Systemic Pathology — MCQs

On this page
A previously healthy 6-year-old girl is brought to the physician by her parents because of slowed growth and fatigue. Over the past year, she went from average height for her age group to the shortest in her class. She has also been having more problems concentrating in class and is less interested in playing. She has not had any change in appetite or diet. She is at the 10th percentile for height and the 90th percentile for weight. Vital signs are within normal limits. There is a nontender mass palpated on the anterior cervical examination. Serum laboratory studies show thyroid-stimulating hormone level of 6.7 μU/mL. Further evaluation is most likely to show which of the following findings?
A 19-year-old woman presents to the primary care clinic to establish care. She has no acute complaints or concerns. Upon further questioning, she shares that she gets frequent nosebleeds and often bleeds from her gums a little after brushing her teeth. She also typically has relatively heavy menstrual periods, soaking eight tampons per day. She has not had any serious bleeding events, and she has never had a blood transfusion. Physical exam is unremarkable. A complete blood count shows mild anemia with a normal platelet count. Which of the following is the next best step in the management of this patient?
A 61-year-old construction worker comes to the physician because of a 3-month history of progressively worsening cough and shortness of breath. He has had a 7.5-kg (16.5-lb) weight loss during this period. He smokes occasionally and does not drink alcohol. Physical examination shows clubbing of the fingers. End-inspiratory crackles are heard in both lower lung fields. X-ray of the chest shows bilateral reticulonodular densities with interstitial fibrosis. Histologic examination of a lung biopsy specimen shows noncaseating granulomas in the interstitium. Which of the following is the most likely underlying mechanism of this patient's condition?
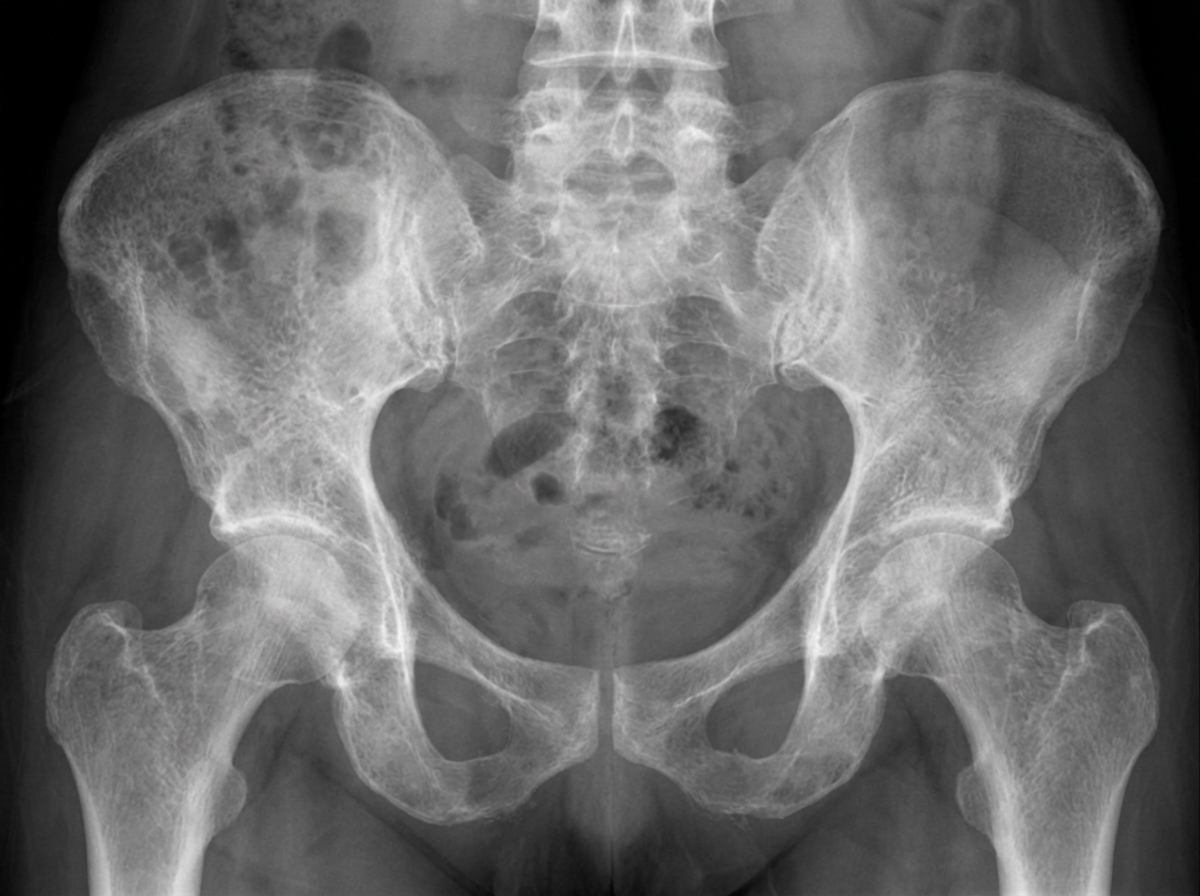
A 67-year-old male presents to his primary care physician complaining of left hip pain for the past six months. He denies any trauma or recent falls. He is accompanied by his wife who reports that he has experienced progressive hearing loss over the same time period. The patient has also noticed that he is no longer able to fit into his favorite hat even though it previously fit well. A radiograph of the patient’s pelvis is shown. Which of the following laboratory abnormalities is most likely to be found in this patient?
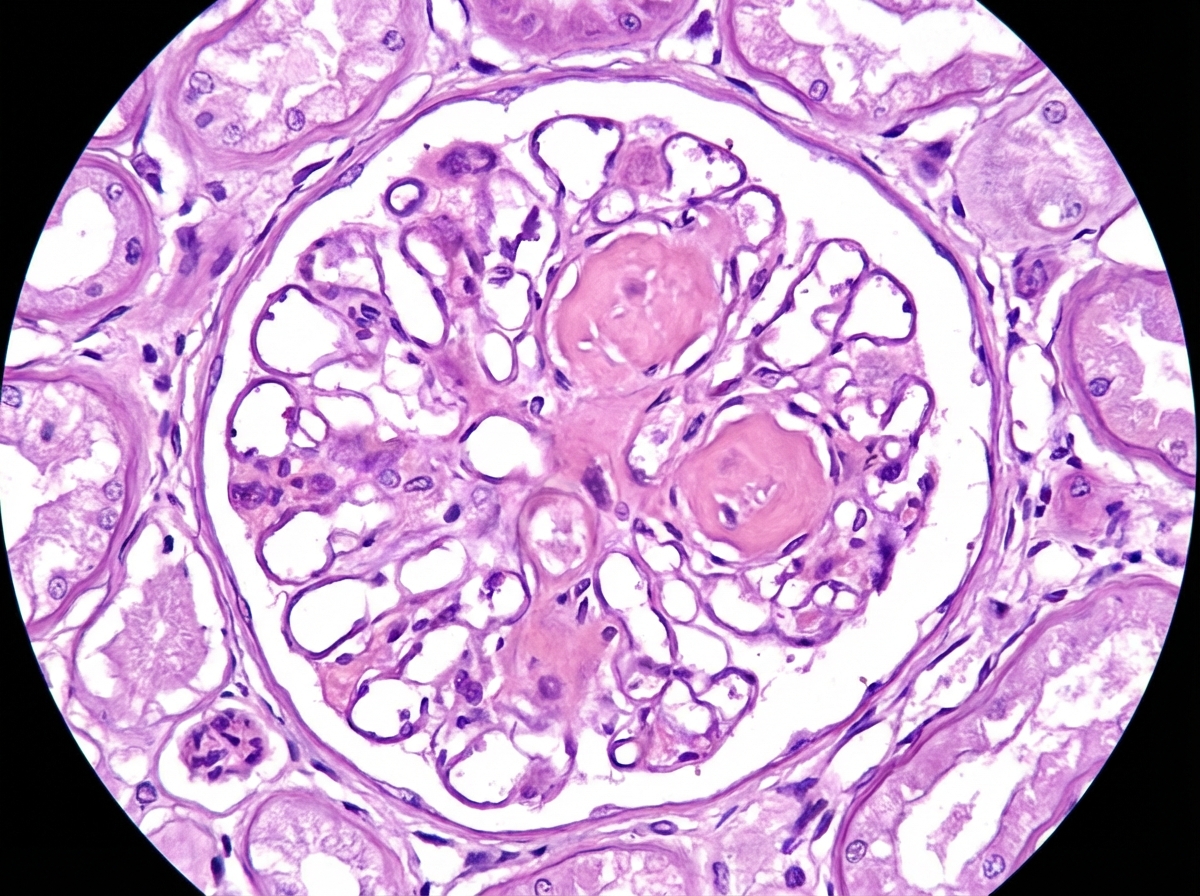
A 32-year-old woman presents to the office with complaints of frothy urine and swelling in her body that started 6 days ago. She says that she first noticed the swelling in her face that gradually involved other parts of her body. On further questioning, she gives a history of rheumatoid arthritis for 2 years. She is taking Penicillamine and Methotrexate for the past 6 months. Vitals include: blood pressure 122/89 mm Hg, pulse rate 55/min, temperature 36.7°C (98.0°F), and a respiratory rate 14/min. On examination, there is generalized pitting edema along with some subcutaneous nodules on the dorsal aspect of the forearm. Urinalysis pH 6.6 Color light yellow RBC none WBC 1–2/HPF Protein 4+ Cast fat globules Glucose absent Crystal none Ketone absent Nitrite absent 24 hours urine protein excretion 4.8 g Basic metabolic panel Sodium 141 mEq/L Potassium 5.1 mEq/L Chloride 101 mEq/L Bicarbonate 22 mEq/L Albumin 3.2 mg/dL Urea nitrogen 17 mg/dL Creatinine 1.3 mg/dL Uric Acid 6.8 mg/ dL Calcium 8.9 mg/ dL Glucose 111 mg/dL A renal biopsy is ordered which shows diffuse capillary and glomerular basement membrane thickening. Which of the following is the most likely cause for her impaired renal function?
A 62-year-old man comes to the physician because of fatigue and decreased urine output for 2 weeks. He has not been to the physician for many years and takes no medications. Serum studies show a urea nitrogen concentration of 42 mg/dL and a creatinine concentration of 2.3 mg/dL. Urinalysis shows heavy proteinuria. A photomicrograph of a section of a kidney biopsy specimen is shown. Which of the following is the most likely underlying cause of this patient's symptoms?
An 80-year-old woman died due to the respiratory complications of lung cancer. She had been a heavy smoker, and battled COPD and adenocarcinoma of the lungs for the last 20 years. The autopsy also revealed a pathological finding in the mitral valve. Which of the following was most likely seen?
A 30-year-old man presents to the emergency department with complaints of red, pinkish urine in the morning. He adds that he has been feeling some abdominal pain. The patient is not taking any medication, and his laboratory test results are as follows: Hb 11.0 g/dL RBC 3.7 x 1012/L WBC 4,000/mm3 PLT 100,000/mm3 Reticulocytes 17% of red cells Coombs test Negative Blood smear Polychromasia Which statement is true about this patient’s condition?
A 49-year-old female with a long history of poorly controlled diabetes mellitus visits her primary care physician with 2+ non-pitting edema in her legs. The patient has a serum creatinine of 2.9 mg/dL and a blood urea nitrogen of 61 mg/dL. A 24-hour urine collection reveals 8.5 grams of protein. A renal biopsy is obtained. Which of the following histologic findings is most likely to be seen upon tissue analysis:
A 26-year-old woman presents with episodes of intermittent fever, arthralgias, constant fatigue, weight loss, and plaque-like rash on sun-exposed areas, which have been gradually increasing over the last 6 months. On presentation, her vital signs include: blood pressure is 110/80 mm Hg, heart rate is 87/min, respiratory rate is 14/min, and temperature is 37.5°C (99.5°F). Physical examination reveals an erythematous scaling rash on the patient’s face distributed in a ‘butterfly-like’ fashion, erythematous keratinized patches on the sun-exposed areas, and mild lower leg edema. During the workup, the patient is found to be positive for anti-Sm (anti-Smith) antibodies. Which process is altered in this patient?
Practice by Chapter
Liver pathology (hepatitis, cirrhosis)
Practice Questions
Gallbladder and biliary tract disorders
Practice Questions
Pancreatic diseases
Practice Questions
Kidney diseases
Practice Questions
Male reproductive pathology
Practice Questions
Female reproductive pathology
Practice Questions
Breast pathology
Practice Questions
Endocrine pathology
Practice Questions
Bone and joint pathology
Practice Questions
Skeletal muscle diseases
Practice Questions
Peripheral nerve disorders
Practice Questions
Soft tissue tumors
Practice Questions
Head and neck pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
