Systemic Pathology — MCQs

On this page
A 55-year-old female presents with pain in both hands and wrists for the past several years. It is associated with morning stiffness that lasts for almost an hour. Physical examination reveals tenderness and swelling in both hands and wrists, most severe over the proximal interphalangeal joints. Laboratory investigation reveals the presence of anti-cyclic citrullinated peptide (anti-CCP). Which of the following immune-mediated injuries is responsible for this patient’s condition?
A 7-year-old boy is brought to the emergency department by his parents with a 2-day history of severe fatigue. His parents say that he has no past medical history, but caught an illness that was going around his school 1 week ago. While ill, he had several days of abdominal pain and bloody diarrhea. His family history is significant for several family members who required blood transfusions, and he lives in an old house. Physical exam reveals conjunctival pallor and mild jaundice. Which of the following would most likely be seen on peripheral blood smear in this patient?
A healthy 29-year-old woman comes to the doctor because of recurrent episodes of bleeding from the nose and gums during the past week. These episodes occur spontaneously and resolve with compression. She also had 1 episode of blood in the urine 2 days ago. Examination shows punctate, nonblanching, reddish macules over the neck, chest, and lower extremities. Her leukocyte count is 8,600/mm3, hemoglobin concentration is 12.9 g/dL, and platelet count is 26,500/mm3. A peripheral blood smear shows a reduced number of platelets with normal morphology. Evaluation of a bone marrow biopsy in this patient is most likely to show which of the following findings?
A 12-year-old boy, otherwise healthy, presents with frequent nosebleeds and lower extremity bruising. His mother reports that his symptoms started about 2 weeks ago and have not improved. The patient received the Tdap vaccine 2 weeks ago. He has no current medications. The review of systems is significant for the patient having a stomach ache after winning a hamburger eating competition 2 weeks ago. The vital signs include: temperature 37.0°C (98.6°F), blood pressure 110/75 mm Hg, pulse 95/min, respirations 15/min, and oxygen saturation 99% on room air. On physical exam, the patient is alert and cooperative. The cardiac exam is normal. The lungs are clear to auscultation bilaterally. The lower extremities findings are shown in the image. Laboratory results are pending. Which of the following best describes the pathogenesis of this patient’s condition?
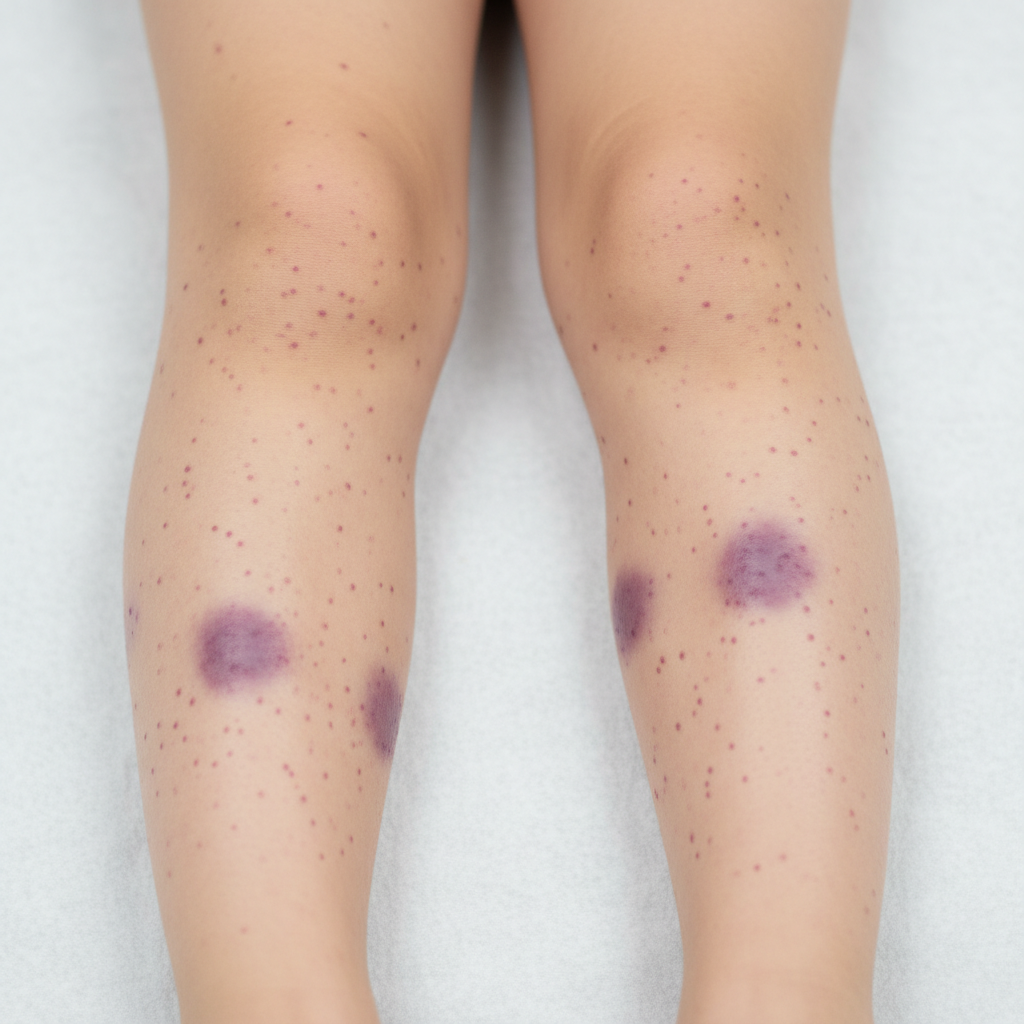
A 68-year-old woman is being evaluated for fatigue during a follow-up visit after implantation of a prosthetic aortic valve a month ago. She reports she has been feeling more tired than usual but associates it with her recent surgery. A complete blood count (CBC) reveals a hemoglobin of 9.5 g/dL and a reticulocyte percentage of 2.8%. Additionally, the serum haptoglobin is decreased while the platelet count is within the normal range. The patient is suspected to have a type of hemolytic anemia secondary to her prosthetic heart valve. Which of the following will most likely be seen in this patient's blood smear?
A 4-year-old boy is brought to the emergency department with 2 days of fever and painful lumps in his legs bilaterally. In addition, he says that his arms and legs are extremely itchy. Since birth he has had recurrent skin and soft tissue infections. Physical exam reveals a pruritic erythematous scaling rash along both upper and lower extremities bilaterally. Palpation of the painful lesions reveal indurated tissue without any production of pus. Which of the following protein functions is most likely disrupted in this patient?
A previously healthy 59-year-old man comes to the physician with a 6-month history of worsening headaches, difficulty chewing, and progressive hearing loss. Examination shows a mildly tender, 1-cm, hard swelling over the left maxilla. The remainder of the examination shows no abnormalities. Serum studies show a calcium concentration of 8.5 mg/dL, alkaline phosphatase activity of 112 U/L, and parathyroid hormone concentration of 310 pg/mL. Audiometry shows bilateral mixed conductive and sensorineural hearing loss. Which of the following processes is the most likely cause of this patient's condition?
An 11-month-old male is brought to the emergency room by his mother. The mother reports that the child is in severe pain and has not moved his right leg since earlier this morning when he was crawling on the floor. The child did not fall or sustain any obvious injury. The child’s past medical history is notable for anemia and recurrent infections since birth. His temperature is 99.1°F (37.3°C), blood pressure is 100/65 mmHg, pulse is 120/min, and respirations are 22/min. Physical examination reveals mild macrocephaly and hepatosplenomegaly. Palpation of the right femur seems to exacerbate the child’s pain. A radiograph demonstrates a transverse mid-shaft femur fracture. Which of the following is the most likely cause of this patient’s condition?
A 20-year-old man comes to the clinic complaining of fever and a sore throat for 5 days. He receives oral penicillin from his primary doctor. After a day of antibiotic treatment, he developed gross hematuria. As a child, he recalls having multiple episodes of hematuria. The vital signs are within normal limits. On physical examination, pharyngeal edema and cervical lymphadenopathy are present. His laboratory examination reveals the following: WBC 11,000/mm3 Neutrophils 76% Lymphocytes 23% Eosinophils 1% Platelets 150,000/mm3 Hemoglobin 14 g/dL Hct 41.2% BUN 16 mg/dL Creatinine 0.9 mg/dL ASO titer 100 Urinalysis shows hematuria but no proteinuria. Immunofluorescence shows granular IgA immune complex deposits in the mesangium. Hepatitis B, hepatitis C, and HIV serology are negative. ASO titers and C3 levels are within normal limits. What is the most likely diagnosis?
A 31-year-old man presents to his primary care physician with shortness of breath. He states that he had a “cold” 2 weeks ago and since then has had a persistent cough and worsening shortness of breath. He denies fever, chills, chest pain, sore throat, or rhinorrhea. His medical history is significant for seasonal allergies. He uses fluticasone nasal spray. He had his tonsils removed when he was 8 years of age. His mother and maternal grandfather have cirrhosis, and his father has depression and hypertension. The patient endorses that he smokes tobacco socially on the weekends and uses marijuana daily. He drinks 1-2 beers after work with his co-workers most evenings. A chest radiograph shows hyperinflation of the lungs and hyperlucency. Routine labs are drawn, as shown below. Serum: Na+: 139 mEq/L Cl-: 105 mEq/L K+: 4.0 mEq/L HCO3-: 26 mEq/L Urea nitrogen: 15 mg/dL Glucose: 100 mg/dL Creatinine: 0.8 mg/dL Alkaline phosphatase: 98 U/L Aspartate aminotransferase (AST, GOT): 46 U/L Alanine aminotransferase (ALT, GPT): 49 U/L Pulmonary function tests are pending. Which of the following is most likely to confirm the patient’s diagnosis?
Practice by Chapter
Liver pathology (hepatitis, cirrhosis)
Practice Questions
Gallbladder and biliary tract disorders
Practice Questions
Pancreatic diseases
Practice Questions
Kidney diseases
Practice Questions
Male reproductive pathology
Practice Questions
Female reproductive pathology
Practice Questions
Breast pathology
Practice Questions
Endocrine pathology
Practice Questions
Bone and joint pathology
Practice Questions
Skeletal muscle diseases
Practice Questions
Peripheral nerve disorders
Practice Questions
Soft tissue tumors
Practice Questions
Head and neck pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
