Abdominal and Pelvic Radiology — MCQs

On this page
What is the most common organ involved in retroperitoneal fibrosis?
What is the imaging of choice (IOC) for ureteric stone with acute colic?
The 'bird of prey' sign is seen in the radiographic barium examination of which condition?
Gas in the great vessels of a fetus indicates which of the following?
A 50-year-old male, a known case of ulcerative colitis, presents with acute onset abdominal distention and vomiting. What would be the next investigation?
What is the best investigation to detect pneumoperitoneum?
Which condition is characterized by the 'thumb printing' sign on imaging?
Which of the following radiographic signs is NOT typically seen in pneumoperitoneum?
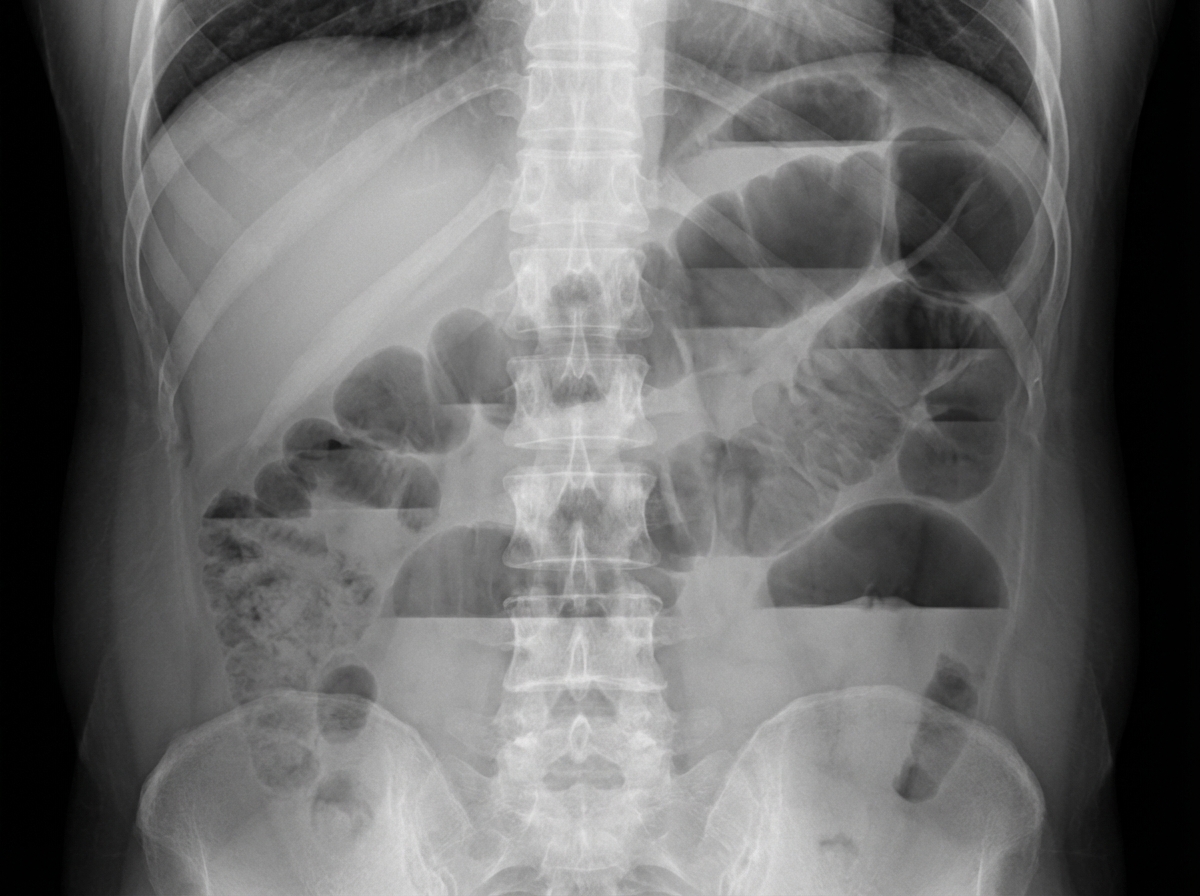
Which of the following is the most probable diagnosis based on the provided X-ray of the abdomen?
The 'spider leg' sign on an intravenous pyelogram (IVP) suggests which of the following conditions?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
