Growth/Development — MCQs

On this page
A 7-year-old boy is brought to the physician by his mother because of a limp for the last 3 weeks. He has also had right hip pain during this period. The pain is aggravated when he runs. He had a runny nose and fever around a month ago that resolved with over-the-counter medications. He has no history of serious illness. His development is adequate for his age. His immunizations are up-to-date. He appears healthy. He is at the 60th percentile for height and at 65th percentile for weight. Vital signs are within normal limits. Examination shows an antalgic gait. The right groin is tender to palpation. Internal rotation and abduction of the right hip is limited by pain. The remainder of the examination shows no abnormalities. His hemoglobin concentration is 11.6 g/dL, leukocyte count is 8,900/mm3, and platelet count is 130,000/mm3. An x-ray of the pelvis is shown. Which of the following is the most likely underlying mechanism?
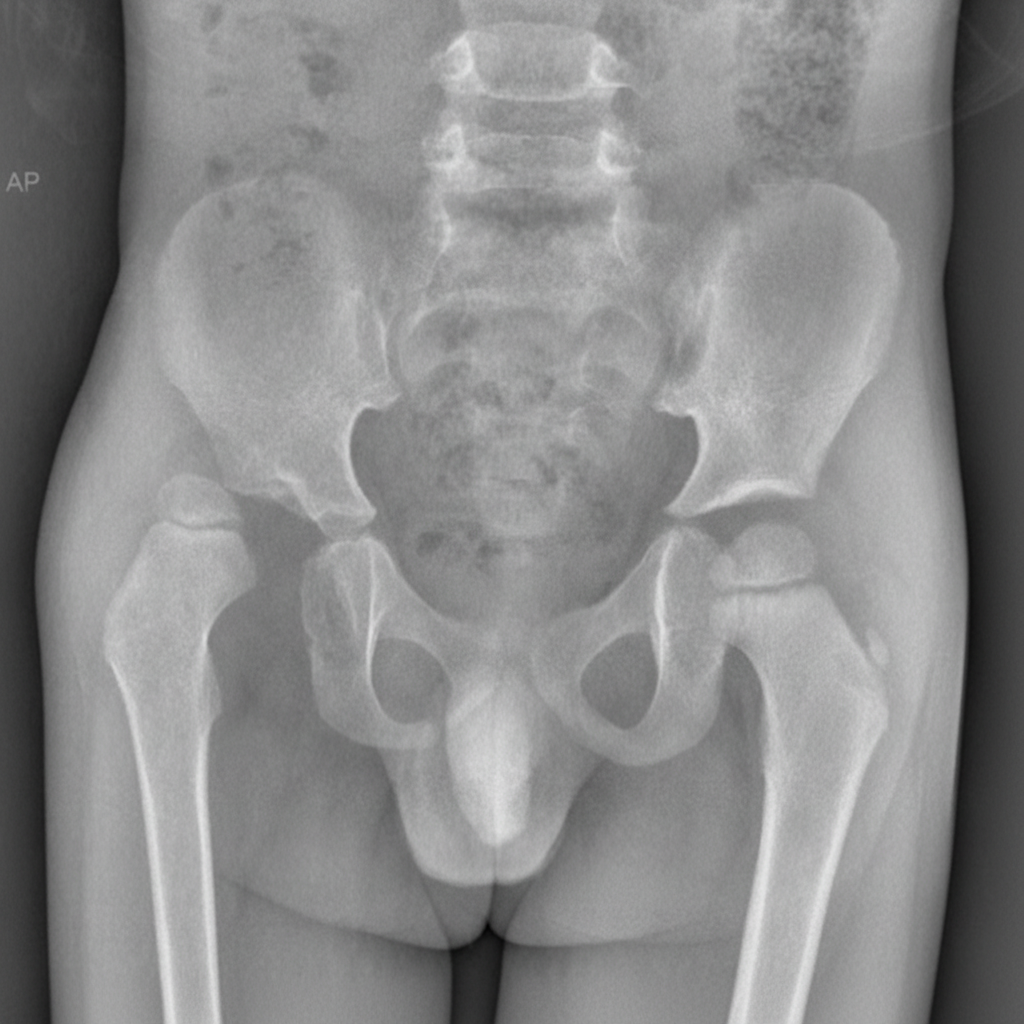
A previously healthy 13-year-old boy is brought to the physician because of a lump beneath his right nipple that he discovered 1 week ago while showering. He has allergic rhinitis treated with cetirizine. He is at the 65th percentile for height and 80th percentile for weight. Examination shows a mildly tender, firm, 2-cm subareolar mass in the right breast; there are no nipple or skin changes. The left breast shows no abnormalities. Sexual development is Tanner stage 3. Which of the following is the most likely explanation for this patient's breast lump?
A 7-week-old male presents to the pediatrician for vomiting. His parents report that three weeks ago the patient began vomiting after meals. They say that the vomitus appears to be normal stomach contents without streaks of red or green. His parents have already tried repositioning him during mealtimes and switching his formula to eliminate cow’s milk and soy. Despite these adjustments, the vomiting has become more frequent and forceful. The patient’s mother reports that he is voiding about four times per day and that his urine looks dark yellow. The patient has fallen one standard deviation off his growth curve. The patient's mother reports that the pregnancy was uncomplicated other than an episode of sinusitis in the third trimester, for which she was treated with azithromycin. In the office, the patient's temperature is 98.7°F (37.1°C), blood pressure is 58/41 mmHg, pulse is 166/min, and respirations are 16/min. On physical exam, the patient looks small for his age. His abdomen is soft, non-tender, and non-distended. Which of the following is the best next step in management?
An 8-month-old girl is brought to her pediatrician because her mom is concerned that she may have a "lazy eye". She was born prematurely at 33 weeks and was 3 pounds at birth. Her mother also says that there is a history of visual problems that run in the family, which is why she wanted to make sure that her daughter was evaluated early. On presentation, she is found to have eyes that are misaligned both horizontally and vertically. Physical examination and labs reveal no underlying disorders, and the patient is discharged with occlusion therapy to help correct the misalignment. Which of the following would most likely have also been seen on physical exam?
A 12-month-old boy is brought to the pediatrician for a routine examination. Past medical history is significant for a pyloric myomectomy at 2 months of age after a few episodes of projectile vomiting. He has reached all appropriate developmental milestones. He currently lives with his parents and pet cat in a house built in the 1990s. He was weaned off of breast milk at 6 months of age. He is a very picky eater, but drinks 5–6 glasses of whole milk a day. The patient's height and weight are in the 50th percentile for his age and sex. The vital signs are within normal limits except for the presence of slight tachycardia. Physical examination reveals an alert infant with a slight pallor. Abdomen is soft and nondistended. A grade 2/6 systolic ejection murmur is noted in the left upper sternal border. Which of the following will most likely be expected in this patient's laboratory results?
A 15-year-old girl comes to the physician with her father for evaluation of short stature. She feels well overall but is concerned because all of her friends are taller than her. Her birth weight was normal. Menarche has not yet occurred. Her father says he also had short stature and late puberty. The girl is at the 5th percentile for height and 35th percentile for weight. Breast development is Tanner stage 2. Pubic and axillary hair is absent. An x-ray of the left hand and wrist shows a bone age of 12 years. Further evaluation of this patient is most likely to show which of the following sets of laboratory findings?
A 1-year-old boy is brought to the emergency department after his mother witnessed him swallow a nickel-sized battery a few hours ago. She denies any episodes of vomiting or hematemesis. The vital signs include: temperature 37.0°C (98.6°F), blood pressure 95/45 mm Hg, pulse 140/min, respiratory rate 15/min, and oxygen saturation 99% on room air. On physical examination, the patient is alert and responsive. The oropharynx is clear. The cardiac exam is significant for a grade 2/6 holosystolic murmur loudest at the left lower sternal border. The lungs are clear to auscultation. The abdomen is soft and nontender with no hepatosplenomegaly. Bowel sounds are present. What is the most appropriate next step in the management of this patient?
An 8-year-old boy is brought to the emergency department with severe dyspnea, fatigue, and vomiting. His mother reports that he has been lethargic for the last several days with an increase in urine output. She thinks he may even be losing weight, despite eating and drinking more than normal for the last couple weeks. Laboratory results are notable for glucose of 440, potassium of 5.8, pH of 7.14 and HCO3 of 17. After administrating IV fluids and insulin, which of the following would you expect?
An 18-month-old boy presents to the clinic with his mother for evaluation of a rash around the eyes and mouth. His mother states that the rash appeared 2 weeks ago and seems to be very itchy because the boy scratches his eyes often. The patient is up to date on all of his vaccinations and is meeting all developmental milestones. He has a history of asthma that was recently diagnosed. On examination, the patient is playful and alert. He has scaly, erythematous skin surrounding both eyes and his mouth. Bilateral pupils are equal and reactive to light and accommodation, and conjunctiva is clear, with no evidence of jaundice or exudates. The pharynx and oral mucosa are within normal limits, and no lesions are present. Expiratory wheezes can be heard in the lower lung fields bilaterally. What is the most likely diagnosis in this patient?
A 12-month-old boy presents with pallor, fatigue, and conjunctival pallor. Examination reveals a grade II systolic ejection murmur. Labs show: Leukocytes 6,500/mm^3, Hemoglobin 6.4 g/dL, Platelets 300,000/mm^3, MCV 71 µm^3, Reticulocytes 2.0%, Serum iron 34 mcg/dL, Ferritin 6 ng/mL (normal 7-140 ng/mL), TIBC 565 mcg/dL (normal 240-450 mcg/dL). Peripheral smear shows microcytosis and hypochromia. In addition to starting iron supplementation, what dietary modification is most important to address the underlying cause?
Practice by Chapter
Normal growth patterns
Practice Questions
Growth charts and interpretation
Practice Questions
Failure to thrive evaluation
Practice Questions
Short stature workup
Practice Questions
Tall stature evaluation
Practice Questions
Obesity in children
Practice Questions
Nutritional assessment tools
Practice Questions
Puberty stages (Tanner stages)
Practice Questions
Precocious puberty
Practice Questions
Delayed puberty
Practice Questions
Growth hormone disorders
Practice Questions
Impact of chronic disease on growth
Practice Questions
Catch-up growth
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
