Abdominal and Pelvic Radiology — MCQs

On this page
The 'spider leg' sign on an intravenous pyelogram (IVP) suggests which of the following conditions?
What is the characteristic "adder head" appearance seen on an IVP?
What is the ideal imaging modality for diagnosing renal artery hypertension?
Fleischner sign on barium study is seen in which of the following conditions?
Cobra head sign on IVP is classically seen with which of the following conditions?
A solitary hypoechoic lesion of the liver without septa or debris is most likely to be:
Non-visualization of the kidney is seen in all EXCEPT?
Which of the following embryonic structures is the earliest ultrasonographically visible indicator of pregnancy?
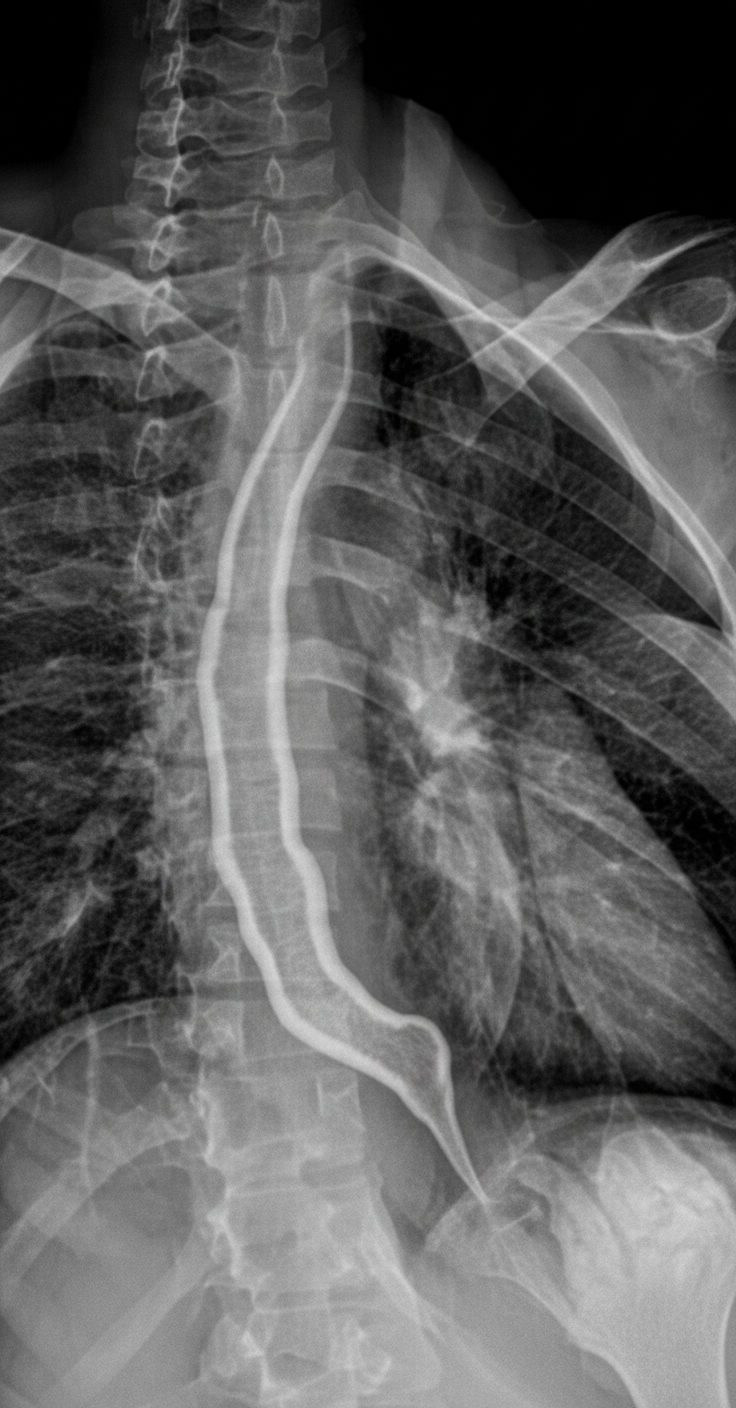
What is the diagnosis demonstrated in the barium esophagogram?
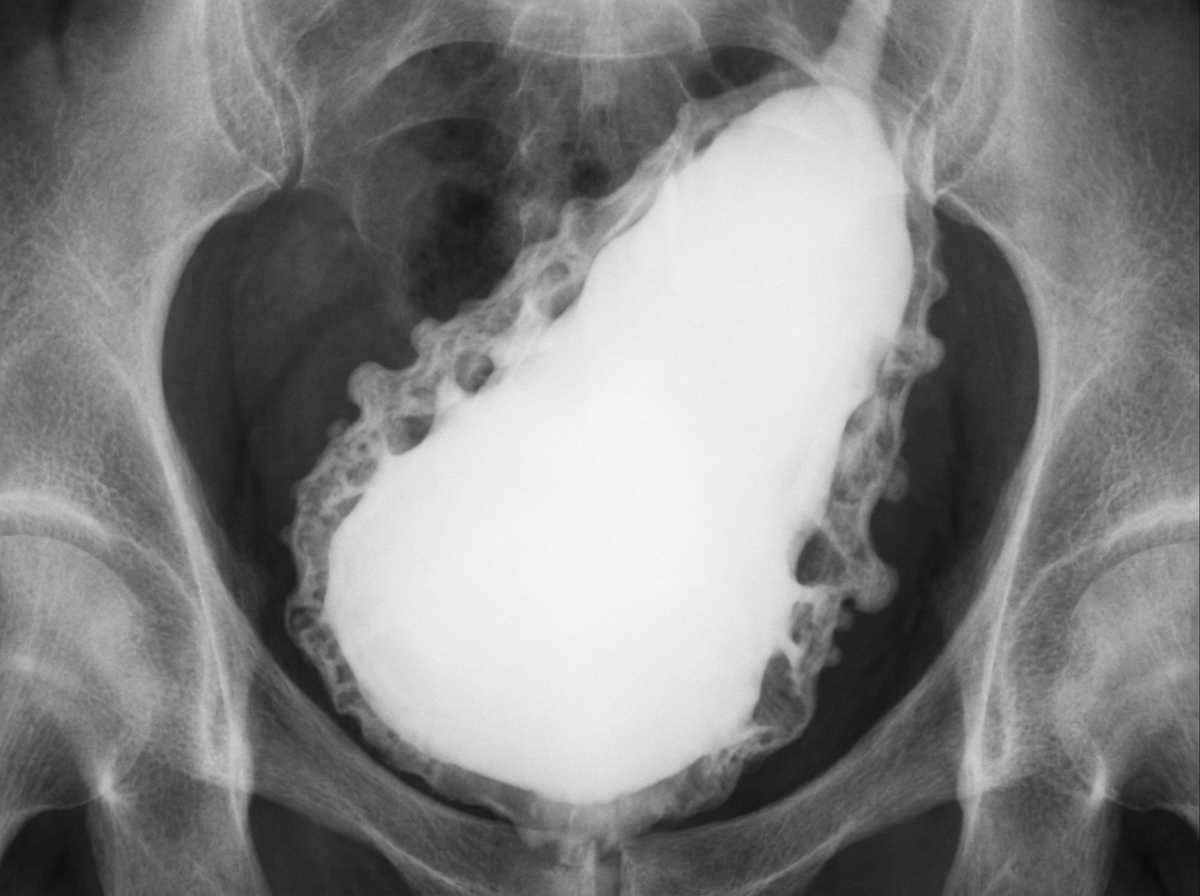
A given cystogram appearance is a characteristic feature of which of the following conditions?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
