Antibiotics — MCQs

On this page
A 70-year-old man presents with fever, headache, and vomiting. He says that symptoms onset acutely 2 days ago and have not improved. He also reports associated weakness and chills. Past medical history is significant for occasional heartburn. His temperature is 39.4°C (103.0°F), the pulse rate is 124/min, the blood pressure is 130/84 mm Hg, and the respiratory rate is 22/min. On physical examination, there is significant nuchal rigidity. No signs of raised intracranial pressure are present. A lumbar puncture is performed and cerebrospinal fluid (CSF) analysis shows lymphocyte-dominant pleocytosis with increased CSF protein levels. Bacteriological culture of the CSF reveals the growth of Listeria monocytogenes. Which of the following antibiotics is the best choice for the treatment of this patient?
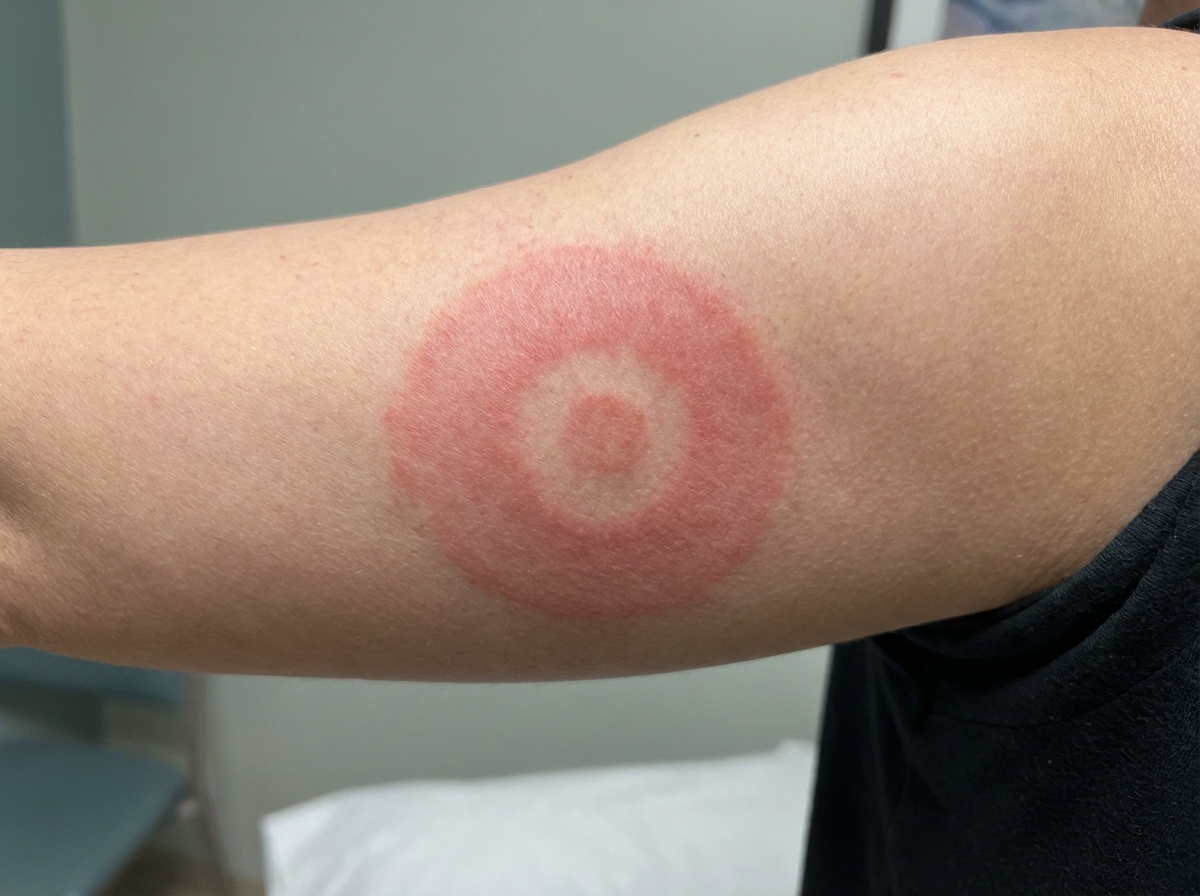
A 28-year-old man presents with fever, chills, and malaise which began 5 days ago. He also mentions that the back of his right upper arm feels itchy. He says he works as a forest guide and recently came back from a forest expedition. Upon asking, he reports that the forest where he works is infested with ticks. His temperature is 38.3°C (100.9°F), the pulse is 87/min, the respiratory rate is 15/min, and the blood pressure is 122/90 mm Hg. On physical examination, there is a rash present on the posterior aspect of his upper right arm which is shown in the image. Which of the following medications is the best course of treatment for this patient?
A 65-year-old man with chronic obstructive lung disease, depression, and type 2 diabetes mellitus comes to the physician with fever, chills, dyspnea, and a productive cough for 5 days. His temperature is 38.8°C (101.8°F) and respirations are 30/min. An x-ray of the chest shows a right lower lobe infiltrate, and sputum culture grows bacteria that are sensitive to fluoroquinolone antibiotics. Pharmacotherapy with oral moxifloxacin is initiated. Three days later, the patient continues to have symptoms despite being compliant with the antibiotic. Serum moxifloxacin levels are undetectable. The lack of response to antibiotic therapy in this patient is most likely due to the concurrent ingestion of which of the following medications?
A 70-year-old Caucasian woman presents to the emergency department complaining of abdominal pain. She is oriented to person but is slow to answer questions and cannot name her location. She is afebrile on exam and endorses mild suprapubic tenderness. Her urine culture was positive for leukocyte esterase and nitrites. She was prescribed appropriate treatments. On follow-up, she complains of a new rash. In the past few days she has noticed that her skin becomes very red and more easily sunburns. Per the patient, her symptoms have resolved and her initial infection has cleared. Which of the following antibiotics was most likely prescribed to this patient?
A 23-year-old woman comes to the physician because of increased urinary frequency and pain on urination for two days. She has had three similar episodes over the past year that resolved with antibiotic treatment. She has no history of serious illness. She is sexually active with one male partner; they do not use barrier contraception. Upon questioning, she reports that she always urinates and cleans herself after sexual intercourse. She drinks 2–3 liters of fluid daily. Her only medication is a combined oral contraceptive. Her temperature is 36.9°C (98.4°F), pulse is 65/min, and blood pressure is 122/65 mm Hg. Examination shows mild tenderness to palpation in the lower abdomen. The remainder of the examination shows no abnormalities. Urinalysis shows WBCs and rare gram-positive cocci. Which of the following is the most appropriate recommendation to prevent similar episodes in the future?
A 19-year-old woman presents to the dermatology clinic for a follow-up of worsening acne. She has previously tried topical tretinoin as well as topical and oral antibiotics with no improvement. She recently moved to the area for college and says the acne has caused significant emotional distress when it comes to making new friends. She has no significant past medical or surgical history. Family and social history are also noncontributory. The patient’s blood pressure is 118/77 mm Hg, the pulse is 76/min, the respiratory rate is 17/min, and the temperature is 36.6°C (97.9°F). Physical examination reveals erythematous skin lesions including both open and closed comedones with inflammatory lesions overlying her face, neck, and upper back. The patient asks about oral isotretinoin. Which of the following is the most important step in counseling this patient prior to prescribing oral isotretinoin?
A 25-year-old man presents with a nodule on his right foot. He says that he first noticed the nodule last week. It has not undergone any change in size and color. He denies any history of trauma or fever. Past medical history is significant for HIV, diagnosed 6 years ago. He is currently not on antiretroviral therapy. His last CD4+ T cell count was 0.19 x 109/L. He is afebrile, and his vital signs are within normal limits. On physical examination, there is a 3 cm x 4 cm nodule on the right foot, tan brown in color, non-tender, and covered with a fine scale. A biopsy of the nodule is performed and histopathological analysis reveals the proliferation of blood vessels with overgrown endothelial cells. Histological staining of the biopsy tissue reveals gram-negative bacilli. Which of the following is the best course of treatment for this patient?
A 7-year-old boy is brought to the physician because of a 4-day history of fever, headache, earache, and sore throat that is worse when swallowing. He has not had a runny nose or cough. He had a similar problem 1 year ago for which he was prescribed amoxicillin, but after developing a skin rash and facial swelling he was switched to a different medication. His immunizations are up-to-date. He is at the 75th percentile for height and the 50th percentile for weight. His temperature is 38.9°C (102°F), pulse is 136/min, and respirations are 28/min. Examination of the oral cavity reveals a coated tongue, red uvula, and enlarged right tonsil covered by a whitish membrane. The deep cervical lymph nodes are enlarged and tender. A throat swab is taken for culture. What is the next most appropriate step in the management of this patient?
A 3-year-old girl is brought to the physician for a well-child visit. Her father is concerned about the color and strength of her teeth. He says that most of her teeth have had stains since the time that they erupted. She also has a limp when she walks. Examination shows brownish-gray discoloration of the teeth. She has lower limb length discrepancy; her left knee-to-ankle length is 4 cm shorter than the right. Which of the following drugs is most likely to have been taken by this child's mother when she was pregnant?
A 24-year-old man presents to the emergency department for severe abdominal pain for the past day. The patient states he has had profuse, watery diarrhea and abdominal pain that is keeping him up at night. The patient also claims that he sees blood on the toilet paper when he wipes and endorses having lost 5 pounds recently. The patient's past medical history is notable for IV drug abuse and a recent hospitalization for sepsis. His temperature is 99.5°F (37.5°C), blood pressure is 120/68 mmHg, pulse is 100/min, respirations are 14/min, and oxygen saturation is 98% on room air. On physical exam, you note a young man clutching his abdomen in pain. Abdominal exam demonstrates hyperactive bowel sounds and diffuse abdominal tenderness. Cardiopulmonary exam is within normal limits. Which of the following is the next best step in management?
Practice by Chapter
Penicillins and beta-lactamase inhibitors
Practice Questions
Cephalosporins
Practice Questions
Carbapenems and monobactams
Practice Questions
Fluoroquinolones
Practice Questions
Aminoglycosides
Practice Questions
Macrolides, ketolides, and lincosamides
Practice Questions
Tetracyclines and glycylcyclines
Practice Questions
Sulfonamides and trimethoprim
Practice Questions
Vancomycin and other glycopeptides
Practice Questions
Oxazolidinones and streptogramins
Practice Questions
Daptomycin and lipopeptides
Practice Questions
Polymyxins
Practice Questions
Antibiotic resistance mechanisms
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
