Arrhythmias — MCQs

On this page
A 25-year-old man presents to the emergency department complaining of palpitations, lightheadedness, and sweating. He just started working at an investment firm and has been working long hours to make a good impression. Today, he had a dozen cups of espresso to keep himself awake and working. He has never had such an episode before. His past medical history is unremarkable. His pulse is 150/min, blood pressure is 134/88 mm Hg, respirations are 12/min, and temperature is 36.7°C (98.0°F). ECG shows supraventricular tachycardia. Which of the following is the next best step in the management of this patient?
A 68-year-old man presents to the emergency department because of difficulty breathing and chest tightness for the last 3 days. He also has a productive cough with excessive amounts of green sputum. He has had chronic obstructive pulmonary disease for the past 10 years, but says that the cough and sputum are different compared to his baseline. He took 2 doses of nebulized albuterol and ipratropium at home, but that did not completely relieve his symptoms. He has a 50 pack-year smoking history and drinks alcohol occasionally. His vital signs include a blood pressure of 110/60 mm Hg, a temperature of 37.2 °C (98.9°F), a respiratory rate of 26/min, an irregular radial pulse at a rate of 110–120/min, and an oxygen saturation of 88%. On physical examination, the patient appears drowsy, crackles are heard on chest auscultation bilaterally, and the heart sounds are irregular. A chest X-ray shows hyperinflation of the lungs bilaterally, and the diaphragm is flattened. An ECG is ordered and shown in the accompanying image. Which of the following is the best initial treatment for this patient’s arrhythmia?
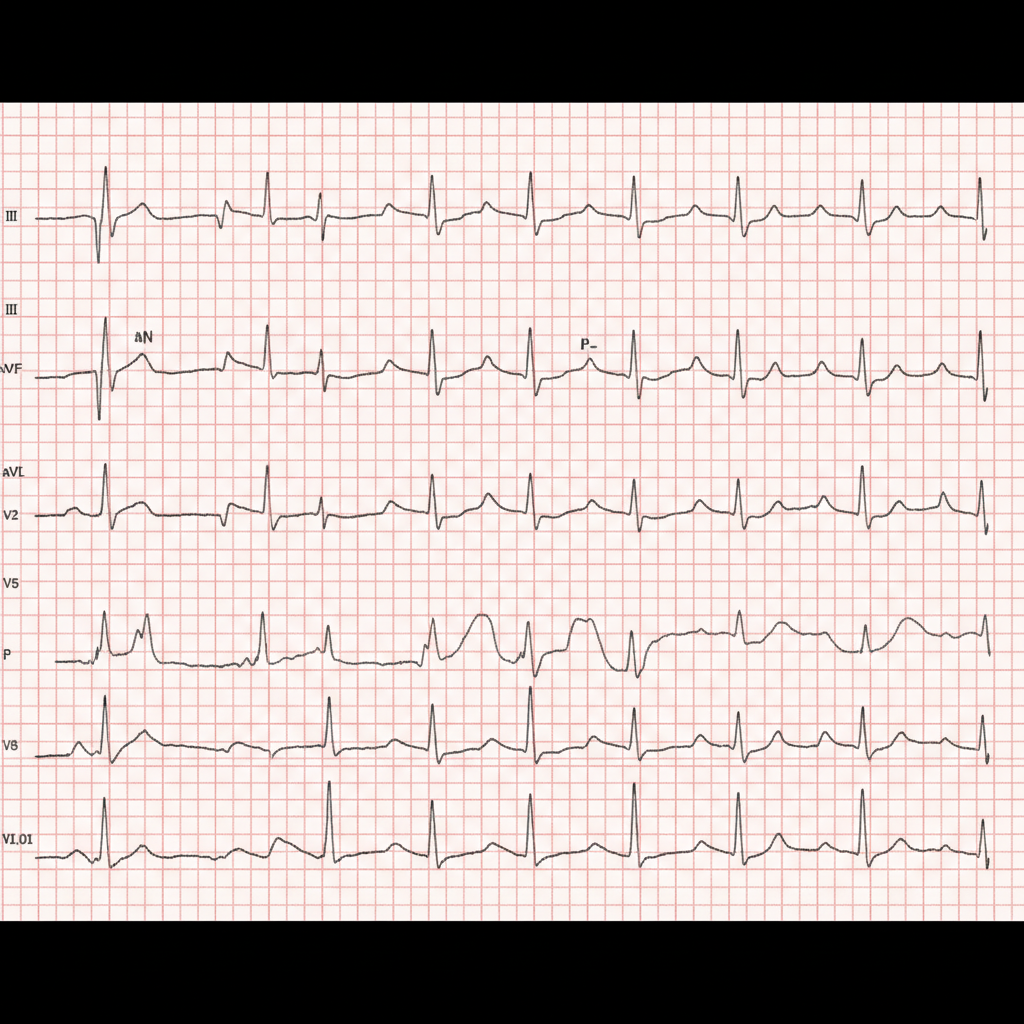
A 40-year-old woman comes to the physician for a 6-month history of recurrent episodes of chest pain, racing pulse, dizziness, and difficulty breathing. The episodes last up to several minutes. She also reports urinary urgency and two episodes of loss of consciousness followed by spontaneous recovery. There is no personal or family history of serious illness. She does not smoke or drink alcohol. Vitals signs are within normal limits. Cardiopulmonary examination shows no abnormalities. Holter monitoring is performed. ECG recordings during episodes of tachycardia show a QRS duration of 100 ms, regular RR-interval, and absent P waves. Which of the following is the most likely underlying cause of this patient's condition?
A 44-year-old man comes to the emergency department because of persistent palpitations for the past 2 hours. The day before, he was at a wedding, where he drank several glasses of wine and 9–10 vodka cocktails. He has never had similar symptoms before. He is a manager at a software company and has recently had a lot of work-related stress. He is otherwise healthy and takes no medications. His temperature is 36.5°C (97.7°F), pulse is 90/min and irregularly irregular, respirations are 13/min, and his blood pressure is 128/60 mm Hg. Physical examination shows no other abnormalities. An ECG is performed; no P-waves can be identified. Echocardiography shows no valvular abnormalities and normal ventricular function. One hour later, a repeat ECG shows normal P waves followed by narrow QRS complexes. He is still experiencing occasional palpitations. Which of the following is the most appropriate next step in management?
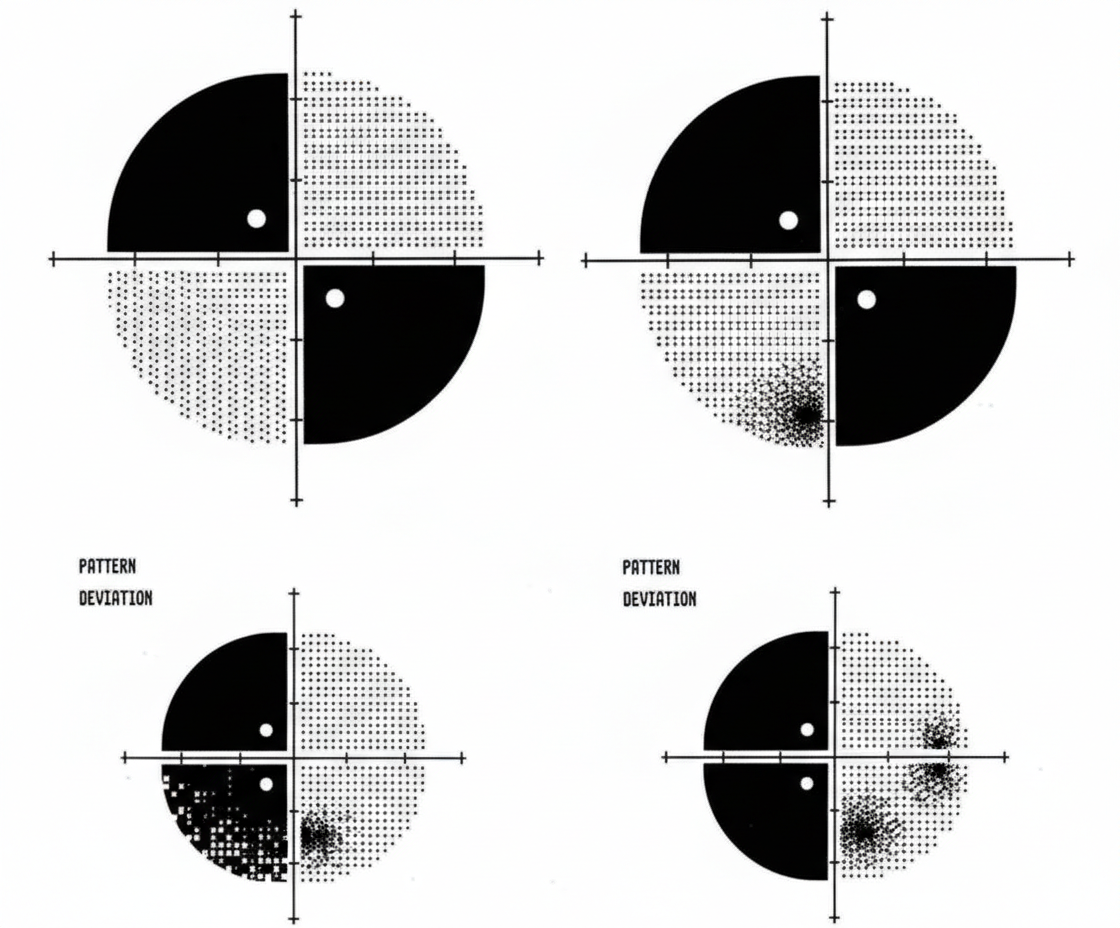
A 62-year-old woman comes to the physician for decreased vision and worsening headaches since this morning. She has hypertension and hypercholesterolemia. Pulse is 119/min and irregular. Current medications include ramipril and atorvastatin. Ocular and funduscopic examination shows no abnormalities. The findings of visual field testing are shown. Which of the following is the most likely cause of this patient's symptoms?
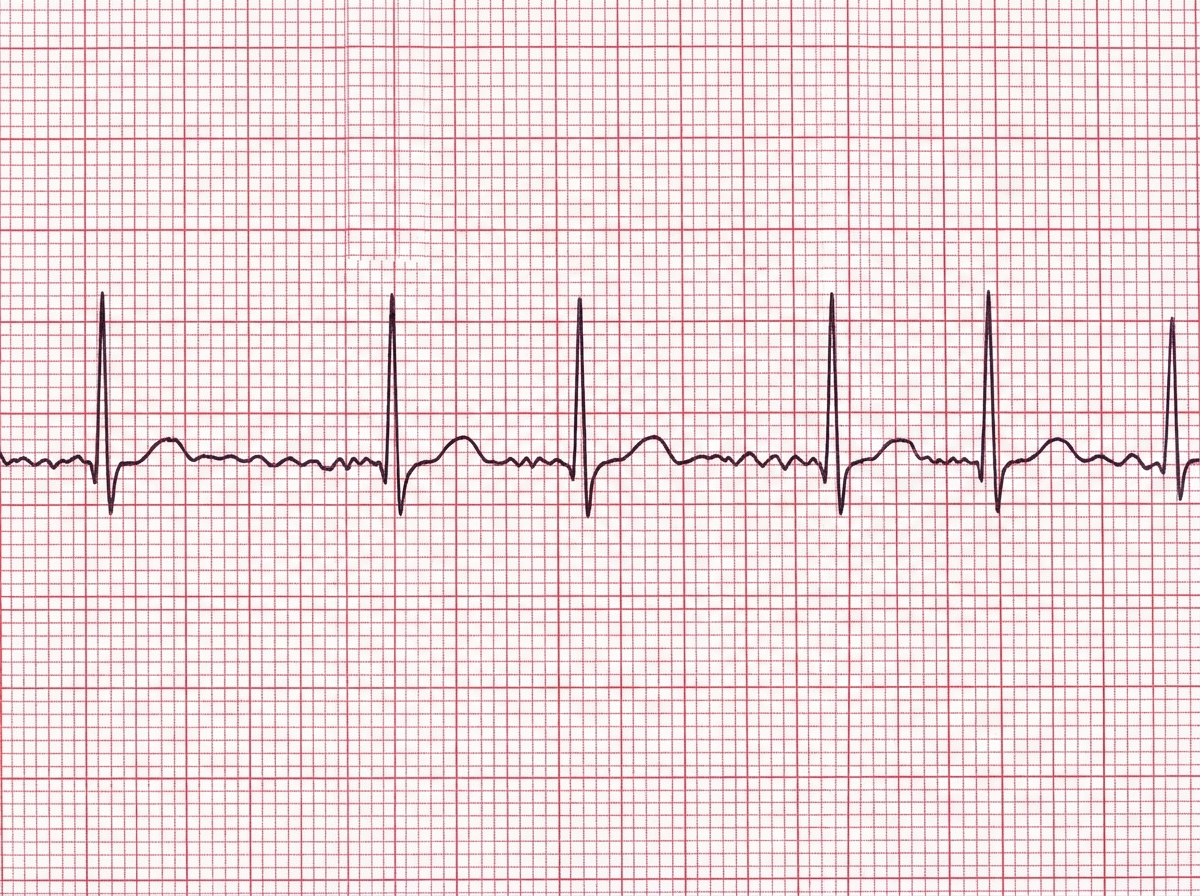
A 54-year-old patient is brought to the emergency department by ambulance with palpitations, lightheadedness, and generalized weakness. He was enjoying the long weekend with his friends at a prolonged destination bachelor’s party over the last several days. They all drank a great deal of alcohol. He can’t quite recall how much he had to drink but he did not blackout. Past medical history includes hypertension. He takes enalapril daily. His blood pressure is 110/75 mm Hg, pulse 140/min, respiratory rate 14/min, temperature 37.0°C (98.6°F). The patient appears ill and has an irregular pulse. An electrocardiogram is performed (see in the picture). The physician explains to the patient that he has an abnormal heartbeat and he needs to be started on anticoagulation therapy to avoid an ischemic stroke from a thrombus that may be forming in his heart. In which of the following locations is a thrombus most likely to be formed?
A 32-year-old woman presents to the emergency department with unilateral vision loss. She states it started suddenly this evening and this has never happened to her before. The patient is not followed by a primary care physician and is not currently taking any medications. She has had a few episodes of weakness or numbness in the past but states her symptoms usually resolve on their own. Her temperature is 97.6°F (36.4°C), blood pressure is 120/74 mmHg, pulse is 88/min, respirations are 12/min, and oxygen saturation is 98% on room air. Physical exam is notable for decreased sensation over the patient's dorsal aspect of her left foot. Visual exam reveals a loss of vision in the patient's left eye and she endorses pain in the eye on exam. Which of the following findings is also likely to be found in this patient?
Two days after admission for myocardial infarction and subsequent coronary angioplasty, a 65-year-old man becomes distressed and diaphoretic in the cardiac intensive care unit. Suddenly he is no longer responsive. Pulse oximetry does not show a tracing. He has a history of hypertension and depression. Prior to his admission, his medication included ramipril and aripiprazole. Examination shows no carotid pulse. An ECG is shown. After beginning chest compressions, which of the following is the most appropriate step in management of the patient?
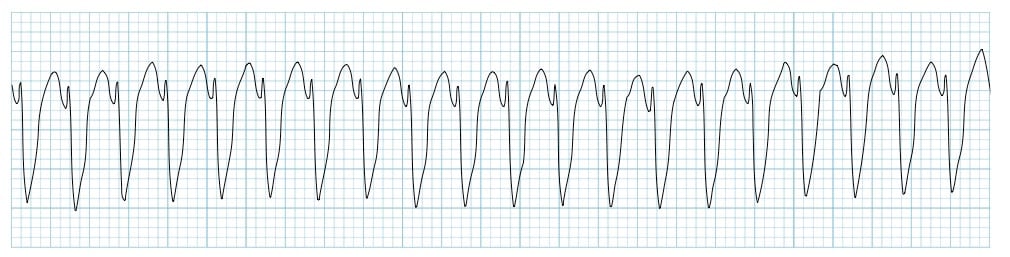
A 15-year-old boy is brought to the emergency department after he passed out in the hallway. On presentation, he is alert but confused about why he is in the hospital. He says that he remembers seeing flashes of light to his right while walking out of class but cannot recall what happened next. His next memory is being woken up by emergency responders who wheeled him into an ambulance. A friend who was with him at the time says that he seemed to be swallowing repeatedly and staring out into space. He has never had an episode like this before, and his past medical history is unremarkable. Which of the following characteristics is most likely true of the cause of this patient's symptoms?
A 28-year-old man presents to the emergency department with lower extremity weakness. He was in his usual state of health until 10 days ago. He then began to notice his legs were “tiring out” during his workouts. This progressed to difficulty climbing the stairs to his apartment. He has asthma and uses albuterol as needed. He has no significant surgical or family history. He smokes marijuana daily but denies use of other recreational drugs. He is sexually active with his boyfriend of 2 years. He has never traveled outside of the country but was camping 3 weeks ago. He reports that he had diarrhea for several days after drinking unfiltered water from a nearby stream. On physical examination, he has 1/5 strength in his bilateral lower extremities. He uses his arms to get up from the chair. Achilles and patellar reflexes are absent. A lumbar puncture is performed, and results are as shown below: Cerebral spinal fluid: Color: Clear Pressure: 15 cm H2O Red blood cell count: 0 cells/µL Leukocyte count: 3 cells/ µL with lymphocytic predominance Glucose: 60 mg/dL Protein: 75 mg/dL A culture of the cerebral spinal fluid is pending. Which of the following is the part of the management for the patient’s most likely diagnosis?
Practice by Chapter
Basic electrophysiology
Practice Questions
ECG interpretation fundamentals
Practice Questions
Supraventricular tachycardias
Practice Questions
Atrial fibrillation and flutter
Practice Questions
Ventricular arrhythmias
Practice Questions
Bradyarrhythmias and conduction disorders
Practice Questions
Sudden cardiac death
Practice Questions
Antiarrhythmic medications
Practice Questions
Cardioversion and defibrillation
Practice Questions
Pacemakers and ICDs
Practice Questions
Catheter ablation procedures
Practice Questions
Secondary arrhythmias (electrolyte, drug-induced)
Practice Questions
Inherited arrhythmia syndromes
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
