Abdominal and Pelvic Radiology — MCQs

On this page
Following is an upper GI contrast study. What is the probable diagnosis?
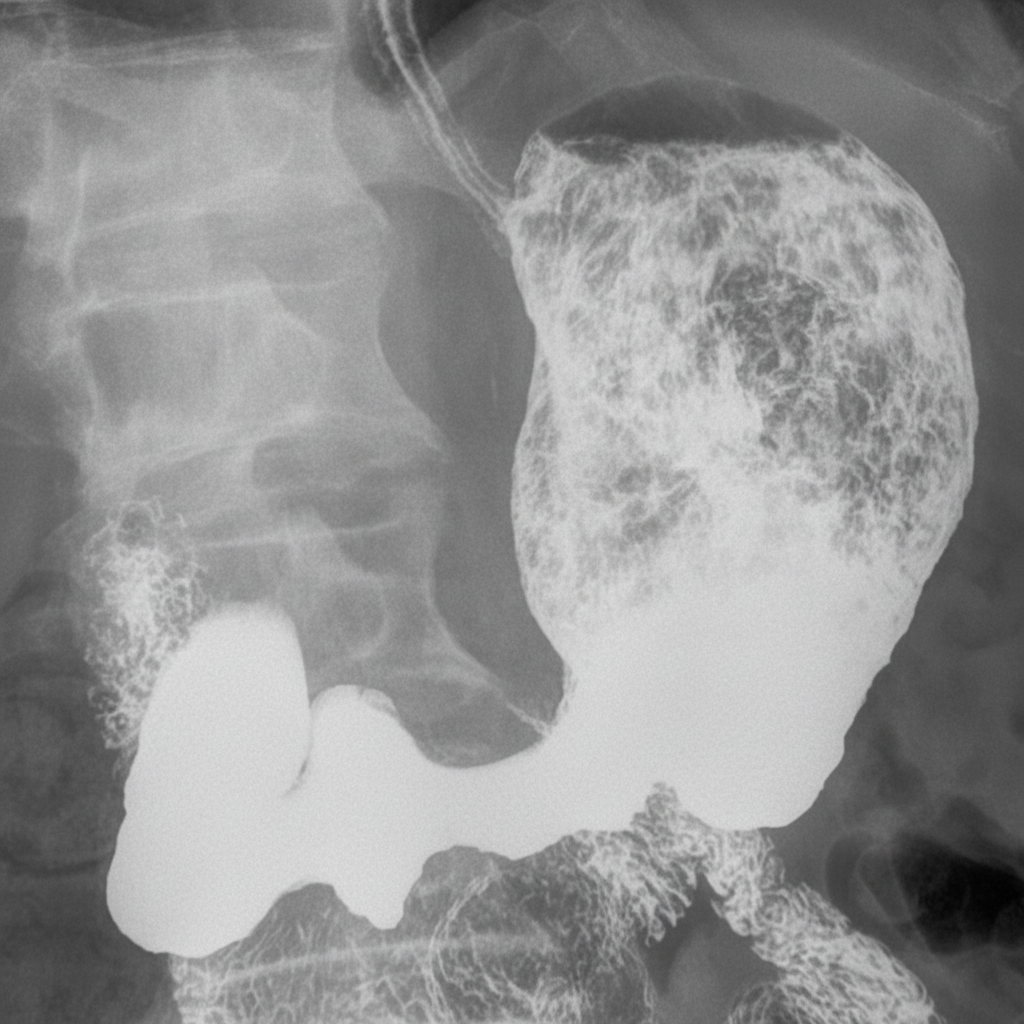
In a patient suspected to be suffering from vesicoureteric reflux, which one of the following radiological investigations may confirm the diagnosis?
The investigation of choice for imaging of urinary tract tuberculosis is:
Which type of renal stone is radiolucent?
Which radiological sign is characteristic of Crohn's disease?
A patient presents with mild abdominal pain and fluctuating bowel habits. The barium enema image is shown below. What is your diagnosis?
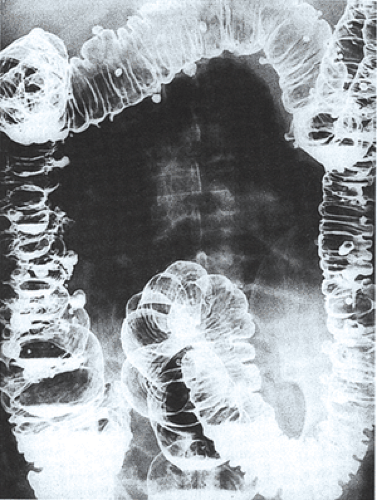
Colonic disease can be diagnosed by all of the following methods except?
String of Kantor is seen in which of the following conditions?
What condition is associated with a soap bubble appearance on abdominal radiography?
What is the characteristic 'crumbled egg appearance' in the liver associated with?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
