Growth/Development — MCQs

On this page
A 6-year-old boy presents to the pediatrician with his parents. He is fully vaccinated and met most developmental milestones. His fine motor milestones are delayed; at present, he cannot eat by himself and has difficulty in self-dressing. His intelligence quotient (IQ) is 65. He listens quietly while spoken to and engages in play with his classmates. He neither talks excessively nor remains mute, but engages in normal social conversation. There is no history of seizures and he is not on any long-term medical treatment. On his physical examination, his vital signs are stable. His height and weight are normal for his age and sex, but his occipitofrontal circumference is less than the 3rd percentile for his age and sex. His neurologic examination is also normal. Which of the following is the most likely diagnosis?
A 4-year-old boy presents with a recent history of frequent falls. The images below depict his movements when he tries to get up from the floor. Which of the following is the most likely diagnosis in this patient?

A 3-year-old boy is brought to the physician because of a 5-day history of yellowing of his eyes and skin. He has had generalized fatigue and mild shortness of breath over the past 2 months. Examination shows pale conjunctivae and scleral jaundice. The spleen is palpated 4 cm below the left costal margin. Laboratory studies show a hemoglobin concentration of 8.5 g/dL and a mean corpuscular volume of 76 μm3. A peripheral blood smear shows round erythrocytes that lack central pallor. Which of the following is the most likely cause of the splenomegaly seen in this child?
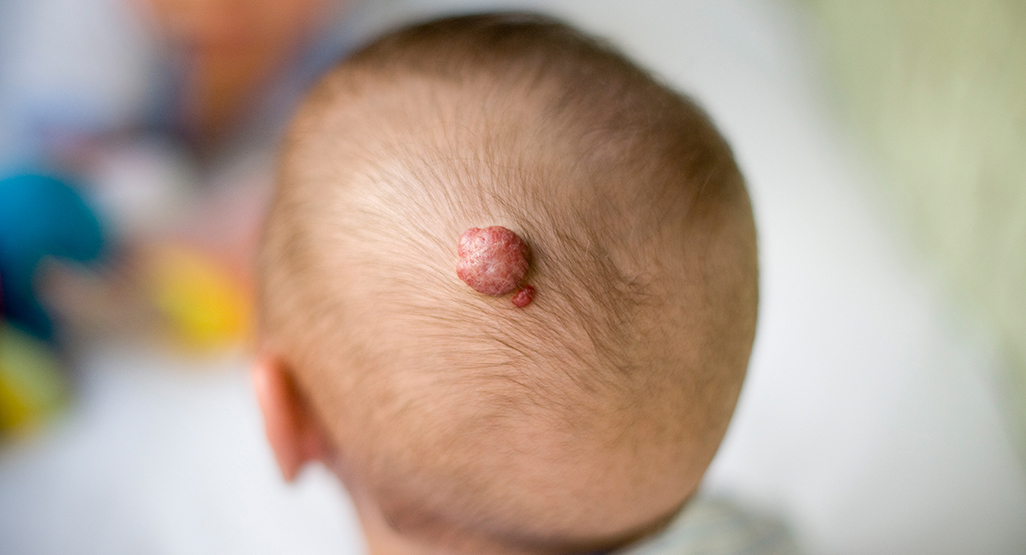
A 5-month-old girl is brought to the physician because of a red lesion on her scalp that was first noticed 2 months ago. The lesion has been slowly increasing in size. It is not associated with pain or pruritus. She was born at 37 weeks' gestation after an uncomplicated pregnancy and delivery. Her older sister is currently undergoing treatment for a fungal infection of her feet. Examination shows a solitary, soft lesion on the vertex of the scalp that blanches with pressure. A photograph of the lesion is shown. Which of the following is the most appropriate next step in management?
A 7-year-old girl is brought to the physician by her parents for the evaluation of pubic hair development. She has a history of a fracture in each leg and one fracture in her right arm. Her performance at school is good. There is no family history of serious illness. She takes no medications. Vital signs are within normal limits. Genital examination shows coarse, dark hair along the labia. The breast glands are enlarged and the breast bud extends beyond the areolar diameter. There are several hyperpigmented macules with rough, serpiginous borders of different sizes on the lower and upper extremities. The remainder of the examination shows no abnormalities. Which of the following is the most likely diagnosis?
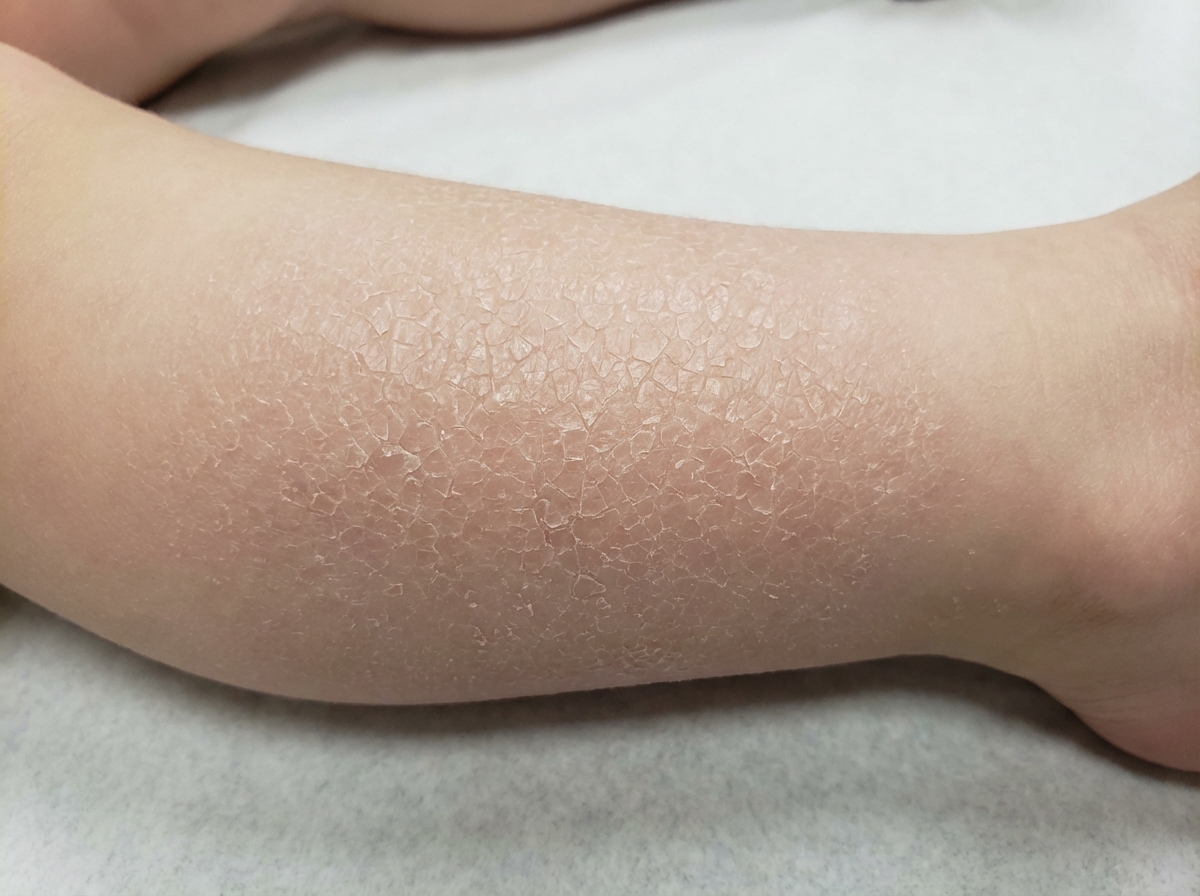
A 13-year-old female comes to your office complaining of dry, scaling skin (Figure A). She is particularly concerned about the appearance of her skin around her peers. She indicates that she did not start having problems until she was 5 years of age, after which her skin has progressively become drier and scalier. She has tried all types of over-the-counter moisturizers with no resolution. What is the most likely diagnosis?
A 2-year-old girl is brought to the physician by her mother for a well-child examination. She is at the 55th percentile for height and the 40th percentile for weight. Vital signs are within normal limits. Physical examination shows no abnormalities. She is able to follow simple commands, such as “close your eyes, then stick out your tongue,” but she is unable to follow 3-step commands. She knows approximately 75 words, and half of her speech is understandable. She can say 2-word phrases, and she is able to name many parts of the body. Assuming normal development, which of the following milestones would be expected in a patient this age?
A 3-year-old girl is brought to the physician by her parents for complaints of breast development and pubic hair growth for the past 6 months. She has no significant birth or medical history. The temperature is 37.0°C (98.6°F), the pulse is 88/min, and the respirations are 20/min. Physical examination shows enlarged breasts at Tanner stage 3 and pubic hair at stage 2. Height and weight are in the normal range. On GnRH stimulation testing, a luteinizing hormone (LH) response of < 5 IU/L is detected. What is the most appropriate next step in diagnosis?
A 3-year-old boy is brought to the physician because he is easily fatigued and has not gained weight. He eats 3 meals and has 3 to 4 bowel movements daily with bulky stools that float. He had recurrent episodes of sinusitis in infancy. He is at the 15th percentile for height and 5th percentile for weight. Examination shows pale conjunctivae. A few scattered expiratory crackles are heard in the thorax. There is abdominal distention. Which of the following is the most likely underlying cause of this patient's failure to thrive?
A 6-month-old girl is brought to the physician because of drooling and excessive crying for 3 days. She calms down when cuddled or with a pacifier in her mouth. She feeds well and has no vomiting or diarrhea. She was breastfed exclusively for 5 months. She is given no medications and was born at 39 weeks gestation via spontaneous vaginal delivery. She is up to date on all vaccines and is meeting all developmental milestones. At the clinic, her weight is 7.3 kg (16 lb 1 oz) and her height is 65.8 cm (25.9 in) in length. She appears irritable. Her pulse is 124/min, the respirations are 32/min, the blood pressure is 92/63 mm Hg, and the temperature is 36.8°C (98.2°F). On physical examination, she has no conjunctivitis, cervical lymphadenopathy, or pharyngeal erythema. Which element of the physical examination is most likely to be present in this patient?
Practice by Chapter
Normal growth patterns
Practice Questions
Growth charts and interpretation
Practice Questions
Failure to thrive evaluation
Practice Questions
Short stature workup
Practice Questions
Tall stature evaluation
Practice Questions
Obesity in children
Practice Questions
Nutritional assessment tools
Practice Questions
Puberty stages (Tanner stages)
Practice Questions
Precocious puberty
Practice Questions
Delayed puberty
Practice Questions
Growth hormone disorders
Practice Questions
Impact of chronic disease on growth
Practice Questions
Catch-up growth
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
