Systemic Pathology — MCQs

On this page
A 49-year-old obese woman presents with a chronic non-healing ulcer on the right medial malleolus. Past medical history is significant for type 2 diabetes mellitus, diagnosed 10 years ago, poorly managed with metformin. Review of systems is significant for a recurrent white vaginal discharge. The patient is afebrile, and her vital signs are within normal limits. Her BMI is 31 kg/m2. On physical examination, there is a 2 cm by 2 cm nontender, erythematous shallow ulcer present over the right medial malleolus. Sensation is decreased symmetrically in the lower extremities below the level of the midcalf. Which of the following histopathological findings would most likely be seen in the peripheral nerves in this patient?
A 2-year-old boy is brought to the pediatrician for recurrent nosebleeds. The boy was adopted two months ago and the parents have no record of his medical or family history. They report that the child has had frequent prolonged nosebleeds several times per week. Despite them applying pressure on the distal aspect of the nares and keeping his head elevated, the bleeding generally continues for hours. On exam, the boy appears pale and lethargic. A blood sample is obtained but the child bleeds through multiple pieces of gauze. No agglutination is observed when ristocetin is added to the patient’s blood. The addition of normal plasma to the sample still does not lead to agglutination. This patient has a condition that is most consistent with which of the following modes of transmission?
A 25-year-old man is brought to the emergency department by ambulance after a motor vehicle accident. His car was rear-ended by a drunk driver while he was stopped at a traffic light. At the scene, he was noted to have multiple small lacerations over his upper extremities from broken glass. He has otherwise been healthy, does not smoke, and drinks 5 beers per night. He notes that he recently started trying out a vegan diet and moved to an apartment located in a historic neighborhood that was built in the 1870s. Physical exam reveals several small lacerations on his arms bilaterally but is otherwise unremarkable. A complete blood workup is sent and some of the notable findings are shown below: Hemoglobin: 12.1 g/dL (normal: 13.5-17.5 g/dL) Platelet count: 261,000/mm^3 (normal: 150,000-400,000/mm^3) Mean corpuscular volume: 74 µm^3 (normal: 80-100 µm^3) Further testing using serum hemoglobin electrophoresis reveals: Hemoglobin A1 92% (normal 95-98%) Hemoglobin A2: 6% (normal: 1.5-3.1%) Which of the following cell morphologies would most likely be seen on blood smear in this patient?
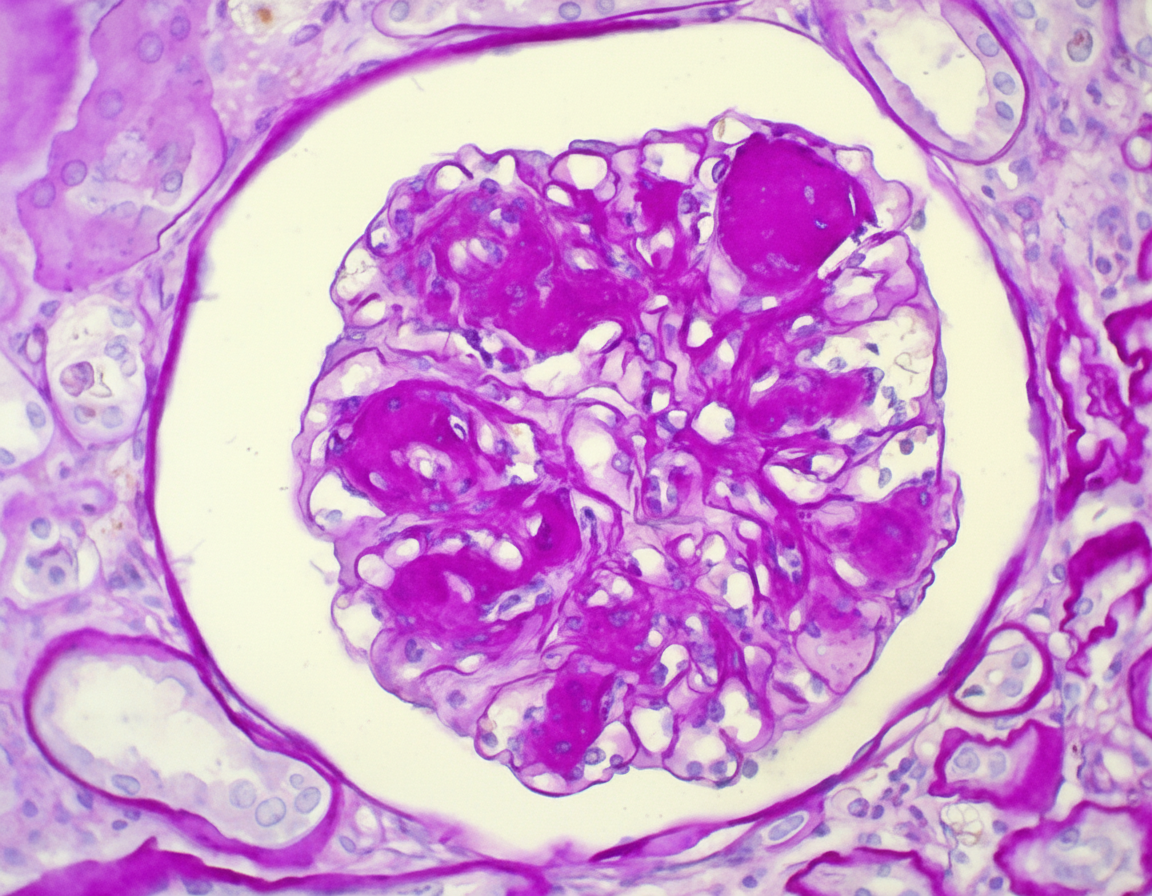
A 64-year-old man comes to the physician because of fatigue and decreased urinary frequency for 6 months. His pulse is 86/min and blood pressure is 150/90 mm Hg. Examination shows 1+ edema on bilateral ankles. His serum creatinine is 2 mg/dL and blood urea nitrogen is 28 mg/dL. Urinalysis shows proteinuria. A photomicrograph of a biopsy specimen from the patient's kidney is shown. Which of the following is the most likely explanation for the patient’s biopsy findings?
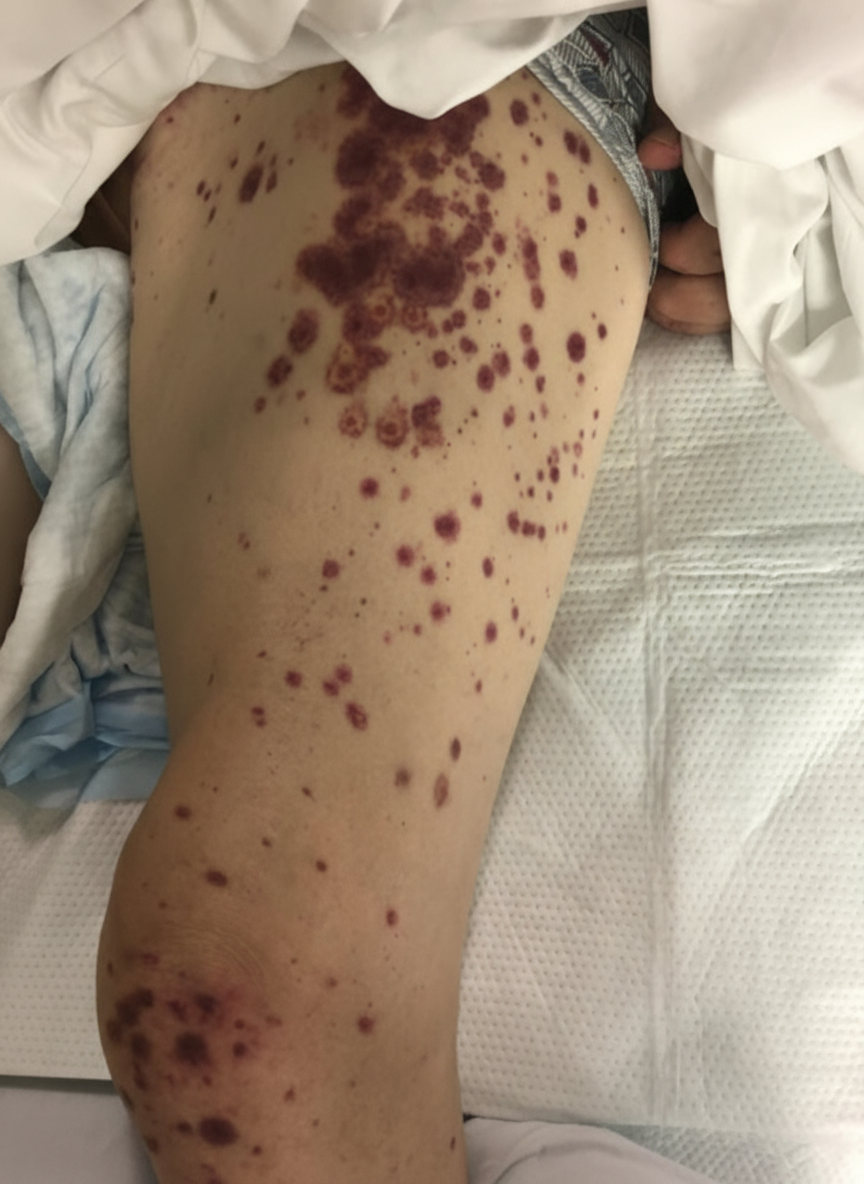
A 12-year-old boy is brought to an outpatient clinic by his mother, who noticed that her son’s urine has been dark for the past 4 days. She initially attributed this to inadequate hydration, so she monitored her son’s fluid intake and encouraged him to drink more water. However, she noticed that the color of the urine kept getting darker until it began to resemble cola. The boy’s medical history is significant for a sore throat approx. 2 weeks ago, which resolved without medication or treatment. The boy has also been complaining of pain in his ankles, which he first noticed shortly after soccer practice 1 week ago. He has had no pain during urination or urethral discharge, however, and does not have any history of previous episodes of cola-colored urine or passage of blood in the urine. However, the boy has been experiencing intermittent episodes of abdominal pain for the past 3 days. The boy also has wheals on his torso, legs, and buttocks, which his mother attributes to seasonal allergies. Physical examination reveals an alert child who is not in obvious distress but who has a mild conjunctival pallor. Vital signs include: respiratory rate is 22/min, temperature is 36.7°C (98.0°F), and blood pressure is 130/90 mm Hg. Examination of the musculoskeletal system reveals multiple skin lesions (see image). Which of the following laboratory findings is most likely associated with this patient’s clinical presentation?
A 55-year-old male presents to his primary care physician complaining of right hip pain for the past eight months. He also reports progressive loss of hearing over the same time period. Radiographic imaging reveals multiple areas of expanded bony cortices and coarsened trabeculae in his right hip and skull. Laboratory analysis reveals an isolated elevation in alkaline phosphatase with normal levels of serum calcium and phosphate. Which of the following histologic findings is most likely to be seen if one of the lesions were biopsied?
A 57-year-old man presents to his primary care physician with a 2-month history of right upper and lower extremity weakness. He noticed the weakness when he started falling far more frequently while running errands. Since then, he has had increasing difficulty with walking and lifting objects. His past medical history is significant only for well-controlled hypertension, but he says that some members of his family have had musculoskeletal problems. His right upper extremity shows forearm atrophy and depressed reflexes while his right lower extremity is hypertonic with a positive Babinski sign. Which of the following is most likely associated with the cause of this patient's symptoms?
A 3-year-old girl is brought to her pediatrician because of a nosebleed that will not stop. Her parents say that she started having a nosebleed about 1 hour prior to presentation. Since then they have not been able to stop the bleeding. Her past medical history is remarkable for asthma, and she has a cousin who has been diagnosed with hemophilia. Physical exam reveals diffuse petechiae and purpura. A panel of bleeding tests are obtained with the following results: Bleeding time: 11 minutes Prothrombin time: 14 seconds Partial thromboplastin time: 32 seconds Platelet count: 195,000/mm^3 Peripheral blood smear shows normal cell morphology. Which of the following characteristics is most likely true about this patient?
An 8-year-old boy is brought to the physician by his parents because of fever for 3 days. During the period, he has had fatigue, severe burning with urination, and increased urination. The mother reports that his urine has red streaks and a “strange” odor. He has taken acetaminophen twice a day for the past two days with no improvement in his symptoms. He has had multiple ear infections in the past but has been healthy in the past year. His immunizations are up-to-date. He appears uncomfortable. His temperature is 39°C (102.2°F). Examination shows right-sided costovertebral angle tenderness. Laboratory studies show a leukocyte count of 16,000/cm3 and an erythrocyte sedimentation rate of 40 mm/hr. Urine dipstick shows leukocyte esterase and nitrites. Urinalysis shows: Blood 2+ Protein 2+ WBC 24/hpf RBC 50/hpf RBC casts none WBC casts numerous Granular casts none Urine cultures are sent to the laboratory. Damage to which of the following structures is the most likely cause of this patient's hematuria?
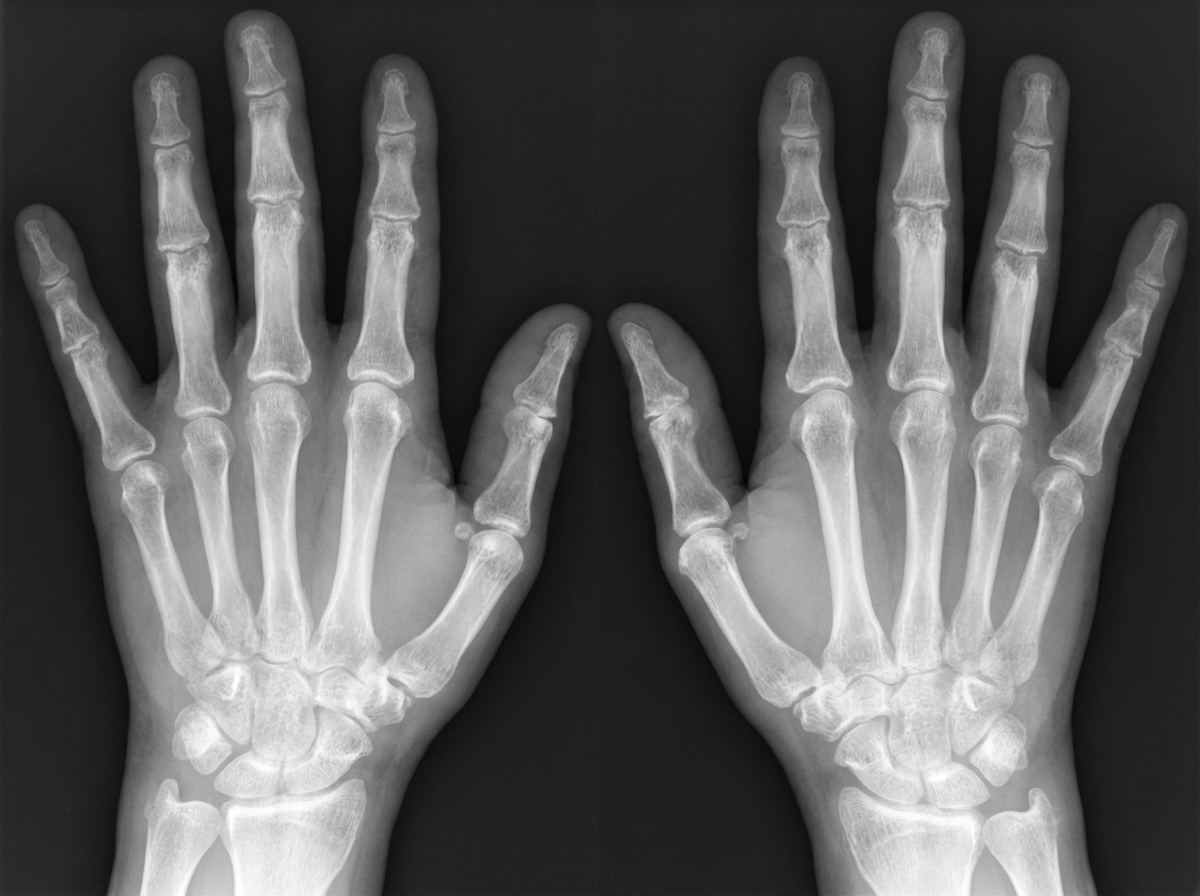
A 42-year-old woman comes to the physician because of a 10-month history of joint pain and stiffness in her wrists and fingers. The symptoms are worse in the morning and improve with activity. Physical examination shows swelling and warmth over the MCP and wrist joints in both hands. An x-ray of the hands is shown. Synovial biopsy from an affected joint would most likely show which of the following?
Practice by Chapter
Liver pathology (hepatitis, cirrhosis)
Practice Questions
Gallbladder and biliary tract disorders
Practice Questions
Pancreatic diseases
Practice Questions
Kidney diseases
Practice Questions
Male reproductive pathology
Practice Questions
Female reproductive pathology
Practice Questions
Breast pathology
Practice Questions
Endocrine pathology
Practice Questions
Bone and joint pathology
Practice Questions
Skeletal muscle diseases
Practice Questions
Peripheral nerve disorders
Practice Questions
Soft tissue tumors
Practice Questions
Head and neck pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
