Abdominal and Pelvic Radiology — MCQs

On this page
A plain abdominal X-ray in a patient with a sigmoid volvulus will show a distended bowel loop with its apex in which location?
What is the preferred imaging modality for confirming choledocholithiasis?
Which imaging study has the highest pickup for a gastrojejunocolic fistula?
What pattern is described as "paint brush-like" in intravenous urography?
What is the term for a condition where blood bypasses the liver through an abnormal connection between the portal vein and the hepatic vein?
Which radiologic feature is suggestive of achalasia cardia?
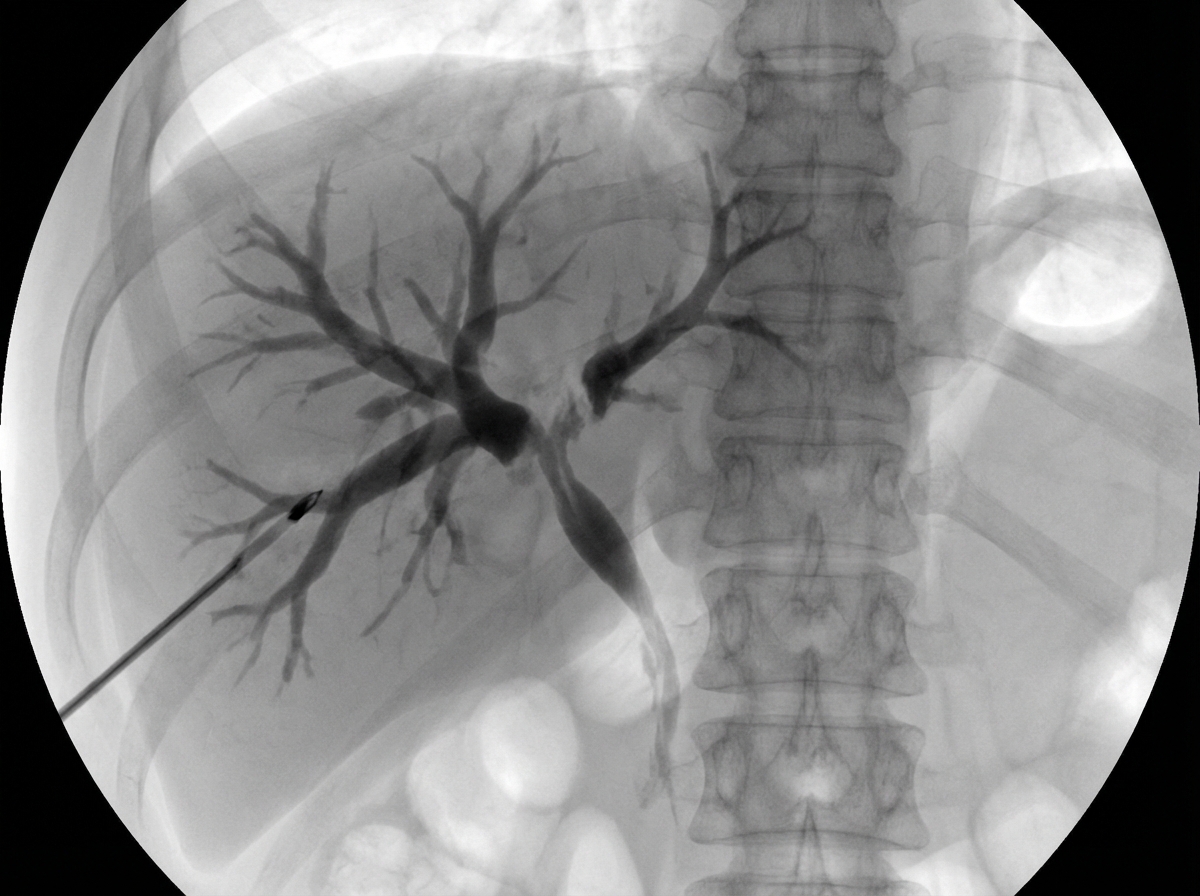
You are shown an AP view from a percutaneous trans-hepatic cholangiogram of a jaundiced patient. What is the MOST likely diagnosis?
USG abdomen of a 30-year-old SLE patient who cannot feel her baby moving for the past 7 days. What is the earliest appearance of Spalding sign?
All of the following statements regarding ileocaecal TB are TRUE, EXCEPT:
Sigmoid esophagus on barium swallow is seen in which of the following conditions?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
