Systemic Pathology — MCQs

On this page
A 46-year-old man comes to the physician because of a 4-month history of progressively worsening fatigue and loss of appetite. Five years ago, he received a kidney transplant from a living family member. Current medications include sirolimus and mycophenolate. His blood pressure is 150/95 mm Hg. Laboratory studies show normocytic, normochromic anemia and a serum creatinine concentration of 3.1 mg/dL; his vital signs and laboratory studies were normal 6 months ago. Which of the following is the most likely underlying mechanism of this patient’s increase in creatinine concentration?
A 53-year-old woman presents to her physician for evaluation of sudden onset respiratory distress for the past few hours. The past medical history includes a myocardial infarction 2 years ago. The vital signs include a blood pressure 70/40 mm Hg, pulse 92/min, respiratory rate 28/min, and SpO2 92% on room air. The physical examination reveals bilateral basal crepitations on auscultation. The echocardiogram reveals an ejection fraction of 34%. She is admitted to the medical floor and started on furosemide. The urine output in 24 hours is 400 mL. The blood urea nitrogen is 45 mg/dL and the serum creatinine is 1.85 mg/dL. The fractional excretion of sodium is 2.4%. Urinalysis revealed muddy brown granular casts. Which of the following is the most likely cause of the abnormal urinalysis?
A 45-year-old woman presents with severe, acute-onset colicky abdominal pain and nausea. She also describes bone pain, constipation, headache, decreased vision, and menstrual irregularity. Past medical history is significant for surgical removal of an insulinoma one year ago. Two months ago, she was prescribed fluoxetine for depression but hasn’t found it very helpful. Family history is significant for a rare genetic syndrome. Non-contrast CT, CBC, CMP, and urinalysis are ordered in the diagnostic work-up. Urine sediment is significant for the findings shown in the picture. Which of the following will also be a likely significant finding in the diagnostic workup?

An autopsy of a patient's heart who recently died in a motor vehicle accident shows multiple nodules near the line of closure on the ventricular side of the mitral valve leaflet. Microscopic examination shows that these nodules are composed of immune complexes, mononuclear cells, and thrombi interwoven with fibrin strands. These nodules are most likely to be found in which of the following patients?
A 32-year-old man presents with a history of diarrhea several days after eating a hot dog at a neighborhood barbeque. He notes that the diarrhea is visibly bloody, but he has not experienced a fever. He adds that several other people from his neighborhood had similar complaints, many of which required hospitalization after eating food at the same barbeque. His temperature is 37°C (98.6°F ), respiratory rate is 16/min, pulse is 77/min, and blood pressure is 100/88 mm Hg. A physical examination is performed and is within normal limits. Blood is drawn for laboratory testing. The results are as follows: Hb%: 12 gm/dL Total count (WBC): 13,100/mm3 Differential count: Neutrophils: 80% Lymphocytes: 15% Monocytes: 5% ESR: 10 mm/hr Glucose, Serum: 90 mg/dL BUN: 21 mg/dL Creatinine, Serum: 1.96 mg/dL Sodium, Serum: 138 mmol/L Potassium, Serum: 5.2 mmol/L Chloride, Serum: 103 mmol/L Bilirubin, Total: 2.5 mg/dL Alkaline Phosphatase, Serum: 66 IU/L Aspartate aminotransferase (AST): 32 IU/L Alanine aminotransferase (ALT): 34 IU/L Urinalysis is normal except for RBC casts. What is the most concerning possible complication?
A 56-year-old African American woman comes to the physician because of frequent urination. For the past year, she has had to urinate multiple times every hour. She has been thirstier and hungrier than usual. She has not had any pain with urination. She has no time to exercise because she works as an accountant. Her diet mostly consists of pizza and cheeseburgers. Her vital signs are within normal limits. Physical examination shows no abnormalities. Today, her blood glucose level is 200 mg/dL and her hemoglobin A1c is 7.4%. Urinalysis shows microalbuminuria. Which of the following is the most likely cause of this patient's proteinuria?
A 67-year-old man comes to the emergency department for the evaluation of two episodes of red urine since this morning. He has no pain with urination. He reports lower back pain and fever. Six months ago, he was diagnosed with osteoarthritis of the right knee that he manages with 1–2 tablets of ibuprofen per day. He has smoked one pack of cigarettes daily for the past 45 years. He does not drink alcohol. His temperature is 38.5°C (101.3°F), pulse is 95/min, and blood pressure is 130/80 mm Hg. Physical examination shows faint, diffuse maculopapular rash, and bilateral flank pain. The remainder of the examination shows no abnormalities. Urinalysis shows: Blood +3 Protein +1 RBC 10–12/hpf RBC cast negative Eosinophils numerous Which of the following is the most likely diagnosis?
A 12-year-old boy who recently immigrated from Namibia is being evaluated for exertional shortness of breath and joint pain for the past month. His mother reports that he used to play soccer but now is unable to finish a game before he runs out of air or begins to complain of knee pain. He was a good student but his grades have recently been declining over the past few months. The mother recalls that he had a sore throat and didn't go to school for 3 days a few months ago. He had chickenpox at the age of 5 and suffers from recurrent rhinitis. He is currently taking over-the-counter multivitamins. His blood pressure is 110/90 mm Hg, pulse rate is 55/min, and respiratory rate is 12/min. On physical examination, subcutaneous nodules are noted on his elbows bilaterally. On cardiac auscultation, a holosystolic murmur is heard over the mitral area that is localized. Lab work shows: Hemoglobin 12.9 g/dL Hematocrit 37.7% Leukocyte count 5,500/mm3 Neutrophils 65% Lymphocytes 30% Monocytes 5% Mean corpuscular volume 82.2 fL Platelet count 139,000/mm3 Erythrocyte sedimentation rate 35 mm/h C-reactive protein 14 mg/dL Antistreptolysin O (ASO) 400 IU (normal range: < 200 IU) Which is the mechanism behind the cause of this boy's symptoms?
A 46-year-old man diagnosed with pancreatic adenocarcinoma is admitted with fever, malaise, and dyspnea. He says that symptoms onset 2 days ago and have progressively worsened. Past medical history is significant for multiple abdominal surgeries including stenting of the pancreatic duct. Current inpatient medications are rosuvastatin 20 mg orally daily, aspirin 81 mg orally daily, esomeprazole 20 mg orally daily, oxycontin 10 mg orally twice daily, lorazepam 2 mg orally 3 times daily PRN, and ondansetron 10 mg IV. On admission, his vital signs include blood pressure 105/75 mm Hg, respirations 22/min, pulse 90/min, and temperature 37.0°C (98.6°F). On his second day after admission, the patient acutely becomes obtunded. Repeat vital signs show blood pressure 85/55 mm Hg, respirations 32/min, pulse 115/min. Physical examination reveals multiple ecchymoses on the trunk and extremities and active bleeding from all IV and venipuncture sites. There is also significant erythema and swelling of the posterior aspect of the left leg. Laboratory findings are significant for thrombocytopenia, prolonged PT and PTT, and an elevated D-dimer. Blood cultures are pending. Which of the following is most likely responsible for this patient’s current condition?
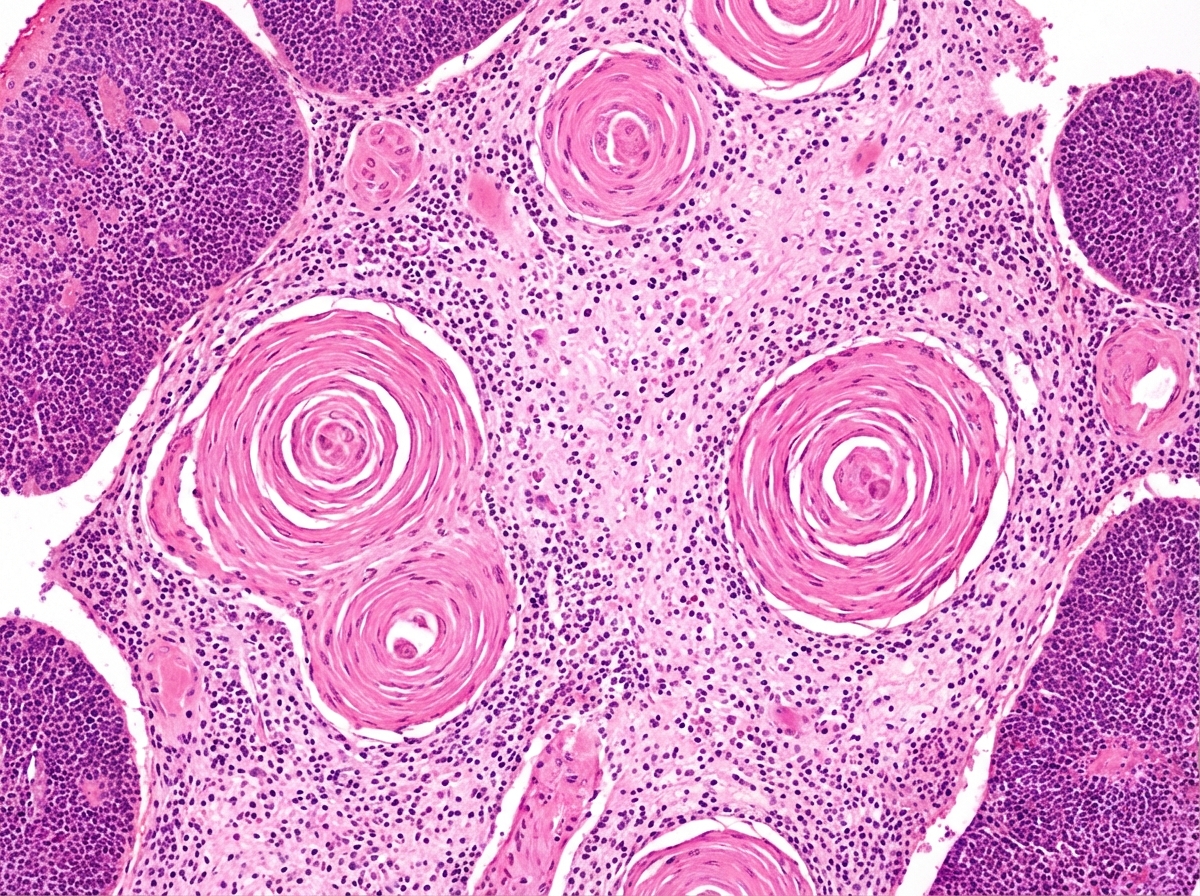
A section from the thymus of a patient with myasthenia gravis is examined (see image). The function of the portion of the thymus designated by the arrow plays what role in the pathophysiology of this disease?
Practice by Chapter
Liver pathology (hepatitis, cirrhosis)
Practice Questions
Gallbladder and biliary tract disorders
Practice Questions
Pancreatic diseases
Practice Questions
Kidney diseases
Practice Questions
Male reproductive pathology
Practice Questions
Female reproductive pathology
Practice Questions
Breast pathology
Practice Questions
Endocrine pathology
Practice Questions
Bone and joint pathology
Practice Questions
Skeletal muscle diseases
Practice Questions
Peripheral nerve disorders
Practice Questions
Soft tissue tumors
Practice Questions
Head and neck pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
