Abdominal and Pelvic Radiology — MCQs

On this page
Which is the best imaging modality for pheochromocytoma?
Which imaging modality is best for detecting focal liver lesions?
What condition is characterized by a "bird beak" appearance?
Which is not a usual feature of Ulcerative colitis on barium enema?
All of the following are signs of Hydatid Cyst except?
What is the characteristic appearance of a "Ca-wheel" on ultrasound?
A 43-year-old woman presents with right upper quadrant abdominal pain and vomiting. She has had three children. The white blood cell count is 14.3x10^9/L and liver function tests are normal. What is the test of choice to establish the diagnosis in this patient?
Cobra head deformity in the lower end of ureter is seen in which of the following conditions?
Radio-lucent renal stones are typically composed of which substance?
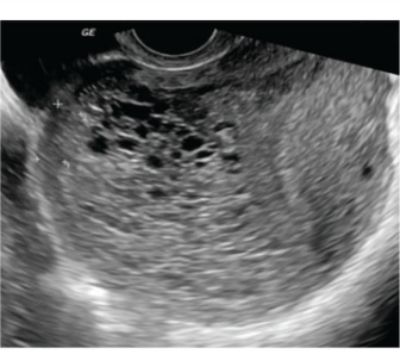
What is the diagnosis based on the ultrasound findings of an early pregnancy?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
