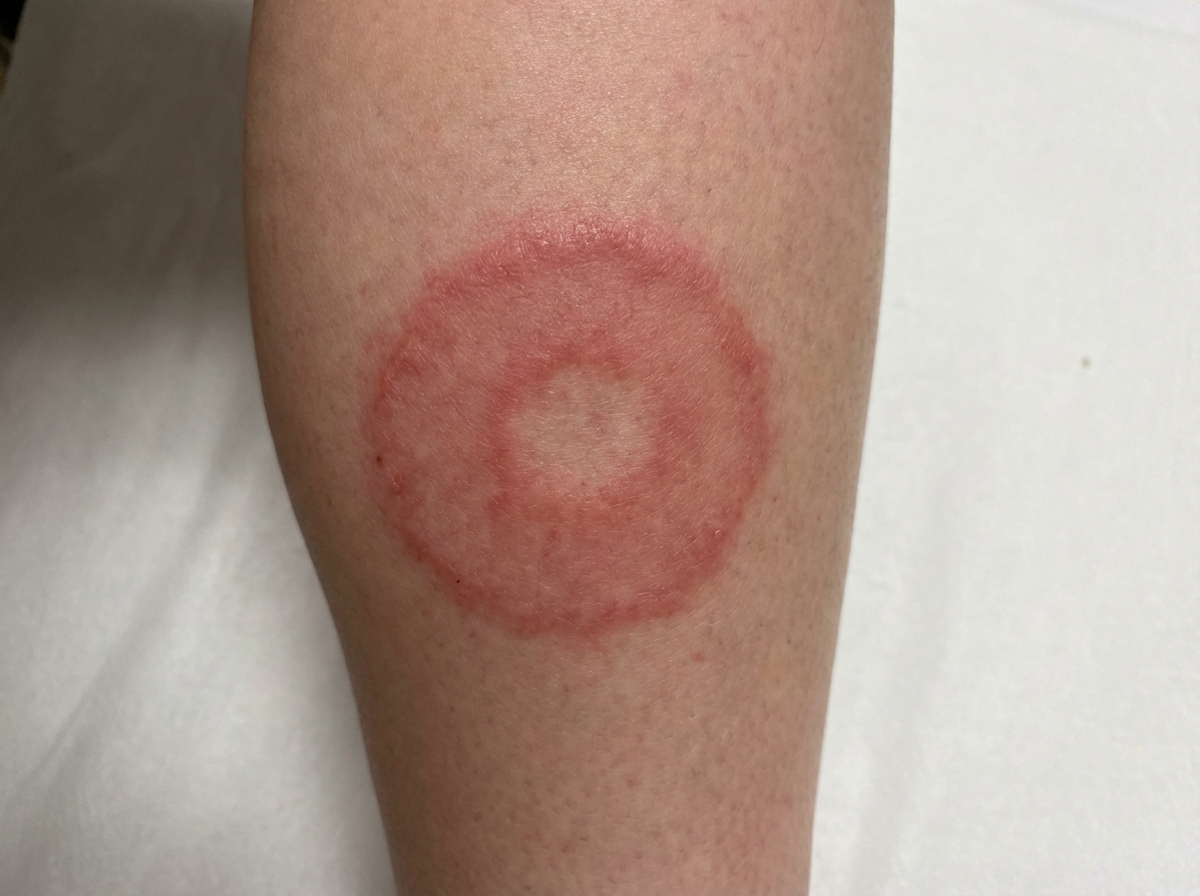
A 27-year-old man visits the office with complaints of pain in his lower limb muscles and joints. He cannot remember exactly when it started, but it intensified after his recent hiking trip. He is a hiking enthusiast and mentions having gone on a recent trekking expedition in Connecticut. He does not recall any particular symptoms after the hike except for a rash on his left calf with distinct borders (image provided in the exhibit). The patient does not complain of fever, chills or any changes in his vision. His vital signs show a blood pressure of 120/70 mm Hg, a pulse of 97/min, and respirations of 18/min. There is tenderness in his left calf with a decreased range of motion in the left knee joint. No joint effusions are noted. Which of the following would be the next best step in the management of this patient?
A 9-year-old boy is brought to the pediatrician by his parents with a fever, cough, and cold symptoms that began 7 days ago. He has been complaining of right ear pain for the last 2 days. He is otherwise a completely healthy child with no known medical conditions. On physical examination, the temperature is 39.0°C (102.2°F), the pulse is 114 /min, the blood pressure is 106/74 mm Hg, and the respiratory rate is 26/min. On chest auscultation, rales are heard over the right subscapular region accompanied by bronchial breathing in the same region. Examination of the right external auditory canal reveals an erythematous, bulging tympanic membrane. The results of a complete blood count are as follows: Hemoglobin % 11 g/dL WBC count 12,000/mm3 Neutrophils 88% Lymphocytes 10% Monocytes 2% Platelet count 200,000/mm3 A chest radiograph shows a focal homogenous opacity in the right lung suggestive of consolidation. Bacteriologic cultures of the blood, nasopharynx, and sputum grew Moraxella catarrhalis. Which of the following is the antibiotic of choice?
A 64-year-old female with type 2 diabetes mellitus comes to the physician because of a 1-week history of painful red swelling on her left thigh. Examination shows a 3- x 4-cm, tender, fluctuant mass. Incision and drainage of the abscess are performed. Culture of the abscess fluid grows gram-positive, coagulase-positive cocci that are resistant to oxacillin. Which of the following best describes the mechanism of resistance of the causal organism to oxacillin?
Practice by Chapter
Penicillins and beta-lactamase inhibitors
Practice Questions
Cephalosporins
Practice Questions
Carbapenems and monobactams
Practice Questions
Fluoroquinolones
Practice Questions
Aminoglycosides
Practice Questions
Macrolides, ketolides, and lincosamides
Practice Questions
Tetracyclines and glycylcyclines
Practice Questions
Sulfonamides and trimethoprim
Practice Questions
Vancomycin and other glycopeptides
Practice Questions
Oxazolidinones and streptogramins
Practice Questions
Daptomycin and lipopeptides
Practice Questions
Polymyxins
Practice Questions
Antibiotic resistance mechanisms
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
