Abdominal and Pelvic Radiology — MCQs

On this page
'Rim' and 'ball' nephrograms in intravenous urography are seen in which condition?
Gasless abdomen on X-ray is found in all except:
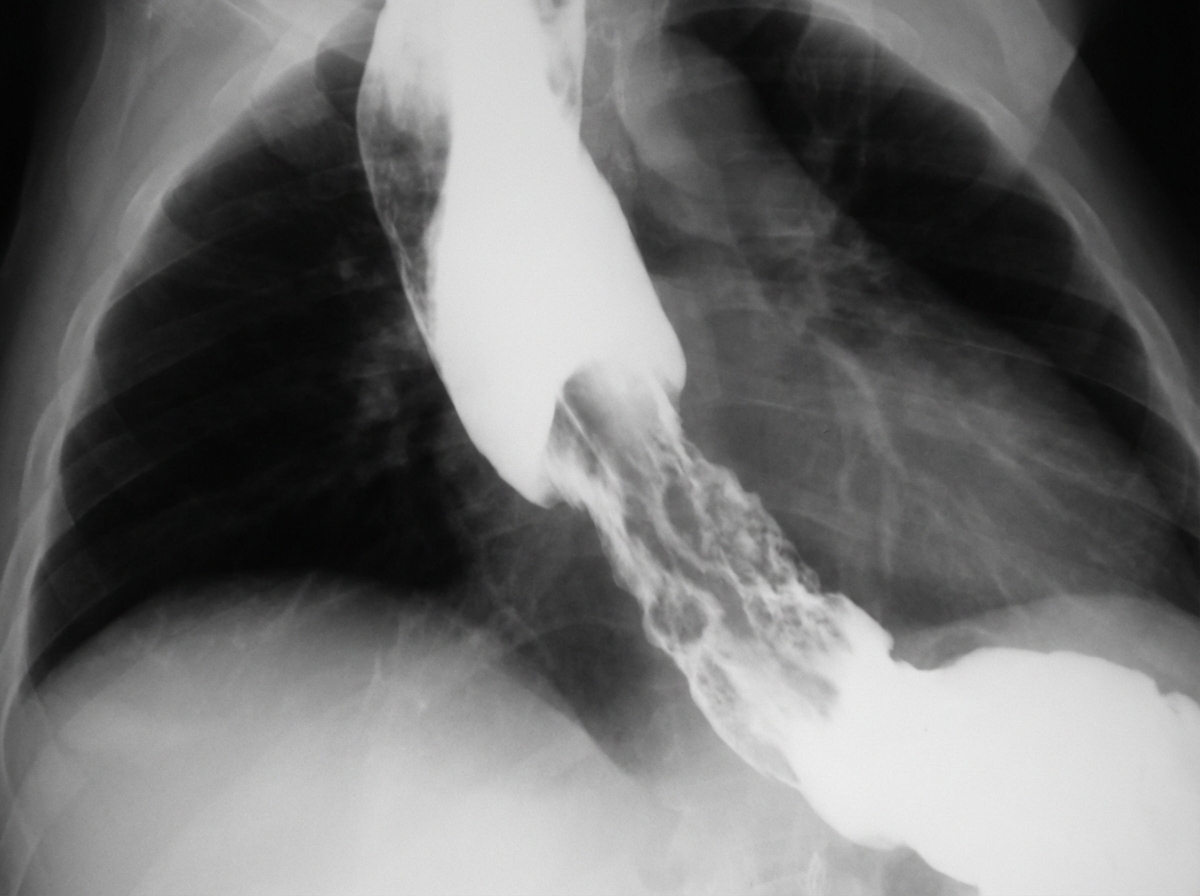
A 64-year-old man develops increasing dysphagia over many months. A barium swallow is performed. What is the most likely cause of his clinical presentation?
What is the current imaging technique of choice for the diagnosis of hydatidiform mole?
What does a hysterosalpingography (HSG) report typically show in cases of tubal patency issues?
A stab wound immediately superior to the pubic symphysis on the anterior pelvic wall would most likely injure which visceral organ first?
Which of the following is the most sensitive imaging modality for the diagnosis of idiopathic chronic pancreatitis (IOC)?
Which of the following is NOT a radiological feature of sigmoid volvulus?
Radiography of which of the following renal stones shows opacity, EXCEPT?
Type II Abernethy malformation refers to:
Practice by Chapter
Imaging of Liver
Practice Questions
Biliary Tract Imaging
Practice Questions
Pancreatic Imaging
Practice Questions
Spleen and Lymphatic System
Practice Questions
Gastrointestinal Tract Imaging
Practice Questions
Renal and Urinary Tract Imaging
Practice Questions
Adrenal Imaging
Practice Questions
Female Pelvic Imaging
Practice Questions
Male Pelvic Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Acute Abdomen Imaging
Practice Questions
Imaging of Peritoneal Cavity and Retroperitoneum
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
