Abdominal and Pelvic Radiology — MCQs

On this page
What is this appearance, seen in early pregnancy, known as?
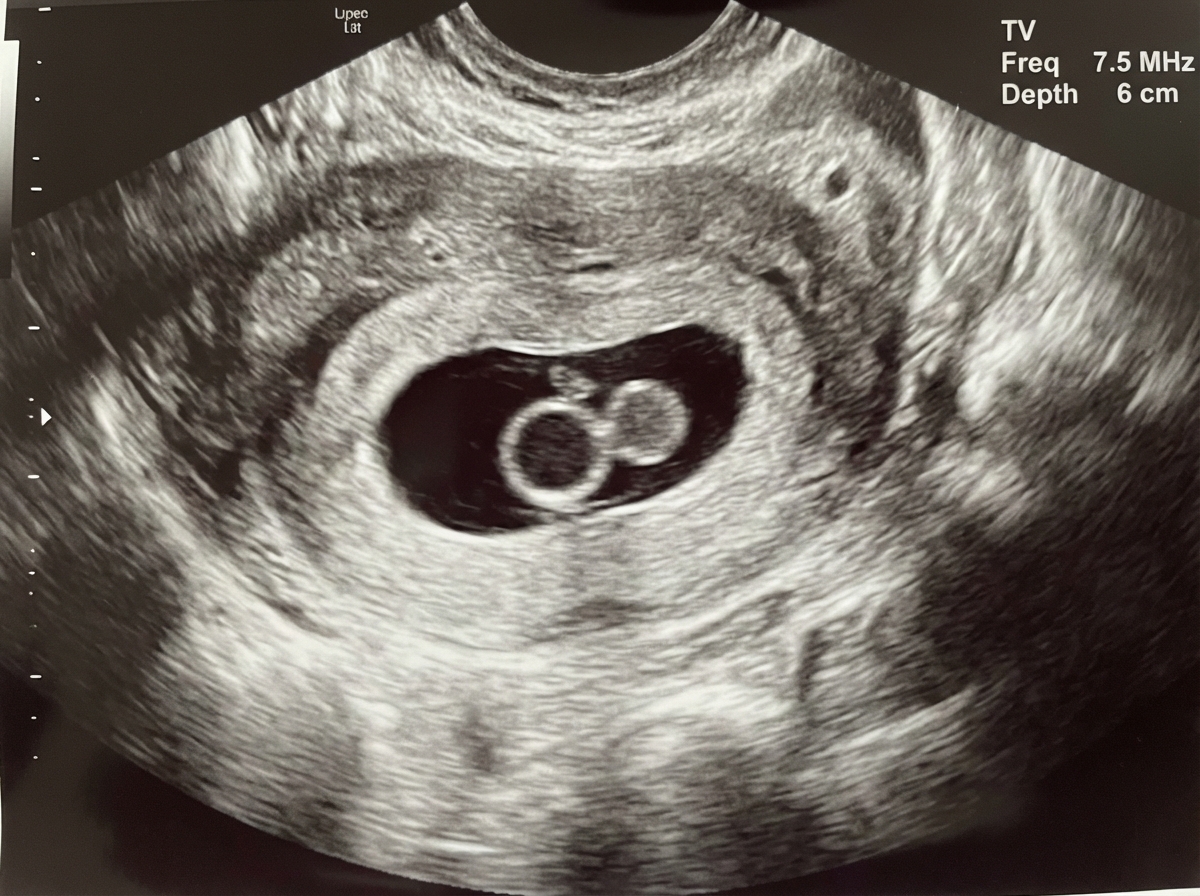
The Carman meniscus sign in a barium meal is pathognomic of which of the following conditions?
What is the initial investigation for suspected gallbladder stones?
Which investigation is most sensitive for detecting minimal intraperitoneal free air?
Which pattern is seen in the jejunum on an X-ray?
A 30-year-old female presents with right hypochondrial pain. CT scan reveals floating membranes in the liver. What is the most likely diagnosis?
Radiographic findings of cardiac achalasia include all except?
What is the best investigation to diagnose Meckel's diverticulum?
A 30-year-old patient presents with acute abdominal pain and obstipation. An X-ray is provided. What is the most likely diagnosis?
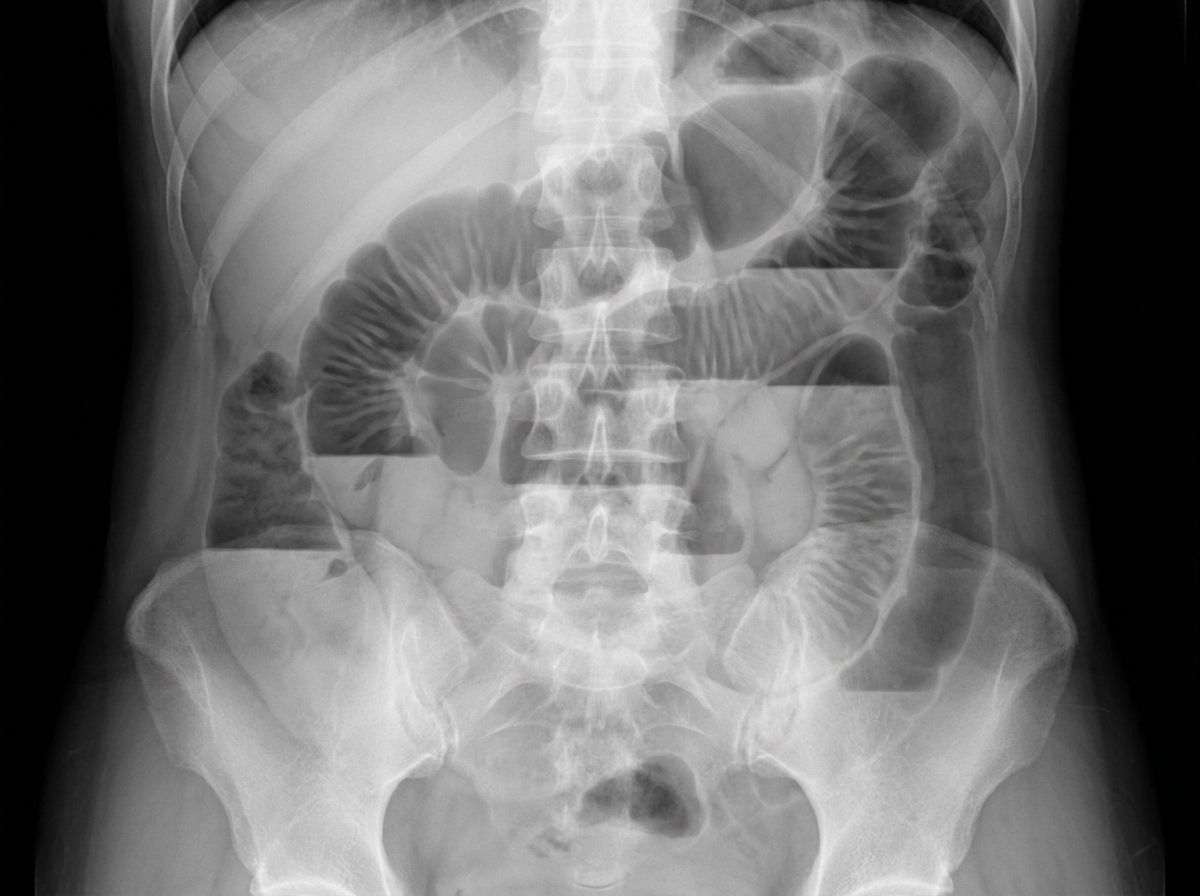
Which of the following investigations is NOT used for the diagnosis of protein-losing enteropathy?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
