Abdominal and Pelvic Radiology — MCQs

On this page
A 13-year-old boy presents with pain in the lower right tooth region with no remarkable medical history. On intraoral examination, tooth 85 was found to be carious and did not respond to EPT. Radiographs show changes in the apical region. What is the most probable diagnosis?
What is the first radiological sign of ulcerative colitis?
String of beads appearance on angiography is seen in which of the following conditions?
Omental caking on CT scan suggests a high possibility of which of the following conditions?
The CT severity index in acute pancreatitis is described by which scoring system?
Spleenic injury is diagnosed on X-ray by which of the following findings?
What is the investigation of choice (IOC) for polycystic kidney disease?
A 44-year-old man with a history of quadriplegia presented to the emergency department with symptoms of a urinary tract infection. What is the diagnosis?
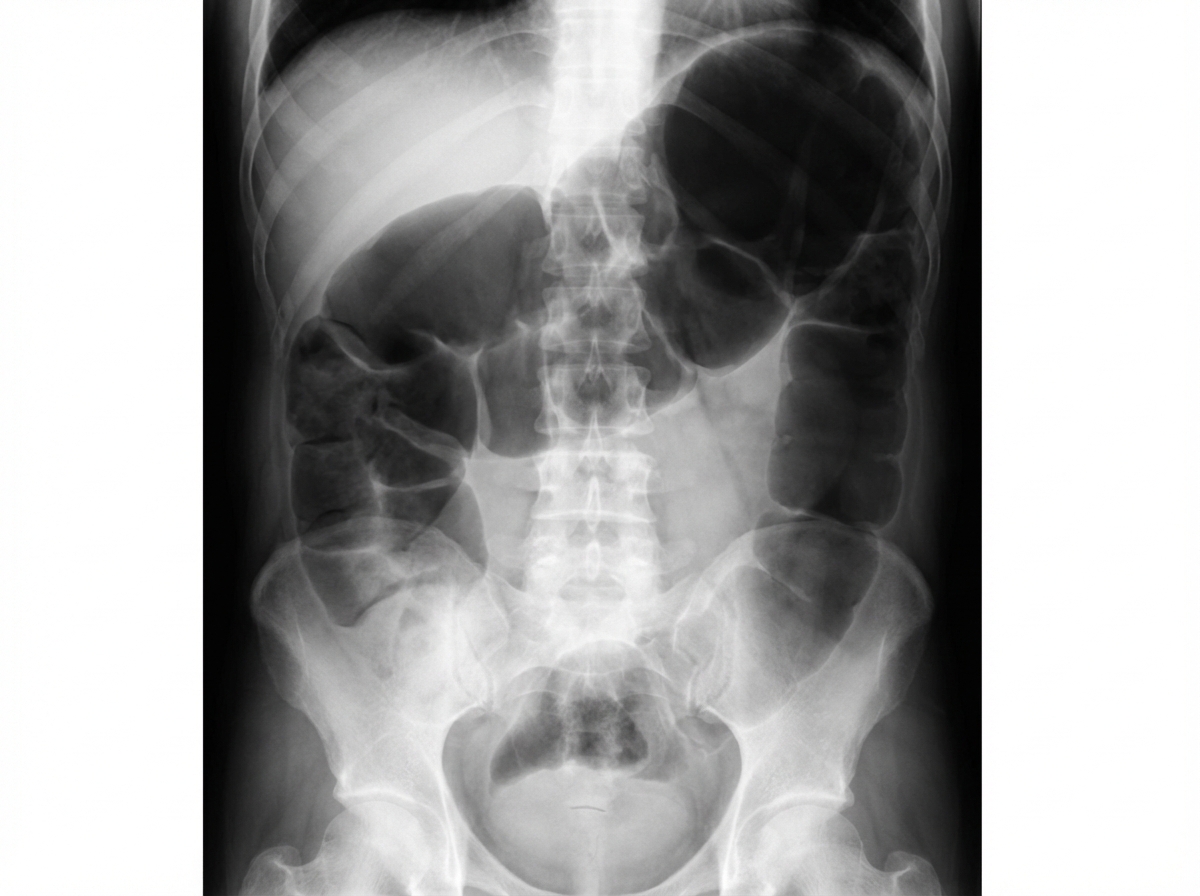
Which structure is outlined with contrast on a CT scan using intraperitoneal contrast material?
Which statement is true regarding the imaging characteristics of a lipoma on Ultrasound (USG), Magnetic Resonance Imaging (MRI), and Computed Tomography (CT)?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
