Systemic Pathology — MCQs

On this page
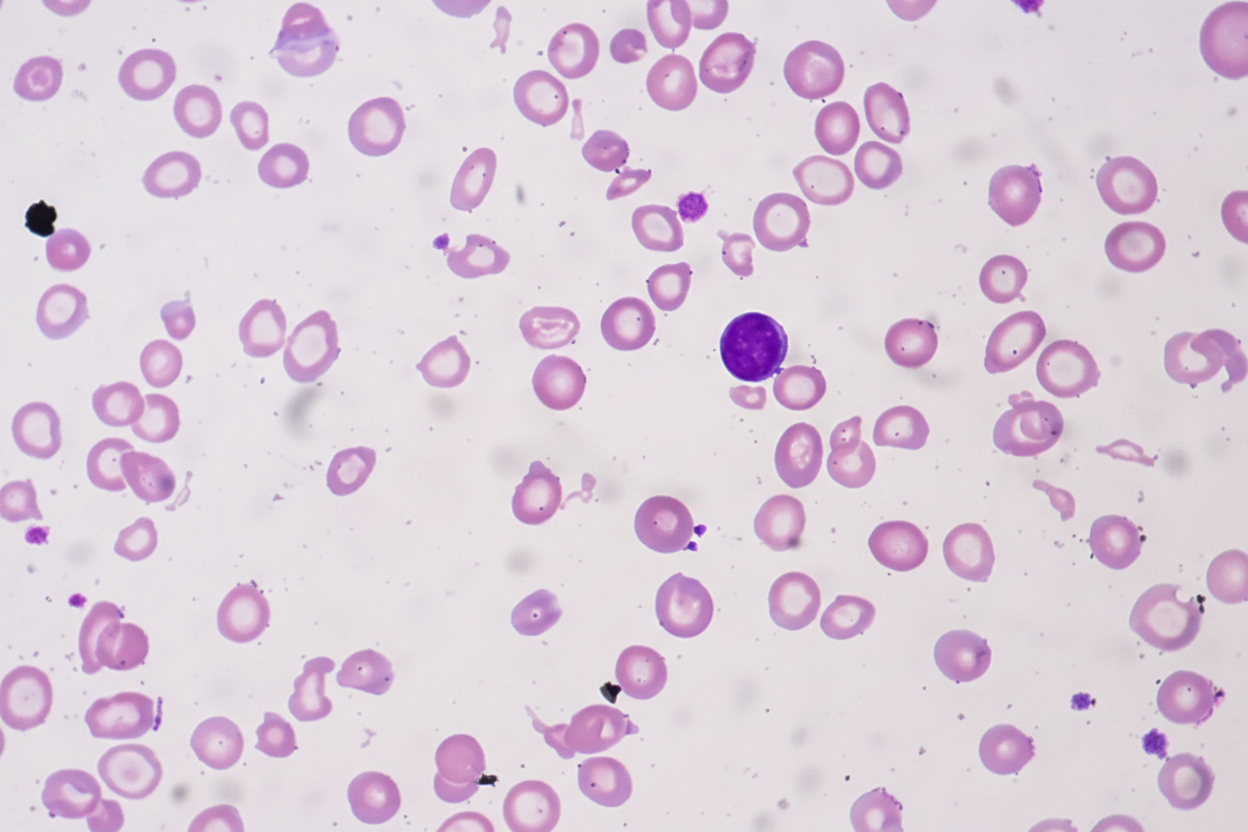
A 33-year-old G2P2 woman presents with a history of fatigue and difficulty breathing upon exertion. She was not able to tolerate antenatal vitamin supplements due to nausea and constipation. Her vital signs include: temperature 37.0°C (98.6°F), blood pressure 112/64 mm Hg, and pulse 98/min. Physical examination reveals conjunctival pallor and spoon nails. Laboratory findings are significant for the following: Hemoglobin 9.1 g/dL Hematocrit 27.3% Mean corpuscular volume (MCV) 73 μm3 Mean corpuscular hemoglobin (MCH) 21 pg/cell Red cell distribution width (RDW) 17.5% (ref: 11.5–14.5%) Serum ferritin 9 ng/mL Which of the following would most likely be seen on a peripheral blood smear in this patient?
A 35-year-old G4P1 woman presents for follow-up after her 3rd miscarriage. All 3 miscarriages occurred during the 2nd trimester. Past medical history is significant for systemic lupus erythematosus (SLE) and a deep vein thrombosis (DVT) in her right lower leg 3 years ago. Her current medication is hydroxychloroquine. The patient denies any tobacco, alcohol, and illicit substance use. Her vitals include: temperature 36.8℃ (98.2℉), blood pressure 114/76 mm Hg, pulse 84/min, respiration rate 12/min. Physical examination reveals a lacy, violaceous discoloration on her lower legs. Which of the following autoantibodies would this patient most likely test positive for?
Two weeks after undergoing allogeneic stem cell transplant for multiple myeloma, a 55-year-old man develops a severely pruritic rash, abdominal cramps, and profuse diarrhea. He appears lethargic. Physical examination shows yellow sclerae. There is a generalized maculopapular rash on his face, trunk, and lower extremities, and desquamation of both soles. His serum alanine aminotransferase is 115 U/L, serum aspartate aminotransferase is 97 U/L, and serum total bilirubin is 2.7 mg/dL. Which of the following is the most likely underlying cause of this patient's condition?
A 61-year-old woman comes to the physician for evaluation of numbness and a burning sensation in her feet for the past 5 months. She has type 2 diabetes mellitus and hypercholesterolemia. Her blood pressure is 119/82 mm Hg. Neurologic examination shows decreased sensation to pinprick, light touch, and vibration over the soles of both feet. There is a nontender ulcer on the plantar surface of her left foot. Pedal pulses are strong bilaterally. Her hemoglobin A1c concentration is 8.6%. Which of the following processes is most likely involved in the pathogenesis of this patient's current symptoms?
A 59-year-old woman comes to the physician because of upper extremity weakness and fatigue for the past 4 months. She has had difficulty combing her hair and lifting objects. She has also had difficulty rising from her bed in the mornings for 2 months. Over the past month, she started using over-the-counter mouth rinses for dry mouth. She has smoked 1 pack of cigarettes daily for 40 years. Examination shows decreased deep tendon reflexes. Repetitive muscle tapping shows increased reflex activity. There are no fasciculations or muscle atrophy. A low-dose CT scan of the chest shows a 3-cm mass with heterogeneous calcifications in the center of the right lung. Which of the following is the most likely underlying mechanism responsible for this patient’s current symptoms?
A 38-year-old woman comes to the physician because of a 1-month history of fatigue and pruritus. Examination of the abdomen shows an enlarged, nontender liver. Serum studies show an alkaline phosphatase level of 140 U/L, aspartate aminotransferase activity of 18 U/L, and alanine aminotransferase activity of 19 U/L. Serum antimitochondrial antibody titers are elevated. A biopsy specimen of this patient's liver is most likely to show which of the following findings?
A 42-year-old male presents to his primary care physician with complaints of fatigue and occasionally darkened urine over the past 3 months. Upon further questioning, the patient reveals that he has regularly had dark, 'cola-colored' urine when he has urinated at night or early in the morning. However, when he urinates during the day, it appears a much lighter yellow color. Laboratory work-up is initiated and is significant for a hemoglobin of 10.1 g/dL, elevated LDH, platelet count of 101,000/uL, and leukopenia. Urinalysis, taken from an early morning void, reveals brown, tea-colored urine with hemoglobinuria and elevated levels of hemosiderin. Which of the following is responsible for this patient's presentation?
A 39-year-old man presents to the emergency room for epistaxis. He reports having frequent nosebleeds over the past 48 hours. He also reports a constant pounding headache over the same timeframe. He is accompanied by his wife who reports that he has seemed "off" lately, frequently forgetting recent events and names of his friends. His past medical history is notable for hypertension and rheumatoid arthritis. He takes lisinopril and methotrexate. He has a 10 pack-year smoking history and drinks 2-3 beers per day. His temperature is 101.1°F (38.4°C), blood pressure is 145/90 mmHg, pulse is 110/min, and respirations are 18/min. On exam, he appears pale, diaphoretic, and has mild scleral icterus. His spleen is palpable but non-tender. Laboratory analysis is shown below: Hemoglobin: 8.9 g/dL Hematocrit: 26% Leukocyte count: 4,900/mm^3 with normal differential Platelet count: 25,000/mm^3 Prothrombin time: 14 seconds Partial thromboplastin time (activated): 27 seconds International normalized ratio: 1.1 Bleeding time: 9 minutes This patient has a condition that is caused by a defect in which of the following processes?
A 33-year-old woman is brought to the emergency department after she was involved in a high-speed motor vehicle collision. She reports severe pelvic pain. Her pulse is 124/min and blood pressure is 80/56 mm Hg. Physical examination shows instability of the pelvic ring. As part of the initial emergency treatment, she receives packed red blood cell transfusions. Suddenly, the patient starts bleeding from peripheral venous catheter insertion sites. Laboratory studies show decreased platelets, prolonged prothrombin time and partial thromboplastin time, and elevated D-dimer. A peripheral blood smear of this patient is most likely to show which of the following findings?
A 25-year-old African-American woman visits the doctor’s office complaining of fatigue for a couple of months. She says that she feels exhausted by the end of the day. She works as a dental assistant and is on her feet most of the time. However, she eats well and also tries to walk for 30 minutes every morning. She also says that she sometimes feels breathless and has to gasp for air, especially when she is walking or jogging. Her past medical history is insignificant, except for occasional bouts of cold during the winters. Her physical exam findings are within normal limits except for moderate conjunctival pallor. Complete blood count results and iron profile are as follows: Hemoglobin 9 g/dL Hematocrit 28.5% RBC count 5.85 x 106/mm3 WBC count 5,500/mm3 Platelet count 212,000/mm3 MCV 56.1 fl MCH 20.9 pg/cell MCHC 25.6 g/dL RDW 11.7% Hb/cell Serum iron 170 mcg/dL Total iron-binding capacity (TIBC) 458 mcg/dL Transferrin saturation 60% A peripheral blood smear is given. When questioned about her family history of anemia, she says that all she remembers is her dad was never allowed to donate blood as he was anemic. Which of the following most likely explains her cell counts and blood smear results?
Practice by Chapter
Liver pathology (hepatitis, cirrhosis)
Practice Questions
Gallbladder and biliary tract disorders
Practice Questions
Pancreatic diseases
Practice Questions
Kidney diseases
Practice Questions
Male reproductive pathology
Practice Questions
Female reproductive pathology
Practice Questions
Breast pathology
Practice Questions
Endocrine pathology
Practice Questions
Bone and joint pathology
Practice Questions
Skeletal muscle diseases
Practice Questions
Peripheral nerve disorders
Practice Questions
Soft tissue tumors
Practice Questions
Head and neck pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
