Abdominal and Pelvic Radiology — MCQs

On this page
Delayed centripetal contrast enhancement pattern is seen in which of the following conditions?
What is the investigation of choice for hydronephrosis?
A "saw-tooth" appearance of the colon on barium enema is typically seen with which of the following conditions?
The "apple core" sign is seen in which of the following conditions?
Which of the following is NOT a radiological finding of papillary necrosis on excretory urography?
A 32-year-old man presents with fever and pain in the right upper quadrant after food intake. What is the investigation of choice?
Hand joining sign is characteristic of?
Widening of the C-loop of the duodenum is diagnostic of which of the following conditions?
Plain abdominal X-ray is useful in which of the following conditions?
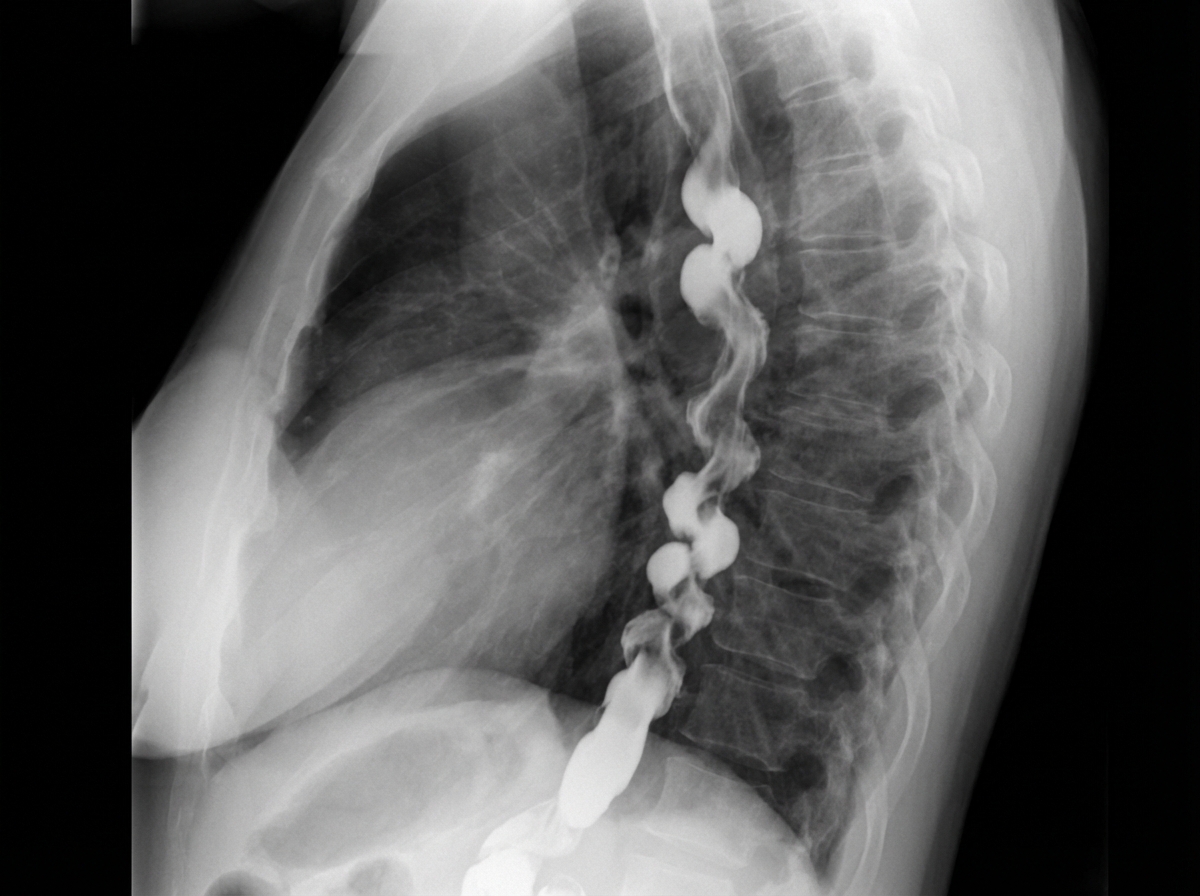
What diagnosis is suggested by this barium swallow?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
