Systemic Pathology — MCQs

On this page
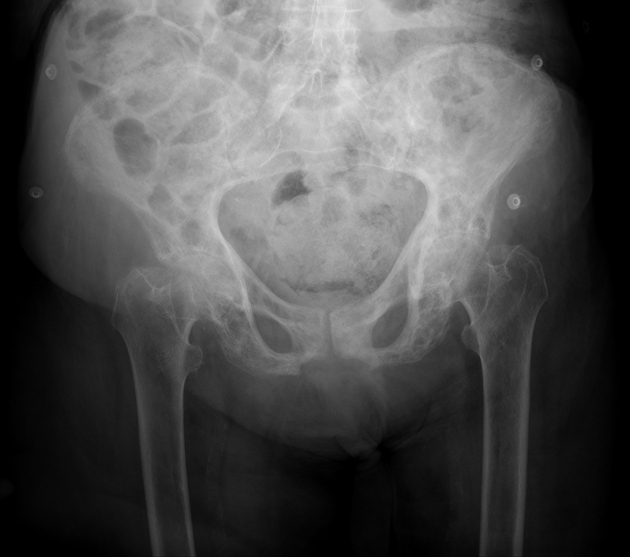
A 67-year-old man presents to the physician because of low-back pain for 6 months. The pain is more localized to the left lower back and sacral area. It is constant without any radiation to the leg. He has no significant past medical history. He takes ibuprofen for pain control. His father developed a bone disease at 60 years of age and subsequently had a fracture in the spine and another in the lower leg. The patient’s vital signs are within normal limits. The neurologic examination shows no focal findings. He has mild tenderness on deep palpation of the left pelvis. The physical examination of the lower extremities shows no abnormalities other than bowed legs. A radiograph of the pelvis is shown in the image. Which of the following serum tests is the most important initial diagnostic study?
A 68-year-old man presents with blisters on the flexor surfaces of his arms and legs. He notes that the lesions appeared 2 days ago and have not improved. He says that he has had similar blisters in the past but has not sought medical attention until now. The man has no significant past medical history. He is afebrile and his vital signs are within normal limits. On physical examination, there are tense bullae present on the flexor surfaces of his arms and legs. Biopsy of a lesion and histopathologic examination reveal a subepidermal blister with a polymorphous but predominantly eosinophilic infiltrate. Which of the following is the best next diagnostic step in this patient?
A 67-year-old man presents to his physician for a follow-up examination. During his last visit 1 month ago, splenomegaly was detected. He has had night sweats for the past several months and has lost 5 kg (11 lb) unintentionally during this period. He has no history of severe illness and takes no medications. The vital signs are within normal limits. The examination shows no abnormalities other than splenomegaly. The laboratory studies show the following: Hemoglobin 9 g/dL Mean corpuscular volume 95 μm3 Leukocyte count 12,000/mm3 Platelet count 260,000/mm3 Ultrasound shows a spleen size of 15 cm and mild hepatomegaly. A peripheral blood smear shows teardrop-shaped and nucleated red blood cells (RBCs) and immature myeloid cells. The marrow is very difficult to aspirate but reveals hyperplasia of all 3 lineages. The tartrate-resistant acid phosphatase (TRAP) test is negative. Clonal marrow plasma cells are not seen. JAK-2 is positive. The cytogenetic analysis is negative for translocation between chromosomes 9 and 22. Which of the following is the most likely diagnosis?
A 45-year-old African American man presents with nausea and severe abdominal pain. He denies vomiting. He says that, 2 days ago, his divorce was finalized, so he went to a bar and had multiple shots of tequila and vodka. This morning, upon waking, he noticed his urine was red, which lasted throughout the day. The patient denies any history of similar symptoms. Past medical history is significant for low blood counts diagnosed on routine laboratory work 6 months ago, which was not followed up due to the stress of the divorce. A review of systems is significant for erectile dysfunction and chronic fatigue. His temperature is 37.2°C (99.0°F), the heart rate is 90/min, the blood pressure is 136/88 mm Hg, and the respiratory rate is 20/min. Physical examination shows scleral icterus. Mucous membranes are pale. Cardiac auscultation reveals a systolic flow murmur loudest along the left sternal border. There is moderate right upper quadrant abdominal tenderness with no rebound or guarding. The remainder of the exam is unremarkable. Laboratory findings are significant for the following: Hematocrit 27% Mean corpuscular volume 81 µm3 Leukocytes 6,000/mm3 Platelets 130,000/µL Haptoglobin 30 mg/dL (50–150 mg/dL) Reticulocyte count 3% Total bilirubin 7.1 mg/dL LDH 766 U/L AST 150 U/L ALT 195 U/L HbA1 96% HbA2 2% HbF 2% CD55 50% of expected The peripheral smear is unremarkable. Which of the following would be the most likely cause of mortality given this patient’s likely diagnosis?
A 55-year-old African American male presents to his primary care physician with complaints of persistent back pain and fatigue over 12 months. Physical examination reveals a blood pressure of 190/150 mm Hg, and laboratory tests reveal hyperlipidemia and a serum creatinine level of 3.0 mg/dL. 4.5 g of protein are excreted in the urine over 24 hours. Renal biopsy shows eosinophilic, acellular material in the glomerular tuft and capillary walls that display apple green-colored birefringence in polarized light upon Congo red tissue staining. The patient most likely suffers from which of the following:
A 30-year-old woman was brought in by ambulance after being struck by a truck while crossing the street. She has lost a large volume of blood, and a transfusion of packed RBCs is indicated. The patient’s blood type is confirmed to be AB+. She is to be given two units of packed red blood cells (RBCs). Which of the following type(s) of packed RBCs would be safe to transfuse into this patient?
A 35-year-old man comes to the physician because of progressive swelling of his legs over the past 2 months. During this period, the patient has had an unintentional 5-kg (11-lb) weight gain. He also reports frequent numbness of the tips of his fingers and cramping in his back and leg muscles. He has a history of HIV infection treated with combined antiretroviral therapy. The patient immigrated to the US from Nigeria 3 years ago. His temperature is 37°C (98.6°F), pulse is 80/min, and blood pressure 150/90 mm Hg. Physical examination shows 3+ periorbital and lower extremity edema bilaterally. Sensation to pinprick and light touch is decreased around the mouth and along the fingers. Laboratory studies show: Serum Albumin 2.5 g/dL Total cholesterol 270 mg/dL HIV antibody positive Urine Blood negative Protein +4 RBC 1-2/hpf RBC casts negative A kidney biopsy is most likely to show which of the following findings under light microscopy?
A 71-year-old male with worsening memory, behavior changes, and disorientation over the span of several years was admitted to the hospital for signs of severe pneumonia. He passes away after failed antibiotic therapy. Which of the following findings would most likely be identified on autopsy?
A 46-year-old man is admitted to the hospital with a 3-day history of productive cough with purulent sputum and fever with chills. On the second day of admission, he develops bloody vomiting, altered mental status, and multiple red spots all over the body. He is oriented only to self. His temperature is 39.3°C (102.7°F), pulse is 110/min, respirations are 26/min, and blood pressure is 86/50 mm Hg. Physical examination shows ecchymoses on both lower extremities. Crackles are heard at the right lung base. Laboratory studies show a platelet count of 45,000/mm3, with a prothrombin time of 44 sec and partial thromboplastin time of 62 sec. D-dimer concentrations are elevated. Which of the following is the most likely cause of this patient's ecchymoses?
A 66-year-old man is brought to the clinic with a history of recurrent falls. He has been slow in his movements and walks clumsily. He denies fever, vision problems, limb weakness, numbness, abnormal sensation in his limbs, trauma, or inability to pass urine. The past medical history is unremarkable, and he only takes calcium and vitamin D supplements. The vital signs include: blood pressure 128/72 mm Hg, heart rate 85/min, respiratory rate 16/min, and temperature 36.9°C (98.4°F). He is awake, alert, and oriented to time, place, and person. His eye movements are normal. There is a tremor in his hands bilaterally, more in the left-hand which decreases with voluntary movements. The muscle tone in all 4 limbs is increased with normal deep tendon reflexes. He walks with a stooped posture and takes small steps with decreased arm swinging movements. During walking, he has difficulty in taking the first few steps and also in changing directions. The speech is slow and monotonous. His mini-mental state examination (MMSE) score is 26/30. What is the most likely pathophysiology of the patient’s condition?
Practice by Chapter
Liver pathology (hepatitis, cirrhosis)
Practice Questions
Gallbladder and biliary tract disorders
Practice Questions
Pancreatic diseases
Practice Questions
Kidney diseases
Practice Questions
Male reproductive pathology
Practice Questions
Female reproductive pathology
Practice Questions
Breast pathology
Practice Questions
Endocrine pathology
Practice Questions
Bone and joint pathology
Practice Questions
Skeletal muscle diseases
Practice Questions
Peripheral nerve disorders
Practice Questions
Soft tissue tumors
Practice Questions
Head and neck pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
