Systemic Pathology — MCQs

On this page
At a routine exam, a 68-year-old woman is discovered to have a serum calcium level of 11.5 mg/dL. Follow-up laboratory tests show a high parathyroid hormone with low phosphorus and mildly elevated alkaline phosphatase. 24-hour urine calcium level is elevated. Review of symptoms includes complaints of fatigue, constipation, and diffuse bone pain for which she takes vitamin D. Past medical history is significant for type 2 diabetes mellitus for 25 years and essential hypertension for 15 years. The patient has a history of kidney stones. Family history is irrelevant. Which of the following radiologic findings is consistent with the patient's condition?
A 42-year-old woman comes to the physician with acute, severe pain in the middle of her lower back. She also complains of constipation and trouble sleeping recently. Menses occur regularly at 28-day intervals. Examination shows localized tenderness to palpation over the lumbar spine. Serum calcium is 14 mg/dL and serum phosphorus is 1.5 mg/dL. An x-ray of the lumbar spine shows a compression fracture of the L4 vertebral body and osteopenia. Which of the following is the most likely underlying cause of this patient's decreased bone mineral density?
A 70-year-old woman is on hospital day 2 in the medical intensive care unit. She was admitted from the emergency department for a 2-day history of shortness of breath and fever. In the emergency department, her temperature is 39.4°C (103.0°F), the pulse is 120/min, the blood pressure is 94/54 mm Hg, the respiratory rate is 36/min, and oxygen saturation was 82% while on 4L of oxygen via a non-rebreather mask. Chest X-ray shows a right lower lobe consolidation. She was intubated, sedated, and started on broad-spectrum antibiotics for sepsis of pulmonary origin and intravenous norepinephrine for blood pressure support. Since then, her clinical condition has been stable, though her vasopressor and oxygen requirements have not improved. Today, her physician is called to the bedside because her nurse noted some slow bleeding from her intravenous line sites and around her urinary catheter. Which of the following most likely represents the results of coagulation studies for this patient?
A 19-year-old man and recent immigrant from Brazil present to the clinic. He has no known past medical, past surgical, or family history. The patient admits to having several regular sexual partners. Today, he complains of a skin rash on his back. He is unclear when it started but became aware when one of his partners pointed it out. A review of systems is otherwise negative. Physical examination reveals numerous hypopigmented skin lesions over his upper back. When questioned, he states that they do not get darker after spending time in the sun. On examination, there is a 5 cm (1.9 in) patch of hypopigmented skin in the center of his back with a fine-scale overlying it. What is the most likely diagnosis?
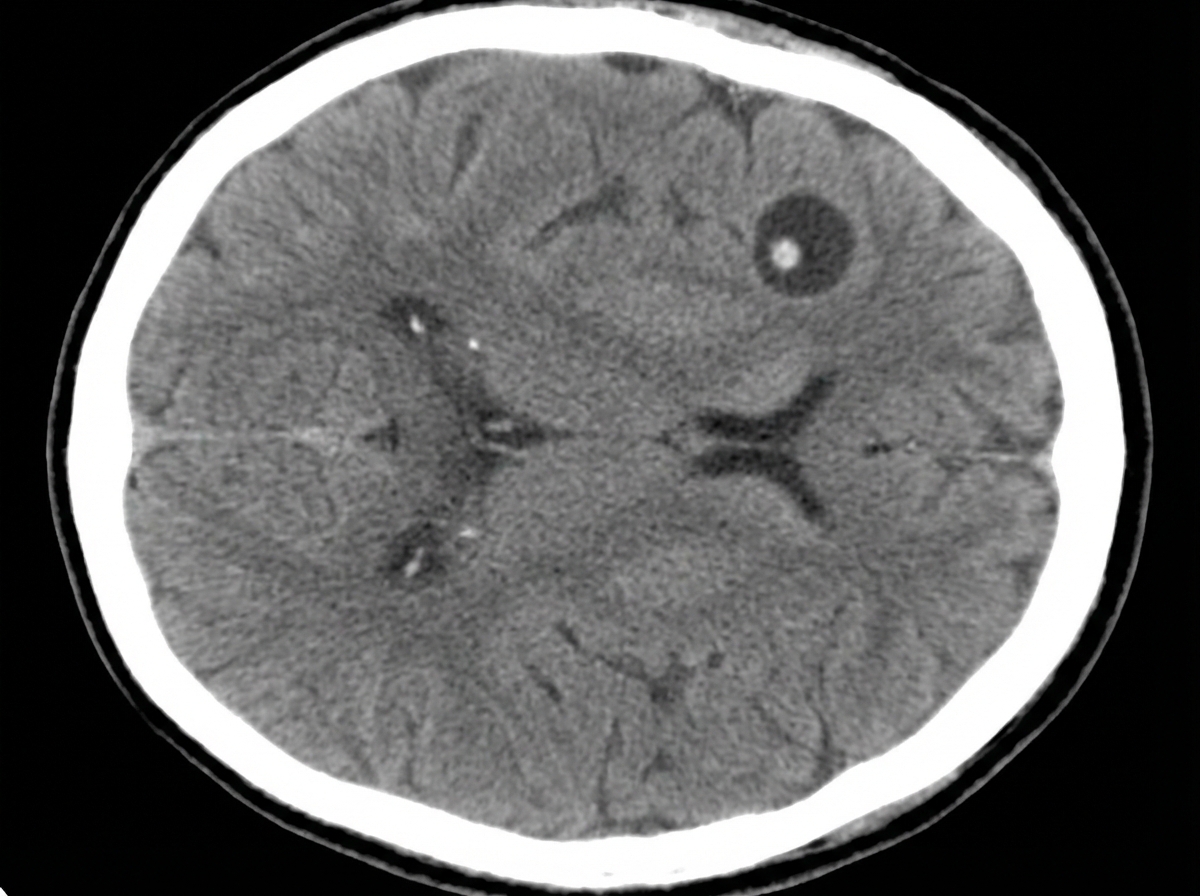
A 53-year-old woman with hypertension is brought to the emergency department 30 minutes after having a generalized, tonic-clonic seizure. She has had recurrent headaches and dizziness in the last 3 months. One year ago, she had diarrhea after a trip to Ecuador that resolved without treatment. She has not received any medical care in the last five years. She has smoked 1 pack of cigarettes daily for 20 years. Her temperature is 36°C (96.8°F) and blood pressure is 159/77mm Hg. Physical examination shows dysarthria and hyperreflexia. She is confused and oriented only to name and place. Four brain lesions are found in a CT scan of the brain; one of the lesions is shown. Which of the following is most likely to have prevented this patient's condition?
A 16-year-old boy is brought to the pediatrician by his mother because she is concerned about the “spots” on his abdomen and back. The patient’s mother reports that there are several “light spots” on the patient’s trunk that have been slowly increasing in number. The lesions are not painful nor pruritic. The patient’s mother is worried because her nephew had vitiligo. The patient reports that he feels “fine,” but reports occasional headaches and increasing difficulty with seeing the board at school. In addition to the patient’s cousin having vitiligo, the patient’s paternal grandfather and uncle have bilateral deafness, and his mother has systemic lupus erythematous. On physical examination, there are multiple, discrete, 2-3 cm hypopigmented macules on the chest, abdomen, back, and posterior shoulders. Which of the following head and neck computed tomography findings is the patient most likely to develop?
A 72-year-old African American man presents with progressive fatigue, difficulty breathing on exertion, and lower extremity swelling for 3 months. The patient was seen at the emergency department 2 times before. The first time was because of back pain, and the second was because of fever and cough. He took medications at the emergency room, but he refused to do further tests recommended to him. He does not smoke or drink alcohol. His family history is irrelevant. His vital signs include a blood pressure of 110/80 mm Hg, temperature of 37.2°C (98.9°F), and regular radial pulse of 90/min. On physical examination, the patient looks pale, and his tongue is enlarged. Jugular veins become distended on inspiration. Pitting ankle edema is present on both sides. Bilateral basal crackles are audible on the chest auscultation. Hepatomegaly is present on abdominal palpation. Chest X-ray shows osteolytic lesions of the ribs. ECG shows low voltage waves and echocardiogram shows a speckled appearance of the myocardium with diastolic dysfunction and normal appearance of the pericardium. Which of the following best describes the mechanism of this patient’s illness?
A 56-year-old African-American man comes to the physician for intermittent episodes of dark urine and mild flank pain. The patient has had 3 episodes of frank reddish discoloration of his urine within 1 month. He has chronic headaches and back pain for which he has been taking aspirin and ibuprofen daily for 1 year. The patient has sickle cell trait. He has smoked a pack of cigarettes daily for 10 years. He appears well. His temperature is 37.4°C (99.3°F). His pulse is 66/min, and his blood pressure is 150/90 mm Hg. Physical exam shows mild, bilateral flank tenderness. Laboratory analysis shows a serum creatinine concentration of 2.4 mg/dL. Urine studies are shown below. Urine Blood 3+ Protein 2+ RBC > 10/hpf WBC 3/hpf Which of the following is the most likely underlying cause of this patient's hematuria?
A 67-year-old male presents with left hip pain. Examination reveals mild effusions in both knees, with crepitus in both patellofemoral joints. He states his hearing has worsened recently and that he feels like his hats don't fit anymore. Bone scan reveals diffuse uptake in the calvarium, right proximal femur, and left ilium. Which of the following laboratory abnormalities would be expected in this patient?
A 23-year-old woman presents to the emergency department with a 3-day history of fever and headache. She says that the symptoms started suddenly after she woke up 3 days ago, though she has been feeling increasingly fatigued over the last 5 months. On presentation, her temperature is 102°F (38.9°C), blood pressure is 117/74 mmHg, pulse is 106/min, and respirations are 14/min. Physical exam reveals diffuse petechiae and conjunctival pallor and selected laboratory results are shown as follows: Bleeding time: 11 minutes Platelet count: 68,000/mm^3 Lactate dehydrogenase: 105 U/L Which of the following would also most likely be true for this patient?
Practice by Chapter
Liver pathology (hepatitis, cirrhosis)
Practice Questions
Gallbladder and biliary tract disorders
Practice Questions
Pancreatic diseases
Practice Questions
Kidney diseases
Practice Questions
Male reproductive pathology
Practice Questions
Female reproductive pathology
Practice Questions
Breast pathology
Practice Questions
Endocrine pathology
Practice Questions
Bone and joint pathology
Practice Questions
Skeletal muscle diseases
Practice Questions
Peripheral nerve disorders
Practice Questions
Soft tissue tumors
Practice Questions
Head and neck pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
