Growth/Development — MCQs

On this page
A 6-year-old girl is brought to the pediatrician for the first time by her mother. Her mother states that her family just emigrated from China and her daughter has seemed to have difficulty adjusting to the American diet. Specifically, she seems to have abdominal discomfort and increased flatulence whenever she eats milk or cheese. The pediatrician orders a test to diagnose the patient. Which of the following results is most likely to be observed in this patient?
A 5-year-old boy is brought to the emergency department by a neighbor who saw him struck by a car. The man reports that the boy is intellectually disabled, and his parents frequently leave him unattended at home for most of the day. He walks around the neighborhood and sometimes has difficulty finding his way home. Today he was struck by a car that sped off. The man called the boy’s mother by phone, but she said that she was too busy to leave her job and asked the man to take the boy to the emergency department for her. A quick review of the boy's electronic medical record reveals that he has not been seen by a physician in several years and has missed several vaccines. On physical exam, the vital signs are normal. He appears dirty, thin, and small for his age with a large bruise forming on his right hip. Which of the following is the most appropriate term for this type of child abuse?
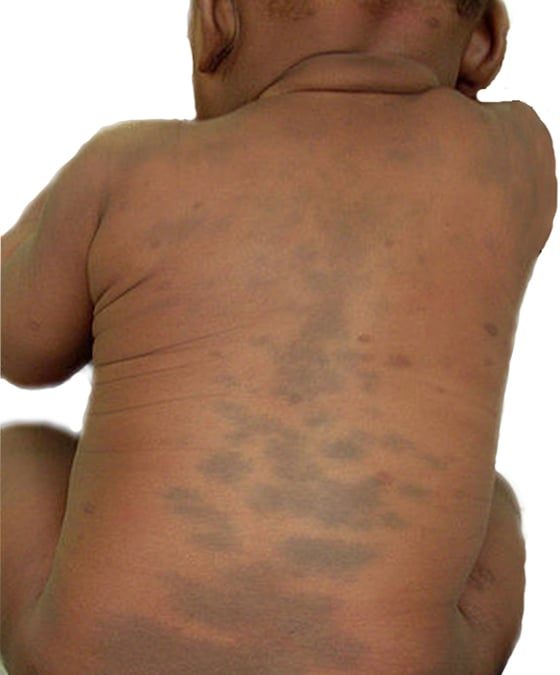
A 2-week-old infant is brought to the physician by her father because of a 1-week history of vaginal discharge. The discharge was initially clear, but now he notices that it is tinged with blood. The father is also concerned about “bruises” on his daughter's back and buttocks. Both parents work so that the infant spends most of her time in daycare or with her aunt. She was born at term following a pregnancy complicated by maternal gonococcal infection that was treated with antibiotics. She appears well. Physical examination shows mild acne across her cheeks and forehead. There are multiple large flat gray-blue patches on her back and buttocks. An image of one of the lesions is shown. Firm breast buds are present. Genitourinary examination shows erythema and swelling of the vulva and vagina with an odorless, blood-stained white discharge. Which of the following is the most appropriate next step in management?
A child with which of the following diseases would have the highest morbidity from being outside during a hot summer day?
A 3-year-old boy is brought to the pediatrician by his parents because of swelling and tenderness of his left upper arm. According to the father, the boy was running in the garden when he fell and injured his arm 2 days ago. His mother had been on a business trip the past week. The boy's father and 18-year-old brother had been taking care of the patient during that time. The mother reports that she noticed her son refusing to use his left arm when she returned from her business trip. Both parents claim there is no history of previous trauma. The boy is at the 60th percentile for height and 40th percentile for weight. The patient clings to his mother when approached by the physician. Physical examination shows swelling and bruising of the medial left upper arm and tenderness along the 8th rib on the left side. An x-ray of the arm and chest shows a nondisplaced spiral fracture of the left proximal humeral shaft and a fracture with callus formation of the left 8th rib. Which of the following is the most appropriate next step in management?
A three-year-old girl presents to general pediatrics clinic for a well-child visit. Her mother reports that she has been growing and developing normally but because of new behaviors she has noticed with her child, she is concerned of possible abuse by the child's stepfather. Vital signs are stable and the physical examination is within normal limits. The child has no visual signs of abuse. Which of the following, if reported by the mother would signify potential sexual abuse in the child?
A new mother brings in her 4-week-old son who has no significant past medical history but she complains of a new, itchy rash on his body. The patient has an older sister who developed similar symptoms when she was around the same age. The patient's blood pressure is 75/50 mm Hg, pulse is 140/min, respiratory rate is 40/min, and temperature is 37.3°C (99.1°F). Physical examination reveals confluent, erythematous patches and plaques with tiny vesicles and scaling overlying his lower back and abdomen. When questioned about possible etiologies, the mother notes that she has been bathing the patient at least twice a day. Which of the following statements is most appropriate for this patient?
A 5-year-old child whose family recently immigrated from Africa is brought in for a wellness visit. The boy appears indifferent, doesn’t seem to make eye contact, and keeps to himself. Upon examination, it is noted that his height and weight are below the 5th percentile. Furthermore, his abdomen is protuberant, and there are multiple zones of hyper- and hypopigmentation and desquamation of the skin. Upon palpation of the abdomen, he is found to have hepatomegaly, and lower extremity inspection reveals pitting edema. Which of the following is the cause of this child’s condition?
A 5 month-old boy with no significant past medical, surgical, or family history is brought the pediatrician by his parents for a new rash. The parents state that the rash started several weeks earlier and has not changed. The boy has breastfed since birth and started experimenting with soft foods at the age of 4 months. Physical examination reveals erythematous plaques with shiny, yellow scales over the scalp and external ears. Vital signs are within normal limits. Complete blood count is as follows: WBC 8,300 cells/ml3 Hct 46.1% Hgb 17.1 g/dL Mean corpuscular volume (MCV) 88 fL Platelets 242 Which of the following is the most likely diagnosis?
An infant boy is brought to the physician for a well-child examination. He was born at term and has been healthy since. He is beginning to crawl but can not yet walk or run. He feeds himself small foods and can bang 2 cubes together. He is just beginning to successfully use a pincer grasp. He has stranger anxiety. He is at the 40th percentile for height and weight. Physical examination shows no abnormalities. Which of the following additional skills or behaviors would be expected in a healthy patient of this developmental age?
Practice by Chapter
Normal growth patterns
Practice Questions
Growth charts and interpretation
Practice Questions
Failure to thrive evaluation
Practice Questions
Short stature workup
Practice Questions
Tall stature evaluation
Practice Questions
Obesity in children
Practice Questions
Nutritional assessment tools
Practice Questions
Puberty stages (Tanner stages)
Practice Questions
Precocious puberty
Practice Questions
Delayed puberty
Practice Questions
Growth hormone disorders
Practice Questions
Impact of chronic disease on growth
Practice Questions
Catch-up growth
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
