Antibiotics — MCQs

On this page
What is the most suitable antibiotic to treat the condition shown in the image ?
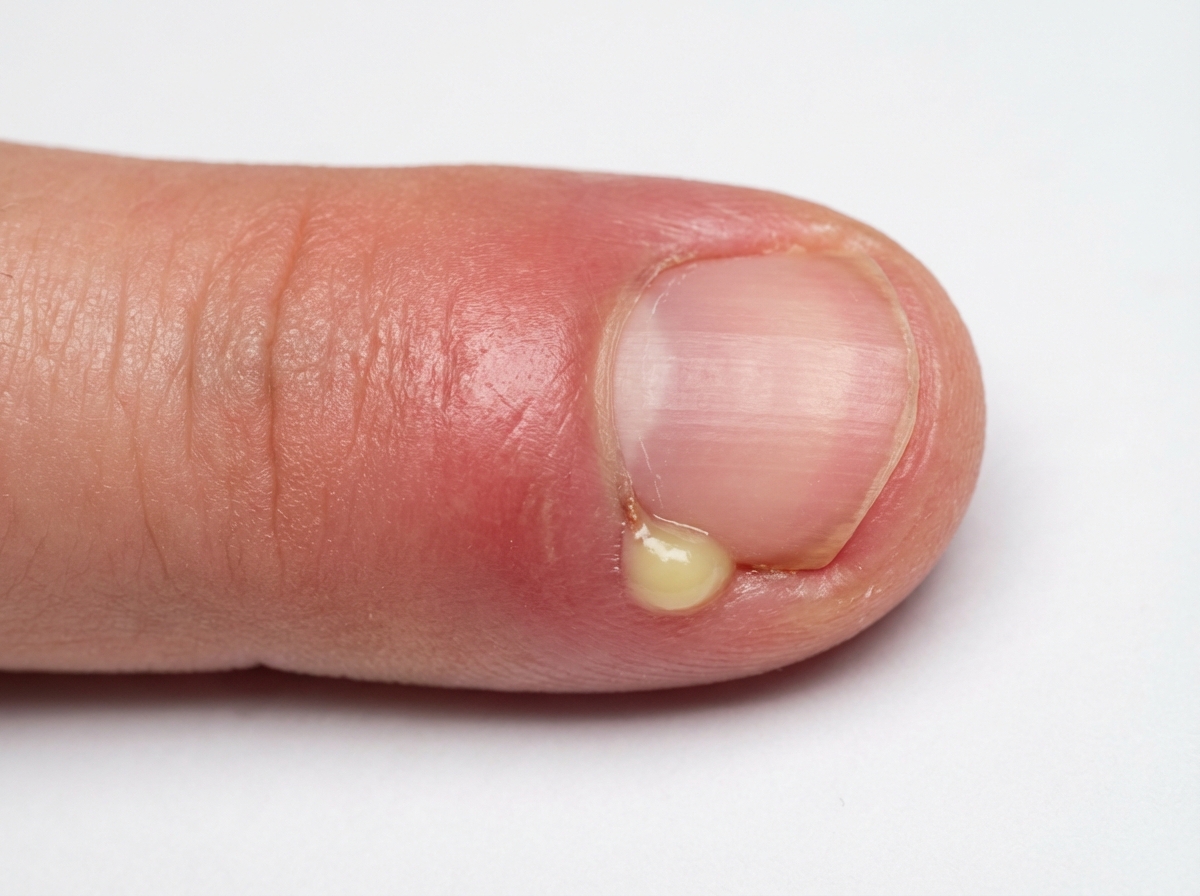
A 57-year-old woman returns to her primary care provider complaining of fever, skin rash, and flank pain. She had just visited her PCP 2 weeks ago complaining of a sore throat and was diagnosed with pharyngitis. She was then given a 10 day prescription for phenoxymethylpenicillin. Today she is on day 6 of her prescription. Her symptoms started yesterday. Past medical history is significant for type 2 diabetes mellitus, essential hypertension, and has gastroesophageal reflux disease. Her medications include metformin, captopril, hydrochlorothiazide, and pantoprazole and a multivitamin that she takes daily. Today her temperature is 38.0°C (100.4°F), the blood pressure is 147/95 mm Hg, and the pulse is 82/min. Physical examination shows a sparse maculopapular rash over her upper trunk. Laboratory results are shown: CBC with Diff Leukocyte count 9,500/mm3 Segmented neutrophils 54% Bands 4% Eosinophils 8% Basophils 0.5% Lymphocytes 30% Monocytes 4% Blood urea nitrogen 25 mg/dL Serum creatinine 2 mg/dL Urinalysis 27 white blood cells/ high powered field 5 red blood cells/high powered field Urine culture No growth after 72 hours A urine cytospin with stained with Wright’s stain shows 4.5% eosinophils. Which of the following is the best initial step in the management of this patient condition?
An 81-year-old man is brought to the emergency department by staff of an assisted living facility where he resides with fever and a cough that produces yellow-green sputum. His temperature is 39.1°C (102.3°F). Physical examination shows diffuse crackles over the right lung fields. An x-ray of the chest shows consolidation in the right lower lobe. Sputum cultures grow an organism that produces blue-green pigments and smells of sweet grapes. Treatment with piperacillin and a second agent is begun. Which of the following is the most likely mechanism of action of the second agent?
A 28-year-old man presents with a complaint of penile discharge. He says that he noticed a yellowish watery discharge from his penis since last week. He adds that he has painful urination only in the mornings, but he sometimes feels a lingering pain in his genital region throughout the day. He denies any fever, body aches, or joint pains. No significant past medical history or current medications. When asked about his social history, he mentions that he has regular intercourse with women he meets in bars, however, he doesn’t always remember to use a condom. Physical examination is unremarkable. The penile discharge is collected and sent for analysis. Ceftriaxone IM is administered, after which the patient is sent home with a prescription for an oral medication. Which of the following oral drugs was most likely prescribed to this patient?
A 45-year-old male presents to the emergency room following a seizure. The patient suffered from an upper respiratory infection complicated by sinusitis two weeks ago. The patient's past medical history is remarkable for hypertension for which he takes hydrochlorathiazide. Temperature is 39.5C, blood pressure is 120/60 mmHg, pulse is 85/min, and respiratory rate is 20/min. Upon interview, the patient appears confused and exhibits photophobia. CSF cultures are obtained. Which of the following is the most appropriate next step in the management of this patient?
A 32-year-old man presents with a fever that has persisted for 3 days. He says that the fever was initially low at around 37.8°C (100.0°F), but, for the past 2 days, it has been around 38.9°C (102.0°F), regardless of his attempts to bring it down. He has also noticed some bumps on his neck. On further questioning, he mentions that he was recently out rabbit hunting with his friends. He is prescribed an antibiotic and requested to follow-up in 2 weeks. On follow-up, the patient seems better, however, he says he now has a slight hearing difficulty. What is the mechanism of action of the drug that was prescribed to this patient?
A 5-year-old girl presents to the emergency room due to difficulty walking. According to her parents, she has been complaining of pain in her right leg for the last few days. Her neighbor’s cat bit her last week and her parents attributed the pain to her healing bite. At the time of the bite they cleaned the wound and irrigated it with sterile saline water from a first aid kit. She has no past medical history and has never been hospitalized. On physical examination her temperature is 102.2°F (39°C), blood pressure is 118/78 mmHg, pulse is 90/min, respirations are 21/min, and pulse oximetry is 99% on room air. The open wound remains present on the thigh with surrounding erythema and edema. MRI is consistent with osteomyelitis. Which of the following is the most appropriate next step in management?
A 66-year-old woman with type 2 diabetes mellitus comes to the physician because of a severely painful right ear with discharge for 10 days. The ear pain was acute in onset and is constant. She has been using over-the-counter eardrops but her symptoms have worsened. Her only medication is insulin, which she uses inconsistently. Her temperature is 39°C (102.2°F), pulse is 108/min, and blood pressure is 130/90 mm Hg. Examination of the right ear shows a swollen pinna and lobule and malodorous purulent discharge; the ear is tender to touch. Posterior auricular lymphadenopathy is present. There is mild hearing loss of the right ear. Otoscopic examination shows a swollen ear canal with granulation tissue. Laboratory studies show: Hemoglobin 13.3 g/dL Hemoglobin A1c 12.2% Leukocyte count 18,300/mm3 Segmented neutrophils 76% Eosinophils 1% Lymphocytes 20% Monocytes 3% Serum Glucose 212 mg/dL Creatinine 1.7 mg/dL A CT scan of the head shows severe thickening and enhancing of the soft tissue of the external auditory canal with patchy destruction of the mastoid process. Culture results of the ear drainage are pending. Which of the following is the most appropriate pharmacotherapy?
A 50-year-old man with acute myeloid leukemia undergoes multiple chemotherapeutic regimens but does not enter remission. His oncologist suggests that he enroll in a trial for a new medication that causes DNA strand breaks and is particularly effective during the G2 phase of the cell cycle. Which of the following anti-cancer agents is this new agent most similar to?
A 35-year-old man comes to the physician because of an ulcer on his penis that he first noticed 4 days ago. He is currently sexually active with multiple male partners and uses condoms inconsistently. Genital examination shows a shallow, nontender ulcer with a smooth base and indurated border along the shaft of the penis. There is bilateral inguinal lymphadenopathy. Darkfield microscopy of a sample from the lesion shows gram-negative, spiral-shaped bacteria. A drug that acts by inhibition of which of the following is the most appropriate treatment for this patient?
Practice by Chapter
Penicillins and beta-lactamase inhibitors
Practice Questions
Cephalosporins
Practice Questions
Carbapenems and monobactams
Practice Questions
Fluoroquinolones
Practice Questions
Aminoglycosides
Practice Questions
Macrolides, ketolides, and lincosamides
Practice Questions
Tetracyclines and glycylcyclines
Practice Questions
Sulfonamides and trimethoprim
Practice Questions
Vancomycin and other glycopeptides
Practice Questions
Oxazolidinones and streptogramins
Practice Questions
Daptomycin and lipopeptides
Practice Questions
Polymyxins
Practice Questions
Antibiotic resistance mechanisms
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
