Abdominal and Pelvic Radiology — MCQs

On this page
A patient presented with right upper quadrant pain and dyspepsia. Ultrasound showed an edematous gallbladder wall. What is the most sensitive investigation to confirm the suspected diagnosis?
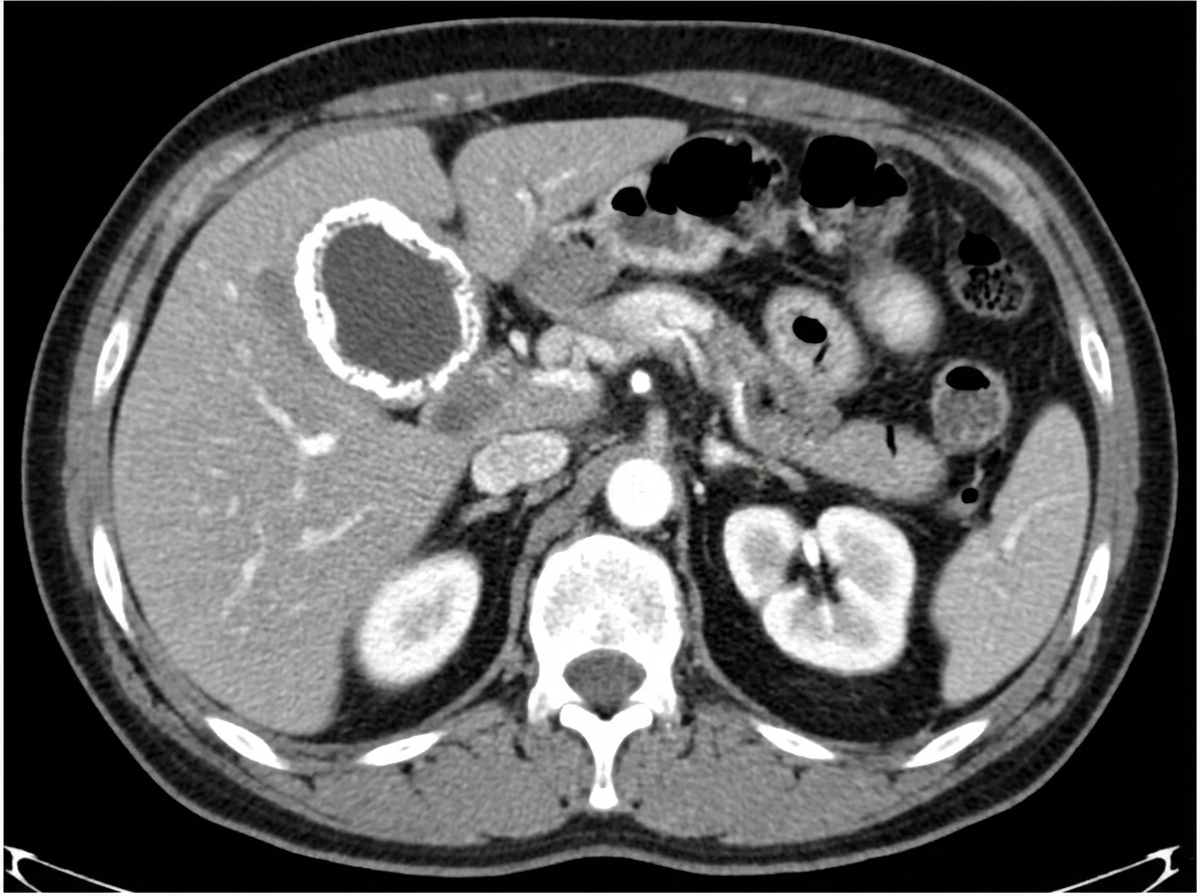
All of the following are true about an incidental finding in a 56-year-old female patient who underwent a CECT abdomen, except?
The 'stipple sign' in transitional cell carcinoma of the renal collecting system is best demonstrated by which imaging modality?
What are the differential diagnoses for right upper quadrant calcification?
What is the most common cause of malignant portal vein thrombosis?
Which of the following is NOT radioopaque?
The triad of vomiting, abdominal distension, and a "string of beads" sign on abdominal X-ray is typically suggestive of what condition?
What is the investigation of choice for evaluating a renal mass?
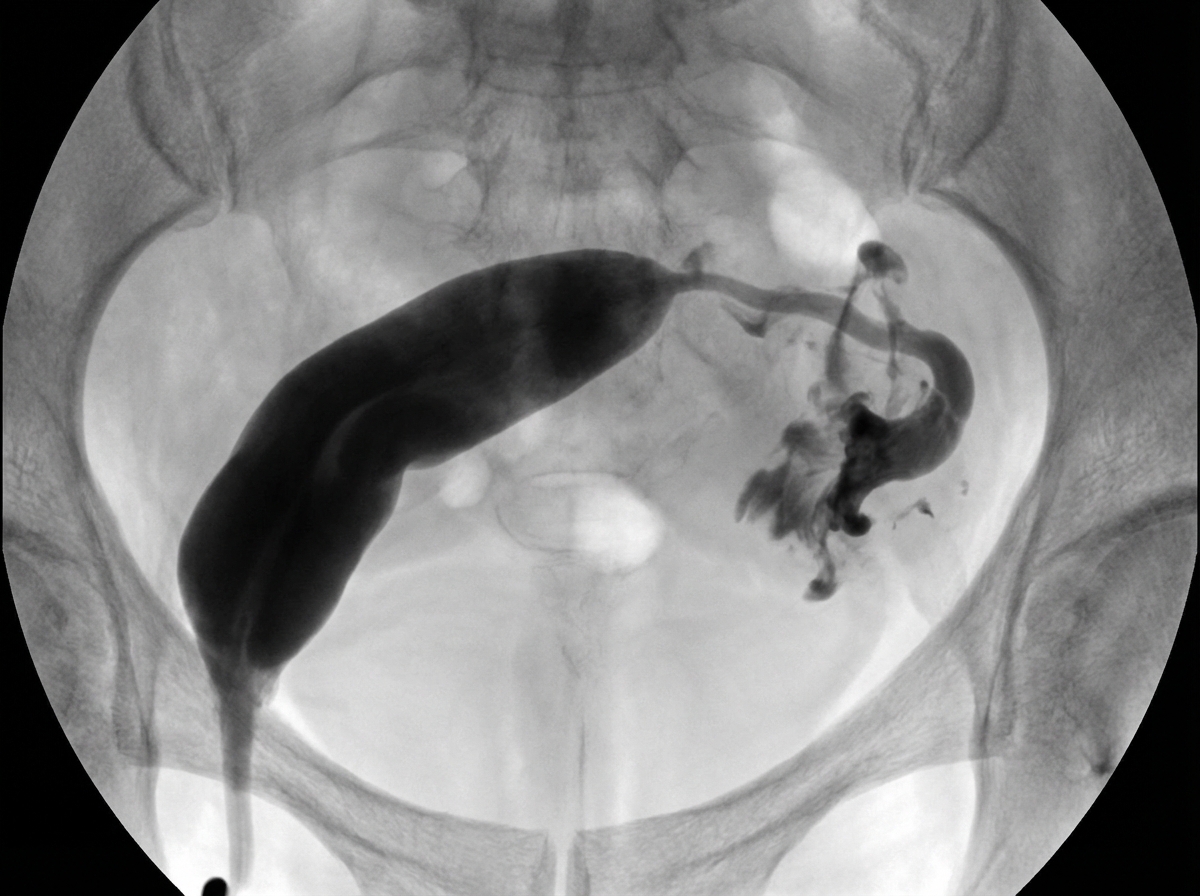
A hysterosalpingogram showing a congenital mullerian anomaly is depicted. What is the most likely diagnosis?
Which of the following is NOT a feature of papillary necrosis?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
