Abdominal and Pelvic Radiology — MCQs

On this page
A 46-year-old woman presents with a 6-month history of vague upper abdominal pain after fatty meals, some abdominal distension, and frequent indigestion. Physical examination shows an obese woman (BMI =32 kg/m2) with right upper quadrant tenderness. A CT scan discloses gallstones and an ectopic kidney. Which of the following is the expected location of the ectopic kidney?
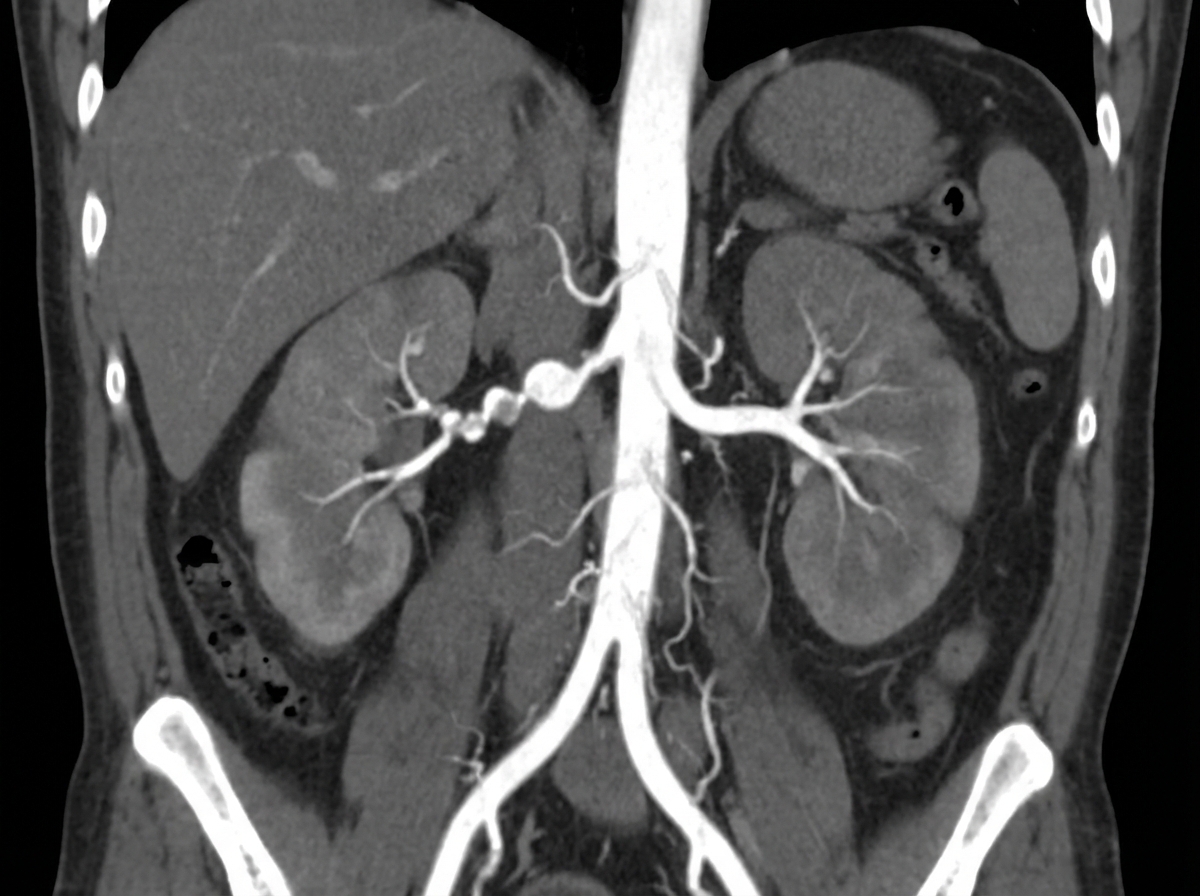
A 26-year-old male presents with abdominal pain and episodes of hematuria. His blood pressure is 160/100 mm Hg and is refractory to standard antihypertensive drugs. Renal Doppler shows a parvus tardus pattern. Subsequent CT renal angiogram was performed. This condition, as depicted, may occur in all of the following except?
Which of the following is NOT a feature of ischemic colitis?
The most appropriate investigation for diagnosing the condition shown in the X-ray is:
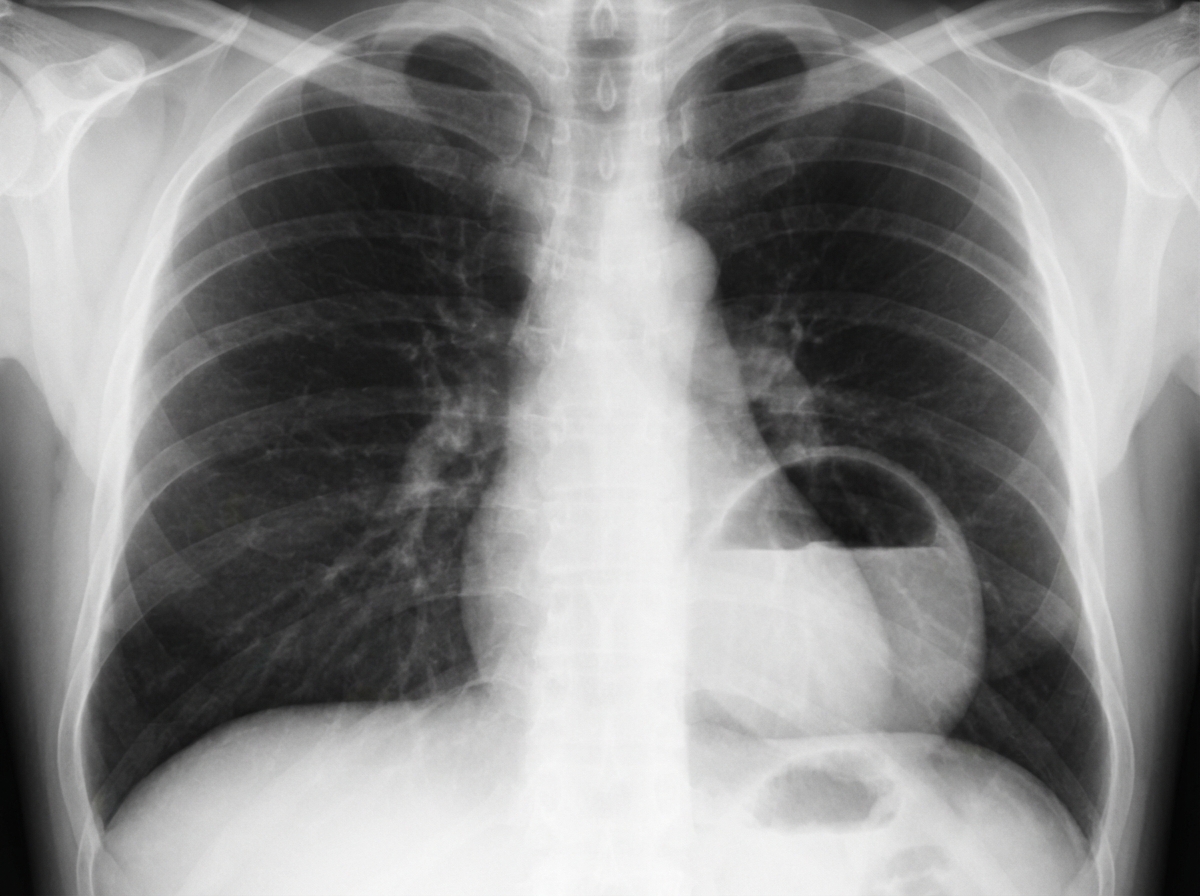
Corkscrew appearance on radiography is typically seen in which of the following conditions?
Confluent areas of pancreatic parenchyma that do not demonstrate enhancement after the administration of intravenous contrast material are known as?
A CT scan of acute pancreatitis will show the following features, except:
Which of the following is NOT a feature suggestive of acute cholecystitis on CT abdomen?
What is the investigation of choice for gall bladder stone?
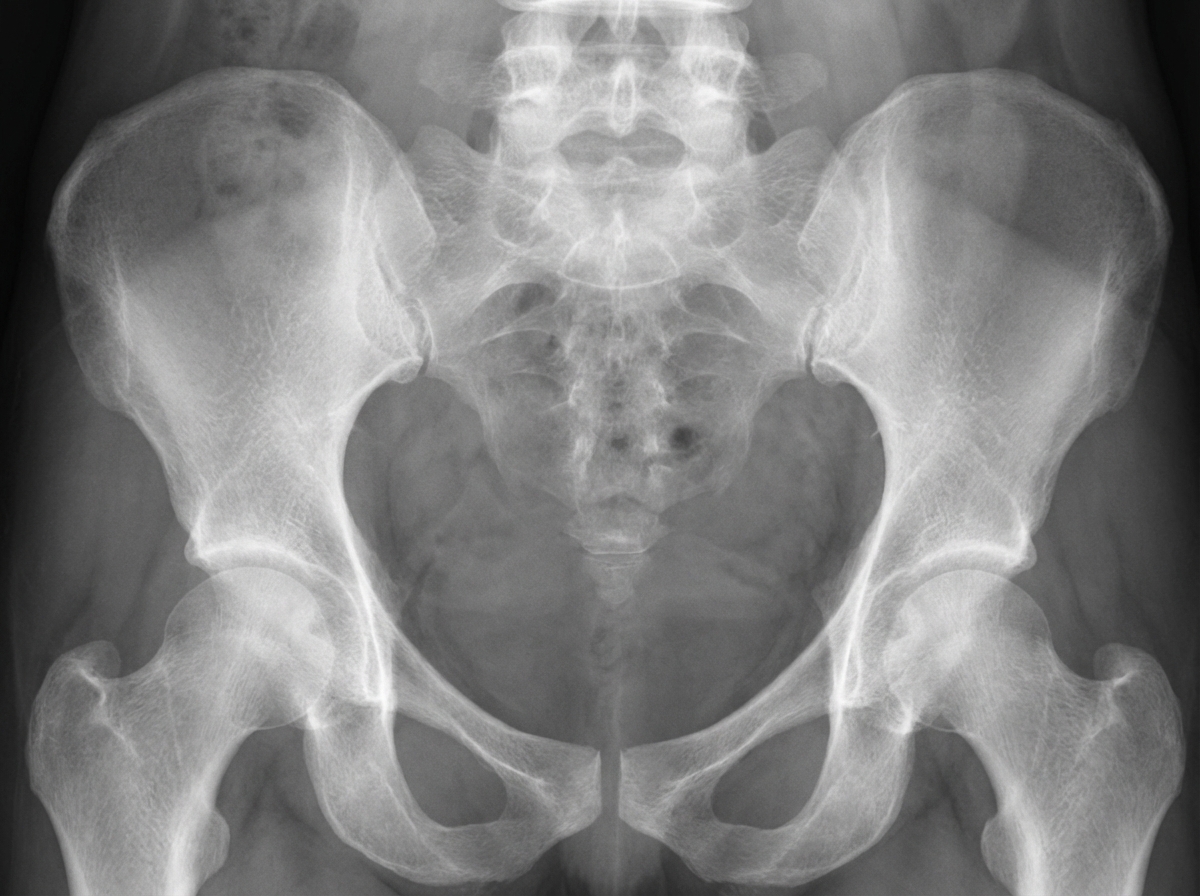
What type of pelvic appearance is this?
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
