Systemic Pathology — MCQs

On this page
A 19-year-old male from rural West Virginia presents to his family medicine doctor to discuss why he is having trouble getting his wife pregnant. On exam, he is 6 feet 2 inches with a frail frame and broad hips for a male his size. He is noted to have mild gynecomastia, no facial hair, and small, underdeveloped testes. He claims that although he has a lower libido than most of his friends, he does have unprotected sex with his wife. His past medical history is notable for developmental delay and difficulties in school. What is the most likely chromosomal abnormality in this patient?
A 42-year-old woman comes to the physician because of a 2-month history of progressive muscular weakness. She has had difficulty climbing stairs, getting up from chairs, and brushing her hair. Her vital signs are within normal limits. Muscle strength is 2/5 with flexion of the hips and 3/5 with abduction of the shoulders. She is unable to stand up from her chair without the use of her arms for support. Laboratory studies show elevations in leukocyte count, erythrocyte sedimentation rate, and creatine kinase concentration. Histological evaluation of a biopsy specimen of the deltoid muscle is most likely to show which of the following?
A 20-year-old man presents with a painless neck mass that has gradually increased in size. The mass is anteromedial to the right sternocleidomastoid muscle and has been present for 3 years. The mass increased in size and became more tender following an upper respiratory infection. An ultrasound of the neck identifies a single, round cystic mass with uniform, low echogenicity, and no internal septations. A contrast-enhanced CT scan of the neck shows a homogeneous mass with low attenuation centrally and with smooth rim enhancement. Which of the following is the most likely diagnosis?
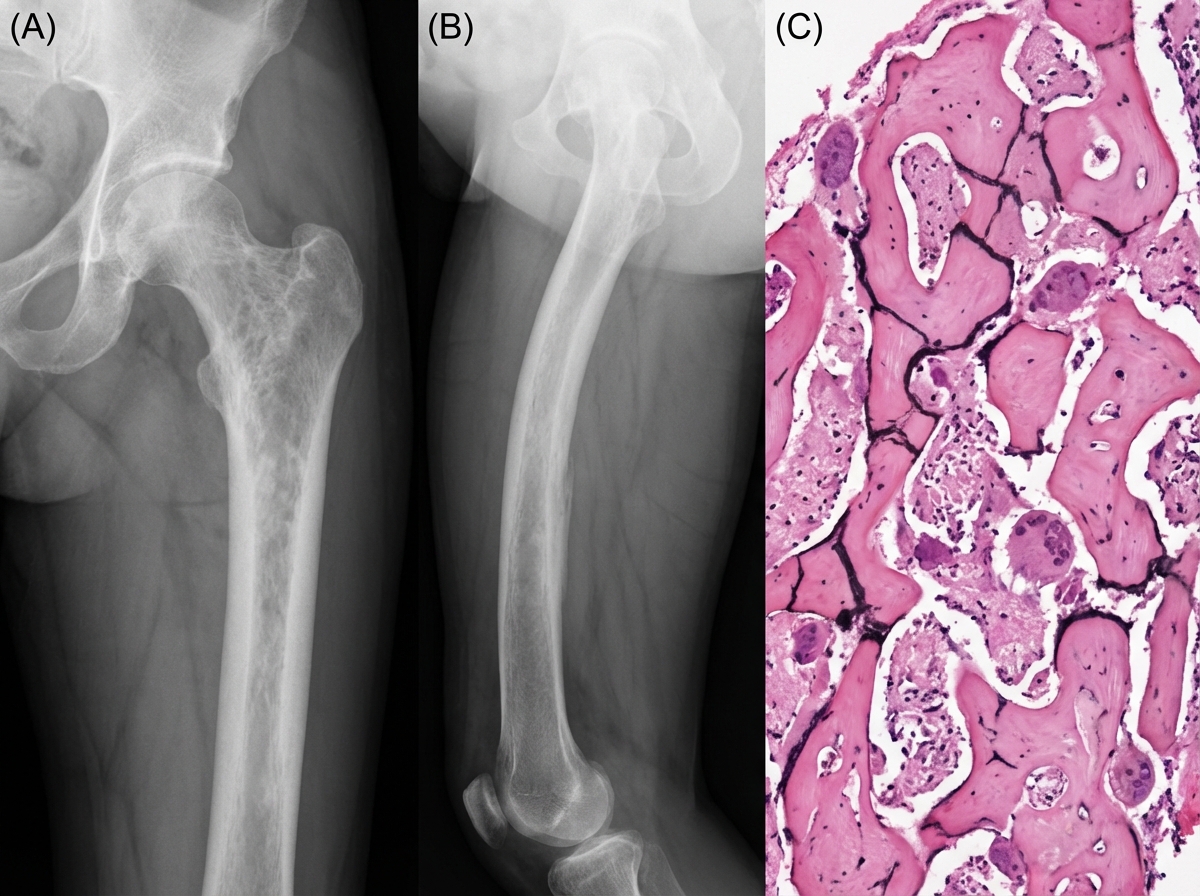
A 55-year-old male presents with left hip pain and stiffness. Radiographs are shown in Figures A and B. Serum alkaline phosphatase levels are elevated. A biopsy of the left femur is performed and shown in Figure C. Which of the following cells are initially responsible for this condition?
Following a recent myocardial infarction, a 60-year-old woman has been started on multiple medications at the time of discharge from the hospital. After 10 days of discharge, she presents to the emergency department with a history of fever, headache, and dark colored urine for 2 days. Her husband mentions that she has not passed urine for the last 24 hours. Her physical examination shows significant pallor, and multiple petechiae are present all over her limbs. Her vital signs include: temperature 38.9°C (102.0°F), pulse rate 94/min, blood pressure 124/82 mm Hg, and respiratory rate 16/min. Her sensorium is altered with the absence of spontaneous speech and spontaneous movements. She responds inappropriately to verbal stimuli. Her laboratory results show the presence of anemia and thrombocytopenia. Examination of peripheral blood smear shows the presence of schistocytes. Serum creatinine is 2 mg/dL. Serum levels of fibrinogen, fibrin monomers, fibrin degradation products and D-dimers are normal. Prothrombin time (PT) and activated partial thromboplastin time (aPTT) are normal. Which is the most likely treatment for this patient’s condition?
A 39-year-old man presents to the emergency department with the complaint of ‘cola-colored’ urine that he noticed this morning. Additionally, he complains of malaise and reports that he has not been able to be productive at work since last week. Lab results revealed a hemoglobin of 6.7 g/dL, leukocyte total count of 1,000 cells/mm3, and a reticulocyte count of 6%. Coomb test is negative and flow cytometry shows CD55/CD59-negative red blood cells. Concerned about the results of his complete blood count, his physician explains the diagnosis to the patient. Which of the following sets of events best describes the mechanism underlying the development of neutropenia?
A 35-year-old man presents with large tense blisters on the flexor surfaces of the upper extremities and trunk. The histologic findings show subepidermal blisters with an eosinophil-rich infiltrate. What is the most likely underlying pathology?
A 29-year-old woman comes to the office with the complaints of severe bleeding after a dental extraction which required local hemostatic therapy. She has a long-term excessive menstrual bleeding and iron-deficiency anemia that required treatment with iron supplement since the age of 17. In addition, she states that her mother also has a history of frequent nosebleeds. The vital signs include: pulse rate 107/min, respiratory rate 17/min, temperature 37.2°C (99.0°F), and blood pressure 90/60 mm Hg. Her physical exam shows generalized pallor. The complete blood count results are as follows: Hemoglobin 10.7 g/dL Hematocrit 41% Leukocyte count 8,000/mm3 Neutrophils 54% Bands 3% Eosinophils 1% Basophils 0% Lymphocytes 32% Monocytes 2% Mean corpuscular hemoglobin 25.4 pg/cell Mean corpuscular hemoglobin concentration 31% Hb/cell Mean corpuscular volume 76 μm3 Platelet count 380,000/mm³ The coagulation test results are as follows: Partial thromboplastin time (activated) 48.0 s Prothrombin time 14.0 s International normalized ratio 0.9 What is the most likely diagnosis?
A 24-year-old woman presents with blisters and erosions on her upper face, chest, and back. The blisters have erythema, scales, and crust formation. Examination shows oromucosal involvement. Histopathologic evaluation reveals a tombstone arrangement at the base of the blister. What is the most likely cause for the patient's condition?
A 32-year-old man comes to the physician because of a 3-week history of cough, weight loss, and night sweats. He migrated from Sri Lanka 6 months ago. He appears emaciated. His temperature is 38.1°C (100.5°F). Physical examination shows enlargement of the right supraclavicular lymph node. Chest and abdominal examination show no abnormalities. An interferon-gamma assay is positive. A biopsy specimen of the cervical lymph node is most likely to show the causal organism in which of the following locations?
Practice by Chapter
Liver pathology (hepatitis, cirrhosis)
Practice Questions
Gallbladder and biliary tract disorders
Practice Questions
Pancreatic diseases
Practice Questions
Kidney diseases
Practice Questions
Male reproductive pathology
Practice Questions
Female reproductive pathology
Practice Questions
Breast pathology
Practice Questions
Endocrine pathology
Practice Questions
Bone and joint pathology
Practice Questions
Skeletal muscle diseases
Practice Questions
Peripheral nerve disorders
Practice Questions
Soft tissue tumors
Practice Questions
Head and neck pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
