Abdominal and Pelvic Radiology — MCQs

On this page
What is the most common cause of widening of the C-loop of the duodenum?
What is the minimum size of a liver metastasis that can be detected by contrast-enhanced computed tomography (CECT)?
What is the investigation of choice for small bowel tumors?
Which of the following imaging modalities can be used to detect carcinoma of the prostate gland?
Comment on the diagnosis shown below?
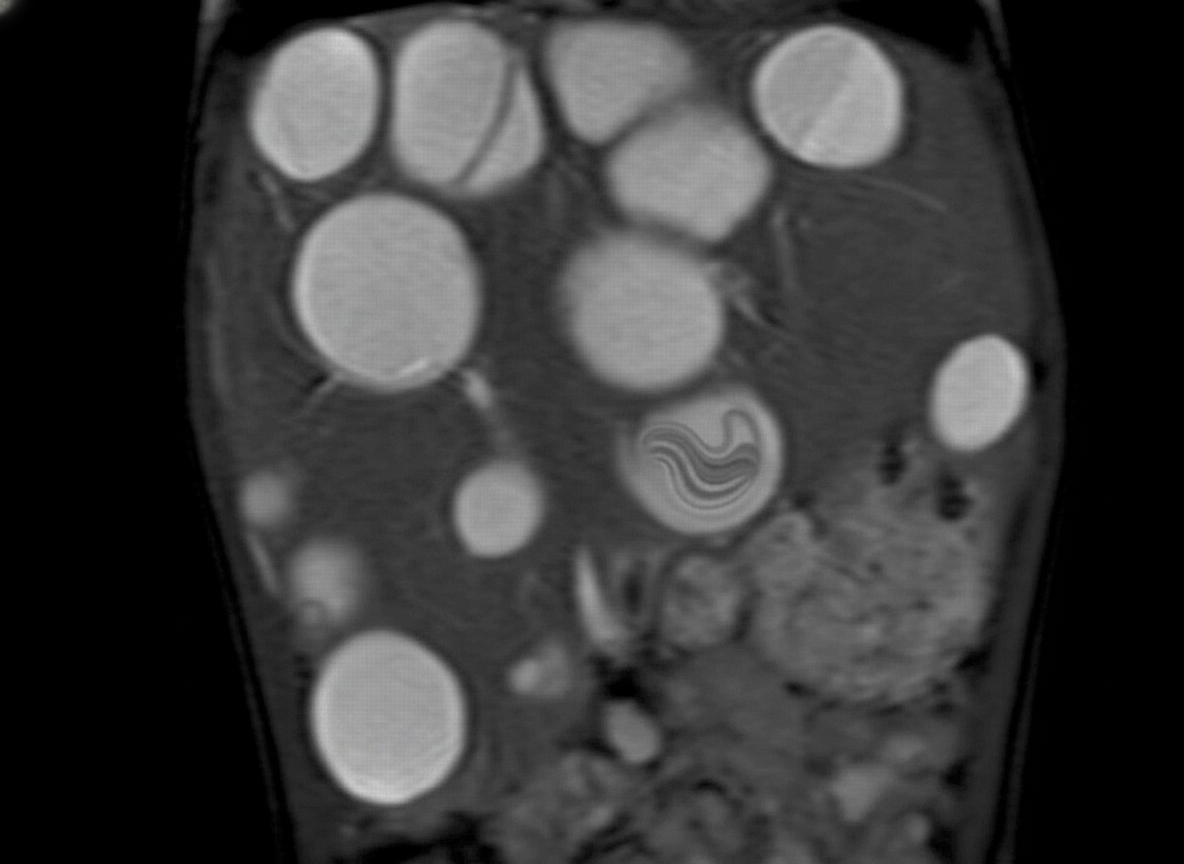
Which sonographic parameter is used to estimate intrauterine growth restriction?
What is the diagnosis suggested by the barium X-ray findings?
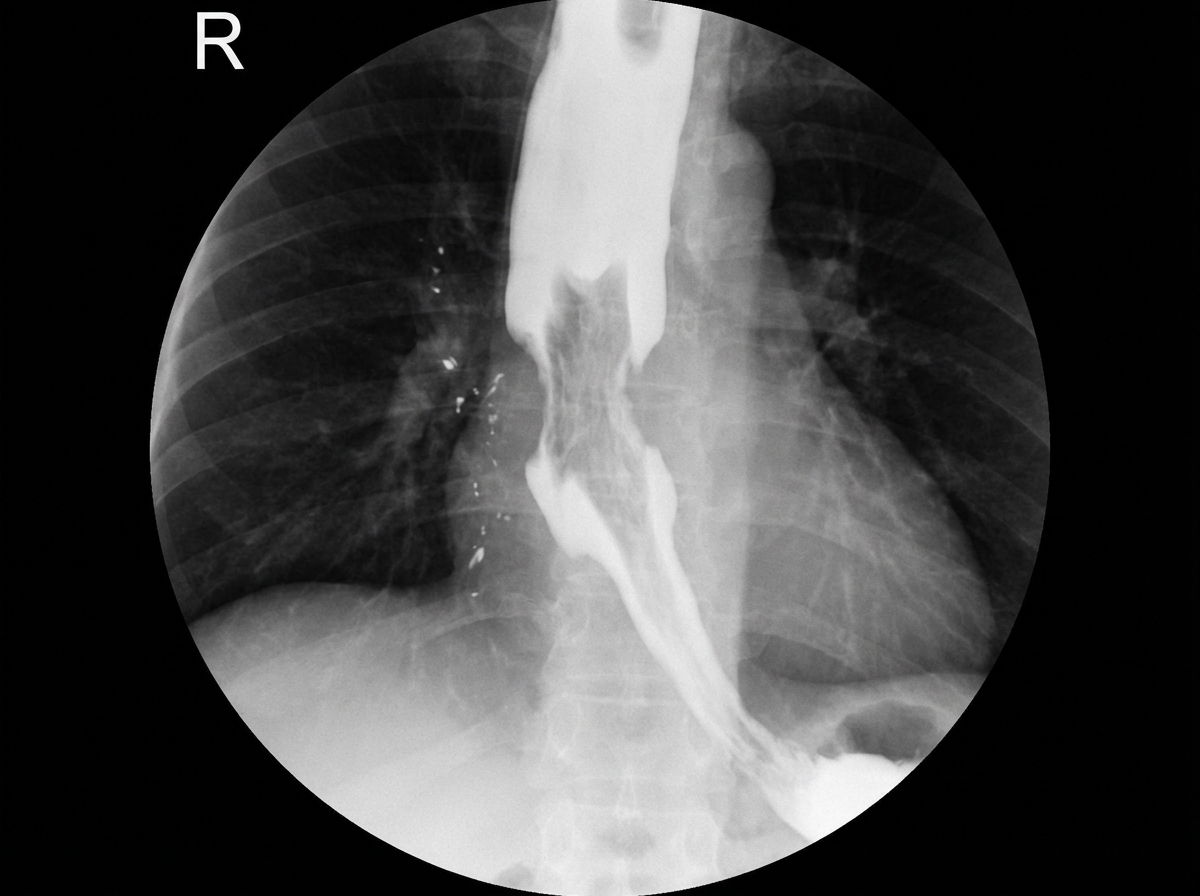
What is the first radiologic sign of Crohn's disease in the terminal ileum?
A 61-year-old man undergoes a CT scan study of the abdomen for unexplained abdominal distension. Low attenuation intraperitoneal collections with enhancing septae are demonstrated. There is scalloping of the liver border and omental thickening. Which one of the following is most likely to be the underlying cause?
Which of the following is true about OCG?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
