Systemic Pathology — MCQs

On this page
A 9-year-old boy is brought to the emergency room by his mother. She is concerned because her son’s face has been swollen over the past 2 days. Upon further questioning, the boy reports having darker urine without dysuria. The boy was seen by his pediatrician 10 days prior to presentation with a crusty yellow sore on his right upper lip that has since resolved. His medical history is notable for juvenile idiopathic arthritis. His temperature is 99°F (37.2°C), blood pressure is 140/90 mmHg, pulse is 95/min, and respirations are 18/min. On exam, he has mild periorbital edema. Serological findings are shown below: C2: Normal C3: Decreased C4: Normal CH50: Decreased Additional workup is pending. This patient most likely has a condition caused by which of the following?
A 38-year-old man presents to the outpatient clinic for an annual employee health checkup. He does not have any complaints at the moment except for skin changes, as seen in the following image. He denies any history of trauma. His medical history is insignificant. His family history is negative for any skin disorders or autoimmune disease. He is a non-smoker and does not drink alcohol. Which of the following is the most likely mechanism for this presentation?

A young Caucasian couple in their late twenties present for an infertility evaluation after trying to conceive over 2 years. On physical exam, the female appears healthy and states that she has regular menstrual cycles. The male partner is noted to have long extremities with wide hips, low muscle mass, gynecomastia, sparse facial or chest hair, and small, firm testes. Laboratory tests of the male partner reveal elevated serum LH and FSH and low testosterone levels. If cytogenetic tests were performed, which of the following would be seen in this male?
A 10-year-old boy is presented to the hospital for a kidney transplant. In the operating room, the surgeon connects an allograft kidney renal artery to the aorta, and after a few moments, the kidney becomes cyanotic, edematous, and dusky with mottling. Which of the following in the recipient’s serum is responsible for this rejection?
A 21-year-old male presents to your office with hematuria 3 days after the onset of a productive cough and fever. Following renal biopsy, immunofluorescence shows granular IgA deposits in the glomerular mesangium. Which of the following do you suspect in this patient?
A 42-year-old woman is brought to the emergency department because of two episodes of hemoptysis over the past 24 hours. The patient has a 6-month history of severe sinusitis and bloody nasal discharge. Her vital parameters are as follows: blood pressure, 155/75 mm Hg; pulse, 75/min; respiratory rate, 14/min; and temperature, 37.9°C (100.2°F). Examination reveals red conjunctiva, and an ulcer on the nasal septum. Pulmonary auscultation indicates diffuse rhonchi. Cardiac and abdominal examinations reveal no abnormalities. Laboratory studies show: Urine Blood 3+ Protein 2+ RBC 10-15/hpf with dysmorphic features RBC cast numerous Based on these findings, this patient is most likely to carry which of the following antibodies?
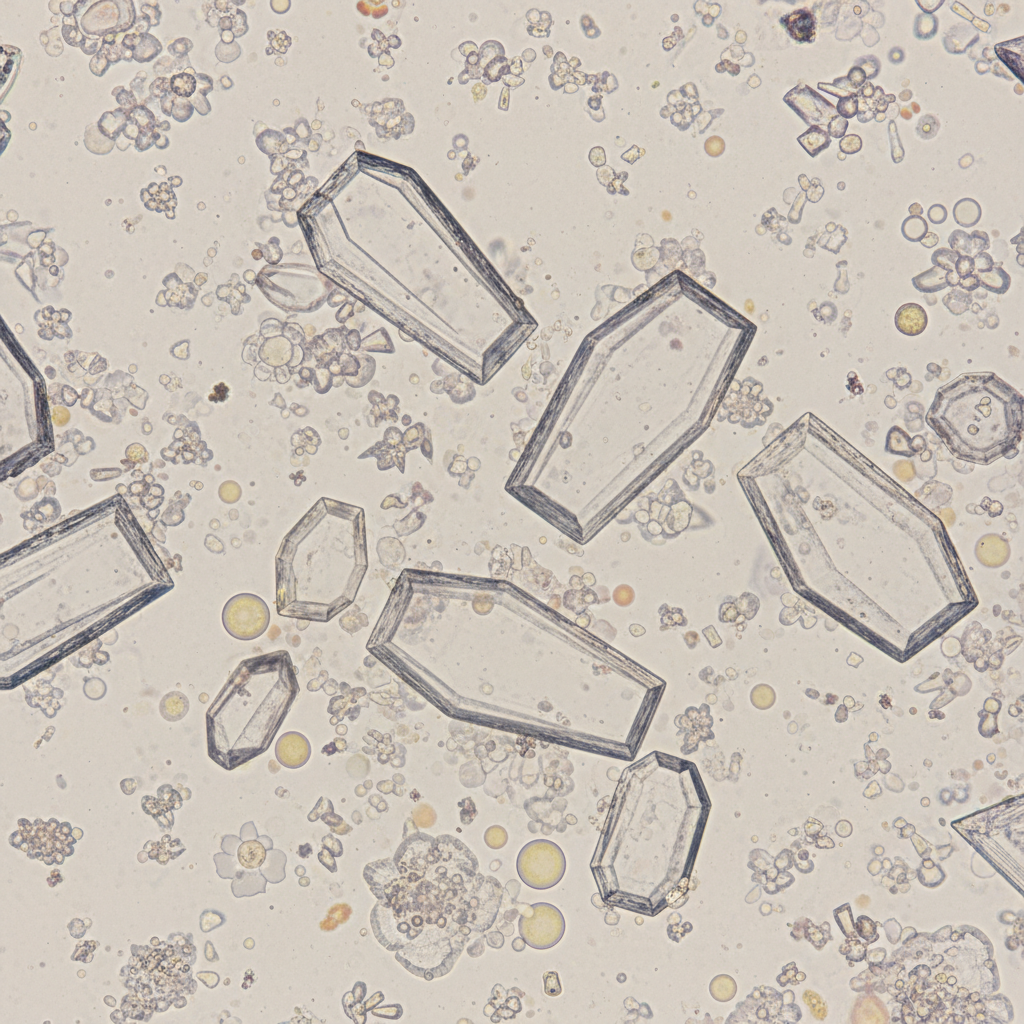
A 32-year-old woman comes to the physician because of a 1-week history of left flank pain and dysuria. She has had 2 episodes of urinary tract infection over the past 2 years. Her temperature is 37°C (98.6°F) and pulse is 82/min. An ultrasound of the kidneys shows left-sided hydronephrosis and echogenic foci with acoustic shadowing. A photomicrograph of the urine is shown. The crystals observed are most likely composed of which of the following?
A 10-year-old boy comes to the physician because of a 4-month history of intermittent red urine. During the past 2 years, he has had recurrent episodes of swelling of his face and feet. Five years ago, he was diagnosed with mild bilateral sensorineural hearing loss. His uncle died of kidney disease in his twenties. His blood pressure is 145/85 mm Hg. Laboratory studies show a hemoglobin concentration of 12.5 g/dL, urea nitrogen concentration of 40 mg/dL, and creatinine concentration of 2.4 mg/dL. Urinalysis shows 5–7 RBC/hpf. Which of the following is the most likely underlying cause of this patient's symptoms?
A 45-year-old male immigrant with rheumatoid arthritis comes to the physician because of severe pain and swelling in both his knees. He also reports an unintentional weight loss of around 10 kg over 3 months and episodic abdominal pain, varying in intensity and location. He has been having loose stools with no blood, 2–3 times a day for 1 month. He denies fever, night sweats, cough, or shortness of breath. Current medications include methotrexate, naproxen, and folic acid. His weight is 68 kg (150 lbs), temperature is 37.4°C (99.3°F), pulse is 90/min, and blood pressure is 130/80 mm Hg. Examination shows pale conjunctivae, cheilitis, and hyperpigmentation of the skin around his neck. Generalized lymphadenopathy is present. Examination of the knee joints shows bilateral warmth, erythema, swelling, tenderness, and limited range of motion. A grade 2/6 early diastolic murmur is heard over the right second intercostal space and an S3 is heard. Abdominal examination shows no abnormalities. Laboratory studies show: Hemoglobin 9.1 g/dL Leukocyte count 3800/mm3 Platelet count 140,000/mm3 Mean corpuscular volume 67 μm3 Erythrocyte sedimentation rate 62 mm/h Serum Glucose 100 mg/dL Creatinine 0.7 mg/dL TIBC 500 mcg/dL Ferritin 10 mcg/dL Rheumatoid factor negative Anti -CCP negative An esophagogastroduodenoscopy is ordered. A biopsy specimen of the duodenum is likely to show which of the following?
A 25-year-old man of Mediterranean descent makes an appointment with his physician because his skin and sclera have become yellow. He complains of fatigue and fever that started at the same time icterus appeared. On examination, he is tachycardic and tachypneic. The oxygen (O2) saturation is < 90%. He has increased unconjugated bilirubin, hemoglobinemia, and an increased number of reticulocytes in the peripheral blood. What is the most likely diagnosis?
Practice by Chapter
Liver pathology (hepatitis, cirrhosis)
Practice Questions
Gallbladder and biliary tract disorders
Practice Questions
Pancreatic diseases
Practice Questions
Kidney diseases
Practice Questions
Male reproductive pathology
Practice Questions
Female reproductive pathology
Practice Questions
Breast pathology
Practice Questions
Endocrine pathology
Practice Questions
Bone and joint pathology
Practice Questions
Skeletal muscle diseases
Practice Questions
Peripheral nerve disorders
Practice Questions
Soft tissue tumors
Practice Questions
Head and neck pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
