Arrhythmias — MCQs

On this page
A 58-year-old man complains of ascending weakness, palpitations, and abdominal pain. He has a history of hypertension, type II diabetes mellitus, diabetic retinopathy, and end-stage renal disease requiring dialysis. He denies any recent infection. Physical examination is notable for decreased motor strength in both his upper and lower extremities, intact cranial nerves, as well as decreased bowel sounds. On further questioning, the patient shares that he has been depressed, as he feels he may not be able to see his grandchildren grow due to his complicated medical course. This caused him to miss two of his dialysis appointments. Which of the following will mostly likely be found on electrocardiography?
A 33-year-old African American woman presents to her primary care physician for a wellness checkup. She states that she has lost 20 pounds over the past 2 months yet has experienced an increased appetite during this period. She endorses hyperhidrosis and increased urinary volume and frequency. Physical exam is notable for an anxious woman and a regular and tachycardic pulse. Laboratory values are ordered as seen below. Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L HCO3-: 25 mEq/L Ca2+: 12.2 mg/dL The patient's urine calcium level is elevated. Which of the following is the most likely diagnosis?
A 45-year-old man presents to the emergency department with complaints of right-sided weakness and slurring of speech for 1 hour. There is no history of head trauma, myocardial infarction, recent surgery, gastrointestinal or urinary bleeding. He has hypertension, chronic atrial fibrillation, and a 20 pack-year cigarette smoking history. The medication list includes valsartan and rivaroxaban. The vital signs include: blood pressure 180/92 mm Hg, pulse 144/min and irregular, and temperature 37.2°C (99.0°F). On physical examination, there is a facial asymmetry with a deviation of angle of mouth to the left side on smiling. Muscle strength is reduced in both upper and lower limbs on the right side while on the left side it’s normal. Random blood glucose is 104 mg/dL. A complete blood count is normal. A CT scan of the head is shown in the image. What is the most appropriate next step in the management of this patient?
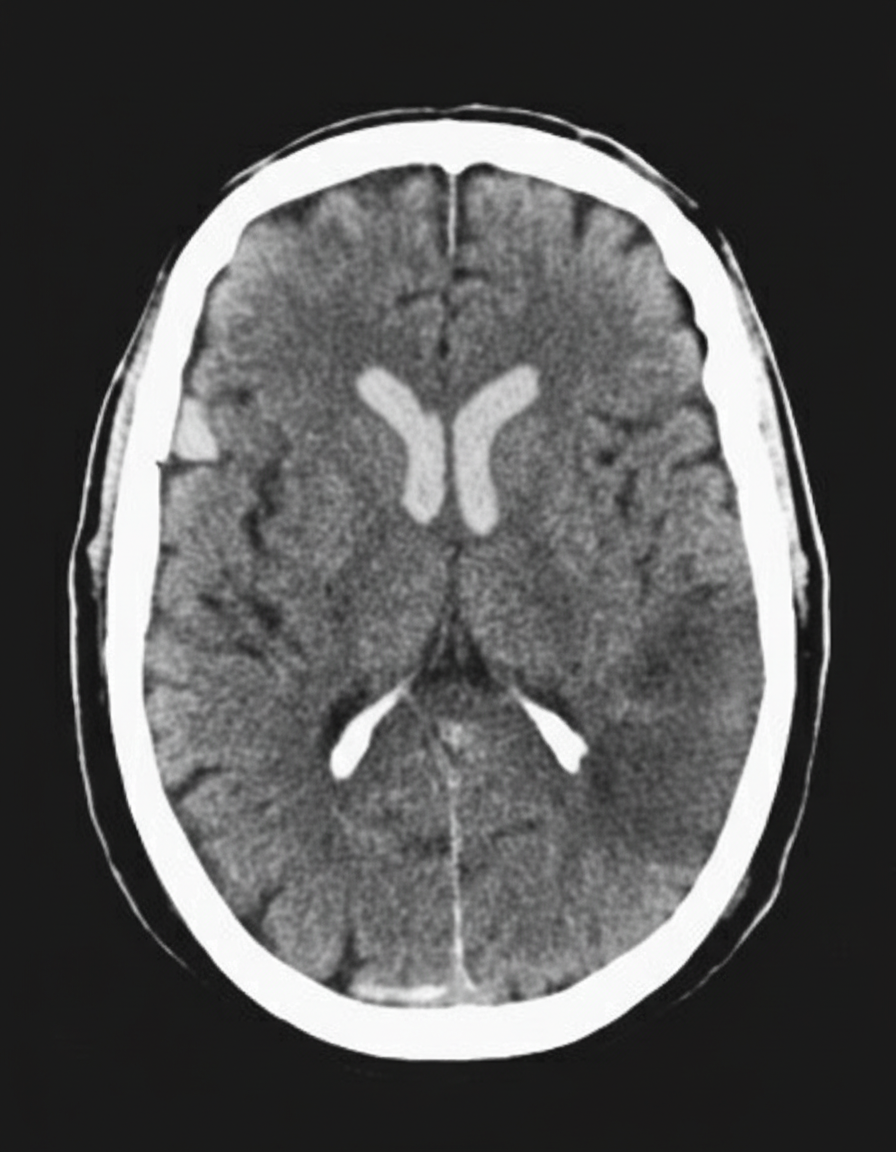
A 65-year-old woman is brought to the emergency department by her husband due to difficulty speaking and confusion for 1 hour. She was gardening when she suddenly developed these symptoms. She is not able to respond to the questions despite multiple repetitions. She also appears unsteady with her gait and is able to walk with support. The past medical history includes type 2 diabetes mellitus, dyslipidemia, and osteoarthritis. The medicine list includes aspirin, atorvastatin, metformin, and chondroitin sulfate. The vital signs include: blood pressure 174/88 mm Hg, heart rate 154/min and irregular, respiratory rate 12/min, and oxygen saturation 96% on room air. She is awake, but not following commands. The pupils are equal bilaterally and reactive to light. There is mild facial droop on the right side. The forehead wrinkles are preserved. When the soles of her feet are stimulated with a blunt instrument, the right-sided big toe goes upward, while the left-sided big toe goes downward. The ECG shows variable R-R intervals and absence of P waves. What is the next step in the management of this patient?
A 75-year-old man presents to the emergency department after an episode of syncope while walking outside with his wife. His wife states that he suddenly appeared pale and collapsed to the ground. She says he remained unconscious for 1 minute. He says he noticed a fluttering in his chest and excessive sweating before the episode. He has type 2 diabetes mellitus, essential hypertension, and chronic stable angina. He has not started any new medications in the past few months. Vital signs reveal: temperature 37.0°C (98.6°F), blood pressure 135/72 mm Hg, and pulse 72/min. Physical examination is unremarkable. ECG shows an old bifascicular block. Echocardiogram and 24-hour Holter monitoring are normal. Which of the following is the best next step in the evaluation of this patient's condition?
A 24-year-old woman presents to the emergency department with palpitations for the last hour. This is her 3rd emergency department visit in the last 8 weeks due to the same complaint. She denies fever, shortness of breath, nasal discharge, bowel changes, weight loss, and heat intolerance. She has asthma that is poorly controlled despite regular inhaler use. She drinks a cup of coffee each morning, and she is physically active and jogs for at least 30 minutes daily. She is in a monogamous relationship with her boyfriend and regularly uses barrier contraceptives. Her last menses was 1 week ago. Physical examination reveals: blood pressure 104/70 mm Hg, pulse 194 /min that is regular, and respiratory rate 18/min. Her ECG is shown in the image. A gentle massage over the carotid artery for 5–10 seconds did not terminate her palpitations. What is the most appropriate next step in the management of this patient?
A 43-year-old woman presents to a physician with weakness and fatigue for a week. She mentions that she has been taking oral fluconazole for the last 4 weeks for the treatment of tinea capitis. She also says that she loves coffee and usually consumes 4–6 cups of coffee every day. On physical examination, her vital signs are stable and examination of all systems, including nervous system, is normal. Her laboratory evaluation reveals that her serum potassium level is 3.1 mmol/L (3.1 mEq/L). The physician orders an ECG. Which of the following findings is most likely to be present?
A 27-year-old man presents to the emergency department with a progressively worsening cough, wheezes, and chest tightness over the last 2 days. He has a history of moderate persistent asthma and his maintenance regimen consists of an inhaled corticosteroid, a long-acting beta-agonist, and albuterol as rescue therapy. He has not improved with his rescue inhaler despite increased use. He reports prior exposure to a person who had symptoms of a respiratory infection. His temperature is 37.4°C (99.3°F), blood pressure is 101/68 mm Hg, heart rate is 99/min, and respiratory rate is 32/min. Physical examination reveals widespread polyphonic wheezes but equal air entry. His oxygen saturation is 92% on room air. The presence of which of the following categorizes this patient’s condition as life-threatening?
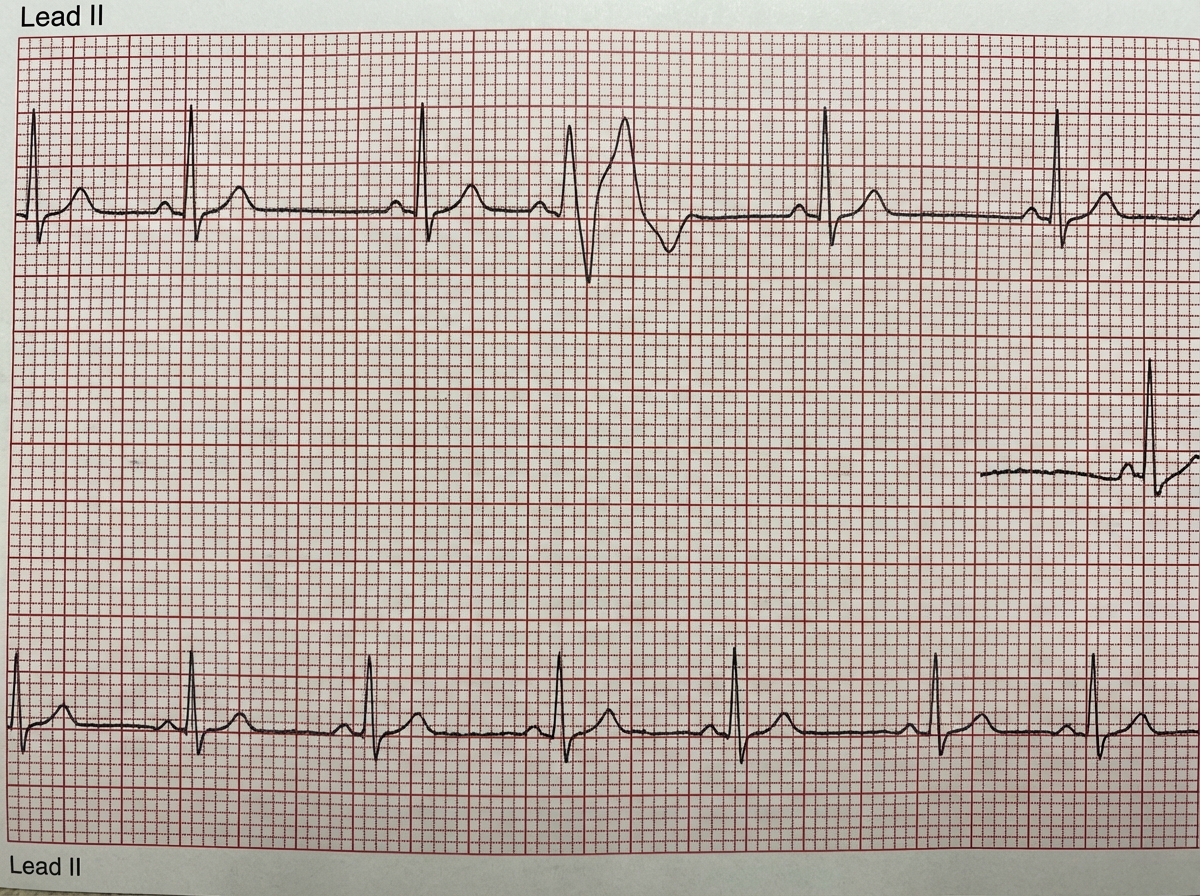
A 26-year-old man comes to the physician because of episodic palpitations for the past 2 months. He has the feeling that sometimes his heart “skips a beat”. His father has a history of atrial fibrillation and myocardial infarction. He has smoked one pack of cigarettes daily for 5 years. He drinks 1–2 beers on the weekends. His vital signs are within normal limits. Physical examination reveals a regular pulse. Cardiopulmonary examination shows no abnormalities. Serum studies, including electrolytes and creatinine, are within normal limits. An excerpt of 24h Holter monitoring is shown. Echocardiography is normal. Which of the following is the most appropriate next step in management?
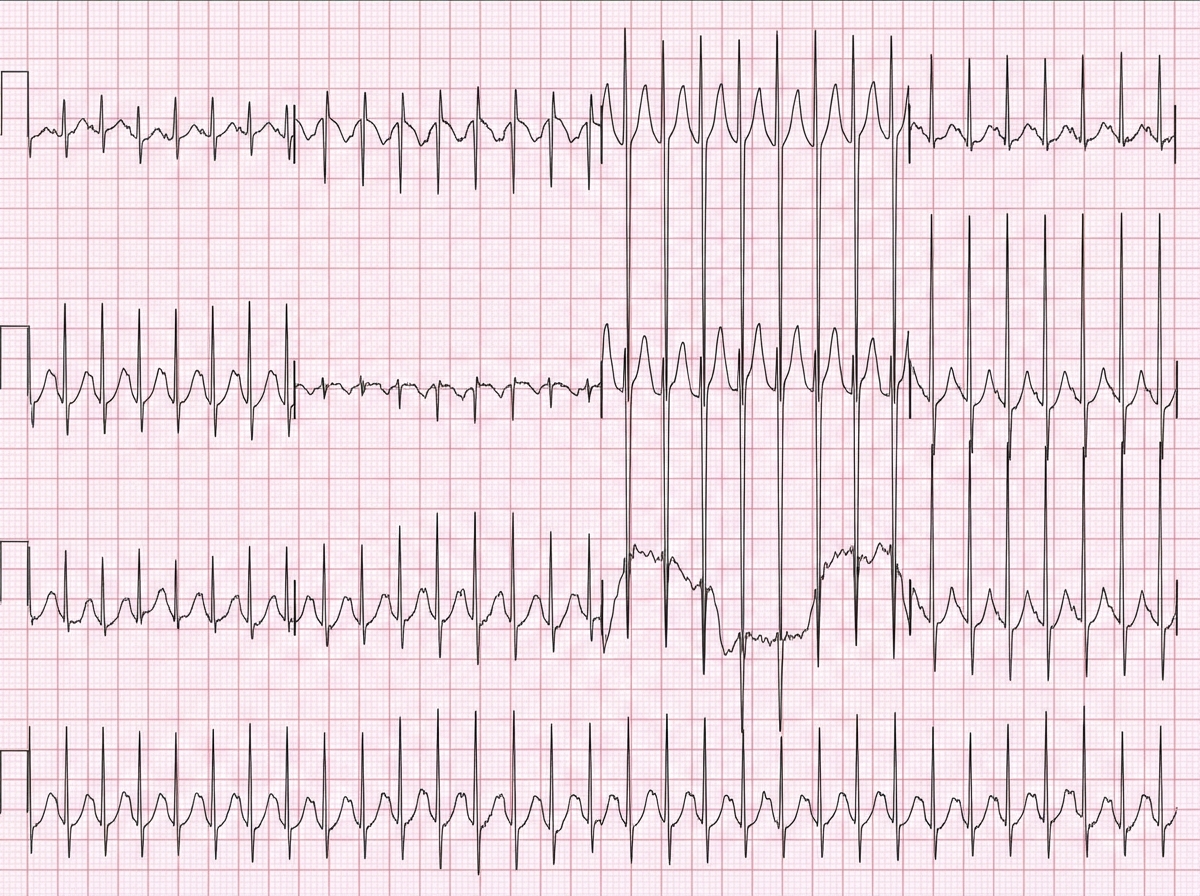
A 23-year-old man comes to the emergency department because of palpitations, dizziness, and substernal chest pain for three hours. The day prior, he was at a friend’s wedding, where he consumed seven glasses of wine. The patient appears diaphoretic. His pulse is 220/min and blood pressure is 120/84 mm Hg. Based on the patient's findings on electrocardiography, the physician diagnoses atrial fibrillation with rapid ventricular response and administers verapamil for rate control. Ten minutes later, the patient is unresponsive and loses consciousness. Despite resuscitative efforts, the patient dies. Histopathologic examination of the heart at autopsy shows an accessory atrioventricular conduction pathway. Electrocardiography prior to the onset of this patient's symptoms would most likely have shown which of the following findings?
Practice by Chapter
Basic electrophysiology
Practice Questions
ECG interpretation fundamentals
Practice Questions
Supraventricular tachycardias
Practice Questions
Atrial fibrillation and flutter
Practice Questions
Ventricular arrhythmias
Practice Questions
Bradyarrhythmias and conduction disorders
Practice Questions
Sudden cardiac death
Practice Questions
Antiarrhythmic medications
Practice Questions
Cardioversion and defibrillation
Practice Questions
Pacemakers and ICDs
Practice Questions
Catheter ablation procedures
Practice Questions
Secondary arrhythmias (electrolyte, drug-induced)
Practice Questions
Inherited arrhythmia syndromes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
