Arrhythmias — MCQs

On this page
A 77-year-old man presents to his primary care physician with lightheadedness and a feeling that he is going to "pass out". He has a history of hypertension that is treated with captopril. In the office, his temperature is 38.3°C (100.9°F), the pulse is 65/min, and the respiratory rate is 19/min. His sitting blood pressure is 133/91 mm Hg. Additionally, his supine blood pressure is 134/92 mm Hg and standing blood pressure is 127/88 mm Hg. These are similar to his baseline blood pressure measured during previous visits. An ECG rhythm strip is obtained in the office. Of the following, what is the likely cause of his presyncope?
A 24-year-old woman comes to the physician for a routine health maintenance examination. She feels well. On questioning, she has had occasional morning dizziness and palpitations during the past year. She is a graduate student. She does not smoke and drinks 1–2 glasses of wine on the weekends. Her vital signs are within normal limits. Physical examination shows an irregular pulse. On auscultation of the chest, S1 and S2 are normal and there are no murmurs. An ECG is shown. Which of the following is the most appropriate next step in management?
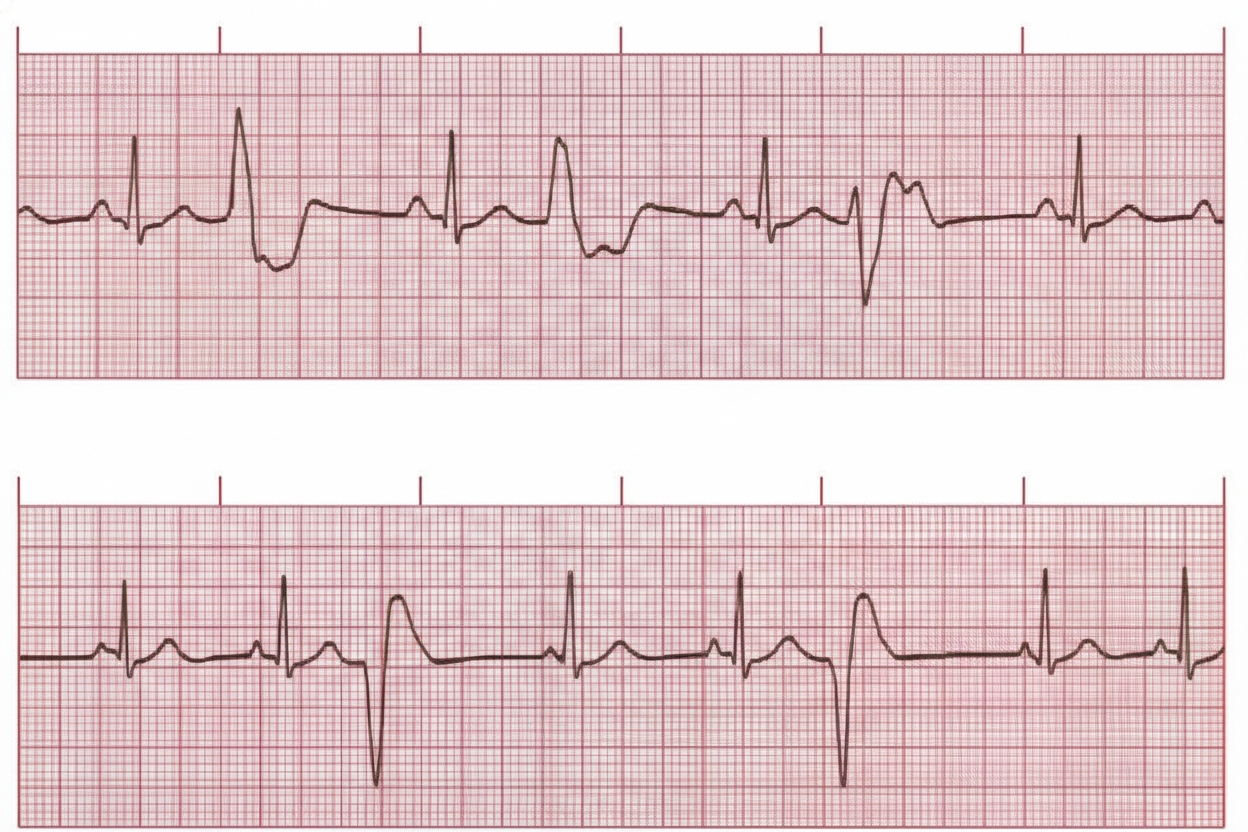
A 62-year-old woman presents to the emergency department complaining of fever, worsening fatigue, and muscle weakness for the previous 48 hours. The patient describes her muscle weakness as symmetric and worse in the upper limbs. Her past medical history is significant for long-standing diabetes type 2 complicated by stage 5 chronic kidney disease (CKD) on hemodialysis. She takes lisinopril, verapamil, metformin, and glargine. Today, the patient’s vital signs include: temperature 38.6°C (101.5°F), pulse 80/min, blood pressure 155/89 mm Hg, respirations 24/min, and 95% oxygen saturation on room air. The cardiac and pulmonary exams are unremarkable. The abdomen is soft and non-tender. Her strength is 3/5 in the upper extremities and 4/5 in the lower extremities and her sensation is intact. Deep tendon reflexes are absent in both the upper and lower limbs. A 12-lead electrocardiogram (ECG) is shown in the image below. Blood work is drawn and the patient is admitted and started on continuous cardiac monitoring. Based on the available information, what is the next best step in managing this patient?
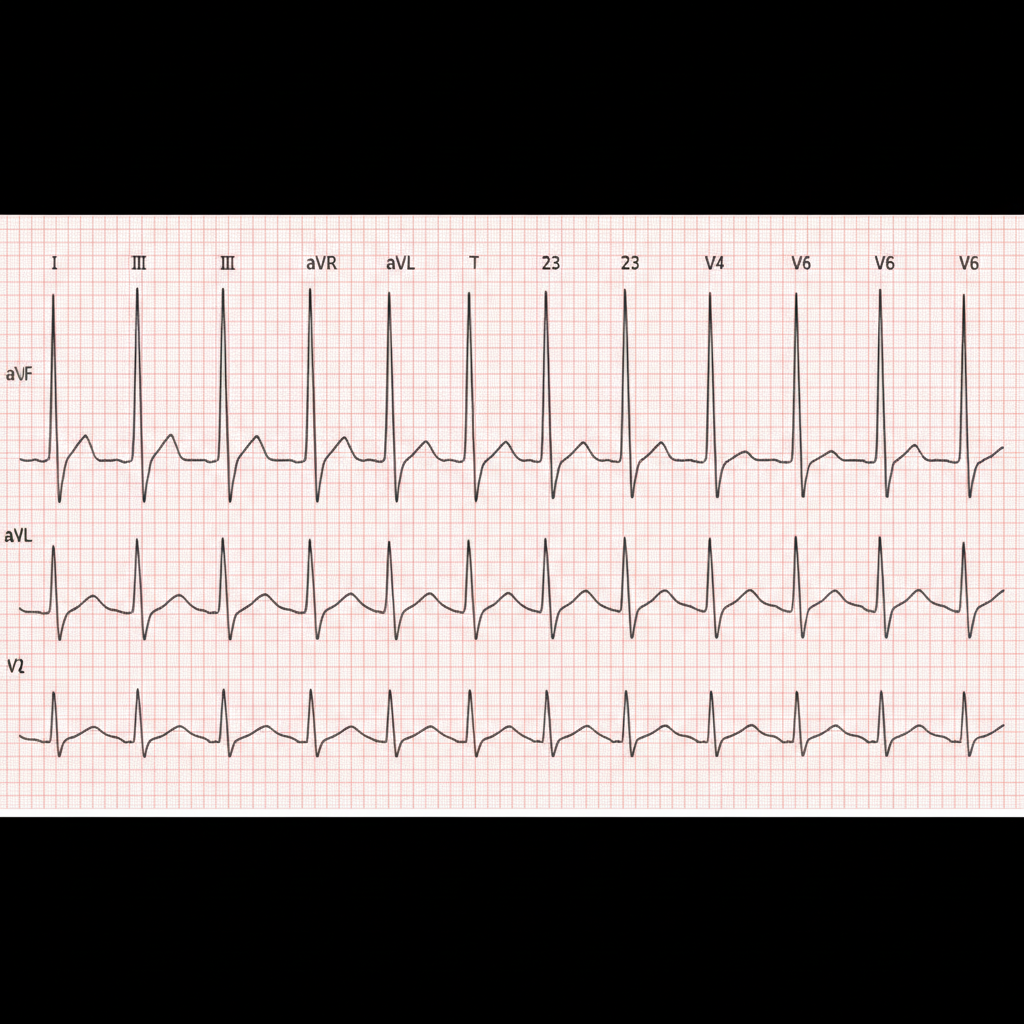
A 64-year-old male presents to the emergency room complaining of chest pain. He reports a pressure-like sensation over his sternum that radiates into his jaw. The pain came on suddenly 2 hours ago and has been constant since then. His past medical history is notable for a stable abdominal aortic aneurysm, hypertension, diabetes, and hyperlipidemia. He takes aspirin, enalapril, spironolactone, atorvastatin, canagliflozin, and metformin. His temperature is 99.1°F (37.3°C), blood pressure is 155/85 mmHg, pulse is 115/min, and respirations are 22/min. On exam, he is diaphoretic and in moderate distress. He is admitted for further management and does well after initial stabilization. He is seen two days later by the admitting team. This patient is at increased risk for a complication that is characterized by which of the following?
A 26-year-old nursing home staff presents to the emergency room with complaints of palpitations and chest pain for the past 2 days. She was working at the nursing home for the last year but has been trying to get into modeling for the last 6 months and trying hard to lose weight. She is a non-smoker and occasionally drinks alcohol on weekends with friends. On examination, she appears well nourished and is in no distress. The blood pressure is 150/84 mm Hg and the pulse is 118/min. An ECG shows absent P waves. All other physical findings are normal. What is the probable diagnosis?
A 29-year-old woman with Wolff-Parkinson-White syndrome presents to her cardiologist’s office for a follow-up visit. She collapsed at her job and made a trip to the emergency department 1 week ago. At that time, she received a diagnosis of atrial fibrillation with rapid ventricular response and hemodynamic instability. While in the emergency department, she underwent direct-current cardioversion to return her heart to sinus rhythm. Her current medications include procainamide. At the cardiologist’s office, her heart rate is 61/min, respiratory rate is 16/min, the temperature is 36.5°C (97.7°F), and blood pressure is 118/60 mm Hg. Her cardiac examination reveals a regular rhythm and a I/VI systolic ejection murmur best heard at the right upper sternal border. An ECG obtained in the clinic is shown. Which of the following is the most appropriate treatment to prevent further episodes of tachyarrhythmia?
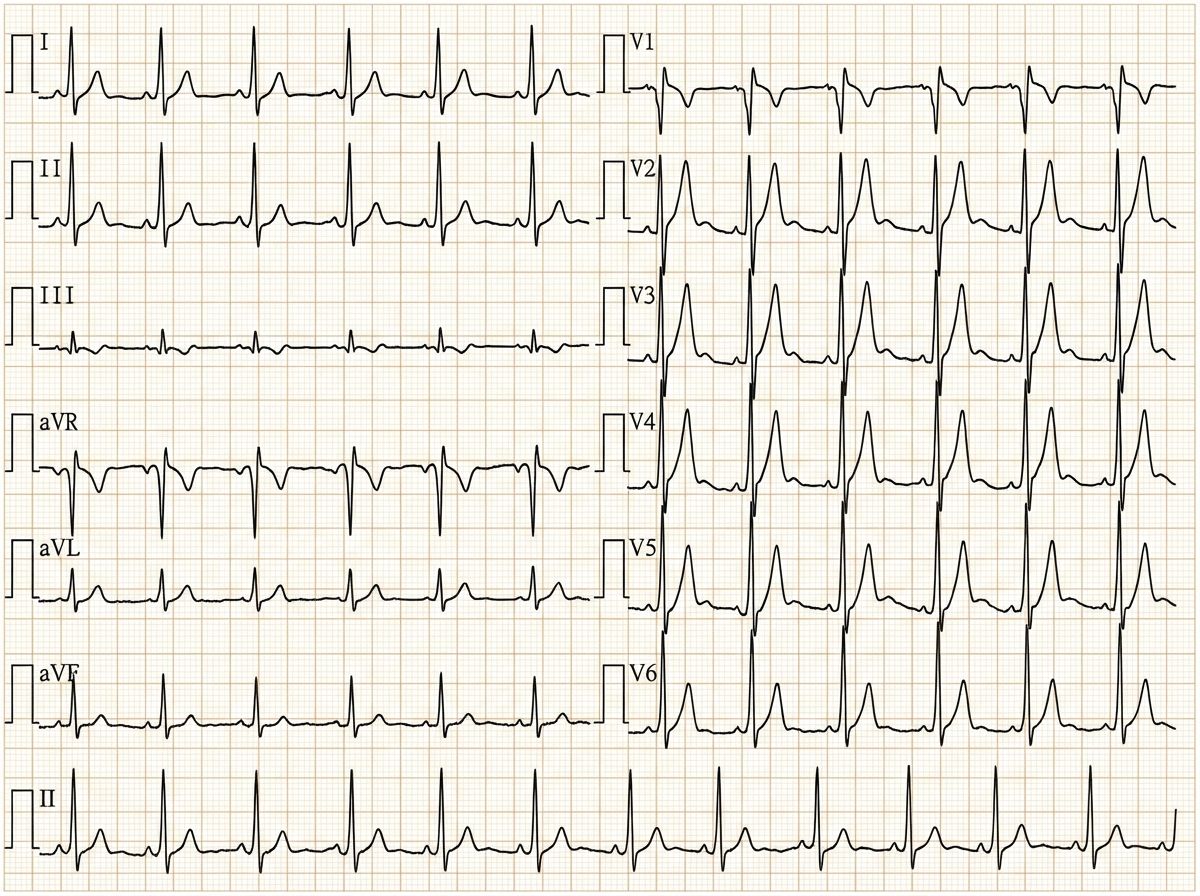
A 73-year-old man noted a rapid onset of severe dizziness and difficulty swallowing while watching TV at home. His wife reports that he had difficulty forming sentences and his gait was unsteady at this time. Symptoms were severe within 1 minute and began to improve spontaneously after 10 minutes. He has had type 2 diabetes mellitus for 25 years and has a 50 pack-year smoking history. On arrival to the emergency department 35 minutes after the initial development of symptoms, his manifestations have largely resolved with the exception of a subtle nystagmus and ataxia. His blood pressure is 132/86 mm Hg, the heart rate is 84/min, and the respiratory rate is 15/min. After 45 minutes, his symptoms are completely resolved, and neurological examination is unremarkable. Which of the following is the most likely cause of this patient’s condition?
A 22-year-old immigrant presents to his primary care physician for a general checkup. This is his first time visiting a physician, and he has no known past medical history. The patient’s caretaker states that the patient has experienced episodes of syncope and what seems to be seizures before but has not received treatment. His temperature is 98.1°F (36.7°C), blood pressure is 121/83 mmHg, pulse is 83/min, respirations are 14/min, and oxygen saturation is 98% on room air. Physical exam is notable for sensorineural deafness. Which of the following ECG changes is most likely to be seen in this patient?
A 68-year-old man presents to the emergency department with palpitations. He also feels that his exercise tolerance has reduced over the previous week. His past history is positive for ischemic heart disease and he has been on multiple medications for a long time. On physical examination, his temperature is 36.9°C (98.4°F), pulse rate is 152/min and is regular, blood pressure is 114/80 mm Hg, and respiratory rate is 18/min. Auscultation of the precordial region confirms tachycardia, but there is no murmur or extra heart sounds. His ECG is obtained, which suggests a diagnosis of atrial flutter. Which of the following findings is most likely to be present on his electrocardiogram?
A 56-year-old man with chronic kidney failure is brought to the emergency department by ambulance after he passed out during dinner. On presentation, he is alert and complains of shortness of breath as well as chest palpitations. An EKG is obtained demonstrating an irregular rhythm with QRS amplitudes that vary in height over time. Other findings include uncontrolled contractions of his muscles. Tapping of his cheek elicits twitching of the facial muscles. Over-repletion of the serum abnormality in this case may lead to which of the following?
Practice by Chapter
Basic electrophysiology
Practice Questions
ECG interpretation fundamentals
Practice Questions
Supraventricular tachycardias
Practice Questions
Atrial fibrillation and flutter
Practice Questions
Ventricular arrhythmias
Practice Questions
Bradyarrhythmias and conduction disorders
Practice Questions
Sudden cardiac death
Practice Questions
Antiarrhythmic medications
Practice Questions
Cardioversion and defibrillation
Practice Questions
Pacemakers and ICDs
Practice Questions
Catheter ablation procedures
Practice Questions
Secondary arrhythmias (electrolyte, drug-induced)
Practice Questions
Inherited arrhythmia syndromes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
