Systemic Pathology — MCQs

On this page
A 31-year-old woman presents to her primary care provider to discuss the results from a previous urine analysis. She has no new complaints and feels well. Past medical history is significant for systemic lupus erythematosus. She was diagnosed 5 years ago and takes hydroxychloroquine every day and prednisone when her condition flares. Her previous urine analysis shows elevated protein levels (4+) and blood (3+). The urine sediment contained red blood cells (6 RBCs/high-power field). The treating physician would like to perform a renal biopsy to rule out lupus nephritis. What type of hypersensitivity is suggestive of lupus nephritis?
A 65-year-old patient presents with rapidly progressive dementia, myoclonus, and ataxia over 3 months. Laboratory studies, including serum vitamin B12 (cyanocobalamin), thyroxine (T4), and thyroid-stimulating hormone concentrations, are within normal limits. A lumbar puncture is performed. Cerebrospinal fluid (CSF) analysis is most likely to show which of the following?
A 29-year-old GP10 woman at 24 weeks estimated gestational age presents for follow-up. Six weeks ago, a complete blood count showed a microcytic hypochromic anemia for which she was prescribed iron sulfate tablets. A repeat complete blood count today shows no improvement in her hemoglobin level. Past medical history is significant for her being Rh-positive with an Rh-negative partner. She emigrated to the United States with her husband 7 years ago and did not have regular medical care in her country. An abdominal ultrasound shows findings consistent with hydrops fetalis. Which of the following is the most likely etiology of the condition of her fetus?
A 25-year-old female with no significant past medical history presents to her primary care physician with several weeks of increased fatigue and decreased exercise tolerance. On physical exam, her skin and conjunctiva appear pale. The physician suspects some form of anemia and orders a complete blood panel, which is remarkable for hemoglobin 11.7 g/dl, MCV 79 fL, MCHC 38% (normal 31.1-34%), and reticulocyte index 3.6%. Peripheral blood smear shows red blood cells with a lack of central pallor. This patient would most likely develop which of the following conditions?
An otherwise healthy 42-year-old man undergoes routine investigations prior to blood donation. His complete blood count is shown: Hemoglobin 9.3 g/dL Mean corpuscular volume (MCV) 71 μm3 Mean corpuscular hemoglobin (MCH) 21 pg/cell White blood cell count 8,200/mm3 Platelet count 317,000/mm3 Iron studies are shown: Serum iron 210 μg/dL Serum ferritin 310 ng/mL Total iron binding capacity (TIBC) 290 μg/dL Transferrin saturation 78% He occasionally drinks alcohol and denies smoking or use of illicit drugs. There is a family history of anemia including his brother and maternal uncle. Examination shows conjunctival pallor, but is otherwise unremarkable. Which of the following is the most likely diagnosis?
A 32-year-old woman is brought to your office by her husband. The husband says that she had been acting strange lately. She has been forgetful, and she sometimes becomes angered for no reason, which is highly unusual for her. She has also been having random, uncontrollable movements, which are also new. On examination, she appears withdrawn and flat. On further questioning, she reveals that her father died at age 45 from a movement disorder. Which of the following is the pathological hallmark of the patient's condition?
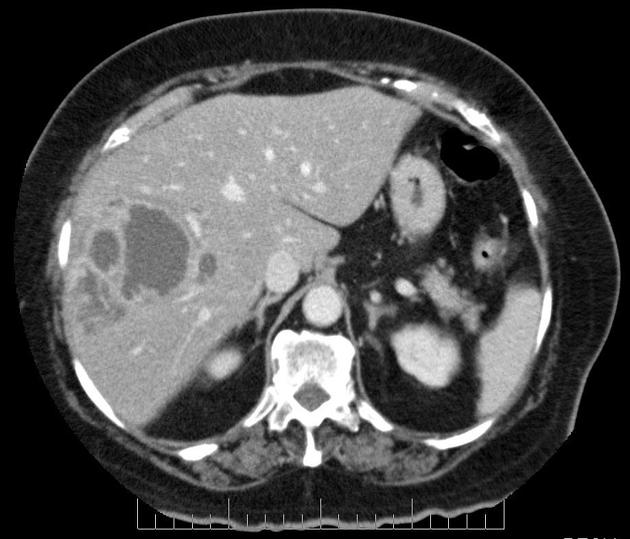
A 40-year-old man presents to the office with complaints of epigastric discomfort for the past 6 months. He adds that the discomfort is not that bothersome as it does not interfere with his daily activities. He does not have any other complaints at the moment. The past medical history is insignificant. He is a non-smoker and does not consume alcohol. He recently came back from a trip to South America where he visited a relative who owned a sheep farm. On physical examination, he has a poorly palpable epigastric non-tender mass with no organomegaly. The hepatitis B and C serology are negative. The liver CT scan and MRI are shown. What is the most likely diagnosis?
A 60-year-old African American woman presents to her family physician with shortness of breath on exertion. She also describes shortness of breath when she lies down to go to bed at night, as well as recent swelling in her ankles. Past medical history is significant for long-standing hypertension, for which she takes amlodipine and lisinopril. Her temperature is 36.8°C (98.2°F), the heart rate is 90/min, the respiratory rate is 15/min, and the blood pressure is 135/80 mm Hg. The physical exam is significant for JVD, lower extremity pitting edema, laterally displaced PMI, left ventricular heave, bilateral pulmonary crackles, and an S4 heart sound. Chest X-ray demonstrates pulmonary vascular congestion, Kerley B lines, and cardiomegaly. Echocardiogram demonstrates a preserved ejection fraction. Kidney biopsy would likely demonstrate which of the following?
A 65-year-old African-American woman comes to the physician because of severe lower back pain. She has had dull lower back pain for several months, which suddenly become sharp in nature after lifting a heavy bucket of water 2 days ago. The pain is midline and does not radiate. She has had frequent vaginal dryness and hot flashes since menopause at the age of 55 years, for which she is on hormone replacement therapy. She has hypertension, hypercholesterolemia, and hypothyroidism. Her other medications include hydrochlorothiazide, simvastatin, and levothyroxine. She attends a 30-minute power walking class twice a week. She has smoked a pack of cigarettes daily for 40 years. She does not drink alcohol. She does not appear in distress. She is 165 cm (5 ft 5 in) tall and weighs 75 kg (165 lb); her BMI is 27.6 kg/m2. Vital signs are within normal limits. Examination shows midline lumbar tenderness. Muscle strength is full and deep tendon reflexes are 2+. Straight-leg raising is negative but painful. MRI of the spine shows an acute compression fracture of the L3 vertebral body and an old compression fracture of the L4 vertebra. Which of the following parts of this patient's history is the strongest predisposing factor for her condition?
A 51-year-old woman with hyperlipidemia comes to the physician because of weakness for one month. At the end of the day, she feels too fatigued to cook dinner or carry a laundry basket up the stairs. She also complains of double vision after she reads for long periods of time. All of her symptoms improve with rest. Her only medication is pravastatin. Physical examination shows drooping of the upper eyelids. Strength is initially 5/5 in the upper and lower extremities but decreases to 4/5 after a few minutes of sustained resistance. Sensation to light touch is intact and deep tendon reflexes are normal. Which of the following best describes the pathogenesis of this patient's condition?
Practice by Chapter
Liver pathology (hepatitis, cirrhosis)
Practice Questions
Gallbladder and biliary tract disorders
Practice Questions
Pancreatic diseases
Practice Questions
Kidney diseases
Practice Questions
Male reproductive pathology
Practice Questions
Female reproductive pathology
Practice Questions
Breast pathology
Practice Questions
Endocrine pathology
Practice Questions
Bone and joint pathology
Practice Questions
Skeletal muscle diseases
Practice Questions
Peripheral nerve disorders
Practice Questions
Soft tissue tumors
Practice Questions
Head and neck pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
