Abdominal and Pelvic Radiology — MCQs

On this page
What is the ideal investigation for fistula-in-ano?
Air on either side of the bowel wall on a radiograph is called:
Spider leg appearance on intravenous urography is typically seen in which of the following conditions?
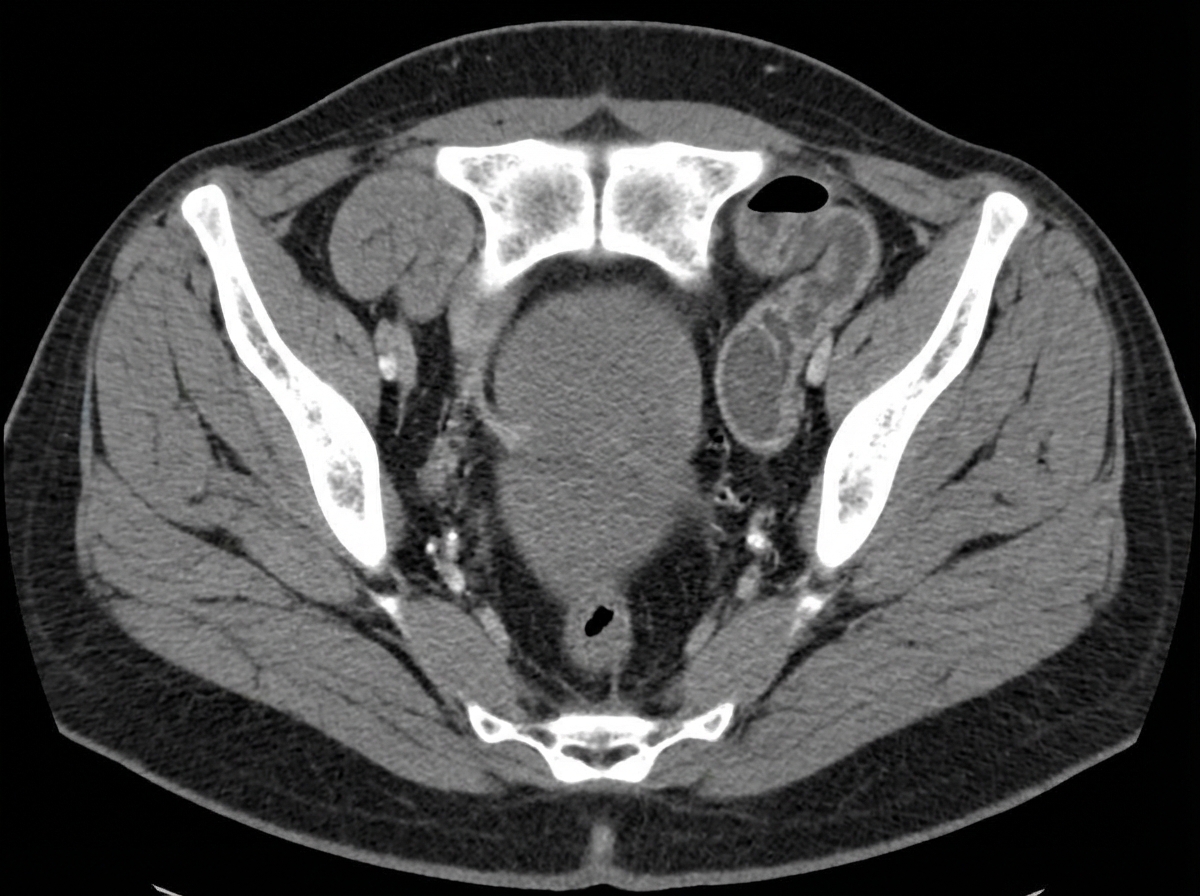
An elderly woman presented with abdominal pain and vomiting for three days. A computed tomogram of the abdomen was obtained. What is the diagnosis?
What is the investigation of choice for gallstones?
In which of the following conditions are fluid levels typically NOT visible on imaging?
Which of the following is the earliest sign of ulcerative colitis on a double contrast barium enema (DCBE) study?
A patient presents with marked loin pain, tenderness, and pyrexia. Initial investigations reveal non-specific findings on IVP. Ultrasound shows a heterogeneous mass with posterior acoustic enhancement and central necrosis and internal debris. CT scan demonstrates marginal enhancement with air densities within. What is the likely diagnosis?
Ultrasound and radionuclide studies are primary imaging modalities used for the assessment of which of the following conditions?
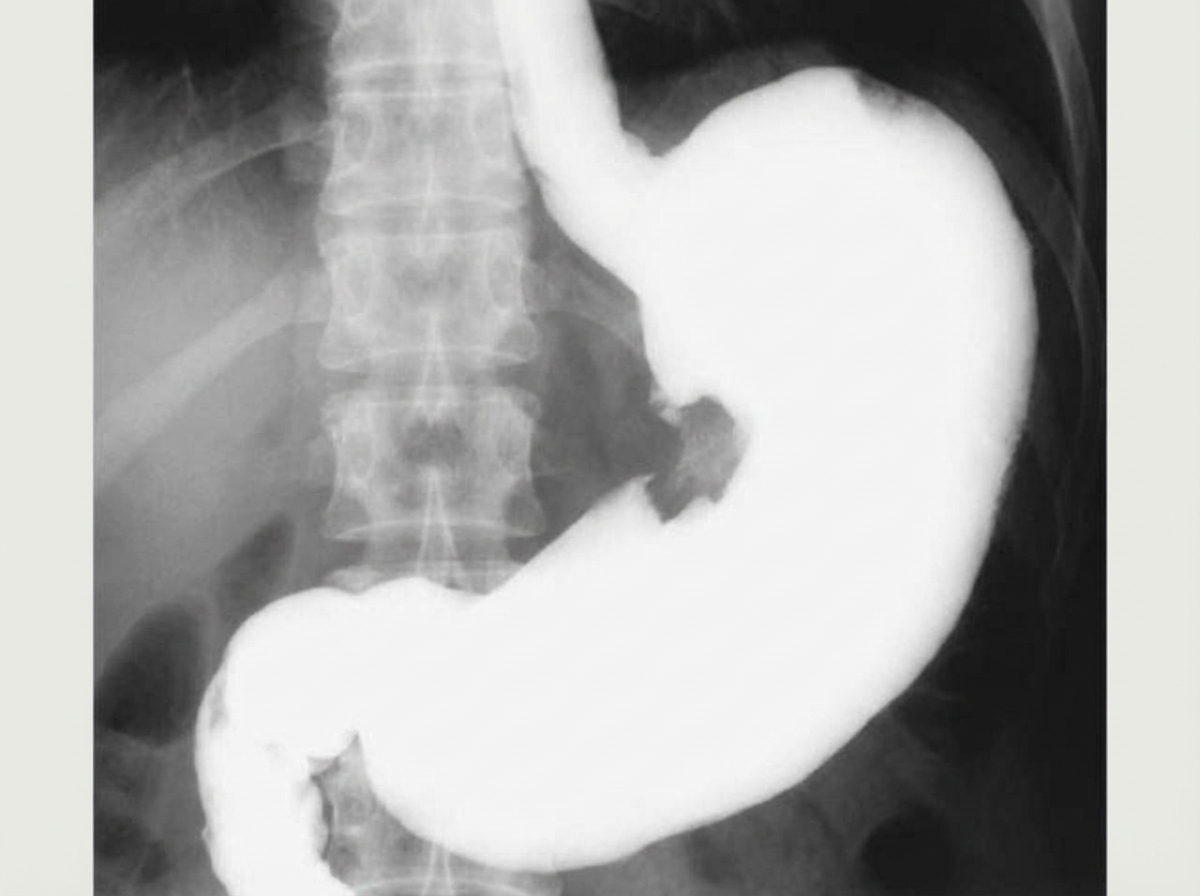
What is indicated by the arrow in the contrast X-ray abdomen?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
