Systemic Pathology — MCQs

On this page
A pathologist receives a patient sample for analysis. Cells in the sample are first labeled with fluorescent antibodies and then passed across a laser beam in a single file of particles. The light scatter and fluorescent intensity of the particles are plotted on a graph; this information is used to characterize the sample. This laboratory method would be most useful to establish the diagnosis of a patient with which of the following?
A 15-year-old boy is brought to the physician because his urine has been pink since that morning. During the past 2 days, he has had a sore throat and difficulty swallowing. He also reports having a low-grade fever. He has no pain with urination or changes in urinary frequency. He has had 2 similar episodes involving a sore throat and pink urine over the past 2 years. His older sister has systemic lupus erythematosus. His temperature is 38.3°C (101°F), pulse is 76/min, and blood pressure is 120/80 mm Hg. Oral examination shows an erythematous pharynx and enlarged tonsils. The remainder of the examination shows no abnormalities. Laboratory studies show: Leukocyte count 20,000/mm3 Serum Urea nitrogen 8 mg/dL Creatinine 1.4 mg/dL Urine Blood 3+ Protein 1+ RBC 15–17/hpf with dysmorphic features RBC casts numerous Ultrasound of both kidneys shows no abnormalities. A renal biopsy is most likely to show which of the following findings?
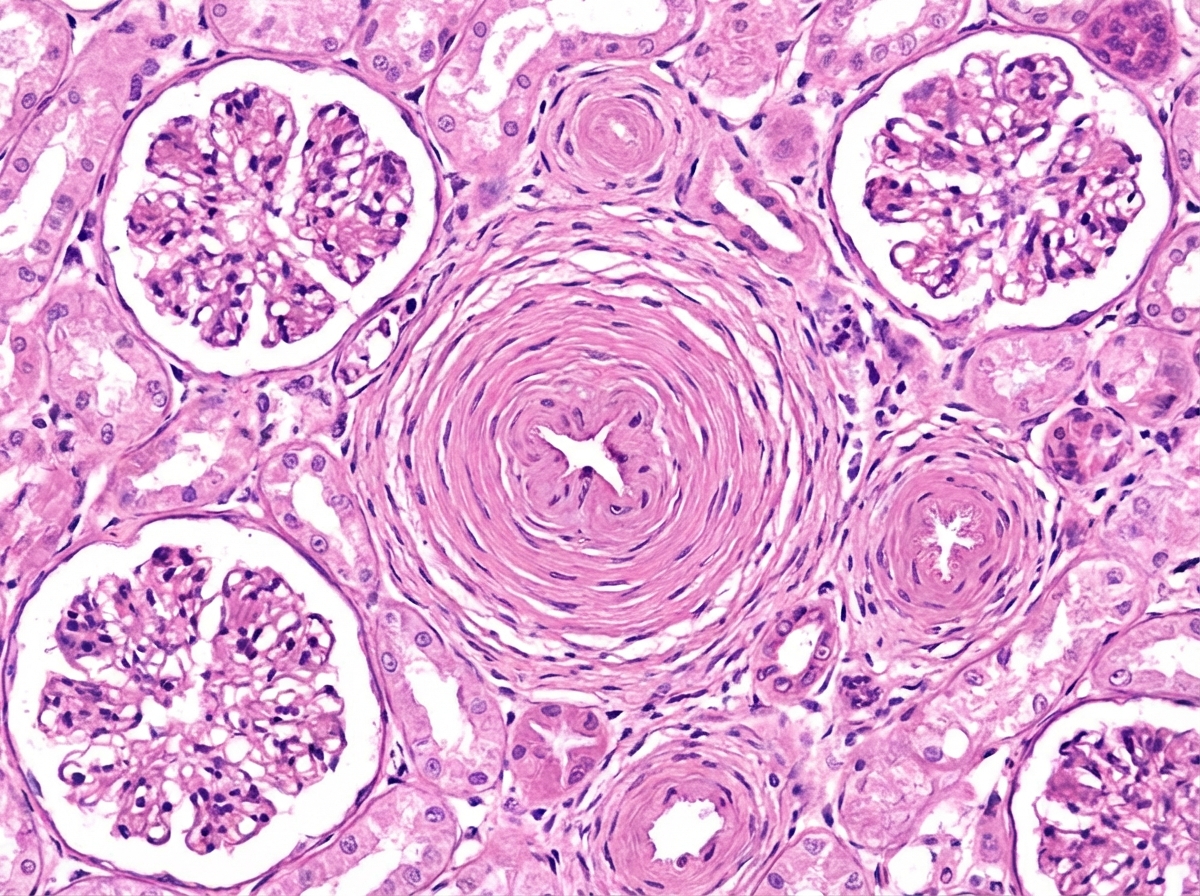
A 53-year-old man is brought to the emergency department by his wife because of a 1-day history of headache, blurry vision, and confusion. His wife also says that he hasn't urinated in the past 24 hours. Despite appropriate measures, the patient dies shortly after admission. A photomicrograph of a section of the kidney obtained at autopsy is shown. Which of the following is the most likely explanation for the findings indicated by the arrow?
A 17-year-old is brought to his primary care provider by his mother. They are concerned that his acne is getting worse and may leave scars. They have tried several over the counter products without success. He is otherwise healthy and without complaint. The boy was born at 39 weeks gestation via spontaneous vaginal delivery. He is up to date on all vaccines with some delay in reaching developmental milestones, especially in language development. He is having trouble with school and has a history of detentions for misbehavior and acting out. On examination, he stands 6 ft 3 inches tall, considerably taller than either parent or other family members with inflamed pustular acne on his face, shoulders, and chest. He is otherwise healthy. Which of the following karyotypes is most likely associated with this patient’s clinical features?
A 6-month-old male presents to the emergency department with his parents after his three-year-old brother hit him on the arm with a toy truck. His parents are concerned that the minor trauma caused an unusual amount of bruising. The patient has otherwise been developing well and meeting all his milestones. His parents report that he sleeps throughout the night and has just started to experiment with solid food. The patient’s older brother is in good health, but the patient’s mother reports that some members of her family have an unknown blood disorder. On physical exam, the patient is agitated and difficult to soothe. He has 2-3 inches of ecchymoses and swelling on the lateral aspect of the left forearm. The patient has a neurological exam within normal limits and pale skin with blue irises. An ophthalmologic evaluation is deferred. Which of the following is the best initial step?
A 69-year-old white man comes to the physician because of a 15-day history of fatigue and lower leg swelling. Over the past 8 months, he has had a 3.8-kg (8.3-lb) weight loss. He has smoked one pack of cigarettes daily for 48 years. Vital signs are within normal limits. He appears thin. Examination shows 2+ pretibial edema bilaterally. An x-ray of the chest shows a right upper lobe density. Laboratory studies show: Hemoglobin 11.3 g/dL Leukocyte count 8600/mm3 Platelet count 140,000/mm3 Serum Urea nitrogen 25 mg/dL Glucose 79 mg/dL Creatinine 1.7 mg/dL Albumin 1.6 mg/dL Total cholesterol 479 mg/dL Urine Blood negative Glucose negative Protein 4+ WBC 0–1/hpf Fatty casts numerous Light microscopic examination of a kidney biopsy reveals thickening of glomerular capillary loops and the basal membrane. Which of the following is the most likely diagnosis?
A 6-year-old boy presents to your office with hematuria. Two weeks ago the patient had symptoms of a sore throat and fever. Although physical exam is unremarkable, laboratory results show a decreased serum C3 level and an elevated anti-DNAse B titer. Which of the following would you most expect to see on renal biopsy?
A 50-year-old man presents to a clinic with oliguria. Four weeks ago, he had a kidney transplant. Postoperative follow-up was normal. He is currently on cyclosporine and admits that sometimes he forgets to take his medication. On physical examination, the vital signs include: temperature 37.1°C (98.8°F), blood pressure 165/110 mm Hg, heart rate 80/min, and respiratory rate 16/min. There is mild tenderness on renal palpation. His serum creatinine level is 4 mg/dL, well above his baseline level after the transplant. Which of the following best describes the histological finding if a biopsy is taken from the transplanted kidney?
A 22-year-old woman presents to her primary care physician complaining of a red, itchy rash on her elbows and shoulders for 2 months. She has no history of medical problems, and review of systems is positive only for occasional loose stools. She is appropriately prescribed dapsone, which relieves the rash within hours. What is the diagnosis?
A 10-year-old male presents with his mother with multiple complaints. A few weeks ago, he had a sore throat for several days that improved without specific therapy. Additionally, over the past several days he has experienced pain in his ankles and wrists and, more recently, his left knee. His mother also noted several bumps on both of his elbows, and he has also had some pain in his center of his chest. He thinks the pain is better when he leans forward. On physical examination, he is noted to be mildly febrile, and a pericardial friction rub is auscultated. Which of the following histopathologic findings is most likely associated with this patient's condition?
Practice by Chapter
Liver pathology (hepatitis, cirrhosis)
Practice Questions
Gallbladder and biliary tract disorders
Practice Questions
Pancreatic diseases
Practice Questions
Kidney diseases
Practice Questions
Male reproductive pathology
Practice Questions
Female reproductive pathology
Practice Questions
Breast pathology
Practice Questions
Endocrine pathology
Practice Questions
Bone and joint pathology
Practice Questions
Skeletal muscle diseases
Practice Questions
Peripheral nerve disorders
Practice Questions
Soft tissue tumors
Practice Questions
Head and neck pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
