Abdominal and Pelvic Radiology — MCQs

On this page
What type of CT scan is used to characterize the chemical composition of kidney stones?
What is the investigation of choice for retroperitoneal soft tissue sarcomas?
A previously healthy 61-year-old woman presents with a 3-week history of altered bowel habit and rectal bleeding. She refuses to undergo colonoscopy. Which of the following is the next best investigation?
A 40-year-old male complains of recurrent urinary tract infections. An X-ray KUB shows a radio-opaque shadow. What is the most likely diagnosis?
What is true regarding the barium study of ileocecal tuberculosis?
Bilateral spider leg appearance of the kidney in IVP is characteristic of which condition?
A middle-aged male, a diagnosed case of chronic ulcerative colitis, presents to the emergency department with fever and diarrhea for one week, and acute onset abdominal pain for six hours. An erect abdominal X-ray was taken as shown. What is the likely diagnosis?
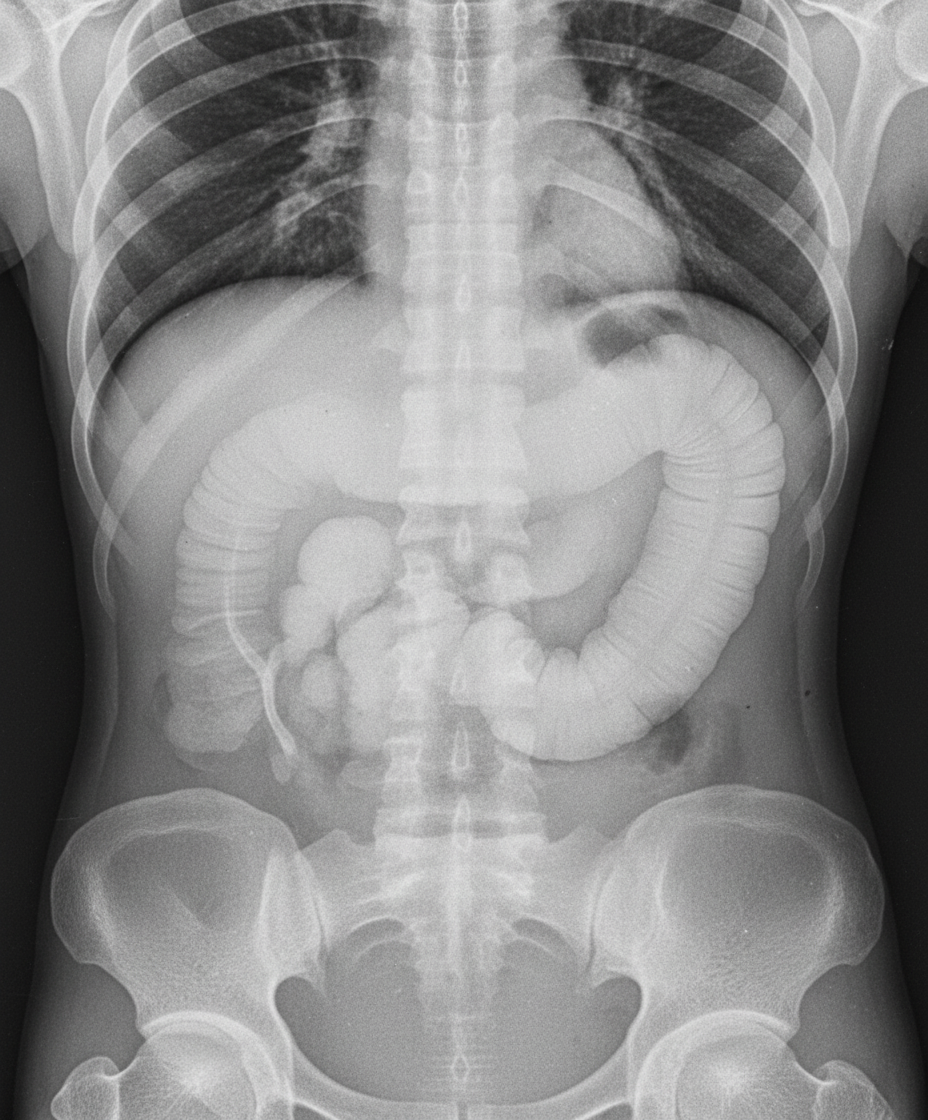
All are true about the radiological features of intestinal obstruction except?
The "string sign" on imaging is suggestive of which of the following conditions?
A middle-aged patient presents with a complaint of right hypochondrial pain. An X-ray shows an elevated right hemidiaphragm. Which of the following is NOT a possible diagnosis?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
