Abdominal and Pelvic Radiology — MCQs

On this page
Gas in the biliary tree on plain abdominal X-ray is suggestive of which of the following conditions?
Rigler's triad consists of which of the following, except?
Semen analysis of a young man presenting with primary infertility revealed low volume, fructose-negative ejaculate with azoospermia. Which of the following is the most useful imaging modality to evaluate the cause of his infertility?
Which radiological finding of urinary bladder calcification resembles a fetal head in the pelvis?
Which of the following is a specific diagnostic criterion for Budd-Chiari syndrome?
Which imaging modality is BEST used to detect distant metastasis in pancreatic cancer?
Diffuse esophageal dilatation on barium swallow is seen in which of the following conditions?
Early arterial phase enhancement on CECT scan of the liver indicates which of the following?
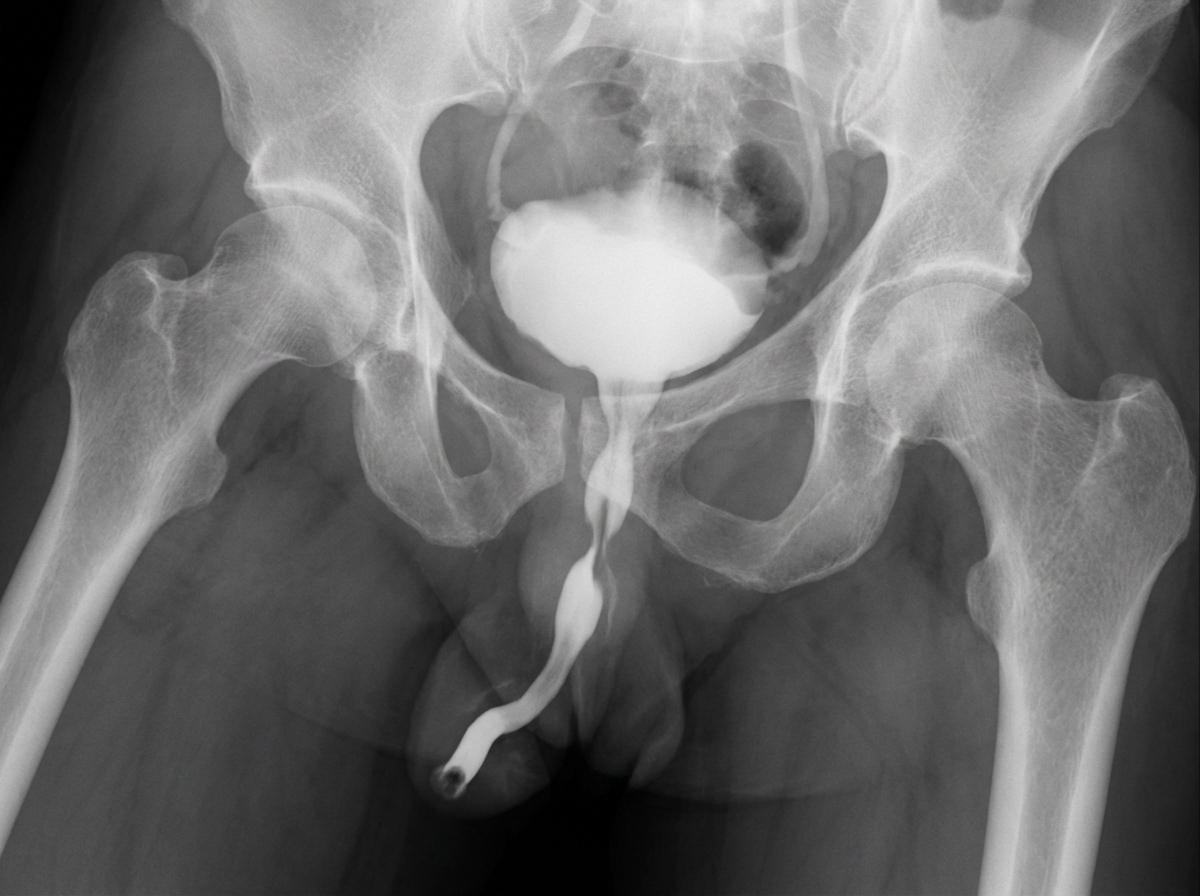
What is the location of the stricture in the given RGU?
What is the best diagnostic investigation for acute appendicitis in children?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
