Abdominal and Pelvic Radiology — MCQs

On this page
Characteristic fallopian tube findings on sonography in pelvic inflammatory disease includes all except?
Which of the following is an investigation for small intestine abnormalities, excluding one option?
A 54-year-old man presents with a 2-day history of mild abdominal pain, bloating, nausea, vomiting, and poor appetite. His past medical history is significant for recent pneumonia. Radiographic examination reveals a paralytic ileus. Which of the following signs would most likely be found during a physical examination?
An 85-year-old woman has a 48-hour history of generalized abdominal pain and vomiting. On examination, she is dehydrated with multiple dilated small bowel loops measuring up to 4 cm in diameter. A linear gas-filled structure is present in the right upper quadrant with short branches extending from it. What is the most likely diagnosis?
The Mercedes Benz sign or Seagull sign is typically seen in which of the following conditions?
Intra-abdominal calcification in a plain X-ray of the abdomen is most often seen in which of the following conditions?
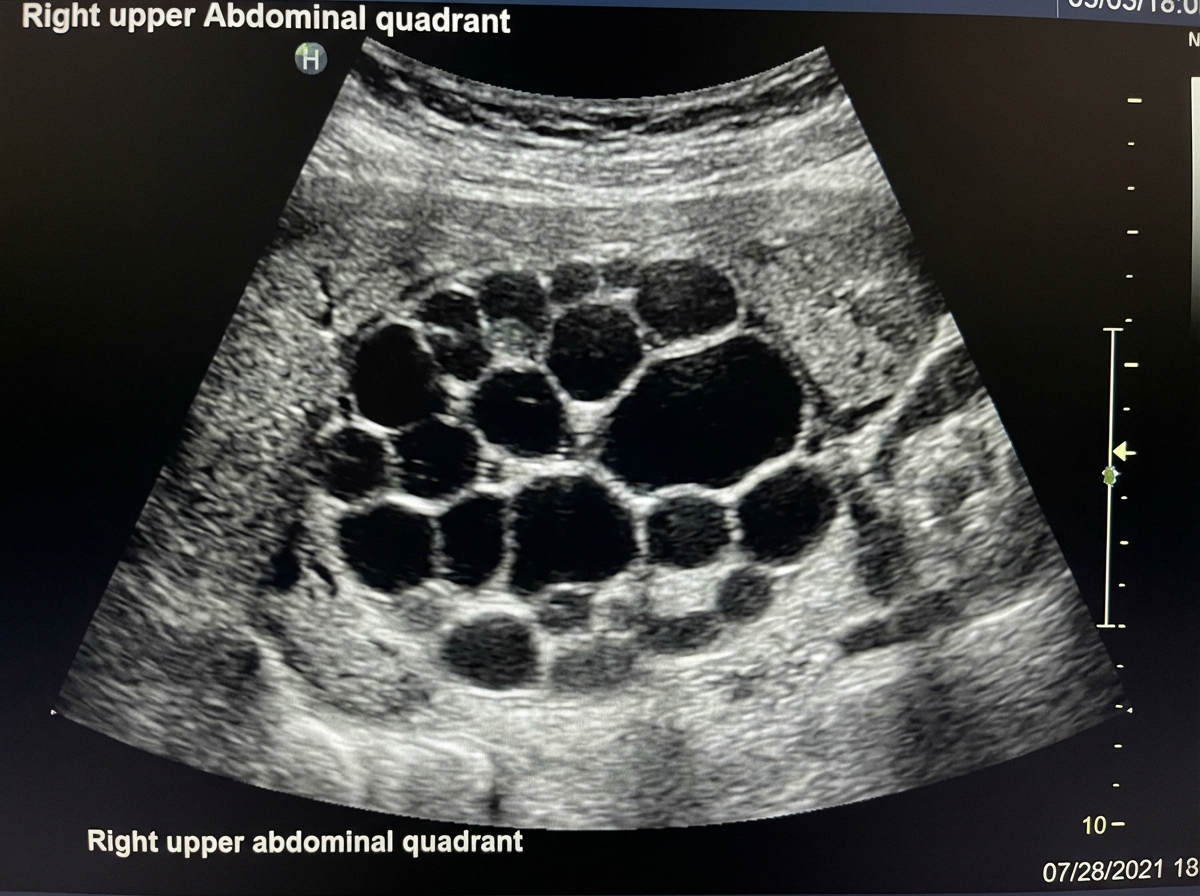
What is the type of Gharbi classification of the given hydatid cyst?
"Double bubble" sign is a feature of which of the following conditions?
Which area of the colon is least visualized by barium studies?
Which of the following gallbladder pathologies can be diagnosed on a simple abdominal X-ray and may warrant consideration for cholecystectomy based on the radiographic findings alone?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
